Abstract
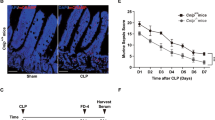
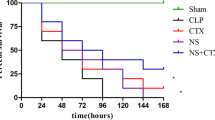
Partially hydrolyzed guar gum (PHGG) protects against intestinal barrier dysfunction and can ameliorate some intestinal diseases. However, whether PHGG has a role in protecting intestinal barrier function (IBF) during sepsis remains unclear. This study aimed to investigate the role and probable mechanism of PHGG in the intestinal mucosa in sepsis. A rat sepsis model was constructed using cecal ligation and puncture (CLP). FITC-dextran 4 (FD-4) flux, serum inflammatory mediator levels, tight junction (TJ) levels, jejunum mucosa pathology, and epithelial intercellular junction ultrastructure were monitored to evaluate the effect of PHGG on IBF. Caco-2 monolayers were used to study the impact and mechanism of PHGG on lipopolysaccharide (LPS)-induced barrier dysfunction in vitro. The expression of zonula occludens protein-1 and occludin and the location of P65 were studied by immunofluorescence. Nuclear factor kappa B (NF-κB) and myosin light chain kinase 3 (MLCK) pathway-related protein expression was verified by quantitative reverse transcriptase polymerase chain reaction or western blotting. The results indicated that the jejunal mucosa structure was destroyed, the villi were disrupted and shortened, and neutrophil infiltration was evident in the septic rats. Compared to Sham group, spetic rats had increased Chiu’s score, serum inflammatory mediator levels, and FD-4 flux but decreased TJ and gap junction density. In addition, the expression of MLCK, p-MLC, and TJ proteins and the expression of P65 in the nucleus were increased in septic rats. Furthermore, compared to those in the Control group, LPS-treated Caco-2 cells showed lower cell viability and transepithelial electrical resistance, while had higher FD-4 flux and the expression of MLCK, p-MLC, TJ proteins and P65 in the nucleus. PHGG pretreatment reversed the above effects induced by CLP or LPS treatment. Moreover, SN50, an NF-κB inhibitor, attenuated the above effects of LPS on Caco-2 cells. Overall, PHGG reduced inflammation, increased TJ protein expression and localization, and relieved damage to the TJ structure and intestinal permeability through suppression of the NF-κB/MLCK pathway. This study provides new insights into the role of PHGG in sepsis therapy.




Similar content being viewed by others
Availability of Data and Materials
All data generated or analysed during this study are included in this published article.
References
Huo, L., Liu, C., Yuan, Y., Liu, X., & Cao, Q. (2023). Pharmacological inhibition of ferroptosis as a therapeutic target for sepsis-associated organ damage. European Journal of Medicial Chemistry, 257, 115438.
Singer, M., Deutschman, C. S., Seymour, C. W., Shankar-Hari, M., Annane, D., Bauer, M., Bellomo, R., Bernard, G. R., Chiche, J. D., Coopersmith, C. M., Hotchkiss, R. S., Levy, M. M., Marshall, J. C., Martin, G. S., Opal, S. M., Rubenfeld, G. D., van der Poll, T., Vincent, J. L., & Angus, D. C. (2016). The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA, 315, 801–810.
De Backer, D., Deutschman, C. S., Hellman, J., Myatra, S. N., Ostermann, M., Prescott, H. C., Talmor, D., Antonelli, M., Pontes Azevedo, L. C., Bauer, S. R., Kissoon, N., Loeches, I. M., Nunnally, M., Tissieres, P., Vieillard-Baron, A., & Coopersmith, C. M. (2024). Surviving sepsis campaign research priorities 2023. Critical Care Medicine, 52, 268–296.
Rudd, K. E., Johnson, S. C., Agesa, K. M., Shackelford, K. A., Tsoi, D., Kievlan, D. R., Colombara, D. V., Ikuta, K. S., Kissoon, N., Finfer, S., Fleischmann-Struzek, C., Machado, F. R., Reinhart, K. K., Rowan, K., Seymour, C. W., Watson, R. S., West, T. E., Marinho, F., Hay, S. I., … Naghavi, M. (2020). Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. Lancet (London, England), 395, 200–211.
