Abstract
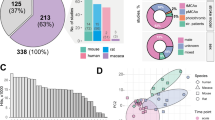
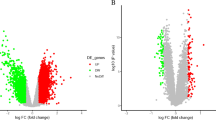
The genetic transcription profile of brain ischemic and reperfusion injury remains elusive. To address this, we used an integrative analysis approach including differentially expressed gene (DEG) analysis, weighted-gene co-expression network analysis (WGCNA), and pathway and biological process analysis to analyze data from the microarray studies of nine mice and five rats after middle cerebral artery occlusion (MCAO) and six primary cell transcriptional datasets in the Gene Expression Omnibus (GEO). (1) We identified 58 upregulated DEGs with more than 2-fold increase, and adj. p < 0.05 in mouse datasets. Among them, Atf3, Timp1, Cd14, Lgals3, Hmox1, Ccl2, Emp1, Ch25h, Hspb1, Adamts1, Cd44, Icam1, Anxa2, Rgs1, and Vim showed significant increases in both mouse and rat datasets. (2) Ischemic treatment and reperfusion time were the main confounding factors in gene profile changes, while sampling site and ischemic time were not. (3) WGCNA identified a reperfusion-time irrelevant and inflammation-related module and a reperfusion-time relevant and thrombo-inflammation related module. Astrocytes and microglia were the main contributors of the gene changes in these two modules. (4) Forty-four module core hub genes were identified. We validated the expression of unreported stroke-associated core hubs or human stroke-associated core hubs. Zfp36 mRNA was upregulated in permanent MCAO; Rhoj, Nfkbiz, Ms4a6d, Serpina3n, Adamts-1, Lgals3, and Spp1 mRNAs were upregulated in both transient MCAO and permanent MCAO; and NFKBIZ, ZFP3636, and MAFF proteins, unreported core hubs implicated in negative regulation of inflammation, were upregulated in permanent MCAO, but not in transient MCAO. Collectively, these results expand our knowledge of the genetic profile involved in brain ischemia and reperfusion, highlighting the crucial role of inflammatory disequilibrium in brain ischemia.





Similar content being viewed by others
Abbreviations
- DEGs:
-
differentially expressed genes
- DE:
-
differential expression
- WGCNA:
-
weighted-gene co-expression network analysis
- MCAO:
-
middle cerebral artery occlusion
- GEO:
-
Gene Expression Omnibus
- DS1:
-
training datasets
- DS2:
-
validation datasets
- AD:
-
Alzheimer’s disease
- PPI:
-
protein-protein interaction
- GWAS:
-
genome-wide association studies
- SNP:
-
single nucleotide polymorphism
- MAPK:
-
mitogen-activated protein kinase
- LAA:
-
large artery atherosclerosis
- BBB:
-
blood-brain barrier
- OGD:
-
oxygen-glucose deprivation
- GSEA:
-
gene set enrichment analysis
- GSVA:
-
gene set variation analysis
- CCA:
-
common carotid artery
- ICA:
-
internal carotid artery
- ECA:
-
external carotid artery
References
Global Burden of Disease Study C (2015) Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 386(9995):743–800. https://doi.org/10.1016/S0140-6736(15)60692-4
Collaborators GBDLRoS, Feigin VL, Nguyen G, Cercy K, Johnson CO, Alam T, Parmar PG, Abajobir AA, et al (2018) Global, regional, and country-specific lifetime risks of stroke, 1990 and 2016. N Engl J Med 379(25):2429–2437. https://doi.org/10.1056/NEJMoa1804492
