Abstract
Purpose/introduction
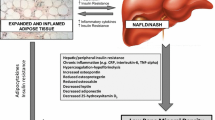
Growing evidence suggests complex interplay between nonalcoholic fatty liver disease (NAFLD) and bone health. The present study’s aim was to examine the impact of metformin treatment on circulating osteoprotegerin (OPG) in patients with NAFLD, a population in which this relationship has not yet been studied.
Methods
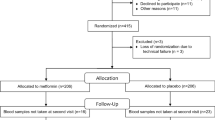
In a randomized, placebo-controlled study, 63 patients with NAFLD were assigned to one of two groups: Group 1 received daily metformin; Group 2 received a placebo. Metabolic parameters, insulin resistance markers and OPG levels were examined at baseline and at the end of the study.
Results
In the placebo group, liver function and OPG levels did not change during the study. Among metformin-treated patients, significant declines in OPG and alkaline phosphatase were observed. CRP and ALT decreased marginally during the 4-month treatment period. While at baseline circulating OPG levels did not differ significantly between the groups, by the end of the study OPG was significantly lower in patients treated with metformin than in the placebo group (p < 0.0001). Delta OPG was significantly greater in the metformin group than the placebo group (p = 0.001). In the general linear model, metformin treatment was the only significant independent predictor of endpoint and delta OPG.
Conclusions
Metformin treatment was associated with a significant decrease in OPG levels in patients with NAFLD. The effect on OPG was associated with exposure to metformin per se.
Clinical trial registration number
NCT01084486.

Similar content being viewed by others
References
Li M, Xu Y, Xu M, et al. Association between nonalcoholic fatty liver disease (NAFLD) and osteoporotic fracture in middle-aged and elderly Chinese. J Clin Endocrinol Metab 2012;97:2033–2038
Pardee PE, Dunn W, Schwimmer JB. Non-alcoholic fatty liver disease is associated with low bone mineral density in obese children. Aliment Pharmacol Ther 2012;35:248–254
Moon SS, Lee YS, Kim SW. Association of nonalcoholic fatty liver disease with low bone mass in postmenopausal women. Endocrine 2012;42:423–429
Manco M, Marcellini M, Giannone G, Nobili V. Correlation of serum TNF-alpha levels and histologic liver injury scores in pediatric nonalcoholic fatty liver disease. Am J Clin Pathol 2007;127:954–960
Chu CJ, Lu RH, Wang SS, et al. Risk factors associated with non-alcoholic fatty liver disease in Chinese patients and the role of tumor necrosis factor-alpha. Hepatogastroenterology 2007;54:2099–2102
Targher G, Bertolini L, Scala L, et al. Associations between serum 25-hydroxyvitamin D3 concentrations and liver histology in patients with non-alcoholic fatty liver disease. Nutr Metab Cardiovasc Dis 2007;17:517–524
Zou W, Hakim I, Tschoep K, Endres S, Bar-Shavit Z. Tumor necrosis factor-alpha mediates RANK ligand stimulation of osteoclast differentiation by an autocrine mechanism. J Cell Biochem 2001;83:70–83
Fernández-Real JM, Ortega F, Gómez-Ambrosi J, Salvador J, Frühbeck G, Ricart W. Circulating osteocalcin concentrations are associated with parameters of liver fat infiltration and increase in parallel to decreased liver enzymes after weight loss. Osteoporos Int 2010;21:2101–2107
Stern A, Laughlin GA, Bergstrom J, Barrett-Connor E. The sex-specific association of serum osteoprotegerin and receptor activator of nuclear factor kappaB legend with bone mineral density in older adults: the Rancho Bernardo study. Eur J Endocrinol 2007;156:555–562
Schoppet M, Preissner KT, Hofbauer LC. RANK Ligand and osteoprotegerin: paracrine regulators of bone metabolism and vascular function. Arterioscler Tromb Vasc Biol 2002;22:549–553
Jono S, Ikari Y, Shioi A, Mori K, Miki T, Hara K, et al. Serum osteoprotegerin levels are associated with the presence and severity of coronary artery disease. Circulation 2002;106:1192–1194