Dellinger, R. P., Levy, M. M., Rhodes, A., Annane, D., Gerlach, H., Opal, S. M., Sevransky, J. E., Sprung, C. L., Douglas, I. S., Jaeschke, R., Osborn, T. M., Nunnally, M. E., Townsend, S. R., Reinhart, K., Kleinpell, R. M., Angus, D. C., Deutschman, C. S., Machado, F. R., Rubenfeld, G. D., … Surviving Sepsis Campaign Guidelines Committee including the Pediatric, S. (2013). Surviving sepsis campaign: International guidelines for management of severe sepsis and septic shock: 2012. Critical Care Medicine, 41, 580–637.
Moschopoulos, C. D., Dimopoulou, D., Dimopoulou, A., Dimopoulou, K., Protopapas, K., Zavras, N., Tsiodras, S., Kotanidou, A., & Fragkou, P. C. (2023). New insights into the fluid management in patients with septic shock. Medicina (Kaunas, Lithuania), 59, 1047.
Munroe, E. S., Hyzy, R. C., Semler, M. W., Shankar-Hari, M., Young, P. J., Zampieri, F. G., & Prescott, H. C. (2023). Evolving management practices for early sepsis-induced hypoperfusion: a narrative review. American Journal of Respiratory and Critical Care Medicine, 207, 1283–1299.
Kamath, S., Hammad Altaq, H., & Abdo, T. (2023). Management of sepsis and septic shock: what have we learned in the last two decades? Microorganisms, 11, 2231.
Schmoch, T., Weigand, M. A., & Brenner, T. (2024). Guideline-conform treatment of sepsis. Die Anaesthesiologie, 73, 4–16.
Hotchkiss, R. S., Monneret, G., & Payen, D. (2013). Sepsis-induced immunosuppression: from cellular dysfunctions to immunotherapy. Nature Reviews Immunology, 13, 862–874.
Huang, M., Cai, S., & Su, J. (2019). The pathogenesis of sepsis and potential therapeutic targets. International Journal of Molecular Sciences, 20, 5376.
Napolitano, L. M. (2018). Sepsis 2018: definitions and guideline changes. Surgical Infections (Larchmt), 19, 117–125.
Sertaridou, E., Papaioannou, V., Kolios, G., & Pneumatikos, I. (2015). Gut failure in critical care: old school versus new school. Annals of Gastroenterology, 28, 309–322.
Klingensmith, N. J., & Coopersmith, C. M. (2016). The gut as the motor of multiple organ dysfunction in critical illness. Critical Care Clinics, 32, 203–212.
Mittal, R., & Coopersmith, C. M. (2014). Redefining the gut as the motor of critical illness. Trends in Molecular Medicine, 20, 214–223.
Lou, X., Xue, J., Shao, R., Mo, C., Wang, F., & Chen, G. (2023). Postbiotics as potential new therapeutic agents for sepsis. Burns & trauma. https://doi.org/10.1093/burnst/tkad022
Fay, K. T., Ford, M. L., & Coopersmith, C. M. (2017). The intestinal microenvironment in sepsis. Biochimica et Biophysica Acta, Molecular Basis of Disease, 1863, 2574–2583.
Oshima, T., & Miwa, H. (2016). Gastrointestinal mucosal barrier function and diseases. Journal of Gastroenterology, 51, 768–778.
Pitman, R. S., & Blumberg, R. S. (2000). First line of defense: The role of the intestinal epithelium as an active component of the mucosal immune system. Journal of Gastroenterology, 35, 805–814.
Qian, T., Qi, B., Fei, Y., Li, J., Luo, L., Lv, B., Song, Y., Sheng, S., Xiao, W., Huang, X., & Wang, X. (2023). PLD2 deletion alleviates disruption of tight junctions in sepsis-induced ALI by regulating PA/STAT3 phosphorylation pathway. International Immunopharmacology, 114, 109561.
