Abstract
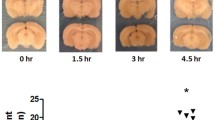
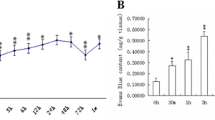
Blood-brain barrier (BBB) dysfunction is involved in the pathogenesis of contrast-induced encephalopathy (CIE), which is a rare adverse event following angiography. In this study, we observed the dynamic effect and potential mechanism of ioversol on the BBB in rats. Eighty-one healthy rats were randomly divided into a normal control group (n = 9), ioversol group (n = 36), and 0.9% NaCl group (n = 36); the latter two groups were separately subdivided into four groups based on time points after treatment (0.5, 3, 6, and 24 h) (n = 9/group). Permeability of the BBB was measured by an Evans Blue (EB) assay. Levels of the tight junction (TJ) proteins ZO-1 and occludin were determined by western blot and immunofluorescence staining. EB content increased at 3 h after the administration of ioversol via the carotid artery and reached a peak at 6 h (P < 0.05), whereas it decreased to its normal level at 24 h. Western blot and immunofluorescence staining indicated that the expression of ZO-1 in brain tissues gradually decreased to its lowest level at 3 h, and then increased gradually, but was still lower than that of the normal control group at 24 h (P < 0.05). Occludin was similar, but its lowest expression appeared at 0.5 h. This study demonstrated that the permeability of BBB in rats increased first and then decreased after ioversol was injected into the carotid artery. The mechanism may be related to altered protein expression of TJs, which are important structures in BBB. Early intervention against TJ proteins may be an effective measure to prevent and treat CIE.




Similar content being viewed by others
Abbreviations
- BBB:
-
Blood–brain barrier
- CIE:
-
Contrast-induced encephalopathy
- EB:
-
Evans Blue
- TJ:
-
Tight junction
- ZO-1:
-
Zonula occludens-1
- CM:
-
Contrast media
- CCA:
-
Common carotid artery
- ECA:
-
External carotid artery
- ICA:
-
Internal carotid artery
- SD:
-
Standard deviation
References
Bassett RC, Rogers JS, Cherry GR, Cruzhit C (1953) The effect of contrast media on the blood-brain-barrier. J Neurosurg 10(1):38–47
Beckett KR, Moriarity AK, Langer JM (2015) Safe use of contrast media: what the radiologist needs to know. Radiographics 35:1738–1750. https://doi.org/10.1148/rg.2015150033
Broman T, Olsson O (1948) The tolerance of cerebral blood-vessels to a contrast medium of the diorast group: an experimental study of the effect on the blood-brain-barrier. Acta Radiol 30:326–342
Cardoso FL, Brites D, Brito MA (2010) Looking at the blood-brain barrier: molecular anatomy and possible investigation approaches. Brain Res Rev 64:328–363. https://doi.org/10.1016/j.brainresrev.2010.05.003
Clark BA, Kim D, Epstein FH (1997) Endothelin and atrial natriuretic peptide levels following radiocontrast exposure in humans. Am J Kidney Dis 30:82–86. https://doi.org/10.1016/S0272-6386(97)90568-0
Dattani A, Au L, Tay K, Davey P (2018) Contrast-induced encephalopathy following coronary angiography with no radiological features: a case report and literature review. Cardiology 139:197–201. https://doi.org/10.1159/000486636
Franke RP, Fuhrmann R, Hiebl B, Jung F (2008) Influence of various radiographic contrast media on the buckling of endothelial cells. Microvasc Res 76:110–113. https://doi.org/10.1016/j.mvr.2008.05.002
Frye RE, Newburger JW, Nugent A, Sahin M (2005) Focal seizure and cerebral contrast retention after cardiac catheterization. Pediatr Neurol 32:213–216. https://doi.org/10.1016/j.pediatrneurol.2004.07.012
