Abstract
Purpose
For patients receiving palliative care, information about prognosis is important to help them set priorities and expectations for care and to assist clinicians in decision-making. The purpose of this study was to investigate prognostic models applicable to the terminal stage of gastrointestinal cancer, especially in terms of accuracy of prediction regarding 3-week survival.
Methods
We validated retrospectively the accuracy of a prognosis prediction model for 354 end-stage gastrointestinal cancer patients who underwent palliative care at our hospital. Using receiver operating characteristic analysis and the area under the curve (AUC), we selected the cut-off value for 3-week survival and evaluated the predictive ability using sensitivity, specificity, positive predictive value, negative predictive value, and accurate diagnosis rate.
Results
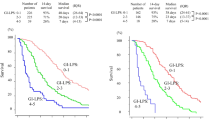
In our analysis of various models, Palliative Prognostic Index (PPI) and Biological Prognostic Score (BPS) version 3 showed excellent predictive performance with AUCs of 0.85 and 0.83, respectively, and accurate diagnosis rates of 80.0 and 79.0, respectively. BPS version 2 showed fair predictive performance with an AUC of 0.76 and an accurate diagnosis rate of 72.0. Using these models, stratification of prognostic prediction was possible.
Conclusions
PPI and BPS were found to be accurate prediction models for short-term survival of terminal gastrointestinal cancer patients.


Similar content being viewed by others
References
Glare P, Virik K, Jones M, Hudson M, Eychmuller S, Simes J, et al. A systematic review of physicians’ survival predictions in terminally ill cancer patients. BMJ (Clin Res Ed). 2003;327(7408):195–8. https://doi.org/10.1136/bmj.327.7408.195.
Maltoni M, Caraceni A, Brunelli C, Broeckaert B, Christakis N, Eychmueller S, et al. Prognostic factors in advanced cancer patients: evidence-based clinical recommendations--a study by the Steering Committee of the European Association for Palliative Care. J Clin Oncol. 2005;23(25):6240–8. https://doi.org/10.1200/JCO.2005.06.866.
Lau F, Downing GM, Lesperance M, Shaw J, Kuziemsky C. Use of Palliative Performance Scale in end-of-life prognostication. J Palliat Med. 2006;9(5):1066–75. https://doi.org/10.1089/jpm.2006.9.1066.
Morita T, Tsunoda J, Inoue S, Chihara S. The Palliative Prognostic Index: a scoring system for survival prediction of terminally ill cancer patients. Support Care Cancer. 1999;7(3):128–33.
Stiel S, Bertram L, Neuhaus S, Nauck F, Ostgathe C, Elsner F, et al. Evaluation and comparison of two prognostic scores and the physicians’ estimate of survival in terminally ill patients. Support Care Cancer. 2010;18(1):43–9. https://doi.org/10.1007/s00520-009-0628-0.
Yoong J, Atkin N, Le B. Use of the palliative prognostic index in a palliative care consultation service in Melbourne, Australia. J Pain Symptom Manag. 2010;39(1):e2–4. https://doi.org/10.1016/j.jpainsymman.2009.08.001.
Masahide O, Masahiro N, Kesashi A, et al. Development of the Biological Prognostic Score in patients with advanced cancer and prospective verification of its external validity: comparison with the Palliative Prognostic Index. Palliat Care Res. 2015;10(4):251–8 (in Japanese).
Masahide O, Saya K, Yuji Y, et al. Development of Biological Prognostic Score versions 2 and 3 for advanced cancer patients and a prospective study on the prediction accuracy: comparison with the Palliative Prognostic Index. Palliat Care Res. 2017;12(1):140–8 (in Japanese).
Shrotriya S, Walsh D, Bennani-Baiti N, Thomas S, Lorton C. C-reactive protein is an important biomarker for prognosis tumor recurrence and treatment response in adult solid tumors: a systematic review. PLoS One. 2015;10(12):e0143080. https://doi.org/10.1371/journal.pone.0143080.
Stotz M, Gerger A, Eisner F, Szkandera J, Loibner H, Ress AL, et al. Increased neutrophil-lymphocyte ratio is a poor prognostic factor in patients with primary operable and inoperable pancreatic cancer. Br J Cancer. 2013;109(2):416–21. https://doi.org/10.1038/bjc.2013.332.
Qi X, Li J, Deng H, Li H, Su C, Guo X. Neutrophil-to-lymphocyte ratio for the prognostic assessment of hepatocellular carcinoma: a systematic review and meta-analysis of observational studies. Oncotarget. 2016;7(29):45283–301. https://doi.org/10.18632/oncotarget.9942.
Smith RA, Bosonnet L, Raraty M, Sutton R, Neoptolemos JP, Campbell F, et al. Preoperative platelet-lymphocyte ratio is an independent significant prognostic marker in resected pancreatic ductal adenocarcinoma. Am J Surg. 2009;197(4):466–72. https://doi.org/10.1016/j.amjsurg.2007.12.057.
Saito H, Kono Y, Murakami Y, Shishido Y, Kuroda H, Matsunaga T, et al. Prognostic significance of platelet-based inflammatory indicators in patients with gastric cancer. World J Surg. 2018;42(8):2542–50. https://doi.org/10.1007/s00268-018-4527-8.
Yamada T, Morita T, Maeda I, Inoue S, Ikenaga M, Matsumoto Y, et al. A prospective, multicenter cohort study to validate a simple performance status-based survival prediction system for oncologists. Cancer. 2017;123(8):1442–52. https://doi.org/10.1002/cncr.30484.
Baba M, Maeda I, Morita T, Inoue S, Ikenaga M, Matsumoto Y, et al. Survival prediction for advanced cancer patients in the real world: a comparison of the Palliative Prognostic Score, Delirium-Palliative Prognostic Score, Palliative Prognostic Index and modified Prognosis in Palliative Care Study predictor model. Eur J Cancer. 2015;51(12):1618–29. https://doi.org/10.1016/j.ejca.2015.04.025.
Morishima T, Lee J, Otsubo T, Imanaka Y. Association of healthcare expenditures with aggressive versus palliative care for cancer patients at the end of life: a cross-sectional study using claims data in Japan. Int J Qual Health Care. 2014;26(1):79–86. https://doi.org/10.1093/intqhc/mzt081.
Ministry of Health Law Electronic score table of diagnosis procedure combination. https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/0000039920.html.
Zimmermann C, Burman D, Bandukwala S, Seccareccia D, Kaya E, Bryson J, et al. Nurse and physician inter-rater agreement of three performance status measures in palliative care outpatients. Support Care Cancer. 2010;18(5):609–16. https://doi.org/10.1007/s00520-009-0700-9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kadokura, M., Okuwaki, T., Imagawa, N. et al. Utility of Prognostic Prediction Models in the Terminal Stage of Gastrointestinal Cancer. J Gastrointest Canc 51, 515–519 (2020). https://doi.org/10.1007/s12029-019-00270-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-019-00270-5