Browner WS, Lui L-Y, Cummings SR. Associations of serum osteoprotegerin levels with diabetes, stroke, bone density, fractures, and mortality in elderly women. J Clin Endocrinol Metab 2001;86:631–637
Pirgon O, Bilgin H, Tolu I, et al. Correlation of insulin sensitivity with bone mineral status in obese adolescents with nonalcoholic fatty liver disease. Clin Endocrinol (Oxf) 2011;75:189–195
Zhen D, Chen Y, Tang X. Metformin reverses the deleterious effects of high glucose on osteoblast function. J Diabetes Complications 2010;24(5):334–344
Sofer E, Boaz M, Matas Z, Mashavi M, Shargorodsky M. Treatment with insulin sensitizer metformin improves arterial properties, metabolic parameters, and liver function in patients with nonalcoholic fatty liver disease: a randomized, placebo-controlled trial. Metabolism 2011;60(9):1278–1284
Joy D, Thava VR, Scott BB. Diagnosis of fatty liver disease: is biopsy necessary? Eur J Gastroenterol Hepatol 2003;15:539–543
Mather KJ, Verma S, Anderson TJ. Improved endothelial function with metformin in type 2 diabetes mellitus. J Am Coll Cardiol 2001;37:1344–1350
Kraemer de Aguiar LG, Bahia LR, Villela N, Laflor C, Sicuro F, Wiernsperger N, et al. Metformin improves endothelial vascular reactivity in first-degree relatives of type 2 diabetic patients with metabolic syndrome and normal glucose tolerance. Diabetes Care 2006;29:1083–1089
Grant PJ. Beneficial effects of metformin on haemostasis and vascular function in man. Diabet Med 2003;29:6s44–6s52
Meaney E, Vela A, Samaniego V, Meaney A, Asbún J, Zempoalteca JC, et al. Metformin, arterial function, intima-media thickness and nitroxidation in metabolic syndrome: the mefisto study. Clin Exp Pharmacol Physiol 2008;35(8):895–903
Syn WK, Choi SS, Liaskou E, et al. Osteopontin is induced by hedgehog pathway activation and promotes fibrosis progression in nonalcoholic steatohepatitis. Hepatology 2011;53:106–115
Lima-Cabello E, García-Mediavilla MV, Miquilena-Colina ME, et al. Enhanced expression of pro-inflammatory mediators and liver X-receptor-regulated lipogenic genes in non-alcoholic fatty liver disease and hepatitis C. Clin Sci (Lond) 2011;120:239–250
Haukeland JW, Dahl TB, Yndestad A, et al. Fetuin A in nonalcoholic fatty liver disease: in vivo and in vitro studies. Eur J Endocrinol 2012;166:503–510
Indridason OS, Franzson L, Sigurdsson G. Serum osteoprotegerin and its relationship with bone mineral density and markers of bone turnover. Osteoporos Int 2005;16:417–423
Oh KW, Rhee EJ, Lee WY, et al. Circulating osteoprotegerin and receptor activator of NF-kappaB ligand system are associated with bone metabolism in middle-aged males. Clin Endocrinol (Oxf) 2005;62:92–89
Szulc P, Hofbauer LC, Heufelder AE, Roth S, Delmas PD. Osteoprotegerin serum levels in men: correlation with age, estrogen, and testosterone status. J Clin Endocrinol Metab 2001;86:3162–3165
Yano K, Tsuda E, Washida N, Kobayashi F, Goto M, Harada A. Immunological characterization of circulating osteoprotegerin/osteoclastogenesis inhibitory factor: increased serum concentrations in postmenopausal women with osteoporosis. J Bone Miner Res 1999;14:518–527
Fraher LJ, Watson PH, Kisiel M, Natale BV, Hodsman AB. Measurement of circulating osteoprotegerin (OPG) in human sera: inhibition of circulating OPG in osteoporotic patients treated with hPTH (1–34). J Bone Miner Res 2000;15(Suppl 1):S441
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent
The study was approved by the regional ethical committee, and all procedures were performed in accordance with the guidelines of the Declaration of Helsinki. Informed written consent was obtained from all the subjects before participation. The study has been registered in the ClinicalTrials.gov registry.
Rights and permissions
About this article
Cite this article
Sofer, E., Shargorodsky, M. Effect of metformin treatment on circulating osteoprotegerin in patients with nonalcoholic fatty liver disease. Hepatol Int 10, 169–174 (2016). https://doi.org/10.1007/s12072-015-9649-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-015-9649-6