Abstract
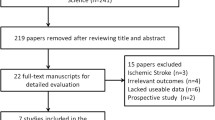
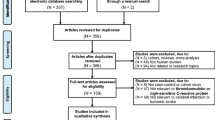
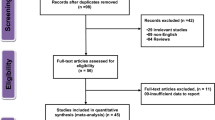
The purpose of this meta-analysis was to investigate the correlation between serum homocysteine (Hcy) levels and the pathogenesis of cerebral infarction (CI). Relevant studies involving serum Hcy levels and the pathogenesis of CI were identified using electronic database search supplemented with manual search. The search result studies were screened in accordance with our strict inclusion and exclusion criteria. Statistical analyses were conducted with Comprehensive Meta Analysis 2.0 (CMA 2.0) software. A total of 13 studies were eligible for our meta-analysis and included 1206 patients with CI and 1202 healthy controls. Our meta-analysis revealed that the serum Hcy levels in CI patients were significantly higher than those in healthy controls. Subgroup analysis based on ethnicity showed that Caucasians and Asians had significantly higher serum Hcy levels in CI patients compared to healthy controls and Africans showed no significant differences in serum Hcy levels between CI patients and controls. In conclusion, our meta-analysis reveals a strong correlation between elevated serum Hcy levels and the pathogenesis of CI, suggesting that serum Hcy levels may be an important biomarker for the early diagnosis and treatment assessment of CI.






Similar content being viewed by others
References
Adinolfi LE, Zampino R, Restivo L et al (2014) Chronic hepatitis C virus infection and atherosclerosis: clinical impact and mechanisms. World J Gastroenterol 20:3410–3417
Bishop MJ, Plank G (2014) Simulating photon scattering effects in structurally detailed ventricular models using a Monte Carlo approach. Front Physiol 5:338
Chen SF, Cui CL, Wu P, Xie NZ (2013) Relationship of serum homocysteine level with nutritional status and HbA1c level in elderly inpatients. Int J Clin Exp Med 6:779–784
Dougu N, Takashima S, Sasahara E et al (2011) Predictors of poor outcome in patients with acute cerebral infarction. J Clin Neurol 7:197–202
Egger M, Davey SG, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558
Kalita J, Kumar G, Bansal V, Misra UK (2009) Relationship of homocysteine with other risk factors and outcome of ischemic stroke. Clin Neurol Neurosurg 111:364–367
Kawamoto R, Kajiwara T, Oka Y, Takagi Y (2002) An association between plasma homocysteine concentrations and ischemic stroke in elderly Japanese. J Atheroscler Thromb 9:121–125
Kim NK, Choi BO, Jung WS, Choi YJ, Choi KG (2003) Hyperhomocysteinemia as an independent risk factor for silent brain infarction. Neurology 61:1595–1599
Kim OJ, Lee JH, Choi JK et al (2010) Association between tumor necrosis factor-alpha (-308G–>A and -238G–>A) polymorphisms and homocysteine levels in patients with ischemic strokes and silent brain infarctions. Cerebrovasc Dis 30:483–490
Ma SG, Xu W, Wei CL et al (2011) Role of ischemia-modified albumin and total homocysteine in estimating symptomatic lacunar infarction in type 2 diabetic patients. Clin Biochem 44:1299–1303
Madonna P, de Stefano V, Coppola A et al (2002) Hyperhomocysteinemia and other inherited prothrombotic conditions in young adults with a history of ischemic stroke. Stroke 33:51–56
Naess H, Nyland H, Idicula T, Waje-Andreassen U (2013) C-reactive protein and homocysteine predict long-term mortality in young ischemic stroke patients. J Stroke Cerebrovasc Dis 22:e435–440
Naureen A, Munazza B, Shaheen R, Khan SA, Fatima F (2012) Serum homocysteine as a risk factor for coronary heart disease. J Ayub Med Coll Abbottabad 24:59–62
O’Donnell MJ, Xavier D, Liu L et al (2010) Risk factors for ischaemic and intracerebral haemorrhagic stroke in 22 countries (the INTERSTROKE study): a case-control study. Lancet 376:112–123
Okubadejo NU, Oladipo OO, Adeyomoye AA, Awosanya GO, Danesi MA (2008) Exploratory study of plasma total homocysteine and its relationship to short-term outcome in acute ischaemic stroke in Nigerians. BMC Neurol 8:26
