Abstract
Background
Primary duodenal adenocarcinomas (PDAC) are uncommon tumors characterized by non-specific symptoms and late diagnosis, and treatments of PDAC have some controversies.
Method
To investigate the early diagnosis and outcomes of surgical treatment of PDAC, 32 patients who were treated surgically between February 1990 and September 2006 were analyzed retrospectively.
Results
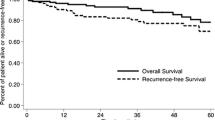
All 32 patients underwent laparotomy, including 18 patients (56.3%) with pancreaticoduodenectomy (PD), six patients (18.7%) with segmental resection (SR), and eight patients with bypass procedures. And, R0 resections were obtained in 22 patients; the other ten procedures were palliative. The total 1-, 3-, and 5-year survival rates in this study were 86.2% (25 of 29), 48.3% (14 of 29), and 20.7% (six of 29), respectively. Moreover, the 1-, 3-, and 5-year survival rates in patients with R0 resection were 100.0% (19 of 19), 73.7% (14 of 19), and 31.6% (six of 19), which were significantly higher than those (50.0% = 5/10, 0% and 0%) in patients with palliative operation (P < 0.05), respectively. Furthermore, the 5-year survival rate was 27.8% (five of 18) in pancreaticoduodenectomy patients and 16.7% (one of six) in segmental resection patients, and there was no significant difference between the above two procedures (P > 0.05).
Conclusion
PD is suggested for the tumor located at the first and second portion of the duodenum, and SR may be appropriate for the selected patients, especially for tumors of the distal duodenum.

Similar content being viewed by others
Abbreviations
- PDAC:
-
Primary duodenal adenocarcinoma
- PD:
-
Pancreaticoduodenectomy
- CT:
-
Computed tomography
- US:
-
Ultrasonography
- CA19-9:
-
CA19-9 antigen
- ALP:
-
Alkaline phosphates
- FT-207:
-
Ftorafur
References
Alwmark A, Anderson A, Lasson A. Primary carcinoma of the duodenum. Ann Surg. 1980;191(1):13–8. doi:10.1097/00000658-198001000-00003.
Egberts JH, Scharrer ML, Hinz S, Schafmayer C, Klomp HJ, Faendrich F, et al. Small bowel cancer: single-centre results over a period of 12 years. Hepatogastroenterology. 2007;54(73):129–34.
Hu JX, Miao XY, Zhong DW, Dai WD, Liu W, Hu W. Surgical treatment of primary duodenal adenocarcinoma. Hepatogastroenterology. 2006;53(72):858–62.
Shao YF, Wu TC, Shan Y, Wu JX, Wang X, Zhao P. Clinico-pathological characteristics of surgical effect on periampullary cancers: report of 631 cases. Zhonghua Yi Xue Za Zhi. 2005;85(8):510–13.
Ramia JM, Villar J, Palomeque A, Muffak K, Mansilla A, Garrote D, et al. Duodenal adenocarcinoma. Cir Esp. 2005;77(4):208–12. doi:10.1016/S0009-739X(05)70839-3.
Saiura A, Yamamoto J, Yamaguchi T. Primary duodenal carcinoma. Gan To Kagaku Ryoho. 2004;31(3):327–30.
Liu JF, Li A, Liu Q, Zhou JS, Sun JB, Li D. Surgical treatment of 475 patients with periampullary carcinoma. Zhonghua Zhong Zhong Liu Za Zhi. 2005;27(4):251–3.
Kaklamanos IG, Bathe OF, Franceschi D, Camarda C, Levi J, Livingstone AS. Extent of resection in the management of duodenal adenocarcinoma. Am J Surg. 2000;179(1):37–41. doi:10.1016/S0002-9610(99)00269-X.
Lowell JA, Rossi RL, Munson JL, Braasch JW. Primary adenocarcinoma of third and fourth portions of duodenum. Favorable prognosis after resection. Arch Surg. 1992;127(5):557–60.
American Joint Committee on Cancer. Small intestine. In: Beahrs OH, Hason DE, Hutter RVP, Kennedy BJ, editors. Manual for staging of cancer. Philadelphia: Lippincott; 1992. p. 69–73.
Declore R, Thomas JH, Forster J. Improving resectability and survival in patients with primary duodenal carcinoma. Am J Surg. 1993;166(12):626–31.
Lang H, Nadalin S, Raab R, Jahne J. Results of surgical therapy of primary adenocarcinoma of the duodenum. Chirurg. 1999;70(5):571–7. doi:10.1007/s001040050688.
Kazerooni EA, Quint LE, Francis IR. Duodenal neoplasm: predictive value of CT for determining malignancy and tumor resectability. AJR Am J Roentgenol. 1992;159(2):303–9.
Jurisic D, Doko M, Glavan E, Rosko D, Vidovic D, Tomic K. Local recurrence of primary non-ampullary adenocarcinoma of duodenum after surgical treatment–a case report and a literature review. Coll Antropo. 2006;30(1):225–9.
Santoro E, Sacchi M, Scutari F, Carboni F, Graziano F. Primary adenocarcinoma of the duodenum: treatment and survival in 89 patients. Hepatogastroenterology. 1997;44(16):1157–63.
Bucher P, Gervaz P, Morel P. Long-term results of radical resection for locally advanced duodenal adenocarcinoma. Hepatogastroenterology. 2005;52(66):1727–29.
Stell D, Mayer D, Mirza D, Buckels J. Delayed diagnosis and lower resection rate of adenocarcinoma of the distal duodenum. Dig Surg. 2004;21(5-6):434–38. doi:10.1159/000083470.
Bakaeen FG, Murr MM, Sarr MG, Thompson GB, Farnell MB, Nagorney DM, et al. What prognostic factors are important in duodenal adenocarcinoma? Arch Surg. 2000;135(6):635–41. doi:10.1001/archsurg.135.6.635.
Bal A, Joshi K, Vaiphei K, Wig JD. Primary duodenal neoplasms: a retrospective clinicopathological analysis. World J Gastroenterol. 2007;13(7):1108–111.
Yang YM, Tian XD, Zhuang Y, Wang WH, Wan YL, Huang YT. Risk factors of pancreatic leakage after pancreaticoduodenectomy. World J Gastroenterol. 2005;11(16):2456–61.
Gibson MK, Holcroft CA, Kvols LK, Haller D. Phase II study of 5-fluorouracil, doxorubicin, and mitomycin C for metastatic small bowel adenocarcinoma. Oncologist. 2005;10(2):132–7. doi:10.1634/theoncologist.10-2-132.
Author information
Authors and Affiliations
Corresponding author
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s12029-012-9385-2
Rights and permissions
About this article
Cite this article
Han, SL., Cheng, J., Zhou, HZ. et al. The Surgical Treatment and Outcome for Primary Duodenal Adenocarcinoma. J Gastrointest Canc 39, 46–50 (2008). https://doi.org/10.1007/s12029-009-9061-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-009-9061-3