Abstract
Objective
No brand direct-acting antiviral agents (DAAs) are available for treatment of HIV-1/HCV co-infected patients in China. This study aimed to observe the therapeutic efficacy and safety of generic DAAs for affected Chinese patients.
Design
Real-world setting to elucidate whether DAAs were tolerated and effective in HIV-1/HCV co-infected patients.
Methods
176 HIV-1/HCV co-infected patients received anti-HCV DAA treatment together with ART regimens for HIV infection. Among the 176 patients, 99 patients were treated with SOF + DCV ± RBV, 60 patients were treated with SOF + LDV ± RBV, and 17 patients received SOF + RBV ± Peg-IFN regimens, for 12 or 24 weeks, respectively. The primary endpoint was undetectable HCV RNA 12 weeks after therapy was completed (SVR12). Data pertaining to safety and adverse events were analyzed.
Results
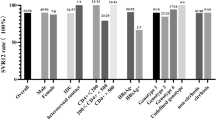
151/176 HIV-1/HCV co-infected patients finished the treatment and 12-week follow-up. SVR12 for the patients treated with regimens of SOF + DCV, SOF + DCV+RBV, SOF + Peg-IFN+RBV, SOF + RBV, SOF + LDV, and SOF + LDV+RBV for 12 or 24 weeks was 100% (75/75), 100% (11/11), 100% (14/14), 100% (2/2), 95.2% (40/42), and 100% (7/7), respectively. HIV-1/HCV co-infected patients with liver cirrhosis achieved well SRV12. Notably, there was no significant difference in adverse effects among patients with different baseline CD4+ T-cell count in those who received DAA regimens with or without Peg-IFN and RBV.
Conclusion
We showed generic SOF + DCV and SOF + LDV regimens were well tolerated and with high efficiency. Patient’s baseline CD4+ T-cell count did not exhibit significant difference in adverse effects.


Similar content being viewed by others
References
Panel AIHG. Hepatitis C guidance: AASLD-IDSA recommendations for testing, managing, and treating adults infected with hepatitis C virus. Hepatology 2015;62(3):932–954. https://doi.org/10.1002/hep.27950
Rockstroh JK, Mocroft A, Soriano V, Tural C, Losso MH, Horban A, et al. Influence of hepatitis C virus infection on HIV-1 disease progression and response to highly active antiretroviral therapy. J Infect Dis 2005;192(6):992–1002. https://doi.org/10.1086/432762
Chen TY, Ding EL, Seage Iii GR, Kim AY. Meta-analysis: increased mortality associated with hepatitis C in HIV-infected persons is unrelated to HIV disease progression. Clin Infect Dis 2009;49(10):1605–1615. https://doi.org/10.1086/644771
Data Collection on Adverse Events of Anti HIVdSG, Smith C, Sabin CA, Lundgren JD, Thiebaut R, Weber R, et al. Factors associated with specific causes of death amongst HIV-positive individuals in the D:A: D Study. AIDS 2010;24(10):1537–1548. https://doi.org/10.1097/qad.0b013e32833a0918
Greub G, Ledergerber B, Battegay M, Grob P, Perrin L, Furrer H, et al. Clinical progression, survival, and immune recovery during antiretroviral therapy in patients with HIV-1 and hepatitis C virus coinfection: the Swiss HIV Cohort Study. Lancet 2000;356(9244):1800–1805
Torriani FJ, Rodriguez-Torres M, Rockstroh JK, Lissen E, Gonzalez-Garcia J, Lazzarin A, et al. Peginterferon Alfa-2a plus ribavirin for chronic hepatitis C virus infection in HIV-infected patients. N Engl J Med 2004;351(5):438–450. https://doi.org/10.1056/NEJMoa040842
Chung RT, Andersen J, Volberding P, Robbins GK, Liu T, Sherman KE, et al. Peginterferon Alfa-2a plus ribavirin versus interferon alfa-2a plus ribavirin for chronic hepatitis C in HIV-coinfected persons. N Engl J Med 2004;351(5):451–459. https://doi.org/10.1056/NEJMoa032653
Zhu SS, Zeng QL, Dong Y, Xu ZQ, Wang LM, Chen DW, et al. Interferon-alpha plus ribavirin yields 98% sustained virologic response in children aged 1–5 years with iatrogenic chronic hepatitis C. Hepatol Int 2015;9(4):578–585. https://doi.org/10.1007/s12072-015-9671-8
Shi J, Li Y, Chang W, Zhang X, Wang FS. Current progress in host innate and adaptive immunity against hepatitis C virus infection. Hepatol Int 2017;11(4):374–383. https://doi.org/10.1007/s12072-017-9805-2
Wyles DL, Sulkowski MS, Dieterich D. Management of hepatitis C/HIV Coinfection in the era of highly effective hepatitis C virus direct-acting antiviral therapy. Clin Infect Dis 2016;63(Suppl 1):S3–S11. https://doi.org/10.1093/cid/ciw219
Wyles DL, Ruane PJ, Sulkowski MS, Dieterich D, Luetkemeyer A, Morgan TR, et al. Daclatasvir plus sofosbuvir for HCV in patients coinfected with HIV-1. N Engl J Med 2015;373(8):714–725. https://doi.org/10.1056/NEJMoa1503153
