Abstract
Background
Acute respiratory distress syndrome (ARDS) is an acute inflammatory respiratory failure condition that may be associated with brain injury. We aimed to describe the types of structural brain injuries detected by brain magnetic resonance imaging (MRI) among patients with ARDS.
Methods
We retrospectively reviewed and collected data on brain injuries as detected by brain MRI during index hospitalization of all patients with ARDS at a single tertiary center in the United States from January 2010 to October 2018 (pre-COVID era). Structural brain injuries were classified as cerebral ischemia (ischemic infarct and hypoxic-ischemic brain injury) or cerebral hemorrhage (intraparenchymal hemorrhage, cerebral microbleeds, subarachnoid hemorrhage, and subdural hematoma). Descriptive statistics were conducted.
Results
Of the 678 patients with ARDS, 66 (9.7%) underwent brain MRI during their ARDS illness. The most common indication for brain MRI was encephalopathy (45.4%), and the median time from hospital admission to MRI was 10 days (interquartile range 4–17). Of 66 patients, 29 (44%) had MRI evidence of brain injury, including cerebral ischemia in 33% (22 of 66) and cerebral hemorrhage in 21% (14 of 66). Among those with cerebral ischemia, common findings were bilateral globus pallidus infarcts (n = 7, 32%), multifocal infarcts (n = 5, 23%), and diffuse hypoxic-ischemic brain injury (n = 3, 14%). Of those with cerebral hemorrhage, common findings were cerebral microbleeds (n = 12, 86%) and intraparenchymal hemorrhage (n = 2, 14%). Patients with ARDS with cerebral hemorrhage had significantly greater use of rescue therapies, including prone positioning (28.6% vs. 5.8%, p = 0.03), inhaled vasodilator (35.7% vs. 11.5%, p = 0.046), and recruitment maneuver (14.3% vs. 0%, p = 0.04).
Conclusions
Structural brain injury was not uncommon among selected patients with ARDS who underwent brain MRI. The majority of brain injuries seen were bilateral globus pallidus infarcts and cerebral microbleeds.



Similar content being viewed by others
References
Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, et al. Acute respiratory distress syndrome: the Berlin definition. JAMA. 2012;307:2526–33.
Bellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A, et al. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA. 2016;315:788–800.
Sasannejad C, Ely EW, Lahiri S. Long-term cognitive impairment after acute respiratory distress syndrome: a review of clinical impact and pathophysiological mechanisms. Crit Care. 2019;23:1–12.
Hopkins RO, Weaver LK, Pope D, Orme JF, Bigler ED, Larson-Lohr V. Neuropsychological sequelae and impaired health status in survivors of severe acute respiratory distress syndrome. Am J Respir Crit Care Med. 1999;160:50–6.
Diaz-granados N, Sc M, Cooper A, Guest CB, Mazer CD, Mehta S, et al. Functional Disability 5 Years after Acute Respiratory Distress Syndrome. N Engl J. 2011;1293–304.
Herridge MS, Tansey CM, Matté A, Tomlinson G, Diaz-Granados N, Cooper A, et al. Functional disability 5 years after acute respiratory distress syndrome. N Engl J Med. 2011;364(14):1293–304.
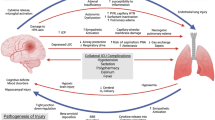
Huang M, Gedansky A, Hassett CE, Price C, Fan TH, Stephens RS, et al. Pathophysiology of brain injury and neurological outcome in acute respiratory distress syndrome: a scoping review of preclinical to clinical studies. Neurocrit Care. 2021;35(2):518–27.
Janz DR, et al. Brain autopsy findings in ICU patients previously suffering from delirium: a pilot study. J Crit Care. 2010;25(538):e7-12.
Hopkins RO, Suchyta MR, Beene K, Jackson JC. Critical illness acquired brain injury: neuroimaging and implications for rehabilitation. Rehabil Psychol. 2016;61:151–64.
Breit H, Jhaveri M, John S. Concomitant delayed posthypoxic leukoencephalopathy and critical illness microbleeds. Neurol Clin Pract. 2018;8:e31–3.
Burad J, Bhakta P, George J, Kiruchennan S. Development of acute ischemic stroke in a patient with acute respiratory distress syndrome (ARDS) resulting from H1N1 pneumonia. Acta Anaesthesiol Taiwan. 2012;50:41–5.
De Stefano P, Nencha U, De Stefano L, Mégevand P, Seeck M. Focal EEG changes indicating critical illness associated cerebral microbleeds in a Covid-19 patient. Clin Neurophysiol Pract. 2020;5:125–9.
Blanch L, Quintel M. Lung–brain cross talk in the critically ill. Intensive Care Med. 2017;43:557–9.
Bilotta F, Giordano G, Sergi PG, Pugliese F. Harmful effects of mechanical ventilation on neurocognitive functions. Crit Care. 2019;23:1–3.
Rodríguez-González R, Ramos-Nuez Á, Martín-Barrasa JL, López-Aguilar J, Baluja A, Álvarez J, et al. Endotoxin-induced lung alveolar cell injury causes brain cell damage. Exp Biol Med. 2015;240:135–42.
Aktas O, Ullrich O, Infante-Duarte C, Nitsch R, Zipp F. Neuronal damage in brain inflammation. Arch Neurol. 2007;64:185–9.
Parnet P, Kelley KW, Bluthé RM, Dantzer R. Expression and regulation of interleukin-1 receptors in the brain. Role in cytokines-induced sickness behavior. J Neuroimmunol. 2002;125:5–14.
