Abstract
Autosomal dominant diseases typically have an age-related onset. Here, I focus on genetic prion disease (gPrD), caused by various mutations in the PRNP gene. While gPrD typically occurs at or after middle age, there can be considerable variability in the specific age of onset. This variability can occur among patients with the same PRNP mutation; in some cases, these differences occur not only between families but even within the same family. It is not known why gPrD onset is typically delayed for decades when the causative mutation is present from birth. Mouse models of gPrD manifest disease; however, unlike human gPrD, which typically takes decades to manifest, mouse models exhibit disease within months. Therefore, the time to onset of prion disease is proportional to species lifespan; however, it is not known why this is the case. I hypothesize that the initiation of gPrD is strongly influenced by the process of aging; therefore, disease onset is related to proportional functional age (e.g., mice vs. humans). I propose approaches to test this hypothesis and discuss its significance with respect to delaying prion disease through suppression of aging.

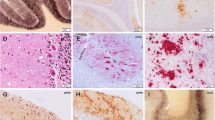
Similar content being viewed by others
Data availability
No materials were used for this manuscript, and no experiments were performed to produce this manuscript.
Code availability
No code has been utilized or described in this article.
References
Asante EA, Gowland I, Grimshaw A et al (2009) Absence of spontaneous disease and comparative prion susceptibility of transgenic mice expressing mutant human prion proteins. J Gen Virol 90(Pt 3):546–558. https://doi.org/10.1099/vir.0.007930-0
Blagosklonny MV (2019) Rapamycin for longevity: opinion article. Aging (Albany NY) 11:8048–67. https://doi.org/10.18632/aging.102355
Brown P, Brandel JP, Sato T et al (2012) Iatrogenic creutzfeldt-jakob disease. Final Asses Emerg Infect Dis 8:901–907. https://doi.org/10.3201/eid1806.120116
Cheikhi A, Barchowsky A, Sahu A et al (2019) Klotho: an elephant in aging research. J Gerontol A Biol Sci Med Sci 74:1031–1042. https://doi.org/10.1093/gerona/glz061
Crutcher E, Pal R, Naini F et al (2019) mTOR and autophagy pathways are dysregulated in murine and human models of Schaaf-Yang syndrome. Sci Rep 9:15935. https://doi.org/10.1038/s41598-019-52287-2
Der G, Batty GD, Benzeval M et al (2012) Is telomere length a biomarker for aging: cross-sectional evidence from the west of Scotland? PLoS One 7:e45166. https://doi.org/10.1371/journal.pone.0045166
Farshim PP, Gillian P, Bates GP (2018) Mouse models of huntington’s disease. Methods Mol Biol 1780:97–120. https://doi.org/10.1007/978-1-4939-7825-0_6
Friedman-Levi Y, Meiner Z, Canello T et al (2011) Fatal prion disease in a mouse model of genetic E200K Creutzfeldt-Jakob disease. PLoS Pathog 7(11):e1002350. https://doi.org/10.1371/journal.ppat.1006294
Gambetti P, Kong Q, Zou W, Parchi P, Chen SG (2003) Sporadic and familial CJD: classification and characterisation. Br Med Bull 66:213–239. https://doi.org/10.1093/bmb/66.1.213
Geschwind MD (2015) Prion diseases. Continuum (Minneap Minn) 21(6):1612–1638. https://doi.org/10.1212/CON.0000000000000251
Hagan C. (2017) When are mice considered old? Jackson Laboratory website, November 2017, accessed 3/2/20, https://www.jax.org/news-and-insights/jax-blog/2017/november/when-are-mice-considered-old
Harrison DE, Strong R, Sharp ZD et al (2009) Rapamycin fed late in life extends lifespan in genetically heterogeneous mice. Nature 460:392–395. https://doi.org/10.1038/nature08221
Heras-Sandoval D, Pérez-Rojas JM, Pedraza-Chaverri J (2020) Novel compounds for the modulation of mTOR and autophagy to treat neurodegenerative diseases. Cell Singla 65:109442. https://doi.org/10.1016/j.cellsig.2019.109442
Jackson WS, Krost C (2014) Peculiarities of prion diseases. PLoS Pathog 10:e1004451. https://doi.org/10.1371/journal.ppat.1004451
Jackson WS, Borkowski AW, Watson NE et al (2013) Profoundly different prion diseases in knock-in mice carrying single PrP codon substitutions associated with human diseases. Proc Natl Acad Sci USA 110:14759–14764. https://doi.org/10.1073/pnas.1312006110
Kim MO, Takada LT, Wong K, Forner SA, Geschwind MD (2018) Genetic PrP prion diseases. Cold Spring Harb Perspect Biol 10(5):a033134. https://doi.org/10.1101/cshperspect.a033134.Review
Kovács GG, Puopolo M, Ladogana A et al (2006) Genetic prion disease: the EUROCJD experience. Hum Genet 118:166–174. https://doi.org/10.1007/s00439-005-0020-1
Lamming DW, Ye L, Sabatini DM, Baur JA (2013) Rapalogs and mTOR inhibitors as anti-aging therapeutics. J Clin Invest 123:980–989. https://doi.org/10.1172/JCI64099