Lees KR, Bluhmki E, von Kummer R, Brott TG, Toni D, Grotta JC, Albers GW, Kaste M et al (2010) Time to treatment with intravenous alteplase and outcome in stroke: an updated pooled analysis of ECASS, ATLANTIS, NINDS, and EPITHET trials. Lancet 375(9727):1695–1703. https://doi.org/10.1016/S0140-6736(10)60491-6
Mizuma A, You JS, Yenari MA (2018) Targeting reperfusion injury in the age of mechanical thrombectomy. Stroke 49(7):1796–1802. https://doi.org/10.1161/STROKEAHA.117.017286
Petrovic-Djergovic D, Goonewardena SN, Pinsky DJ (2016) Inflammatory disequilibrium in stroke. Circ Res 119(1):142–158. https://doi.org/10.1161/CIRCRESAHA.116.308022
McBride DW, Zhang JH (2017) Precision stroke animal models: the permanent MCAO model should be the primary model, not transient MCAO. Transl Stroke Res https://doi.org/10.1007/s12975-017-0554-2
Ramasamy A, Mondry A, Holmes CC, Altman DG (2008) Key issues in conducting a meta-analysis of gene expression microarray datasets. PLoS Med 5(9):e184. https://doi.org/10.1371/journal.pmed.0050184
Malik R, Chauhan G, Traylor M, Sargurupremraj M, Okada Y, Mishra A, Rutten-Jacobs L, Giese AK et al (2018) Multiancestry genome-wide association study of 520,000 subjects identifies 32 loci associated with stroke and stroke subtypes. Nature Gen 50(4):524–537. https://doi.org/10.1038/s41588-018-0058-3
Network NSG, International Stroke Genetics C (2016) Loci associated with ischaemic stroke and its subtypes (SiGN): a genome-wide association study. Lancet Neurol 15(2):174–184. https://doi.org/10.1016/S1474-4422(15)00338-5
Khasanova LT, Stakhovskaya LV, Koltsova EA, Shamalov NA (2019) Genetic characteristics of stroke. Zhurnal nevrologii i psikhiatrii imeni SS Korsakova 119(12. Vyp. 2):65–72. https://doi.org/10.17116/jnevro201911912265
Pluta R, Ulamek-Koziol M, Januszewski S, Czuczwar SJ (2020) Shared genomic and proteomic contribution of amyloid and tau protein characteristic of Alzheimer’s disease to brain ischemia. Int J Mol Sci 21(9). https://doi.org/10.3390/ijms21093186
Cahoy JD, Emery B, Kaushal A, Foo LC, Zamanian JL, Christopherson KS, Xing Y, Lubischer JL et al (2008) A transcriptome database for astrocytes, neurons, and oligodendrocytes: a new resource for understanding brain development and function. J Neurosci 28(1):264–278. https://doi.org/10.1523/JNEUROSCI.4178-07.2008
Albright AV, Gonzalez-Scarano F (2004) Microarray analysis of activated mixed glial (microglia) and monocyte-derived macrophage gene expression. J Neuroimmunol 157(1-2):27–38. https://doi.org/10.1016/j.jneuroim.2004.09.007
Stoll G, Nieswandt B (2019) Thrombo-inflammation in acute ischaemic stroke - implications for treatment. Nat Rev Neurol 15(8):473–481. https://doi.org/10.1038/s41582-019-0221-1
Nieswandt B, Watson SP (2003) Platelet-collagen interaction: is GPVI the central receptor? Blood 102(2):449–461. https://doi.org/10.1182/blood-2002-12-3882
Aslam MS, Aslam MS, Aslam KS, Iqbal A, Yuan L (2022) Therapeutical significance of serpina3n subsequent cerebral ischemia via cytotoxic granzyme B inactivation. Biomed Res Int 2022:1557010. https://doi.org/10.1155/2022/1557010
Zhang Y, Chen Q, Chen D, Zhao W, Wang H, Yang M, Xiang Z, Yuan H (2022) SerpinA3N attenuates ischemic stroke injury by reducing apoptosis and neuroinflammation. CNS Neurosci Ther 28(4):566–579. https://doi.org/10.1111/cns.13776