Haussner, F., Chakraborty, S., Halbgebauer, R., & Huber-Lang, M. (2019). Challenge to the intestinal mucosa during sepsis. Frontiers in Immunology, 10, 891.
Yan, Z., Niu, L., Wang, S., Gao, C., & Pan, S. (2024). Intestinal Piezo1 aggravates intestinal barrier dysfunction during sepsis by mediating Ca(2+) influx. Journal of Translational Medicine, 22, 332.
Fang, Q., Yu, L., Tian, F., Zhang, H., Chen, W., & Zhai, Q. (2023). Effects of dietary irritants on intestinal homeostasis and the intervention strategies. Food Chemistry, 409, 135280.
Thombare, N., Jha, U., Mishra, S., & Siddiqui, M. Z. (2016). Guar gum as a promising starting material for diverse applications: a review. International Journal of Biological Macromolecules, 88, 361–372.
Li, Y. X., Yi, P., Wang, N. N., Liu, J., Liu, X. Q., Yan, Q. J., & Jiang, Z. Q. (2017). High level expression of beta-mannanase (RmMan5A) in Pichia pastoris for partially hydrolyzed guar gum production. International Journal of Biological Macromolecules, 105, 1171–1179.
Mudgil, D., Barak, S., Patel, A., & Shah, N. (2018). Partially hydrolyzed guar gum as a potential prebiotic source. International Journal of Biological Macromolecules, 112, 207–210.
Ohashi, Y., Sumitani, K., Tokunaga, M., Ishihara, N., Okubo, T., & Fujisawa, T. (2015). Consumption of partially hydrolysed guar gum stimulates Bifidobacteria and butyrate-producing bacteria in the human large intestine. Beneficial Microbes, 6, 451–455.
Stewart, M. L., & Slavin, J. L. (2006). Molecular weight of guar gum affects short-chain fatty acid profile in model intestinal fermentation. Molecular Nutrition & Food Research, 50, 971–976.
Takagi, T., Naito, Y., Higashimura, Y., Ushiroda, C., Mizushima, K., Ohashi, Y., Yasukawa, Z., Ozeki, M., Tokunaga, M., Okubo, T., Katada, K., Kamada, K., Uchiyama, K., Handa, O., Itoh, Y., & Yoshikawa, T. (2016). Partially hydrolysed guar gum ameliorates murine intestinal inflammation in association with modulating luminal microbiota and SCFA. British Journal of Nutrition, 116, 1199–1205.
Fujii, T., Chiba, Y., Nakayama-Imaohji, H., Onishi, S., Tanaka, A., Katami, H., Kaji, T., Ieiri, S., Miki, T., Ueno, M., Kuwahara, T., & Shimono, R. (2019). Partially hydrolyzed guar gum alleviates small intestinal mucosal damage after massive small bowel resection along with changes in the intestinal microbiota. Journal of Pediatric Surgery, 54, 2514–2519.
Russo, L., Andreozzi, P., Zito, F. P., Vozzella, L., Savino, I. G., Sarnelli, G., & Cuomo, R. (2015). Partially hydrolyzed guar gum in the treatment of irritable bowel syndrome with constipation: effects of gender, age, and body mass index. Saudi Journal of Gastroenterology, 21, 104–110.
Alam, N. H., Ashraf, H., Kamruzzaman, M., Ahmed, T., Islam, S., Olesen, M. K., Gyr, N., & Meier, R. (2015). Efficacy of partially hydrolyzed guar gum (PHGG) supplemented modified oral rehydration solution in the treatment of severely malnourished children with watery diarrhoea: a randomised double-blind controlled trial. Journal of Health, Population, and Nutrition, 34, 3.
Minekus, M., Jelier, M., Xiao, J. Z., Kondo, S., Iwatsuki, K., Kokubo, S., Bos, M., Dunnewind, B., & Havenaar, R. (2005). Effect of partially hydrolyzed guar gum (PHGG) on the bioaccessibility of fat and cholesterol. Bioscience, Biotechnology, and Biochemistry, 69, 932–938.