Petras M, Tatarkova Z, Kovalska M et al (2014) Hyperhomocysteinemia as a risk factor for the neuronal system disorders. J Physiol Pharmacol 65:15–23
Sen S, Rabinstein AA, Elkind MS, Powers WJ (2012) Recent developments regarding human immunodeficiency virus infection and stroke. Cerebrovasc Dis 33:209–218
Sobol AB, Bald E, Loba J (2005) Fractions of total plasma homocysteine in patients with ischemic stroke before the age of 55 years. Angiology 56:201–209
Song IU, Kim JS, Ryu SY et al (2009) Are plasma homocysteine levels related to neurological severity and functional outcome after ischemic stroke in the Korean population? J Neurol Sci 278:60–63
Sterne JA, Egger M (2001) Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol 54:1046–1055
Tan Y, Zhang JC, Hu XX (2009) Clinical value of serum Hcy and thrombo- precursor protein (TpP) levels determination of early diagnosis of acute cerebral infarction. J Radioimmunol 67–68
Towfighi A, Saver JL (2011) Stroke declines from third to fourth leading cause of death in the United States: historical perspective and challenges ahead. Stroke 42:2351–2355
Tranchina L, Centofanti M, Oddone F et al (2011) Levels of plasma homocysteine in pseudoexfoliation glaucoma. Graefes Arch Clin Exp Ophthalmol 249:443–448
Tu WJ, Zhao SJ, Liu TG, Yang DG, Chen H (2013) Combination of high-sensitivity C-reactive protein and homocysteine predicts the short-term outcomes of Chinese patients with acute ischemic stroke. Neurol Res 35:912–921
Turaj W, Slowik A, Wnuk M, Szczudlik A (2009) Gender-related differences in diagnostic evaluation and outcome of ischemic stroke in Poland. Stroke 40:980–982
Wang QY, Wang WJ, Wu L, Liu L, Han LZ (2013) Meta-analysis of APOE epsilon2/epsilon3/epsilon4 polymorphism and cerebral infarction. J Neural Transm 120:1479–1489
Wang RY (2014) Clinical significance of homocystein in the diagnosis of acute cerebral infarction. Lab Med Clinic 902-903
Wikstrom EA, Naik S, Lodha N, Cauraugh JH (2009) Balance capabilities after lateral ankle trauma and intervention: a meta-analysis. Med Sci Sports Exerc 41:1287–1295
Wu XQ, Ding J, Ge AY, Liu FF, Wang X, Fan W (2013) Acute phase homocysteine related to severity and outcome of atherothrombotic stroke. Eur J Intern Med 24:362–367
Xiang GQ, Feng DY, Zhao HC, Wang XJ (2014) Serum lipid and homocysteine levels in ischemic cerebrovascular disease. Chin J Health Lab Technol. 390-391
Xu SF, Xu YH (2013) Homocysteine, D-dimer and fibrinogen in patients with acute cerebral infarction. J Clin Transfusion Lab Med 241-242
Xu X, Li X, Li J, Ou R, Sheng W (2010) Meta-analysis of association between variation in the PDE4D gene and ischemic cerebral infarction risk in Asian populations. Neurogenetics 11:327–333
Ye YL, Fei XM (2014) Homocysteine and fibrinogen in the diagnosis of acute cerebral infarction. Chin J Health Lab Technol 87-89
Yoldas T, Gonen M, Godekmerdan A, Ilhan F, Bayram E (2007) The serum high-sensitive C reactive protein and homocysteine levels to evaluate the prognosis of acute ischemic stroke. Mediators Inflamm 2007:15929
Zhang W, Zhang X (2014) Correlation between the youth cerebral infarction in different TOAST classifications and high homocysteine. Cell Biochem Biophys
Zhong C, Lv L, Liu C et al (2014) High homocysteine and blood pressure related to poor outcome of acute ischemia stroke in Chinese population. PLoS One 9:e107498
Zintzaras E, Ioannidis JP (2005a) HEGESMA: genome search meta-analysis and heterogeneity testing. Bioinformatics 21:3672–3673
Zintzaras E, Ioannidis JP (2005b) Heterogeneity testing in meta-analysis of genome searches. Genet Epidemiol 28:123–137
Acknowledgments
We would like to appreciate the reviewers for their helpful comments on this paper.
Conflict of Interest
The authors have proclaimed that there are no existing competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fu, HJ., Zhao, LB., Xue, JJ. et al. Elevated Serum Homocysteine (Hcy) Levels May Contribute to the Pathogenesis of Cerebral Infarction. J Mol Neurosci 56, 553–561 (2015). https://doi.org/10.1007/s12031-015-0497-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-015-0497-6