Luetkemeyer AF, McDonald C, Ramgopal M, Noviello S, Bhore R, Ackerman P. 12 weeks of daclatasvir in combination with sofosbuvir for HIV–HCV coinfection (ALLY-2 study): efficacy and safety by HIV combination antiretroviral regimens. Clin Infect Dis 2016;62(12):1489–1496. https://doi.org/10.1093/cid/ciw163
Naggie S, Cooper C, Saag M, Workowski K, Ruane P, Towner WJ, et al. Ledipasvir and sofosbuvir for HCV in patients coinfected with HIV-1. N Engl J Med 2015;373(8):705–713. https://doi.org/10.1056/NEJMoa1501315
Osinusi A, Townsend K, Kohli A, Nelson A, Seamon C, Meissner EG, et al. Virologic response following combined ledipasvir and sofosbuvir administration in patients with HCV genotype 1 and HIV co-infection. JAMA 2015;313(12):1232–1239. https://doi.org/10.1001/jama.2015.1373
Zhang F, Zhu H, Wu Y, Dou Z, Zhang Y, Kleinman N, et al. HIV, hepatitis B virus, and hepatitis C virus co-infection in patients in the China National Free Antiretroviral Treatment Program, 2010–2012: a retrospective observational cohort study. Lancet Infect Dis 2014;14(11):1065–1072. https://doi.org/10.1016/S1473-3099(14)70946-6
Zeng QL, Xu GH, Zhang JY, Li W, Zhang DW, Li ZQ, et al. Generic ledipasvir-sofosbuvir for patients with chronic hepatitis C: a real-life observational study. J Hepatol 2017;66(6):1123–1129. https://doi.org/10.1016/j.jhep.2017.01.025
European Association for the Study of the Liver. Electronic address eee. EASL recommendations on treatment of hepatitis C 2016. J Hepatol 2017;66(1):153–194. https://doi.org/10.1016/j.jhep.2016.09.001
Hezode C, Bronowicki JP. Ideal oral combinations to eradicate HCV: the role of ribavirin. J Hepatol 2016;64(1):215–225. https://doi.org/10.1016/j.jhep.2015.09.009
Foster GR, Irving WL, Cheung MC, Walker AJ, Hudson BE, Verma S, et al. Impact of direct acting antiviral therapy in patients with chronic hepatitis C and decompensated cirrhosis. J Hepatol 2016;64(6):1224–1231. https://doi.org/10.1016/j.jhep.2016.01.029
Simmons B, Saleem J, Hill A, Riley RD, Cooke GS. Risk of late relapse or reinfection with hepatitis C virus after achieving a sustained virological response: a systematic review and meta-analysis. Clin Infect Dis 2016;62(6):683–694. https://doi.org/10.1093/cid/civ948
Hagan H, Jordan AE, Neurer J, Cleland CM. Incidence of sexually transmitted hepatitis C virus infection in HIV-positive men who have sex with men. AIDS 2015;29(17):2335–2345. https://doi.org/10.1097/QAD.0000000000000834
El-Sherif O, Khoo S, Solas C. Key drug-drug interactions with direct-acting antiviral in HIV–HCV coinfection. Curr opin HIV AIDS 2015;10(5):348–354. https://doi.org/10.1097/COH.0000000000000185
Younossi ZM, Stepanova M, Sulkowski M, Naggie S, Henry L, Hunt S. Sofosbuvir and ledipasvir improve patient-reported outcomes in patients co-infected with hepatitis C and human immunodeficiency virus. J Viral Hepatitis 2016;23(11):857–865. https://doi.org/10.1111/jvh.12554
Younossi ZM, Stepanova M, Sulkowski M, Wyles D, Kottilil S, Hunt S. Patient-reported outcomes in patients co-infected with hepatitis C virus and human immunodeficiency virus treated with sofosbuvir and velpatasvir: the ASTRAL-5 study. Liver Int 2017;37(12):1796–1804. https://doi.org/10.1111/liv.13462
Funding
This study was supported by The National Natural Science Foundation of China (No. 81601731).
Author information
Authors and Affiliations
Contributions
Yuanyuan Li, Linghua Li, and Jun Liu contributed equally as co-first authors. Fu-Sheng Wang contributed to the design of this study. All authors contributed to data collection, the interpretation of data, the drafting, and revision of this manuscript. The final version of this manuscript was approved by all authors.
Corresponding authors
Ethics declarations
Conflict of interest
Yuanyuan Li, Linghua Li, Jun Liu, Da-Wei Zhang, Fang Zhao, Li Wang, Aizezi Mahemure, Ronghui Xie, Suyun Lei, Weiping Cai, Xicheng Wang, Zhanjun Shu, Xiejie Chen, Hui Wang, and Fu-Sheng Wang declared that there were no conflicts regarding funding or interest with this manuscript.
Ethical approval
This study protocol had been approved by the ethical committee of the Beijing 302 hospital and other institutions involved.
Rights and permissions
About this article
Cite this article
Li, Y., Li, L., Liu, J. et al. Tolerable and curable treatment in HIV/HCV co-infected patients using anti-HCV direct antiviral agents: a real-world observation in China. Hepatol Int 12, 465–473 (2018). https://doi.org/10.1007/s12072-018-9891-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-018-9891-9