Hung, T. V., & Suzuki, T. (2018). Dietary Fermentable Fibers Attenuate Chronic Kidney Disease in Mice by Protecting the Intestinal Barrier. Journal of Nutrition, 148, 552–561.
Toscano, M. G., Ganea, D., & Gamero, A. M. (2011). Cecal ligation puncture procedure. Journal of Visualized Experiments. https://doi.org/10.3791/2860
Yoseph, B. P., Klingensmith, N. J., Liang, Z., Breed, E. R., Burd, E. M., Mittal, R., Dominguez, J. A., Petrie, B., Ford, M. L., & Coopersmith, C. M. (2016). Mechanisms of intestinal barrier dysfunction in sepsis. Shock, 46, 52–59.
Xue, M., Liu, Y., Xu, H., Zhou, Z., Ma, Y., Sun, T., Liu, M., Zhang, H., & Liang, H. (2019) Propolis modulates the gut microbiota and improves the intestinal mucosal barrier function in diabetic rats. Biomedicine & pharmacotherapy = Biomedecine & pharmacotherapie 118, 109393.
Chiu, C. J., McArdle, A. H., Brown, R., Scott, H. J., & Gurd, F. N. (1970). Intestinal mucosal lesion in low-flow states. I. A morphological, hemodynamic, and metabolic reappraisal. Archives of Surgery, 101, 478–483.
Lea, T. (2015) Caco-2 Cell Line, in The Impact of Food Bioactives on Health: in vitro and ex vivo models, (K. Verhoeckx, P. Cotter, I. Lopez-Exposito, C. Kleiveland, T. Lea, A. Mackie, T. Requena, D. Swiatecka and H. Wichers eds), Cham (CH): pp. 103–111.
Guo, S., Chen, S., Ma, J., Ma, Y., Zhu, J., Ma, Y., Liu, Y., Wang, P., & Pan, Y. (2019). Escherichia coli Nissle 1917 protects intestinal barrier function by inhibiting NF-kappaB-mediated activation of the MLCK-P-MLC signaling pathway. Mediators of Inflammation, 2019, 5796491.
Gao, Y., Nan, X., Shi, X., Mu, X., Liu, B., Zhu, H., Yao, B., Liu, X., Yang, T., Hu, Y., & Liu, S. (2019). SREBP1 promotes the invasion of colorectal cancer accompanied upregulation of MMP7 expression and NF-kappaB pathway activation. BMC Cancer, 19, 685.
Jo, H., Hwang, D., Kim, J. K., & Lim, Y. H. (2017). Oxyresveratrol improves tight junction integrity through the PKC and MAPK signaling pathways in Caco-2 cells. Food and Chemical Toxicology, 108, 203–213.
Fu, J., Li, G., Wu, X., & Zang, B. (2019). Sodium butyrate ameliorates intestinal injury and improves survival in a rat model of cecal ligation and puncture-induced sepsis. Inflammation, 42, 1276–1286.
Chen, S., Zhu, J., Chen, G., Zuo, S., Zhang, J., Chen, Z., Wang, X., Li, J., Liu, Y., & Wang, P. (2015). 1,25-Dihydroxyvitamin D3 preserves intestinal epithelial barrier function from TNF-alpha induced injury via suppression of NF-kB p65 mediated MLCK-P-MLC signaling pathway. Biochemical and Biophysical Research Communications, 460, 873–878.
Assimakopoulos, S. F., Triantos, C., Thomopoulos, K., Fligou, F., Maroulis, I., Marangos, M., & Gogos, C. A. (2018). Gut-origin sepsis in the critically ill patient: pathophysiology and treatment. Infection, 46, 751–760.
Turner, J. R. (2009). Intestinal mucosal barrier function in health and disease. Nature Reviews Immunology, 9, 799–809.
Lee, B., Moon, K. M., & Kim, C. Y. (2018). Tight junction in the intestinal epithelium: its association with diseases and regulation by phytochemicals. Journal of Immunology Research, 2018, 2645465.
