Abstract
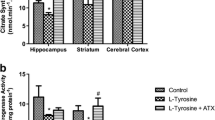
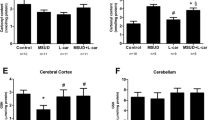
Tissue accumulation and high urinary excretion of argininosuccinate (ASA) is the biochemical hallmark of argininosuccinate lyase deficiency (ASLD), a urea cycle disorder mainly characterized by neurologic abnormalities, whose pathogenesis is still unknown. Thus, in the present work, we evaluated the in vitro and in vivo effects of ASA on a large spectrum of oxidative stress parameters in brain of adolescent rats in order to test whether disruption of redox homeostasis could be involved in neurodegeneration of this disorder. ASA provoked in vitro lipid and protein oxidation, decreased reduced glutathione (GSH) concentrations, and increased reactive oxygen species generation in cerebral cortex and striatum. Furthermore, these effects were totally prevented or attenuated by the antioxidants melatonin and GSH. Similar results were obtained by intrastriatal administration of ASA, in addition to increased reactive nitrogen species generation and decreased activities of superoxide dismutase, glutathione peroxidase, and glutathione S-transferase. It was also observed that melatonin and N-acetylcysteine prevented most of ASA-induced in vivo pro-oxidant effects in striatum. Taken together, these data indicate that disturbance of redox homeostasis induced at least in part by high brain ASA concentrations per se may potentially represent an important pathomechanism of neurodegeneration in patients with ASLD and that therapeutic trials with appropriate antioxidants may be an adjuvant treatment for these patients.









Similar content being viewed by others
References
Allan JD, Cusworth DC, Dent CE, Wilson VK (1958) A disease, probably hereditary characterised by severe mental deficiency and a constant gross abnormality of aminoacid metabolism. Lancet 1:182–187. https://doi.org/10.1016/s0140-6736(58)90666-4
Bizzoco E, Faussone-Pellegrini MS, Vannucchi MG (2007) Activated microglia cells express argininosuccinate synthetase and argininosuccinate lyase in the rat brain after transient ischemia. Exp. Neurol. 208:100–109. https://doi.org/10.1016/j.expneurol.2007.07.018
Braissant O, Gotoh T, Loup M, Mori M, Bachmann C (1999a) L-arginine uptake, the citrulline-NO cycle and arginase II in the rat brain: an in situ hybridization study. Mol. Brain Res. 70:231–241. https://doi.org/10.1016/S0169-328X(99)00151-5
Braissant O, Honegger P, Loup M, Iwase K, Takiguchi M, Bachmann C (1999b) Hyperammonemia: regulation of argininosuccinate synthetase and argininosuccinate lyase genes in aggregating cell cultures of fetal rat brain. Neurosci. Lett. 266:89–92. https://doi.org/10.1016/s0304-3940(99)00274-8
Nagamani SC, Erez A, Lee B (2012a) Argininosuccinate lyase deficiency. Genet. Med. 14:501–507. https://doi.org/10.1038/gim.2011.1
Ratner S, Petrack B (1953) The mechanism of arginine synthesis from citrulline in kidney. J. Biol. Chem. 200:175–185
Tomlinson S, Westall RG (1964) Argininosuccinic aciduria. Argininosuccinase and arginase in human blood cells. Clin Sci. 26:261–269
Wu G, Borbolla AG, Knabe DA (1994) The uptake of glutamine and release of arginine, citrulline and proline by the small intestine of developing pigs. J. Nutr. 124:2437–2444. https://doi.org/10.1093/jn/124.12.437
