Abstract
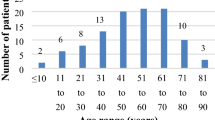
To study the age & sex distribution, etiology, formulate most suitable management protocol and evaluate the results of our study and compare our data with similarly published studies to look for any changing trends. All the patients presenting with epistaxis who came to our institute, a tertiary care centre of central India were included in the study. The diagnostic confirmation was done with clinical along with radiological and endoscopic evaluation. Various parameters categorized accordingly. Total 304 patients were included in the study. Epistaxis was found prevalent in 1st to 3rd decade, more common in males, frequently seen in cold, anterior epistaxis more common. Trauma and infection being more common in children and young adults, whereas hypertension in the elderly. Although the treatment of epistaxis hasn’t change much, we found cauterization to be a very efficient and effective method to control epistaxis and required less hospitalization.

Similar content being viewed by others
References
The American Heritage (2002) Stedman’s medical dictionary. Houghton Miffin Company, Boston
Mcgarry GW (2008) Epistaxis. In: Gleeson M (ed) Scott-Brown’s otorhinolaryngology, head and neck surgery, vol 2, 7th edn. chapt 126 H. CRC Press, London, pp 1603–1608
Simmen DB, Jones NS, Cummings CW, Flint PW, Harker LA (2005) Epistaxis. Otolaryngol Head Neck Surg 5:682–693
Petruson B (1979) Epistaxis in childhood. Rhinology 17:83–90
Hussain G, Iqbal M, Shah SA, Said M, Sanaulla KSA et al (2006) Evaluation of aetiology and efficacy of management protocol of epistaxis. J Ayyub Med College Abbottabad 18(4):62–65
Juselius H (1974) Epistaxis: a clinical study of 1724 patients. J Laryngol Otol 88:317–327
Jain L, Qureshi S, Maurya A, Jadia S, Mrityunjay S (2017) Hand dominance and blood group: association in Epistaxis. Indian J Otolaryngol Head Neck Surg 69(1):121–124
Emanuel JM (1998) Epistaxis. Otolaryngol Head Neck Surg 2:852–865
Hara J (1962) Severe Epistaxis. Arch Otolaryngol 7S:258
Razdan U, Zada R, Chaturvedi VN (1999) Epistaxis: study of aetiology, site and side of bleeding. Indian J Med Sci 53(12):1545–1552
Razdan U, Raizada RM (2004) Efficacy of conservative treatment modalities used in epistaxis. Indian J Otolaryngol Head Neck Surg 56(1):20–23
Pollice PA, Yude MG (1997) A retrospective review of 249 hospitalised patients with epistaxis. AJO Head Neck Surg 1997:49–53
Funding
This study was not funded by anyone.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Sandeep Sharma declares that he has no conflict of interest. Sadat Qureshi declares that he has no conflict of interest. Shalini Jadia declares that she has no conflict of interest. Lavi Ukawat declares that she has no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sharma, S., Qureshi, S., Jadia, S. et al. Epistaxis: Revisited. Indian J Otolaryngol Head Neck Surg 72, 480–483 (2020). https://doi.org/10.1007/s12070-020-01930-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-020-01930-w