Gonsette RE, Liesenborgh L (1980) New contrast media in cerebral angiography: animal experiments and preliminary clinical studies. Investig Radiol 15:S270–S274
Greene C, Campbell M (2016) Tight junction modulation of the blood brain barrier: CNS delivery of small molecules. Tissue Barriers 4:e1138017. https://doi.org/10.1080/21688370.2015.1138017
Haley EC Jr (1984) Encephalopathy following arteriography: a possible toxic effect of contrast agents. Ann Neurol 15:100–102. https://doi.org/10.1002/ana.410150118
Haseloff RF, Dithmer S, Winkler L, Wolburg H, Blasig IE (2015) Transmembrane proteins of the tight junctions at the blood-brain barrier: structural and functional aspects. Semin Cell Dev Biol 38:16–25. https://doi.org/10.1016/j.semcdb.2014.11.004
Heyman SN, Clark BA, Kaiser N, Spokes K, Rosen S, Brezis M, Epstein FH (1992) Radiocontrast agents induce endothelin release in vivo and in vitro. J Am Soc Nephrol 3:58–65
Jiao H, Wang Z, Liu Y, Wang P, Xue Y (2011) Specific role of tight junction proteins claudin-5, occludin, and ZO-1 of the blood-brain barrier in a focal cerebral ischemic insult. J Mol Neurosci 44:130–139. https://doi.org/10.1007/s12031-011-9496-4
Junck L, Marshall WH (1983) Neurotoxicity of radiological contrast agents. Ann Neurol 13(5):469–484
Keaney J, Campbell M (2015) The dynamic blood-brain barrier. FEBS J 282:4067–4079. https://doi.org/10.1111/febs.13412
Khatri P, Broderick JP, Khoury JC, Carrozzella JA, Tomsick TA, Investigators III (2008) Microcatheter contrast injections during intra-arterial thrombolysis may increase intracranial hemorrhage risk. Stroke 39:3283–3287. https://doi.org/10.1161/Strokeaha.108.522904
Khatri R, McKinney AM, Swenson B, Janardhan V (2012) Blood-brain barrier, reperfusion injury, and hemorrhagic transformation in acute ischemic stroke. Neurology 79:S52–S57. https://doi.org/10.1212/WNL.0b013e3182697e70
Knowland D, Arac A, Sekiguchi KJ, Hsu M, Lutz SE, Perrino J, Steinberg GK, Barres BA, Nimmerjahn A, Agalliu D (2014) Stepwise recruitment of transcellular and paracellular pathways underlies blood-brain barrier breakdown in stroke. Neuron 82:603–617. https://doi.org/10.1016/j.neuron.2014.03.003
Kopecky KK, Becker GJ, Conces DJ Jr (1989) Ioversol 320: a new nonionic, water-soluble contrast medium for body computed tomography clinical trial. Investig Radiol 24(Suppl 1):S33–S34
Krueger M, Hartig W, Reichenbach A, Bechmann I, Michalski D (2013) Blood-brain barrier breakdown after embolic stroke in rats occurs without ultrastructural evidence for disrupting tight junctions. PLoS One 8:e56419. https://doi.org/10.1371/journal.pone.0056419
Kurosawa Y, Lu AG, Khatri P, Carrozzella JA, Clark JF, Khoury J, Tomsick TA (2010) Intra-arterial iodinated radiographic contrast material injection administration in a rat middle cerebral artery occlusion and reperfusion model possible effects on intracerebral hemorrhage. Stroke 41:1013–1017. https://doi.org/10.1161/Strokeaha.110.578245
Leong S, Fanning NF (2012) Persistent neurological deficit from iodinated contrast encephalopathy following intracranial aneurysm coiling: a case report and review of the literature. Interv Neuroradiol 18:33–41. https://doi.org/10.1177/159101991201800105
Nakamura I, Hori S, Funabiki T, Sekine K, Kimura H, Fujishima S, Aoki K, Kuribayashi S, Aikawa N (2002) Cardiopulmonary arrest induced by anaphylactoid reaction with contrast media. Resuscitation 53:223–226
Nico B, Ribatti D (2012) Morphofunctional aspects of the blood-brain barrier. Curr Drug Metab 13:50–60
