Abstract
Purpose
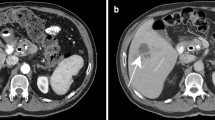
Eosinophilic liver abscesses (ELAs) are frequently encountered in the clinical field based on typical computed tomography (CT) findings and the presence of peripheral eosinophilia. In this study, the authors evaluated the clinical features and natural course of CT diagnosed ELAs.
Methods
The medical records of patients that underwent abdominal CT from July 2004 to February 2008 at Seoul National University Hospital were retrospectively evaluated. ELA was clinically diagnosed by the presence of peripheral eosinophilia (≥500 μL−1) and typical CT findings. The presumptive causes of clinically diagnosed ELA were divided into three categories, namely, parasitic infections, malignancies, and unidentified etiologies. Clinical courses and responses to treatment were evaluated.
Results
Clinically diagnosed ELAs were identified in 164 patients and the incidence of ELA was 0.68%. Of these patients, 118 (71.9%) showed radiologic resolution of clinically diagnosed ELA at a median 6.2 (0.2–33.1) months. In addition, 79 (48.2%) patients also achieved normalization of peripheral eosinophilia with radiologic resolution of clinically diagnosed ELA. In patients without identified etiologies, mean time to radiologic resolution was significantly shorter for patients treated empirically with an anti-parasitic drug than for those not treated [4.4 (0.9–26.3) vs. 12.2 (1.5–33.2) months, median (range), P = 0.001].
Conclusions
Clinically diagnosed ELA adopts a relatively benign course. Empirical anti-parasitic treatment in patients without an identified etiology may shorten the duration of clinically diagnosed ELA.
Similar content being viewed by others
References
Musso C, Castelo JS, Tsanaclis AM, Pereira FE. Prevalence of Toxocara-induced liver granulomas, detected by immunohistochemistry, in a series of autopsies at a Children’s Reference Hospital in Vitoria, ES, Brazil. Virchows Arch 2007;450:411–417
Kaplan KJ, Goodman ZD, Ishak KG. Eosinophilic granuloma of the liver: a characteristic lesion with relationship to visceral larva migrans. Am J Surg Pathol 2001;25:1316–1321
Sakakibara A, Baba K, Niwa S, Yagi T, Wakayama H, Yoshida K, Kobayashi T, Yokoi T, Hara K, Itoh M, Kimura E. Visceral larva migrans due to Ascaris suum which presented with eosinophilic pneumonia and multiple intra-hepatic lesions with severe eosinophil infiltration-outbreak in a Japanese area other than Kyushu. Intern Med 2002;41:574–579
Azuma K, Yashiro N, Kinoshita T, Yoshigi J, Ihara N. Hepatic involvement of visceral larva migrans due to Toxocara canis: a case report—CT and MR findings. Radiat Med 2002;20:89–92
Yoo SY, Han JK, Kim YH, Kim TK, Choi BI, Han MC. Focal eosinophilic infiltration in the liver: radiologic findings and clinical course. Abdom Imaging 2003;28:326–332
Byun JH, Yang DH, Yoon SE, Won HJ, Shin YM, Jeong YY, Jang SJ. Contrast-enhancing hepatic eosinophilic abscess during the hepatic arterial phase: a mimic of hepatocellular carcinoma. Am J Roentgenol 2006;186:168–173
Lee WJ, Lim HK, Lim JH, Kim SH, Choi SH, Lee SJ. Foci of eosinophil-related necrosis in the liver: imaging findings and correlation with eosinophilia. Am J Roentgenol 1999;172:1255–1261
Lim JH. Toxocariasis of the liver: visceral larva migrans. Abdom Imaging 2008;33:151–156
