Abstract
Introduction
Helicobacter pylori has been implicated in the etiopathogenesis of various malignant conditions; however, there is a dearth of studies on the correlation between H. pylori infection and pancreatic cancers. Hence, this study was carried out to evaluate the association between H. pylori infection and periampullary and pancreatic cancer.
Methods
This was a single-centre, retrospective, case–control study in which all consecutive patients of periampullary or pancreatic cancer were included. The demographic details with tumour characteristics were recorded. Age and gender-matched controls were patients with other extra-abdominal benign conditions. H. pylori and the Cag A status were determined using IgG antibodies and Cag A antibodies respectively. The association between H. pylori infection and periampullary and pancreatic cancer was the primary outcome.
Results
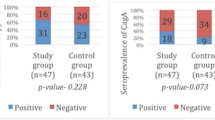
A total of 155 patients, 61 in the study and 94 in the control group were included. The overall prevalence of H. pylori in the study group (78.6%) was similar to that of the control group (76.5%) (p = 0.76). Although a higher trend of IgG and Cag A seropositivity was seen in the study group, the difference was not significant. The correlation of H. pylori and Cag A seropositivity showed a higher trend with site-specificity, differentiation, and nodal status. However, the difference was not significant.
Conclusion
There was no association between H. pylori infection and Cag A seropositivity with periampullary and pancreatic cancers. The various tumour characteristics were also not associated with H. pylori infection. Thus, routine eradication of H. pylori infection may not be recommended in periampullary and pancreatic cancers.
Similar content being viewed by others
References
Testerman TL, Morris J. Beyond the stomach: an updated view of Helicobacter pylori pathogenesis, diagnosis, and treatment. World J Gastroenterol. 2014;20:12781–808.
Kusters JG, van Vliet AHM, Kuipers EJ. Pathogenesis of Helicobacter pylori infection. Clin Microbiol Rev. American Society for Microbiology (ASM); 2006 [cited 2021 Aug 8];19:449. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1539101/.
Risch HA. Pancreatic cancer: Helicobacter pylori colonization, N-nitrosamine exposures, and ABO blood group. Mol Carcinog. 2012;51:109–18.
Trikudanathan G, Philip A, Dasanu CA, Baker WL. Association between Helicobacter pylori infection and pancreatic cancer. A cumulative meta-analysis. JOP. 2011;12:26–31.
Lee JY, Park HW, Choi JY, Lee J-S, Koo JE, Chung EJ, et al. Helicobacter pylori infection with atrophic gastritis is an independent risk factor for advanced colonic neoplasm. Gut Liver. 2016 [cited 2021 Aug 25];10:902–9. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5087929/.
Ashokkumar S, Agrawal S, Mandal J, Sureshkumar S, Sreenath GS, Kate V. Hybrid therapy versus sequential therapy for eradication of Helicobacter pylori: a randomized controlled trial. J Pharmacol Pharmacother. Wolters Kluwer — Medknow Publications; 2017 [cited 2021 Jul 27];8:62. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5497401/.
Hidalgo M. Pancreatic cancer. N Engl J Med. 2010;362:1605–17.
Miura F, Takada T, Amano H, Yoshida M, Furui S, Takeshita K. Diagnosis of pancreatic cancer. HPB (Oxford). 2006 [cited 2021 Aug 25];8:337–42. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2020745/.
Ai F, Hua X, Liu Y, Lin J, Feng Z. Preliminary study of pancreatic cancer associated with Helicobacter pylori infection. Cell Biochem Biophys. 2015;71:397–400.
Raderer M, Wrba F, Kornek G, Maca T, Koller DY, Weinlaender G, et al. Association between Helicobacter pylori infection and pancreatic cancer. OCL. Karger Publishers; 1998 [cited 2021 Aug 25];55:16–9. Available from: https://www.karger.com/Article/FullText/11830.
Tomtitchong P, Siribumrungwong B, Vilaichone R-K, Kasetsuwan P, Matsukura N, Chaiyakunapruk N. Systematic review and meta-analysis: Helicobacter pylori eradication therapy after simple closure of perforated duodenal ulcer. Helicobacter. 2012;17:148–52.
Franceschi F, Zuccalà G, Roccarina D, Gasbarrini A. Clinical effects of Helicobacter pylori outside the stomach. Nat Rev Gastroenterol Hepatol. 2014;11:234–42.
Sibony M, Jones NL. Recent advances in Helicobacter pylori pathogenesis. Curr Opin Gastroenterol. 2012;28:30–5.
Venerito M, Selgrad M, Malfertheiner P. Helicobacter pylori: gastric cancer and extragastric malignancies — clinical aspects. Helicobacter. 2013;18(Suppl 1):39–43.
Ilic M, Ilic I. Epidemiology of pancreatic cancer. World J Gastroenterol. 2016;22:9694–705.
Sikdar N, Saha G, Dutta A, Ghosh S, Shrikhande SV, Banerjee S. Genetic alterations of periampullary and pancreatic ductal adenocarcinoma: an overview. Curr Genomics. 2018;19:444–63.
Xiao M, Wang Y, Gao Y. Association between Helicobacter pylori infection and pancreatic cancer development: a meta-analysis. PLoS One. 2013;8:e75559.
Hirabayashi M, Inoue M, Sawada N, Saito E, Abe SK, Hidaka A, et al. Helicobacter pylori infection, atrophic gastritis, and risk of pancreatic cancer: a population-based cohort study in a large Japanese population: the JPHC Study. Sci Rep. 2019 [cited 2021 Aug 8];9:6099. Available from: https://www.nature.com/articles/s41598-019-42365-w.
Risch HA, Lu L, Kidd MS, Wang J, Zhang W, Ni Q, et al. Helicobacter pylori seropositivities and risk of pancreatic carcinoma. Cancer Epidemiol Biomarkers Prev. 2014;23:172–8.
Pandol SJ, Apte MV, Wilson JS, Gukovskaya AS, Edderkaoui M. The burning question: why is smoking a risk factor for pancreatic cancer? Pancreatology. 2012;12:344–9.
Rawla P, Sunkara T, Gaduputi V. Epidemiology of pancreatic cancer: global trends, etiology and risk factors. World J Oncol. 2019;10:10–27.
Li D. Diabetes and pancreatic cancer. Mol Carcinog. 2012;51:64–74.
Lee S-W, Chang C-S, Lee T-Y, Yeh H-Z, Tung C-F, Peng Y-C. Risk factors and therapeutic response in Chinese patients with peptic ulcer disease. World J Gastroenterol. 2010;16:2017–22.
Author information
Authors and Affiliations
Contributions
Vikram Kate and A. Anandhi contributed to the conception and design of the research; Vikram Kate contributed to the overall supervision and validation of the work; Giri B Laya contributed to the acquisition and analysis of the data; Vikram Kate, A. Anandhi and Jharna Mandal contributed to the interpretation of the data; Giri B Laya and Balakrishnan Gurushankari drafted and edited the manuscript under supervision. All authors critically revised the manuscript, agree to be fully accountable for ensuring the integrity and accuracy of the work, and read and approved the final manuscript.
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Laya, G.B., Anandhi, A., Gurushankari, B. et al. Association Between Helicobacter pylori and Periampullary and Pancreatic Cancer: a Case–Control Study. J Gastrointest Canc 53, 902–907 (2022). https://doi.org/10.1007/s12029-021-00766-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-021-00766-z