Fries M, Bickenbach J, Henzler D, Beckers S, Dembinski R, Sellhaus B, et al. S-100 protein and neurohistopathologic changes in a porcine model of acute lung injury. Anesthesiology. 2005;102:761–7.
Kremer S, Lersy F, Anheim M, Merdji H, Schenck M, Oesterlé H, et al. Neurologic and neuroimaging findings in patients with COVID-19: a retrospective multicenter study. Neurology. 2020;95:E1868–82.
Agarwal S, Jain R, Dogra S, Krieger P, Lewis A, Nguyen V, et al. Cerebral microbleeds and leukoencephalopathy in critically Ill patients with COVID-19. Stroke. 2020;51:2649–55.
Latchaw RE, Alberts MJ, Lev MH, Connors JJ, Harbaugh RE, Higashida RT, et al. Recommendations for imaging of acute ischemic stroke: a scientific statement from the American Heart Association. Stroke. 2009;40(11):3646–78.
Huang BY, Castillo M. Hypoxic-Ischemic brain injury: Imaging findings from birth to adulthood. Radiographics. 2008;28:417–39.
Greenberg SM, Eng JA, Ning MM, Smith EE, Rosand J. Hemorrhage burden predicts recurrent intracerebral hemorrhage after lobar hemorrhage. Stroke. 2004;35:1415–20.
Hegde AN, Mohan S, Lath N, Lim CCT. Differential diagnosis for bilateral abnormalities of the basal ganglia and thalamus. Radiographics. 2011;31:5–30.
Nelson S, Toma H, LaMonica H, Chabrashvili T. Major cognitive changes and micrographia following globus pallidus infarct. Case Rep Neurol Med. 2014;2014:1–4.
Lersy F, Willaume T, Brisset JC, Collange O, Helms J, Schneider F, et al. Critical illness-associated cerebral microbleeds for patients with severe COVID-19: etiologic hypotheses. J Neurol. 2021;268:2676–84.
Kallenberg K, Dehnert C, Dörfler A, Schellinger PD, Bailey DM, Knauth M, et al. Microhemorrhages in nonfatal high-altitude cerebral edema. J Cereb Blood Flow Metab. 2008;28:1635–42.
Riech S, Kallenberg K, Moerer O, Hellen P, Bärtsch P, Quintel M, et al. The pattern of brain microhemorrhages after severe lung failure resembles the one seen in high-altitude cerebral edema. Crit Care Med. 2015;43:e386–9.
Shoskes A, Huang M, Gedansky A, Hassett C, Buletko AB, Duggal A, et al. MRI of cerebrovascular injury associated with COVID-19 and non-COVID-19 acute respiratory distress syndrome: a matched case-control study. Crit Care Med. 2022;50:1638–43.
Fanou EM, Coutinho JM, Shannon P, Kiehl TR, Levi MM, Wilcox ME, et al. Critical illness-associated cerebral microbleeds. Stroke. 2017;48:1085–7.
Liebeskind DS, Sanossian N, Sapo ML, Saver JL. Cerebral microbleeds after use of extracorporeal membrane oxygenation in children. J Neuroimaging. 2013;23:75–8.
Le Guennec L, Bertrand A, Laurent C, Roze H, Chastre J, Combes A, et al. Diffuse cerebral microbleeds after extracorporeal membrane oxygenation support. Am J Respir Crit Care Med. 2015;191(5):594–6.
Heuer JF, Pelosi P, Hermann P, Perske C, Crozier TA, Brück W, et al. Acute effects of intracranial hypertension and ARDS on pulmonary and neuronal damage: a randomized experimental study in pigs. Intensive Care Med. 2011;37:1182–91.
Massberg S, Grahl L, Von Bruehl ML, Manukyan D, Pfeiler S, Goosmann C, et al. Reciprocal coupling of coagulation and innate immunity via neutrophil serine proteases. Nat Med. 2010;16:887–96.
Iba T, Levy JH. Inflammation and thrombosis: roles of neutrophils, platelets and endothelial cells and their interactions in thrombus formation during sepsis. J Thromb Haemost. 2018;16(2):231–41.
Roberts GW, Quinn SJ, Valentine N, Alhawassi T, O’Dea H, Stranks SN, et al. Relative hyperglycemia, a marker of critical illness: introducing the stress hyperglycemia ratio. J Clin Endocrinol Metab. 2015;100:4490–7.
Patrick P, Price TO, Diogo AL, Sheibani N, Banks WA, Shah GN. Topiramate protects pericytes from glucotoxicity: role for mitochondrial CA VA in cerebromicrovascular disease in diabetes HHS public access. J Endocrinol Diabet. 2015;2:1–7.
Legras A, Caille A, Begot E, Lhéritier G, Lherm T, Mathonnet A, et al. Acute respiratory distress syndrome (ARDS)-associated acute cor pulmonale and patent foramen ovale: a multicenter noninvasive hemodynamic study. Crit Care. 2015;19:174.
Funding
None.
Author information
Authors and Affiliations
Contributions
Study concept and design: MH, AG, AD, KU, S-MC, ABB. Acquisition, analysis, or interpretation of data: MH, AG, CE.H. Statistical analysis: MH. Tables and figures: MH. First drafting of the manuscript: MH. Critical revision for important intellectual content and final approval of the manuscript: AG, AS, CE.H, AD, S-MC, KU, ABB.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflicts of interest.
Ethical Approval
All ethical guidelines and use of informed consent were followed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huang, M., Gedansky, A., Hassett, C.E. et al. Structural Brain Injury on Brain Magnetic Resonance Imaging in Acute Respiratory Distress Syndrome. Neurocrit Care 40, 187–195 (2024). https://doi.org/10.1007/s12028-023-01823-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-023-01823-0