Niimi Y, Kupersmith MJ, Ahmad S, Song J, Berenstein A (2008) Cortical blindness, transient and otherwise, associated with detachable coil embolization of intracranial aneurysms. AJNR Am J Neuroradiol 29:603–607. https://doi.org/10.3174/ajnr.A0858
O’Donnell DH, Moloney MA, Bouchier-Hayes DJ, Lee MJ (2010) Iodinated contrast media alter immune responses in pro-inflammatory states. Acta Radiol 51:635–640. https://doi.org/10.3109/02841851.2010.481679
Obermeier B, Daneman R, Ransohoff RM (2013) Development, maintenance and disruption of the blood-brain barrier. Nat Med 19:1584–1596. https://doi.org/10.1038/nm.3407
Potsi S, Chourmouzi D, Moumtzouoglou A, Nikiforaki A, Gkouvas K, Drevelegas A (2012) Transient contrast encephalopathy after carotid angiography mimicking diffuse subarachnoid haemorrhage. Neurol Sci 33:445–448. https://doi.org/10.1007/s10072-011-0765-3
Spina R, Simon N, Markus R, Muller DW, Kathir K (2017) Recurrent contrast-induced encephalopathy following coronary angiography. Intern Med J 47:221–224. https://doi.org/10.1111/imj.13321
Tiwari YV, Lu JF, Shen Q, Cerqueira B, Duong TQ (2017) Magnetic resonance imaging of blood-brain barrier permeability in ischemic stroke using diffusion-weighted arterial spin labeling in rats. J Cere Blood Flow Metab 37:2706–2715. https://doi.org/10.1177/0271678x16673385
Wolburg H, Lippoldt A (2002) Tight junctions of the blood-brain barrier: development, composition and regulation. Vasc Pharmacol 38:323–337
Yu J, Dangas G (2011) New insights into the risk factors of contrast-induced encephalopathy. J Endovasc Ther 18:545–546. https://doi.org/10.1583/11-3476c.1
Zihni C, Mills C, Matter K, Balda MS (2016) Tight junctions: from simple barriers to multifunctional molecular gates. Nat Rev Mol Cell Biol 17:564–580. https://doi.org/10.1038/nrm.2016.80
Zweifler RM, Rothrock JF (1995) Aseptic meningoencephalitis following iohexol myelography. Neuroradiology 37:148–149
Acknowledgments
We thank the members of the Laboratory of Neurology, Xijing Hospital, Air Force Military Medical University. We also thank Prof. Ming Shi (Department of Neurology, Xijing Hospital, Air Force Military Medical University) for his advice on our experimental design, as well as Dr. Yajun Shi (Department of Neurology, Xijing Hospital, Air Force Military Medical University) for helping us with our experimental methods.
Funding
This work was supported by grants from the Shaanxi Science Research Project, China (No. 2010K16-08-02, 2015SF009) and the Second Affiliated Hospital Science Research Project, Xi’an Jiaotong University of China.
Author information
Authors and Affiliations
Contributions
Heying Wang and Guilian Zhang wrote the main manuscript text. Heying Wang, Tao Li, Lili Zhao, Jiao Liu, and Guilian Zhang designed the experiment, Heying Wang, Man Sun, Yating Jian, Yiheng Zhang, Ye Li, and Meijuan Dang collected sample and analyzed the data. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
All the study procedures complied with the National Institute of Health Guide for the Care and Use of Laboratory Animals (NIH Publication No. 80-23). The animal experiments were approved by the Committee on the Ethics of Animal Experiments of the Xi’an Jiaotong University College of Medicine.
Conflict of Interest
The authors declare that they have no conflict of interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, H., Li, T., Zhao, L. et al. Dynamic Effects of Ioversol on the Permeability of the Blood-Brain Barrier and the Expression of ZO-1/Occludin in Rats. J Mol Neurosci 68, 295–303 (2019). https://doi.org/10.1007/s12031-019-01305-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-019-01305-z