Sun JS, Kim JK, Won JH, Lee KM, Cheong JY, Kim YB. MR findings in eosinophilic infiltration of the liver. J Comput Assist Tomogr 2005;29:191–194
Lim JH, Lee WJ, Lee DH, Nam KJ. Hypereosinophilic syndrome: CT findings in patients with hepatic lobar or segmental involvement. Korean J Radiol 2000;1:98–103
Jang HJ, Lee WJ, Lee SJ, Kim SH, Lim HK, Lim JH. Focal eosinophilic necrosis of the liver in patients with underlying gastric or colorectal cancer: CT differentiation from metastasis. Korean J Radiol 2002;3:240–244
Saito F, Okabe Y, Suga H, Watanabe T, Arinaga T, Naito Y, Uchida S, Hisaka T, Toyonaga A, Kojiro M, Kinoshita H, Tsuruta O, Sata M. A case of hepatic eosinophilic granuloma, which needs distinction with metastatic liver cancer. Nippon Shokakibyo Gakkai Zasshi 2008;105:1509–1514
Rey P, Bredin C, Carrere C, Froment N, Casassus-Builhe D. Toxocariasis mimicking liver tumor. Presse Med 2005;34:1715–1716
Jackson G, Kathuria M, Abraham B, Schnadig VJ. Fine needle aspiration diagnosis of necrotizing eosinophilic abscess clinically mimicking hepatic neoplasia: a case report. Acta Cytol 2010;54:60–62
Hotez PJ. Neglected infections of poverty in the United States of America. PLoS Negl Trop Dis 2008;2:e256
Rubinsky-Elefant G, Hirata CE, Yamamoto JH, Ferreira MU. Human toxocariasis: diagnosis, worldwide seroprevalences and clinical expression of the systemic and ocular forms. Ann Trop Med Parasitol 2010;104:3–23
Kim YS, Park SJ, Kim HK, Park JM. A case of eosinophilic abscess mistaken for metastasis due to FDG uptake in PET-CT. Korean J Gastroenterol 2009;54:349–354
Choi JI, Lee JM, Kim SH, Lee JY, Lee MW, Han CJ, Han JK, Choi BI. Differentiating focal eosinophilic necrosis of the liver from hepatic metastases using unenhanced and portal venous phase computed tomographic imagings: results of univariate and multivariate statistical analyses. J Comput Assist Tomogr 2009;33:705–709
Weller PF. Eosinophilia and eosinophil related disorders. In Adkinson NF, editor. Middleton’s allergy principles and practice. 6th edn. Philadelphia: Mosby; 2003. p. 1117
Lowe D, Jorizzo J, Hutt MS. Tumour-associated eosinophilia: a review. J Clin Pathol 1981;34:1343–1348
Hong SW, Cho MY, Park C. Expression of eosinophil chemotactic factors in stomach cancer. Yonsei Med J 1999;40:131–136
Lee MK, Hong SJ, Kim HR. Seroprevalence of tissue invading parasitic infections diagnosed by ELISA in Korea. J Korean Med Sci 2010;25:1272–1276
Chusid MJ, Dale DC, West BC, Wolff SM. The hypereosinophilic syndrome: analysis of fourteen cases with review of the literature. Medicine (Baltimore) 1975;54:1–27
Kwon NH, Oh MJ, Lee SP, Lee BJ, Choi DC. The prevalence and diagnostic value of toxocariasis in unknown eosinophilia. Ann Hematol 2006;85:233–238
Yoon YS, Lee CH, Kang YA, Kwon SY, Yoon HI, Lee JH, Lee CT. Impact of toxocariasis in patients with unexplained patchy pulmonary infiltrate in Korea. J Korean Med Sci 2009;24:40–45
Acknowledgements
This work was supported by a grant of the Korea Health 21 R&D Project (AO30001) from the Ministry of Health and Welfare, Republic of Korea, and by a grant from Seoul National University Hospital (04-2008-0400).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kwon, JW., Kim, TW., Kim, KM. et al. Clinical features of clinically diagnosed eosinophilic liver abscesses. Hepatol Int 5, 949–954 (2011). https://doi.org/10.1007/s12072-011-9272-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-011-9272-0