AlTassan R, Bubshait D, Imtiaz F, Rahbeeni Z (2018) A retrospective biochemical, molecular, and neurocognitive review of Saudi patients with argininosuccinic aciduria. Eur. J. Med. Genet. 61:307–311. https://doi.org/10.1016/j.ejmg.2018.01.007
Brusilow SW, Maestri NE (1996) Urea cycle disorders: diagnosis, pathophysiology, and therapy. Adv. Pediatr. 43:127–170
Mercimek-Mahmutoglu S, Moeslinger D, Häberle J, Engel K, Herle M, Strobl MW, Scheibenreiter S, Muehl A et al (2010) Long-term outcome of patients with argininosuccinate lyase deficiency diagnosed by newborn screening in Austria. Mol. Genet. Metab. 100:24–28. https://doi.org/10.1016/j.ymgme.2010.01.013
Nagamani SCS, Lee B, Erez A (2012b) Optimizing therapy for argininosuccinic aciduria. Mol. Genet. Metab. 107:10–14. https://doi.org/10.1016/j.ymgme.2012.07.009
Summar ML, Koelker S, Freedenberg D, Le Mons C, Haberle J, Lee HS, Kirmse B (2013) The European registry and network for intoxication type metabolic diseases (E-IMD), the members of the urea cycle disorders consortium (UCDC): the incidence of urea cycle disorders. Mol. Genet. Metab. 110:179–180. https://doi.org/10.1016/j.ymgme.2013.07.008
Tuchman T, Lee B, Lichter-Konecki U, Summar ML, Yudkoff M, Cederbaum SD, Kerr DS, Diaz GA et al (2008) Cross-sectional multicenter study of patients with urea cycle disorders in the United States. Mol. Genet. Metab. 94:397–402. https://doi.org/10.1016/j.ymgme.2008.05.004
Brusilow SW, Horwich AL (2014) Urea Cycle Enzymes. In: Valle D, Beaudet AL, Vogelstein B, Kinzler KW, Antonarakis SE, Ballabio A, Gibson K, Mitchell G (eds) The online metabolic and molecular bases of inherited disease. McGraw-Hill, New York http://ommbid.mhmedical.com/content.aspx?bookid=971§ionid=62674945. Accessed June 13, 2019
Kleijer WJ, Garritsen VH, Linnebank M, Mooyer P, Huijmans JG, Mustonen A, Simola KO, Arslan-Kirchner M et al (2002) Clinical, enzymatic, and molecular genetic characterization of a biochemical variant type of argininosuccinic aciduria: prenatal and postnatal diagnosis in five unrelated families. J. Inherit. Metab. Dis. 25:399–410. https://doi.org/10.1023/A:1020108002877
Trevisson E, Salviati L, Baldoin MC, Toldo I, Casarin A, Sacconi S, Cesaro L, Basso G et al (2007) Argininosuccinate lyase deficiency: mutational spectrumin Italian patients and identification of a novel ASL pseudogene. Hum. Mutat. 28:694–702. https://doi.org/10.1002/humu.20498
Balmer C, Pandey AV, Rüfenacht V, Nuoffer JM, Fang P, Wong LJ, Häberle J (2014) Mutations and polymorphisms in the human argininosuccinate lyase (ASL) gene. Hum. Mutat. 35:27–35. https://doi.org/10.1002/humu.22469
Aoyagi K, Nagase S, Gotoh M, Akiyama K, Satoh M, Hirayama A, Koyama A (1996a) Role of reactive oxygen and argininosuccinate in guanidinosuccinate synthesis in isolated rat hepatocytes. Enzyme Protein 49:205–211
Aoyagi K, Nagase S, Tomida C, Takemura K, Akiyama K, Koyama A (1996b) Synthesis of guanidinosuccinate from argininosuccinate and reactive oxygen in vitro. Enzyme Protein 49:199–204
Aoyagi K, Akiyama K, Shahrzad S, Tomida C, Hirayama A, Nagase S, Takemura K, Koyama A et al (1999) Formation of guanidinosuccinic acid, a stable nitric oxide mimic, from argininosuccinic acid and nitric oxide-derived free radicals. Free Radic Res. 31:59–65
