Abstract
Background and aims
Early identification of non-response to steroids is critical in patients with autoimmune hepatitis (AIH) causing acute-on-chronic liver failure (ACLF). We assessed if this non-response can be accurately identified within first few days of treatment.
Methods
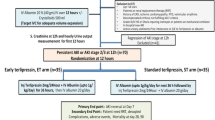
Patients with AIH-ACLF without baseline infection/hepatic encephalopathy were identified from APASL ACLF research consortium (AARC) database. Diagnosis of AIH-ACLF was based mainly on histology. Those treated with steroids were assessed for non-response (defined as death or liver transplant at 90 days for present study). Laboratory parameters, AARC, and model for end-stage liver disease (MELD) scores were assessed at baseline and day 3 to identify early non-response. Utility of dynamic SURFASA score [− 6.80 + 1.92*(D0-INR) + 1.94*(∆%3-INR) + 1.64*(∆%3-bilirubin)] was also evaluated. The performance of early predictors was compared with changes in MELD score at 2 weeks.
Results
Fifty-five out of one hundred and sixty-five patients (age—38.2 ± 15.0 years, 67.2% females) with AIH-ACLF [median MELD 24 (IQR: 22–27); median AARC score 7 (6–9)] given oral prednisolone 40 (20–40) mg per day were analyzed. The 90 day transplant-free survival in this cohort was 45.7% with worse outcomes in those with incident infections (56% vs 28.0%, p = 0.03). The AUROC of pre-therapy AARC score [0.842 (95% CI 0.754–0.93)], MELD [0.837 (95% CI 0.733–0.94)] score and SURFASA score [0.795 (95% CI 0.678–0.911)] were as accurate as ∆MELD at 2 weeks [0.770 (95% CI 0.687–0.845), p = 0.526] and better than ∆MELD at 3 days [0.541 (95% CI 0.395, 0.687), p < 0.001] to predict non-response. Combination of AARC score > 6, MELD score > 24 with SURFASA score ≥ − 1.2, could identify non-responders at day 3 (concomitant— 75% vs either − 42%, p < 0.001).
Conclusion
Baseline AARC score, MELD score, and the dynamic SURFASA score on day 3 can accurately identify early non-response to steroids in AIH-ACLF.




Similar content being viewed by others
Abbreviations
- AARC:
-
APASL ACLF research consortium
- ACLF:
-
Acute-on-chronic liver failure
- AIH:
-
Autoimmune hepatitis
- ALF:
-
Acute liver failure
- APASL:
-
Asia Pacific Association of Study of Liver Disease
- HAV:
-
Hepatitis A virus
- HEV:
-
Hepatitis E virus
- MELD:
-
Model for end-stage liver disease
References
Mack CL, Adams D, Assis DN, et al. Diagnosis and management of autoimmune hepatitis in adults and children: 2019 practice guidance and guidelines from the American association for the study of liver diseases. Hepatology. 2020. https://doi.org/10.1002/hep.31065
Rahim MN, Liberal R, Miquel R, Heaton ND, Heneghan MA. Acute severe autoimmune hepatitis: corticosteroids or liver transplantation? Liver Transpl. 2019;25(6):946–959. https://doi.org/10.1002/lt.25451
Rahim MN, Miquel R, Heneghan MA. Approach to the patient with acute severe autoimmune hepatitis. JHEPReport. 2020;2:6. https://doi.org/10.1016/j.jhepr.2020.100149
Sarin SK, Choudhury A, Sharma MK, et al. Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific association for the study of the liver (APASL): an update. Hepatol Int. 2019;13(4):353–390. https://doi.org/10.1007/s12072-019-09946-3
Yeoman AD, Westbrook RH, Zen Y, et al. Prognosis of acute severe autoimmune hepatitis (AS-AIH): the role of corticosteroids in modifying outcome. J Hepatol. 2014;61(4):876–882. https://doi.org/10.1016/j.jhep.2014.05.021
Zachou K, Arvaniti P, Azariadis K, et al. Prompt initiation of high-dose i.v. corticosteroids seems to prevent progression to liver failure in patients with original acute severe autoimmune hepatitis. Hepatol Res. 2019;49(1):96–104. https://doi.org/10.1111/hepr.13252