Lyu C, Chen Y, Zhu M, Jin X, Liu P, Zheng Z, Li C, Zhu F, et al (2015) Association of ADAMTS-1 gene polymorphisms with ischemic stroke caused by large artery atherosclerosis. Zhonghua yi xue yi chuan xue za zhi = Zhonghua yixue yichuanxue zazhi = Chin J Med Gen 32(6):844–848. https://doi.org/10.3760/cma.j.issn.1003-9406.2015.06.021
Pelisek J, Deutsch L, Ansel A, Pongratz J, Stadlbauer T, Gebhard H, Matevossian E, Eckstein HH (2017) Expression of a metalloproteinase family of ADAMTS in human vulnerable carotid lesions. J Cardiovasc Med 18(1):10–18. https://doi.org/10.2459/JCM.0000000000000254
Wang L, Zhou C, Wang Z, Liu J, Jing Z, Zhang Z, Wang Y (2011) Dynamic variation of genes profiles and pathways in the hippocampus of ischemic mice: a genomic study. Brain Res 1372:13–21. https://doi.org/10.1016/j.brainres.2010.11.099
Rahimian R, Beland LC, Kriz J (2018) Galectin-3: mediator of microglia responses in injured brain. Drug Discov Today Technol 23(2):375–381. https://doi.org/10.1016/j.drudis.2017.11.004
Shirakawa K, Endo J, Kataoka M, Katsumata Y, Yoshida N, Yamamoto T, Isobe S, Moriyama H, et al (2018) IL (Interleukin)-10-STAT3-galectin-3 axis is essential for osteopontin-producing reparative macrophage polarization after myocardial infarction. Circulation 138(18):2021–2035. https://doi.org/10.1161/CIRCULATIONAHA.118.035047
Venkatraman A, Hardas S, Patel N, Singh Bajaj N, Arora G, Arora P (2018) Galectin-3: an emerging biomarker in stroke and cerebrovascular diseases. Eur J Neurol 25(2):238–246. https://doi.org/10.1111/ene.13496
Li Y, Dammer EB, Zhang-Brotzge X, Chen S, Duong DM, Seyfried NT, Kuan CY, Sun YY (2017) Osteopontin is a blood biomarker for microglial activation and brain injury in experimental hypoxic-ischemic encephalopathy. eNeuro 4(1). https://doi.org/10.1523/ENEURO.0253-16.2016
Son YO, Kim HE, Choi WS, Chun CH, Chun JS (2019) RNA-binding protein ZFP36L1 regulates osteoarthritis by modulating members of the heat shock protein 70 family. Nat Commun 10(1):77. https://doi.org/10.1038/s41467-018-08035-7
Galloway A, Saveliev A, Lukasiak S, Hodson DJ, Bolland D, Balmanno K, Ahlfors H, Monzon-Casanova E, Mannurita SC, et al (2016) RNA-binding proteins ZFP36L1 and ZFP36L2 promote cell quiescence. Science 352(6284):453–459. https://doi.org/10.1126/science.aad5978
Makita S, Takatori H, Nakajima H (2021) Post-transcriptional regulation of immune responses and inflammatory diseases by RNA-binding ZFP36 family proteins. Front Immunol 12:711633. https://doi.org/10.3389/fimmu.2021.711633
Jing Q, Huang S, Guth S, Zarubin T, Motoyama A, Chen J, Di Padova F, Lin SC, et al (2005) Involvement of microRNA in AU-rich element-mediated mRNA instability. Cell 120(5):623–634. https://doi.org/10.1016/j.cell.2004.12.038
Tiedje C, Diaz-Munoz MD, Trulley P, Ahlfors H, Laass K, Blackshear PJ, Turner M, Gaestel M (2016) The RNA-binding protein TTP is a global post-transcriptional regulator of feedback control in inflammation. Nucleic Acids Res 44(15):7418–7440. https://doi.org/10.1093/nar/gkw474