Baruteau J, Jameson E, Morris AA, Chakrapani A, Santra S, Vijay S, Kocadag H, Beesley CE et al (2017) Expanding the phenotype in argininosuccinic aciduria: need for new therapies. J Inherit Metab. Dis. 40:357–368. https://doi.org/10.1007/s10545-017-0022-x
Baruteau J, Diez-Fernandez C, Lerner S, Ranucci G, Gissen P, Dionisi-Vici C, Nagamani S, Erez A et al (2019) Argininosuccinic aciduria: recent pathophysiological insights and therapeutic prospects. J. Inherit. Metab. Dis. https://doi.org/10.1002/jimd.12047
Sijens PE, Reijngoud DJ, Soorani-Lunsing RJ, Oudkerk M, van Spronsen FJ (2006) Cerebral 1H MR spectroscopy showing elevation of brain guanidinoacetate in argininosuccinate lyase deficiency. Mol. Genet. Metab. 88:100–102. https://doi.org/10.1016/j.ymgme.2005.10.013
van Spronsen FJ, Reijngoud DJ, Verhoeven NM, Soorani-Lunsing RJ, Jakobs C, Sijens PE (2006) High cerebral guanidinoacetate and variable creatine concentrations in argininosuccinate synthetase and lyase deficiency: implications for treatment? Mol. Genet. Metab. 89:274–276. https://doi.org/10.1016/j.ymgme.2006.02.005
Ficicioglu C, Mandell R, Shih VE (2009) Argininosuccinate lyase deficiency: long term outcome of 13 patients detected by newborn screening. Mol. Genet. Metab. 98:273–277. https://doi.org/10.1016/j.ymgme.2009.06.011
Baruteau J, Perocheau DP, Hanley J, Lorvellec M, Rocha-Ferreira E, Karda R, Ng J, Suff N et al (2018) Argininosuccinic aciduria fosters neuronal nitrosative stress reversed by Asl gene transfer. Nat. Commun. 29:3505–3514. https://doi.org/10.1038/s41467-018-05972-1
Erez A, Nagamani SC, Shchelochkov OA, Premkumar MH, Campeau PM, Chen Y, Garg HK, Li L et al (2011) Requirement of argininosuccinate lyase for systemic nitric oxide production. Nat. Med. 17:1619–1626. https://doi.org/10.1038/nm.2544
Diez-Fernandez C, Hertig D, Loup M, Diserens G, Henry H, Vermathen P, Nuoffer JM, Häberle J et al (2019) Argininosuccinate neurotoxicity and prevention by creatine in argininosuccinate lyase deficiency: an in vitro study in rat three-dimensional organotypic brain cell cultures. J. Inherit. Metab. Dis. https://doi.org/10.1002/jimd.12090
Halliwell B, Gutteridge JMC (2015) Cellular responses to oxidative stress: adaptation, damage, repair, senescence and death. In: Halliwell B, Gutteridge JMC (eds) Free radicals in biology and medicine, 5th edn. Oxford University Press Inc., Oxford, pp. 199–283
Evelson P, Travacio M, Repetto M, Escobar J, Llesuy S, Lissi EA (2001) Evaluation of total reactive antioxidant potential (TRAP) of tissue homogenates and their cytosols. Arch. Biochem. Biophys. 388:261–266. https://doi.org/10.1006/abbi.2001.2292
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J. Biol. Chem. 193:265–275
Zanatta Â, Cecatto C, Ribeiro RT, Amaral AU, Wyse AT, Leipnitz G, Wajner M (2018) S-Adenosylmethionine promotes oxidative stress and decreases Na+, K+-ATPase activity in cerebral cortex supernatants of adolescent rats: implications for the pathogenesis of S-adenosylhomocysteine hydrolase deficiency. Mol. Neurobiol. 55:5868–5878. https://doi.org/10.1007/s12035-017-0804-z
Paxinos G, Watson C (2013) The rat brain in stereotaxic coordinates, 7th edn. Academic, Cambridge
Seminotti B, Zanatta Â, Ribeiro RT, da Rosa MS, Wyse ATS, Leipnitz G, Wajner M (2019) Disruption of brain redox homeostasis, microglia activation and neuronal damage induced by intracerebroventricular administration of S-adenosylmethionine to developing rats. Mol. Neurobiol. 56:2760–2773. https://doi.org/10.1007/s12035-018-1275-6
