Abstract
Background
We report our experience of 3 years in the management of tracheobronchial foreign bodies in our department of cardiothoracic surgery.
Materials and methods
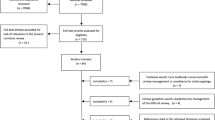
This is a retrospective study of confirmed tracheobronchial Foreign Body (FB) between May 2006 and October 2009. Patients with severe respiratory distress and pneumonia were electively ventilated for 48 h before any intervention. Flexible fibreoptic bronchoscopy was performed for the initial diagnosis and assessment of tracheobronchial FB. Once confirmed removal was done by rigid bronchoscopy. Patient was kept in intensive surgical unit for 2–4 h with chest X-ray repeated at arrival and after 24 h. Majority of patients were discharged the next day with advice to come for follow up after 1 week. Chest X ray was done at 1st follow up depending on which further follow up treatment course was planned.
Results
The study consists of 50 patients. The most common age group was 7 months to 18 months. There were 34 males and 16 females. The most common symptom was cough and wheezing which was present in all the patients. 1 patient was in severe respiratory distress. This child was electively ventilated for 48 h before intervention.Obstructive emphysema was the most common radiological finding. 42 patients had foreign body lodged in Right Main Bronchus (RMB). Two patients required thoracotomy for removal of foreign body.The majority of foreign bodies in our cases were organic like ground nut seeds, chana and imli seed. Follow up was uneventful.
Conclusions
In conclusion, diagnosis of tracheobronchial FB depends on a high index of suspicion. Flexible fibreoptic bronchoscopy is the diagnostic investigation of choice for initial evaluation and rigid bronchoscopy is the standard for removal of foreign body.Thoracotomy may be life saving in endoscopically non retrievable foreign bodies. Once identified, FB should be removed as early as possible but one should not rush overlooking the general condition of the patient.
Similar content being viewed by others
References
Killian G. Meeting of the Society of Physicians of Freiburg, Freiburg. 1897, Dec 17. Munchen Med Wschr. 1898;45:378.
Zavala DC, Rhodes ML. Experimental removal of foreign bodies by fibreoptic bronchoscopy. Am Rev Respir Dis. 1974;110:357–60.
Zavala DC, Rhodes ML. Foreign body removal: a new role for the fibreoptic bronchoscope. Ann Otol Rhinol Laryngol. 1975;84:650–6.
Ouoba K, Diara C, Dao MO, Ouedraogo I, Sanou I, Cisse R. Laryngo-tracheo-bronchial foreign bodies in children at the University Hospital center of Ouagadougou (analysis of 96 cases). Med Trop (Mars). 2002;62:611–4.
Freiman MA, McMurray JS. Unique presentation of a bronchial foreign body in an asymptomatic child. Ann Otol Rhinol Laryngol. 2001;110:495–7.
Tsolov Ts, Melnicharov M, Perinovska P, Krutilin F. Foreign bodies in the upper airways of children-problems relating to diagnosis and treatment. Khirurgiia (Sofiia). 1999;55:33–4.
Lan RS. Non-asphyxiating tracheobronchial foreign bodies in adults. Eur Respir J. 1994;7:510–4.
Limper AH, Prakash UB. Tracheobronchial foreign bodies in adults. Ann Intern Med. 1990;112:604–9.
Chiu CY, Wong KS, Lai SH, Hsia SH, Wu CT. Factors predicting early diagnosis of foreign body aspiration in children. Pediatr Emerg Care. 2005;21:161–4.
Martinot A, Deschildre A, Brichet A, Leclerc F. Indications of bronchial endoscopy in suspected tracheo-bronchial foreign body in children. Rev Mal Respir. 1999;16:673–8.
Karakoc F, Karadag B, Akbenlioglu C, et al. Foreign body aspiration: what is the outcome? Pediatr Pulmonol. 2002;34:30–6.
Mu LC, Sun DQ, He P. Radiological diagnosis of aspirated foreign bodies in children: review of 343 cases. J Laryngol Otol. 1990;104:778–82.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dixit, S., Agarwal, R., Kumar, N. et al. Management of tracheobronchial foreign bodies-experience of cardiothoracic department of cardiology institute. Indian J Thorac Cardiovasc Surg 27, 33–35 (2011). https://doi.org/10.1007/s12055-010-0071-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12055-010-0071-3