Abstract
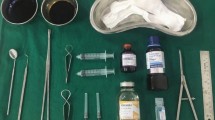
The aim of this study was to assess the efficacy of 10% dextrose prolotherapy in the management of temporomandibular joint disorder. Thirty patients aged between 18 and 62 years, diagnosed with Temporomandibular Disorders (TMDs) persisting for more than six months and unresponsive to other conservative treatments, were enrolled in the study. Over four subsequent visits, spaced six weeks apart, each patient received injections of 3 ml of 10% dextrose solution into the temporomandibular joint space. Parameters assessed included pain levels, frequency of luxations/dislocations, episodes of locking per month, maximal mouth opening, and clicking, evaluated every six weeks for a duration of three months. All patients exhibited improvements in Temporomandibular Disorders (TMDs), manifested as reduced pain, clicking sounds, locking episodes, and increased maximal mouth opening, following prolotherapy treatment. These improvements were found to be statistically significant (p-value < 0.05). Dextrose prolotherapy is a treatment method with broad applications and should be considered prior to resorting to long-term pharmacotherapy or surgical interventions. The use of 10% dextrose prolotherapy presents a promising treatment modality for temporomandibular joint disorders, as evidenced by its therapeutic benefits.



Similar content being viewed by others
References
Gedney E (1951) Disk syndrome. Osteopath Prof 18(12):11-15-38–46
Dorman T (1991) Treatment for spinal pain arising in ligaments using prolotherapy: a retrospective study. J Orthop Med 13:13–19
Klein RG, Bjorn CE, DeLong B et al (1993) A randomized double blind trial of dextrose-glycerine-phenol injections for chronic low back pain. J Spinal Disord 6:23
Schultz LW (1937) A treatment of subluxation of the temporomandibular joint. JAMA 109:1032
Reeves KD (2000) Prolotherapy: basic science, clinical studies, and technique. In: Lennard TA (ed) Pain procedures in clinical practice, 2nd edn. Hanley and Belfus, Philadelphia, pp 172–190
Hauser R, Hauser M, Blakemore K (2007) Dextrose prolotherapy and pain of chronic TMJ dysfunction. Pract Pain Manag 7:49
Banks A (1991) A rationale for prolotherapy. J Orthop Med 13:54
Oh S, Ettema AM, Zhao C et al (2008) Dextrose-induced subsynovial connective tissue fibrosis n the rabbit carpal tunnel: A potential model to study carpal tunnel syndrome? Hand 3:34–40
Nitzan DW, Dolwick MF, Martinez GA (1991) Temporo- mandibular joint arthrocentesis: a simplified treatment for severe, limited mouth opening. J Oral Maxillofac Surg 49(11):1163–1170
Izumi K, Feinberg SE, Iida A, Yoshizawa M (2003) Intraoral grafting of an ex vivo produced oral mucosa equivalent: a preliminary report. Int J Oral Maxillofac Surg 32:188–197
Okeson JP (2008) Management of temporomandibular disorders and occlusion, 6th edn. CV Mosby, St. Louis
Okeson JP (1995) Bell ‘s orofacial pains, 5th edn. Quintessence Publishing Co, Chicago, pp 208–210
Fricton J (2007) Myogenous temporomandibular disorders: Diagnostic and management considerations. Dent Clin North Am 51:61–83
Wright EF (2005) Manual of temporomandibular disorders. Blackwell, Ames
de Leeuw R, Post MVA (2008) TMD patients endorse more general symptoms than nontrauma TMD patients. J Evid Based Dent Pract 8(4):246–248
Bonjardim LR, Lopes-Filho RJ, Amado G, Albuquerque Junior RLC, Gonçalves SRJ (2009) Association between symptoms of temporomandibular disorders and gender, morphological occlusion, and psychological factors in a group of university students. Indian J Dent Res 20:190–194
Macfarlane TV, Kenealy P, Kingdon HA, Mohlin BO, Pilley JR, Richmond S et al (2009) Twenty-year cohort study of health gain from orthodontic treatment: temporomandibular disorders. Am J Orthod Dentofacial Orthop 135:692.e1-e8
Marklund S, Wänman A (2010) Risk factors associated with incidence and persistence of signs and symptoms of temporomandibular disorders. Acta Odontol Scand 68:289–299
Refai H, Altahhan O, Elsharkawy R (2011) The efficacy of dextrose prolotherapy for temporomandibular joint hypermobility: a preliminary prospective, randomized, double-blind, placebo- controlled clinical trial. J Oral Maxillofac Surg 69(9):2962–2970
Monteiro DR, Zuim PRJ, Pesqueira AA, Ribeiro PP, Garcia AR (2011) Relationship between anxiety and chronic orofacial pain of temporomandibular disorder in a group of university students. J Prosthodont Res 55:154–158
Abubaker AO, Raslan WF, Sotereanos GC (1993) Estrogen and progesterone receptors in temporomandibular joint discs of symptomatic and asymptomatic persons: a preliminary study. J Oral Maxillofac Surg 51:1096–1100
Hackett G, Henderson D (1955) Joint stabilization: an experimental histologic study with comments on the clinical application in ligament proliferation. Am J Surg 89:968–973
Hakala RV, Ledermann KM (2010) The use of prolotherapy for temporomandibular joint dysfunction. J Prolother 2(3):439–446
Alsehimy M, Ayman Al-Dharrab A, Jamal B (2016) The use of dextrose prolotherapy for myofascial pain dysfunction syndrome: a double-blind placebo-controlled study. Egypt J Oral Maxillofacl Surg 7:75–80
Majumdar SK, Krishna S, Chatterjee A, Chakraborty R, Ansari N (2016) Single injection technique prolotherapy for hypermobility disorders of TMJ using 25% dextrose: a clinical study. J Maxillofac Oral Surg 16:226–230
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Singh, S., Sharma, N.K., Jaiswara, C. et al. Evaluation of Efficacy of 10% Dextrose Prolotherapy in Management of Temporomandibular Joint Disorders: A Prospective Study. Indian J Otolaryngol Head Neck Surg (2024). https://doi.org/10.1007/s12070-024-04726-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12070-024-04726-4