Yagi K (1998) Simple procedure for specific assay of lipid hydroperoxides in serum or plasma. Methods Mol. Biol. 108:107–110. https://doi.org/10.1385/0-89603-472-0:107
Reznick AZ, Packer L (1994) Oxidative damage to proteins: spectrophotometric method for carbonyl assay. Methods Enzymol 233:357–363. https://doi.org/10.1016/s0076-6879(94)33041-7
Aksenov MY, Markesbery WR (2001) Changes in thiol content and expression of glutathione redox system genes in the hippocampus and cerebellum in Alzheimer’s disease. Neurosci. Lett. 302:141–145. https://doi.org/10.1016/s0304-3940(01)01636-6
Browne RW, Armstrong D (1998) Reduced glutathione and glutathione disulfide. Methods Mol. Biol. 108:347–352. https://doi.org/10.1385/0-89603-472-0:347
LeBel CP, Ischiropoulos H, Bondy SC (1992) Evaluation of the probe 2′, 7′-dichlorofluorescin as an indicator of reactive oxygen species formation and oxidative stress. Chem. Res. Toxicol. 5:227–231. https://doi.org/10.1021/tx00026a012
Navarro-Gonzálvez JA, Garcia-Benayas C, Arenas J (1998) Semiautomated measurement of nitrate in biological fluids. Clin. Chem. 44:679–681
Marklund SL (1985) Pyrogallol autoxidation. Handbook for Oxygen Radical Research. CRC Press, Boca Raton, pp. 243–247
Wendel A (1981) Glutathione peroxidase. Methods Enzymol. 77:325–332. https://doi.org/10.1016/s0076-6879(81)77046-0
Guthenberg C, Mannervik B (1981) Glutathione S-transferase (transferase pi) from human placenta is identical or closely related to glutathione S-transferase (transferase rho) from erythrocytes. Biochim. Biophys Acta. 661:255–260. https://doi.org/10.1016/0005-2744(81)90012-7
Häberle J, Burlina A, Chakrapani A, Dixon M, Karall D, Lindner M, Mandel H, Martinelli D et al (2019) Suggested guidelines for the diagnosis and management of urea cycle disorders: first revision. J. Inherit. Metab. Dis. https://doi.org/10.1002/jimd.12100
Batshaw ML, MacArthur RB, Tuchman M (2001) Alternative pathway therapy for urea cycle disorders: twenty years later. J Pediatr. 138:S46–S54. https://doi.org/10.1067/mpd.2001.111836
Dalle-Donne I, Rossi R, Giustarini D, Milzani A, Colombo R (2003) Protein carbonyl groups as biomarkers of oxidative stress. Clin. Chim. Acta 329:23–38. https://doi.org/10.1016/s0009-8981(03)00003-2
Davies MJ (2003) Singlet oxygen-mediated damage to proteins and its consequences. Biochem. Biophys. Res. Commun. 305:761–770. https://doi.org/10.1016/s0006-291x(03)00817-9
Fedorova M, Griesser E, Vemula V, Weber D, Ni Z, Hoffmann R (2014) Protein and lipid carbonylation in cellular model of nitrosative stress: mass spectrometry, biochemistry and microscopy study. Free Radic. Biol. Med. 75:S15. https://doi.org/10.1016/j.freeradbiomed.2014.10.589
Fritz KS, Petersen DR (2013) An overview of the chemistry and biology of reactive aldehydes. Free Radic. Biol. Med. 59:85–91. https://doi.org/10.1016/j.freeradbiomed.2012.06.025
Orioli M, Aldini G, Beretta G, Facino RM, Carini M (2005) LC-ESI-MS/MS determination of 4-hydroxy-trans-2-nonenal Michael adducts with cysteine and histidine-containing peptides as early markers of oxidative stress in excitable tissues. J. Chromatogr. B. Analyt. Technol. Biomed. Life Sci. 827:109–118. https://doi.org/10.1016/j.jchromb.2005.04.025