Liu H, Fergusson MM, Castilho RM et al (2007) Augmented Wnt signaling in a mammalian model of accelerated aging. Science 317:803–806. https://doi.org/10.1126/science.1143578
Liu Y, Pan J, Pan X et al (2019) Klotho-mediated targeting of CCL2 suppresses the induction of colorectal cancer progression by stromal cell senescent microenvironments. Mol Oncol 13:2460–2475. https://doi.org/10.1002/1878-0261.12577
Marín-Moreno A, Espinosa JC, Torres JM (2020) Transgenic mouse models for the study of prion diseases. Prog Mol Biol Transl Sci 175:147–177. https://doi.org/10.1016/bs.pmbts.2020.08.007
Minikel EV, Vallabh SM, Lek M et al (2016) Quantifying prion disease penetrance using large population control cohorts. Sci Transl Med 8(322):322ra9. https://doi.org/10.1126/scitranslmed.aad5169
Minikel EV, Vallabh SM, Orseth MC et al (2019) Age at onset in genetic prion disease and the design of preventive clinical trials. Neurology 93:e125–e134. https://doi.org/10.1212/WNL.0000000000007745
Minikel EV, Zhao HT, Le J et al (2020) Prion protein lowering is a disease-modifying therapy across prion disease stages, strains, and endpoints. Nucleic Acids Res 48:10615–10631. https://doi.org/10.1093/nar/gkaa616
Nitsan Z, Cohen OS, Chapman J et al (2020) Familial Creutzfeldt-Jakob disease homozygous to the E200K mutation: clinical characteristics and disease course. J Neurol 267:2455–2458. https://doi.org/10.1007/s00415-020-09826-z
Prokhorova TA, Boksha IS, Savushkina OK, Tereshkina EB, Burbaeva GS (2019) α-Klotho protein in neurodegenerative and mental diseases. Zh Nevrol Psikhiatr Im S Korsakova 119:80–88. https://doi.org/10.17116/jnevro201911901180
Reita D, Bour C, Benbrika R et al (2019) Synergistic anti-tumor effect of mTOR inhibitors with irinotecan on colon cancer cells. Cancers (basel) 11:1581. https://doi.org/10.3390/cancers11101581
Robanus-Maandag EC, Koelink PJ, Breukel C et al (2010) A new conditional Apc-mutant mouse model for colorectal cancer. Carcinogenesis 31:946–952. https://doi.org/10.1093/carcin/bgq046
Rubinstein TA, Shahmoon S, Zigmond E et al (2019) Klotho suppresses colorectal cancer through modulation of the unfolded protein response. Oncogene 38:794–807. https://doi.org/10.1038/s41388-018-0489-4
Rudge P, Jaunmuktane Z, Adlard P et al (2015) Iatrogenic CJD due to pituitary-derived growth hormone with genetically determined incubation times of up to 40 years. Brain 138(Pt 11):3386–3399. https://doi.org/10.1093/brain/awv235
Semba RD, Cappola AR, Sun K et al (2011) Plasma klotho and mortality risk in older community-dwelling adults. J Gerontol A Biol Sci Med Sci 66:794–800. https://doi.org/10.1093/gerona/glr058
Simon ES, Kahana E, Chapman J et al (2000) Creuzfeldt-Jakob disease profile in patients homozygous for the PRNP E200K mutation. Ann Neurol 47:257–260. https://doi.org/10.1002/1531-8249(200002)47:2%3c257::AID-ANA20%3e3.0.CO;2-U
Synofzik M, Bauer P, Schöls L (2009) Prion mutation D178N with highly variable disease onset and phenotype. J Neurol Neurosurg Psychiatry 80:345–346. https://doi.org/10.1136/jnnp.2008.149922
Vallabh SM, Zou D, Pitstick R et al (2023) Therapeutic trial of anle 138b in mouse models of genetic prion disease. J Virology. https://doi.org/10.1128/jvi.01672-22
Watts JC, Giles K, Bourkas MEC et al (2016) Towards authentic transgenic mouse models of heritable PrP prion diseases. Acta Neuropathol 132:593–610. https://doi.org/10.1007/s00401-016-1585-6
Weissmann C, Enari M, Klöhn P-C, Rossi D, Flechsig E (2002) Transmission of prions. J Infect Dis 186(Supplement 2):S157–S165. https://doi.org/10.1086/344575
Xie B, Nie S, Hu G et al (2019) The involvement of NF-κB/Klotho signaling in colorectal cancer cell survival and invasion. Pathol Oncol Res 25:1553–1565. https://doi.org/10.1007/s12253-018-0493-6
Acknowledgments
MB is supported by the Geisinger Commonwealth School of Medicine. Dr. Darina Lazarova is thanked for the critical reading of the manuscript.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
This manuscript is entirely the work of MB.
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical approval
Not required.
Consent for publication
MB gives my consent for the information detailed in this publication to be published in the journal Theory in Biosciences.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bordonaro, M. Hypothesis: functional age and onset of autosomal dominant genetic prion disease. Theory Biosci. 142, 143–150 (2023). https://doi.org/10.1007/s12064-023-00389-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12064-023-00389-x