Anand L, Choudhury A, Bihari C, et al. Flare of autoimmune hepatitis causing acute on chronic liver failure: diagnosis and response to corticosteroid therapy. Hepatology. 2019;70(2):587–596. https://doi.org/10.1002/hep.30205
Fujiwara K, Yasui S, Yokosuka O. Autoimmune acute liver failure: an emerging etiology for intractable acute liver failure. Hepatol Int. 2013;7(2):335–346. https://doi.org/10.1007/s12072-012-9402-3
Ichai P, Duclos-Vallée JC, Guettier C, et al. Usefulness of corticosteroids for the treatment of severe and fulminant forms of autoimmune hepatitis. Liver Transpl. 2007;13(7):996–1003. https://doi.org/10.1002/lt.21036
Joshita S, Yoshizawa K, Umemura T, et al. Clinical features of autoimmune hepatitis with acute presentation: a Japanese nationwide survey. J Gastroenterol. 2018;53(9):1079–1088. https://doi.org/10.1007/s00535-018-1444-4
Martin ED, Coilly A, Chazouillères O, et al. Early liver transplantation for corticosteroid non-responders with acute severe autoimmune hepatitis: the SURFASA score. J Hepatol. 2021;74(6):1325–1334. https://doi.org/10.1016/j.jhep.2020.12.033
Noguchi F, Chu P, sung, Yoshida A, et al. Early dynamics of meld scores predict corticosteroid responsiveness to severe acute-onset autoimmune hepatitis. Clin Gastroenterol Hepatol. 2021. https://doi.org/10.1016/j.cgh.2021.06.006
Shalimar N, Kedia S, Mahapatra SJ, et al. Severity and outcome of acute-on-chronic liver failure is dependent on the etiology of acute hepatic insults: analysis of 368 patients. J Clin Gastroenterol. 2017;51(8):734–741. https://doi.org/10.1097/MCG.0000000000000823
Sharma S, Agarwal S, Gopi S, et al. Determinants of outcomes in autoimmune hepatitis presenting as acute on chronic liver failure without extrahepatic organ dysfunction upon treatment with steroids. J Clin Exp Hepatol. 2021;11(2):171–180. https://doi.org/10.1016/j.jceh.2020.08.007
Granito A, Muratori P, Muratori L. Acute-on-chronic liver failure: a complex clinical entity in patients with autoimmune hepatitis. J Hepatol. 2021. https://doi.org/10.1016/j.jhep.2021.06.035
Stravitz RT, Lefkowitch JH, Fontana RJ, et al. Autoimmune acute liver failure: proposed clinical and histological criteria. Hepatology. 2011;53(2):517–526. https://doi.org/10.1002/hep.24080
Choudhury A, Jindal A, Maiwall R, et al. Liver failure determines the outcome in patients of acute-on-chronic liver failure (ACLF): comparison of APASL ACLF research consortium (AARC) and CLIF-SOFA models. Hepatol Int. 2017;11(5):461–471. https://doi.org/10.1007/s12072-017-9816-z
Funding
None.
Author information
Authors and Affiliations
Consortia
Corresponding authors
Ethics declarations
Conflict of interests
Sanchit Sharma, Samagra Agarwal, Anoop Saraya, Ashok Kumar Choudhury, Sanjiv Saigal, A S Soin, Akash Shukla, Manoj K Sahu, Laurentius A Lesmana, Renaldi C Lesmana, Samir N Shah, Jinhua Hu, Soek Siam Tan, Dinesh Jothimani, Mohammed Rela, Hasmik L Ghazinyan, DN Amrapurkar, C E Eapen, Ashish Goel, Diana Alcantra Payawal, Saeed Hamid, Amna S Butt, Duan Zhongping, Virender Singh, Ajay Duseja, Ajit Sood, Vandana Midha, Mamun Al Mahtab, Dong Joon Kim, Qin Ning, Anand V Kulkarni, PN Rao, Guan Huei Lee, Sombat Treeprasertsuk, Xin Shaojie, Md. Fazal Karim, Jose D Sollano, Kemal Fariz Kalista, Rino Alvani Gani, VG Mohan Prasad, Shiv Kumar Sarin are none of the authors had any conflicts of interests.
Consent for publication
Waived off from IEC board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sharma, S., Agarwal, S., Saraya, A. et al. Identifying the early predictors of non-response to steroids in patients with flare of autoimmune hepatitis causing acute-on-chronic liver failure. Hepatol Int 17, 989–999 (2023). https://doi.org/10.1007/s12072-023-10482-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-023-10482-4