Bonini MG, Rota C, Tomasi A, Mason RP (2006) The oxidation of 2′,7′-dichlorofluorescin to reactive oxygen species: a self-fulfilling prophesy? Free Radic. Biol. Med. 40:968–975. https://doi.org/10.1016/j.freeradbiomed.2005.10.042
Chen X, Zhong Z, Xu Z, Chen L, Wang Y (2010) 2′,7′-Dichlorodihydrofluorescein as a fluorescent probe for reactive oxygen species measurement: forty years of application and controversy. Free Radic. Res. 44:587–604. https://doi.org/10.3109/10715761003709802
Myhre O, Andersen JM, Aarnes H, Fonnum F (2003) Evaluation of the probes 2′,7′-dichlorofluorescin diacetate, luminol, and lucigenin as indicators of reactive species formation. Biochem. Pharmacol. 65:1575–1582. https://doi.org/10.1016/s0006-2952(03)00083-2
Galano A, Reiter RJ (2018) Melatonin and its metabolites vs oxidative stress: from individual actions to collective protection. J. Pineal Res. 65:e12514. https://doi.org/10.1111/jpi.12514
Ding K, Wang H, Xu J, Li T, Zhang L, Ding Y, Zhu L, He J et al (2014) Melatonin stimulates antioxidant enzymes and reduces oxidative stress in experimental traumatic brain injury: the Nrf2-ARE signaling pathway as a potential mechanism. Free Radic. Biol. Med. 73:1–11. https://doi.org/10.1016/j.freeradbiomed.2014.04.031
Kilic U, Kilic E, Tuzcu Z, Tuzcu M, Ozercan IH, Yilmaz O, Sahin F, Sahin K (2013) Melatonin suppresses ciplatin-induced nephrotoxicity via activation of Nrf-2/Ho-1 pathway. Nutr. Metab. 10:7. https://doi.org/10.1186/1743-7075-10-7
Vriend J, Reiter RJ (2015) The Keap1-Nrf2-antioxidant response element pathway: a review of its regulation by melatonin and the proteasome. Mol. Cell. Endocrinol. 401:213–220. https://doi.org/10.1016/j.mce.2014.12.013
Moldogazieva NT, Mokhosoev IM, Feldman NB, Lutsenko SV (2018) ROS and RNS signalling: adaptive redox switches through oxidative/nitrosative protein modifications. Free Radic. Res. 52:507–543. https://doi.org/10.1080/10715762.2018.1457217
Radi R (2018) Oxygen radicals, nitric oxide, and peroxynitrite: Redox pathways in molecular medicine. PNAS 115:5839–5848. https://doi.org/10.1073/pnas.1804932115
Singh P, Jain A, Kaur G (2004) Impact of hypoglycemia and diabetes on CNS: correlation of mitochondrial oxidative stress with DNA damage. Mol. Cell. Biochem. 260:153–159
Mazariegos G, Shneider B, Burton B, Fox IJ, Hadzic N, Kishnani P, Morton DH, McIntire S et al (2014) Liver transplantation for pediatric metabolic disease. Mol. Genet. Metab. 111:418–427. https://doi.org/10.1016/j.ymgme.2014.01.006
Funding
This work was supported by Conselho Nacional de Desenvolvimento Científico e Tecnológico (grant number no. 425914/2016-0), Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul (grant number no. 2266-2551/14-2), Financiadora de Estudos e Projetos/Rede Instituto Brasileiro de Neurociência (grant number no. 01.06.0842-00), and Instituto Nacional de Ciência e Tecnologia em Excitotoxicidade e Neuroproteção (INCT-EN) (grant number no. 465671/2014-4).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Seminotti, B., da Silva, J.C., Ribeiro, R.T. et al. Free Radical Scavengers Prevent Argininosuccinic Acid-Induced Oxidative Stress in the Brain of Developing Rats: a New Adjuvant Therapy for Argininosuccinate Lyase Deficiency?. Mol Neurobiol 57, 1233–1244 (2020). https://doi.org/10.1007/s12035-019-01825-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-019-01825-0