Kang JG, Amar MJ, Remaley AT, Kwon J, Blackshear PJ, Wang PY, Hwang PM (2011) Zinc finger protein tristetraprolin interacts with CCL3 mRNA and regulates tissue inflammation. J Immunol. 187(5):2696–2701. https://doi.org/10.4049/jimmunol.1101149
Liang J, Lei T, Song Y, Yanes N, Qi Y, Fu M (2009) RNA-destabilizing factor tristetraprolin negatively regulates NF-kappaB signaling. J Biol Chem 284(43):29383–29390. https://doi.org/10.1074/jbc.M109.024745
Guo H, Jiang Y, Gu Z, Ren L, Zhu C, Yu S, Wei R (2022) ZFP36 protects against oxygen-glucose deprivation/reoxygenation-induced mitochondrial fragmentation and neuronal apoptosis through inhibiting NOX4-DRP1 pathway. Brain Res Bull 179:57–67. https://doi.org/10.1016/j.brainresbull.2021.12.003
Muta T, Yamazaki S, Eto A, Motoyama M, Takeshige K (2003) IkappaB-zeta, a new anti-inflammatory nuclear protein induced by lipopolysaccharide, is a negative regulator for nuclear factor-kappaB. J Endotoxin Res 9(3):187–191. https://doi.org/10.1179/096805103125001612
Ishiguro-Oonuma T, Ochiai K, Hashizume K, Morimatsu M (2015) The role of IFN-gamma in regulating Nfkbiz expression in epidermal keratinocytes. Biomedical Res 36(2):103–107. https://doi.org/10.2220/biomedres.36.103
Slowikowski K, Nguyen HN, Noss EH, Simmons DP, Mizoguchi F, Watts GFM, Gurish MF, Brenner MB, et al (2020) CUX1 and IkappaBzeta (NFKBIZ) mediate the synergistic inflammatory response to TNF and IL-17A in stromal fibroblasts. Proc Natl Acad Sci USA 117(10):5532–5541. https://doi.org/10.1073/pnas.1912702117
Cui Y, Wan Q (2019) NKT Cells in neurological diseases. Front Cell Neurosci 13:245. https://doi.org/10.3389/fncel.2019.00245
Miyake T, Satoh T, Kato H, Matsushita K, Kumagai Y, Vandenbon A, Tani T, Muta T, et al (2010) IkappaBzeta is essential for natural killer cell activation in response to IL-12 and IL-18. Proc Natl Acad Sci USA 107(41):17680–17685. https://doi.org/10.1073/pnas.1012977107
Katsuoka F, Yamamoto M (2016) Small Maf proteins (MafF, MafG, MafK): History, structure and function. Gene 586(2):197–205. https://doi.org/10.1016/j.gene.2016.03.058
von Scheidt M, Zhao Y, de Aguiar Vallim TQ, Che N, Wierer M, Seldin MM, Franzen O, Kurt Z et al (2021) Transcription factor MAFF (MAF basic leucine zipper transcription factor F) regulates an atherosclerosis relevant network connecting inflammation and cholesterol metabolism. Circulation 143(18):1809–1823. https://doi.org/10.1161/CIRCULATIONAHA.120.050186
Huang X, Feng Z, Jiang Y, Li J, Xiang Q, Guo S, Yang C, Fei L et al (2019) VSIG4 mediates transcriptional inhibition of Nlrp3 and Il-1beta in macrophages. Sci Adv 5(1):eaau7426. https://doi.org/10.1126/sciadv.aau7426
Henstridge CM, Hyman BT, Spires-Jones TL (2019) Beyond the neuron-cellular interactions early in Alzheimer disease pathogenesis. Nat Rev Neurosci 20(2):94–108. https://doi.org/10.1038/s41583-018-0113-1
Kunkle BW, Grenier-Boley B, Sims R, Bis JC, Damotte V, Naj AC, Boland A, Vronskaya M et al (2019) Genetic meta-analysis of diagnosed Alzheimer’s disease identifies new risk loci and implicates Abeta, tau, immunity and lipid processing. Nature Gen 51(3):414–430. https://doi.org/10.1038/s41588-019-0358-2
Zhao N, Ren Y, Yamazaki Y, Qiao W, Li F, Felton LM, Mahmoudiandehkordi S, Kueider-Paisley A et al (2020) Alzheimer’s risk factors age, APOE genotype, and sex drive distinct molecular pathways. Neuron 106(5):727–742 e726. https://doi.org/10.1016/j.neuron.2020.02.034
