Abstract
Purpose
The present study aimed to investigate the clinical implications of apical lymph node metastasis (ALNM) after curative resection of stage III colorectal cancer.
Methods
A retrospective study was conducted of 1403 consecutive colorectal cancer patients who underwent surgical resection at a single institution between April 2008 and January 2020. The characteristics of ALNM, the recurrence status and the relapse-free survival (RFS) were examined.
Results
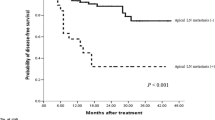
The numbers of patients with stage ≤ I, II, III, and IV disease were 350, 437, 476, and 140 patients, respectively. Among these patients with stage III disease, ALNM was seen in 21 patients (4.4% of stage III patients). Among them, curative resection was performed in 19 patients. Recurrence was observed in 68% (13/19) of the patients with ALNM who received curative resection. The first sites of recurrence included the lymph nodes 53.8% (7/13), liver 30.8% (4/13), lung 15.4% (2/13), brain 7.7% (1/13), bone 7.7% (1/13), and peritoneum 7.7% (1/13). There was no significant difference in the RFS of patients with ALNM who were managed with or without adjuvant chemotherapy (P = 0.207). Furthermore, the RFS of the group managed without adjuvant chemotherapy and the group that received adjuvant chemotherapy with/without oxaliplatin did not differ to a statistically significant extent (P = 0.318). In stage III colorectal cancer patients with ALNM, recurrence was observed significantly more frequently in comparison to stage III colorectal cancer patients without ALNM (P = 0.007). The first site of recurrence in patients with ALNM was most frequently seen in the distant lymph nodes (P = 0.004).
Conclusion
Our findings suggest that ALNM is strongly associated with recurrence in the distant lymph nodes and that it may lead to the development of systemic disease. The current regimen for stage III colorectal cancer may therefore not be sufficient for patients with stage III ALNM.



Similar content being viewed by others
References
Brierley JD, Gospodarowicz MK, Wittekind C. TNM Classification of Malignant Tumours, 8th Edition. Wiley-Blackwell, 2016.
JSfCotCa R. Japanese classification of colorectal, appendiceal, and anal carcinoma: the 3d English Edition [Secondary Publication]. J Anus Rectum Colon. 2019;3:175–95.
Kang J, Hur H, Min BS, et al. Prognostic impact of inferior mesenteric artery lymph node metastasis in colorectal cancer. Ann Surg Oncol. 2011;18:704–10.
Ang CW, Tweedle EM, Campbell F, Rooney PS. Apical node metastasis independently predicts poor survival in Dukes C colorectal cancer. Colorectal Dis. 2011;13:526–31.
Kawada H, Kurita N, Nakamura F, et al. Incorporation of apical lymph node status into the seventh edition of the TNM classification improves prediction of prognosis in stage III colonic cancer. Br J Surg. 2014;101:1143–52.
Tsai HL, Chen YT, Yeh YS, et al. Apical lymph nodes in the distant metastases and prognosis of patients with stage III colorectal cancer with adequate lymph node retrieval following FOLFOX adjuvant chemotherapy. Pathol Oncol Res. 2019;25:905–13.
Hida J, Okuno K, Yasutomi M, et al. Number versus distribution in classifying regional lymph node metastases from colon cancer. J Am Coll Surg. 2005;201:217–22.
Wang LM, Hirano YM, Ishii TM, et al. The role of apical lymph node metastasis in right colon cancer. Int J Colorectal Dis. 2020;35:1887–94.
Yi JW, Lee TG, Lee HS, et al. Apical-node metastasis in sigmoid colon or rectal cancer: is it a factor that indicates a poor prognosis after high ligation?. Int J Colorectal Dis. 2012;27:81–7.
Suzuki O, Sekishita Y, Shiono T, et al. Number of lymph node metastases is better predictor of prognosis than level of lymph node metastasis in patients with node-positive colon cancer. J Am Coll Surg. 2006;202:732–6.
Grinnell RS. Results of ligation of inferior mesenteric artery at the aorta in resections of carcinoma of the descending and sigmoid colon and rectum. Surg Gynecol Obstet. 1965;120:1031–6.
André T, Boni C, Mounedji-Boudiaf L, et al. Oxaliplatin, fluorouracil, and leucovorin as adjuvant treatment for colon cancer. N Engl J Med. 2004;350:2343–51.
Haller DG, Tabernero J, Maroun J, et al. Capecitabine plus oxaliplatin compared with fluorouracil and folinic acid as adjuvant therapy for stage III colon cancer. J Clin Oncol. 2011;29:1465–71.
Yothers G, O’Connell MJ, Allegra CJ, et al. Oxaliplatin as adjuvant therapy for colon cancer: updated results of NSABP C-07 trial, including survival and subset analyses. J Clin Oncol. 2011;29:3768–74.
Shimada Y, Hamaguchi T, Mizusawa J, et al. Randomised phase III trial of adjuvant chemotherapy with oral uracil and tegafur plus leucovorin versus intravenous fluorouracil and levofolinate in patients with stage III colorectal cancer who have undergone Japanese D2/D3 lymph node dissection: final results of JCOG0205. Eur J Cancer. 2014;50:2231–40.
Yoshida M, Ishiguro M, Ikejiri K, et al. S-1 as adjuvant chemotherapy for stage III colon cancer: a randomized phase III study (ACTS-CC trial). Ann Oncol. 2014;25:1743–9.
Acknowledgements
The authors would like to thank Dr. Keiichiro Okuyama, Dr. Hiroshi Kubo, Dr. Osamu Ikeda, Dr. Atsushi Miyoshi, and Dr. Seiji Sato who all belong to Department of Surgery, Saga Medical Center Koseikan, Saga, Japan, for treating the patients and their useful discussions. We also thank Ms. Shiori Joujima who belongs to Medical Information Division, Life Science Research Institution, Saga Medical Center Koseikan, Saga, Japan, for the data collection.
Author information
Authors and Affiliations
Contributions
M Hiraki and T Tanaka designed this study. M Hiraki, T Tanaka, H Sato, and K Kitahara treated the patients. M Hiraki and E Sadashima (specialist in statistics) analyzed the data. M Hiraki and T Tanaka interpreted the results and wrote the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
The medical ethics committee of Saga Medical Center Koseikan reviewed and approved this study design (permission number: 21–03-01–04).
Consent to Participate
All patients and their families were informed about the surgical procedure and provided their written consent. Informed broad consent for this study was obtained.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hiraki, M., Tanaka, T., Sadashima, E. et al. The Clinical Impact of Apical Lymph Node Metastasis of Colorectal Cancer After Curative Resection. J Gastrointest Canc 54, 506–512 (2023). https://doi.org/10.1007/s12029-022-00828-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-022-00828-w