Chen, C., Wang, P., Su, Q., Wang, S., & Wang, F. (2012). Myosin light chain kinase mediates intestinal barrier disruption following burn injury. PLoS One, 7, e34946.
Hashimoto, K., & Shimizu, M. (1993). Epithelial properties of human intestinal Caco-2 cells cultured in a serum-free medium. Cytotechnology, 13, 175–184.
Majima, A., Handa, O., Naito, Y., Suyama, Y., Onozawa, Y., Higashimura, Y., Mizushima, K., Morita, M., Uehara, Y., Horie, H., Iida, T., Fukui, A., Dohi, O., Okayama, T., Yoshida, N., Kamada, K., Katada, K., Uchiyama, K., Ishikawa, T., … Itoh, Y. (2017). Real-time monitoring of trans-epithelial electrical resistance in cultured intestinal epithelial cells: The barrier protection of water-soluble dietary fiber. Journal of Digestive Diseases, 18, 151–159.
Tang, X., Liu, B., Wang, X., Yu, Q., & Fang, R. (2018). Epidermal growth factor, through alleviating oxidative stress, protect IPEC-J2 cells from lipopolysaccharides-induced apoptosis. International Journal of Molecular Sciences, 19, 848.
Wu, X. X., Huang, X. L., Chen, R. R., Li, T., Ye, H. J., Xie, W., Huang, Z. M., & Cao, G. Z. (2019). Paeoniflorin prevents intestinal barrier disruption and inhibits lipopolysaccharide (LPS)-induced inflammation in Caco-2 cell monolayers. Inflammation, 42, 2215–2225.
Sheth, P., Delos Santos, N., Seth, A., LaRusso, N. F., & Rao, R. K. (2007). Lipopolysaccharide disrupts tight junctions in cholangiocyte monolayers by a c-Src-, TLR4-, and LBP-dependent mechanism. American Journal of Physiology. Gastrointestinal and Liver Physiology, 293, G308-318.
Ye, D., Ma, I., & Ma, T. Y. (2006). Molecular mechanism of tumor necrosis factor-alpha modulation of intestinal epithelial tight junction barrier. American Journal of Physiology. Gastrointestinal and Liver Physiology, 290, G496-504.
Nie, N., Bai, C., Song, S., Zhang, Y., Wang, B., & Li, Z. (2020). Bifidobacterium plays a protective role in TNF-alpha-induced inflammatory response in Caco-2 cell through NF-kappaB and p38MAPK pathways. Molecular and Cellular Biochemistry, 464, 83–91.
Haak, B. W., & Wiersinga, W. J. (2017). The role of the gut microbiota in sepsis. The Lancet Gastroenterology & Hepatology 2, 135–143.
Acknowledgements
Not applicable.
Funding
This work was supported by the Wu Jieping Medical Foundation [grant number 320.6750.2022-2-25]; the Guangdong Clinical Research Center for Critical Care Medicine [grant number 2020B1111170005], the Sun Yat sen University Clinical Research Program 5010 [grant number 2019002].
Author information
Authors and Affiliations
Contributions
ZT, YZ, CC, and XG contributed to the study conception and design and drafted the manuscript. ZT and YZ contributed to animal experiment. XH and KL contributed to cell experiment. ZT, XS and SL analyzed and interpreted the data. ZT and YZ are joint first authors. CC and XG are joint senior authors. All the authors revised the manuscript for important intellectual content, read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Ethics Approval and Consent to Participate
All animal experiments were performed in accordance with the Guide for the Care and Use of Laboratory Animals (National Institutes of Health). All experiments and procedures were reviewed and approved by the ethics committee of the Sun Yat-sen University First Affiliated Hospital (Guangzhou, China). All efforts were made to minimize the suffering of the animals during experiments.
Consent for Publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, Z., Zhu, Y., Hu, X. et al. Improving Intestinal Barrier Function in Sepsis by Partially Hydrolysed Guar Gum via the Suppression of the NF-κB/MLCK Pathway. Mol Biotechnol (2024). https://doi.org/10.1007/s12033-024-01180-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12033-024-01180-z