Deming Y, Filipello F, Cignarella F, Cantoni C, Hsu S, Mikesell R, Li Z, Del-Aguila JL et al (2019) The MS4A gene cluster is a key modulator of soluble TREM2 and Alzheimer’s disease risk. Sci Transl Med 11(505). https://doi.org/10.1126/scitranslmed.aau2291
Zhou H, Qiu Z, Gao S, Chen Q, Li S, Tan W, Liu X, Wang Z (2016) Integrated analysis of expression profile based on differentially expressed genes in middle cerebral artery occlusion animal models. Int J Mol Sci 17(5). https://doi.org/10.3390/ijms17050776
Zhou Y, Zhou B, Pache L, Chang M, Khodabakhshi AH, Tanaseichuk O, Benner C, Chanda SK (2019) Metascape provides a biologist-oriented resource for the analysis of systems-level datasets. Nat Comm 10(1):1523. https://doi.org/10.1038/s41467-019-09234-6
Hanzelmann S, Castelo R, Guinney J (2013) GSVA: gene set variation analysis for microarray and RNA-seq data. BMC Bioinformatics 14:7. https://doi.org/10.1186/1471-2105-14-7
Smith HK, Russell JM, Granger DN, Gavins FN (2015) Critical differences between two classical surgical approaches for middle cerebral artery occlusion-induced stroke in mice. J Neurosci Methods 249:99–105. https://doi.org/10.1016/j.jneumeth.2015.04.008
Guo P, Jin Z, Wu H, Li X, Ke J, Zhang Z, Zhao Q (2019) Effects of irisin on the dysfunction of blood-brain barrier in rats after focal cerebral ischemia/reperfusion. Brain Behav 9(10):e01425. https://doi.org/10.1002/brb3.1425
Lv W, Deng B, Duan W, Li Y, Song X, Ji Y, Li Z, Liu Y, et al (2019) FGF9 alters the Wallerian degeneration process by inhibiting Schwann cell transformation and accelerating macrophage infiltration. Brain Res Bull 152:285–296. https://doi.org/10.1016/j.brainresbull.2019.06.011
Acknowledgements
We thank LetPub (www.letpub.com) for its linguistic assistance during the preparation of this manuscript.
Availability of Data and Materials
The datasets analyzed during the current study are available in the GEO dataset (https://www.ncbi.nlm.nih.gov/).
Funding
This work was supported by the National Key R&D Program of China (2019YFC0120000; 2018YFC1312300), the National Natural Science Foundation of China (NSFC: 82071385), and the Key Research and Development Project of Shandong (2019JZZY021010) to Q.W.
Author information
Authors and Affiliations
Contributions
W.L. collected and analyzed the data and was a major contributor in writing the manuscript; J.J., Y.X., and Z.C. performed the experimental validation; Q.W. reviewed and revised the manuscript and provided financial support; A.X., X.Z., and Z.W. provided experimental guidance and training; T.Q. was a major contributor to the production of the images and charts.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
The rights and interests of mice met the requirements of the Laboratory Animal Welfare Ethics Committee of Qingdao University (No. 20210401C572420210831043).
Consent for Publication
Not applicable
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1:
Table S1. Characteristics of studies in DS1, DS2 and primary cells.
ESM 2:
Table S2. Information of top 5% upregulated and downregulated DEGs in DS1.
ESM 3:
Table S3. DEGs that were obvious in both DS1 and DS2
ESM 4:
Table S4. Module genes overlapped with cell type-specific markers and DEGs of primary
ESM 5:
Table S5. Pathways and process of modules identified by metascape, GSEA and GSVA analysis.
ESM 6:
Table S6. Expression of core hub-genes of ischemia related modules.
ESM 7:
Table S7. Expression of core hub-genes of blue and turquoise modules in primary astrocyte, microglia, epithelium, macrophages from GEO datasets.
ESM 8:
Table S8. Primers in RT-qPCR analysis.
ESM 9:
Table S9. Previously-identified genes implicated in ischemic stroke and their distribution in modules or DS1-DEGs.
ESM 10:
Figure S1. (a) Clustering analysis and traits of all samples in DS1, bases on overlapped DEGs of DS1 and DS2. Colors range from light to dark red: Group – control, MCAO; Sample sites – cortex, penumbra, CA1 region of hippocampus, hemisphere, core, and striatum; ischemia time – 0 h, 0.17 h, 0.5 h, 0.75 h, 1 h, 2 h, 6 h; reperfusion time – 0 h, 2 h, 3 h, 8 h, 24 h, 48 h, 72 h. (b) Clustering analysis in 101 rat samples, bases on DEGs of rat samples. (c) Clustering analysis in DS2, bases on DS2 - DEGs, and on overlapped DEGs of DS1 and DS2. (d) Clustering analysis of the modules on eigengenes-based dissimilarity in DS1, the red line indicates the cutline, modules with dissimilarity <0.2 are merged for further analysis. (e) Correlations of Gene significance for group (A value of correlation between the group and gene expression) and Module Membership in modules (A value of correlation between a specific module and gene expression). The dots concentrated in the upper right corner represent a high correlation between modules and the group. For group in (b) and (c): white bar - control, red bar - MCAO. Figure S2. (a) Clustering analysis of MCAO samples in DS1 on ‘TOM’-based dissimilarity. (b) Heatmap of relationships between modules and reperfusion time, the values are set as the ‘correlation coefficient (p-value)’. (c) Clustering analysis of the reperfusion time related modules on eigengenes-based dissimilarity in DS1 - MCAO samples, the red line indicates the cutline; all dissimilarities of modules > 0.8. (d) Correlations of Gene significance for ischemia time (A value of correlation between the ischemia time and gene expression) and Module Membership in modules (A value of correlation between a specific module and gene expression). The dots concentrated in the upper right corner represent a high correlation between modules and the reperfusion time. Figure S3. (a) The overlap of upregulated and downregulated DEGs in DS1 and the AD dataset GSE122063 (hypergeometric test), respectively. (b) The overlap of DS1-module genes and the AD frontal cortex DEGs in GSE122063 (hypergeometric test). (c) Heatmaps and bar-plots of eigengenes expression in the group-related-blue, turquoise, brown and purple module, respectively. (d) Venn diagrams of upregulated DEGs-DS1-DS2 with primary inflammatory cells’ DEGs. (e) Venn diagrams of upregulated DEGs-DS1-DS2 with blue module core-hubs and turquoise module core-hubs. Figure S4. (a-d) Metascape network plots of enriched terms in the blue, turquoise, brown, and purple modules, respectively. Each node represents an enriched term and is colored first by its cluster ID. Term labels are only shown for one term per cluster. Nodes marked with red border present overlapped terms of GSEA, GSVA, and metascape analysis. Figure S5. Expression of unreported core hubs in DS1. P value ≥ 0.05 is ns; 0.05>p value≥0.01 is *; 0.01>p value≥0.001 is **; 0.001>p value≥0.0001 is ***; p value<0. 0001 is ****.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lv, W., Jiang, J., Xu, Y. et al. Re-Exploring the Inflammation-Related Core Genes and Modules in Cerebral Ischemia. Mol Neurobiol 60, 3439–3451 (2023). https://doi.org/10.1007/s12035-023-03275-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-023-03275-1