Abstract
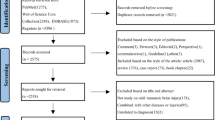
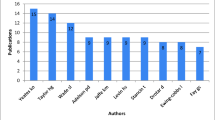
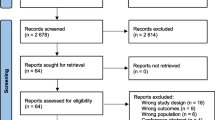
Traumatic brain injury (TBI) is the leading cause of mortality and disability among trauma-related injuries. Neuromonitoring plays an essential role in the management and prognosis of patients with severe TBI. Our bibliometric study aimed to identify the knowledge base, define the research front, and outline the social networks on neuromonitoring in severe TBI. We conducted an electronic search for articles related to neuromonitoring in severe TBI in Scopus. A descriptive analysis retrieved evidence on the most productive authors and countries, the most cited articles, the most frequently publishing journals, and the most common author’s keywords. Through a three-step network extraction process, we performed a collaboration analysis among universities and countries, a cocitation analysis, and a word cooccurrence analysis. A total of 1884 records formed the basis of our bibliometric study. We recorded an increasing scientific interest in the use of neuromonitoring in severe TBI. Czosnyka, Hutchinson, Menon, Smielewski, and Stocchetti were the most productive authors. The most cited document was a review study by Maas et al. There was an extensive collaboration among universities. The most common keywords were “intracranial pressure,” with an increasing interest in magnetic resonance imaging and cerebral perfusion pressure monitoring. Neuromonitoring constitutes an area of active research. The present findings indicate that intracranial pressure monitoring plays a pivotal role in the management of severe TBI. Scientific interest shifts to magnetic resonance imaging and individualized patient care on the basis of optimal cerebral perfusion pressure.


Similar content being viewed by others
References
Charry J, Rubiano A, Nikas C, et al. Results of early cranial decompression as an initial approach for damage control therapy in severe traumatic brain injury in a hospital with limited resources. J Neurosci Rural Pract. 2016;7(01):7–12.
Selassie A, Zaloshnja E, Langlois J, Miller T, Jones P, Steiner C. Incidence of long-term disability following traumatic brain injury hospitalization, United States, 2003. J Head Trauma Rehabil. 2008;23(2):123–31.
Teasdale G, Maas A, Lecky F, Manley G, Stocchetti N, Murray G. The Glasgow coma scale at 40 years: standing the test of time. Lancet Neurol. 2014;13(8):844–54.
Stocchetti N, Carbonara M, Citerio G, et al. Severe traumatic brain injury: targeted management in the intensive care unit. Lancet Neurol. 2017;16(6):452–64.
Makarenko S, Griesdale D, Gooderham P, Sekhon M. Multimodal neuromonitoring for traumatic brain injury: a shift towards individualized therapy. J Clin Neurosci. 2016;26:8–13.
Kirkman M, Smith M. Multimodality neuromonitoring. Anesthesiol Clin. 2016;34(3):511–23.
Smith M. Multimodality neuromonitoring in adult traumatic brain injury. Anesthesiology. 2018;128(2):401–15.
Citerio G, Oddo M, Taccone F. Recommendations for the use of multimodal monitoring in the neurointensive care unit. Curr Opin Crit Care. 2015;21(2):113–9.
Le Roux P, Menon D, Citerio G, et al. Consensus summary statement of the international multidisciplinary consensus conference on multimodality monitoring in neurocritical care. Intensive Care Med. 2014;40(9):1189–209.
Stocchetti N, Picetti E, Berardino M, et al. Clinical applications of intracranial pressure monitoring in traumatic brain injury. Acta Neurochir. 2014;156(8):1615–22.
Aria M, Cuccurullo C. bibliometrix: an R-tool for comprehensive science mapping analysis. J Informetr. 2017;11(4):959–75.
Maas A, Stocchetti N, Bullock R. Moderate and severe traumatic brain injury in adults. Lancet Neurol. 2008;7(8):728–41.
Rosner M, Rosner S, Johnson A. Cerebral perfusion pressure: management protocol and clinical results. J Neurosurg. 1995;83(6):949–62.
Chesnut R, Temkin N, Carney N, et al. A trial of intracranial-pressure monitoring in traumatic brain injury. N Engl J Med. 2012;367(26):2471–81.
Robertson C, Valadka A, Hannay H, et al. Prevention of secondary ischemic insults after severe head injury. Crit Care Med. 1999;27(10):2086–95.
Steiner L, Czosnyka M, Piechnik S, et al. Continuous monitoring of cerebrovascular pressure reactivity allows determination of optimal cerebral perfusion pressure in patients with traumatic brain injury. Crit Care Med. 2002;30(4):733–8.
Nafade V, Nash M, Huddart S, et al. A bibliometric analysis of tuberculosis research, 2007–2016. PLoS ONE. 2018;13(6):e0199706.
Syrimi E, Lewison G, Sullivan R, Kearns P. Analysis of global pediatric cancer research and publications. JCO Glob Oncol. 2020;6:9–18.
Yang C, Wang X, Tang X, Bao X, Wang R. Research trends of stem cells in ischemic stroke from 1999 to 2018: a bibliometric analysis. Clin Neurol Neurosurg. 2020;192:105740.
Hyder A, Wunderlich C, Puvanachandra P, Gururaj G, Kobusingye O. The impact of traumatic brain injuries: a global perspective. NeuroRehabilitation. 2007;22(5):341–53.
Dewan M, Rattani A, Gupta S, et al. Estimating the global incidence of traumatic brain injury. J Neurosurg. 2019;130(4):1080–97.
Barone D, Czosnyka M. Brain monitoring: do we need a hole? An update on invasive and noninvasive brain monitoring modalities. ScientificWorldJournal. 2014;2014:1–6.
Weerakkody R, Czosnyka M, Zweifel C, et al. Near infrared spectroscopy as possible non-invasive monitor of slow vasogenic ICP waves. Acta Neurochir Suppl. 2012;181–5.
Cardim D, Robba C, Bohdanowicz M, et al. Non-invasive monitoring of intracranial pressure using transcranial doppler ultrasonography: is it possible? Neurocrit Care. 2016;25(3):473–91.
Nag D, Sahu S, Swain A, Kant S. Intracranial pressure monitoring: gold standard and recent innovations. World J Clin Cases. 2019;7(13):1535–53.
Isa R, Adnan W, Ghazali G, et al. Outcome of severe traumatic brain injury: comparison of three monitoring approaches. Neurosurg Focus. 2003;15(6):1–7.
Meixensberger J. Brain tissue oxygen guided treatment supplementing ICP/CPP therapy after traumatic brain injury. J Neurol Neurosurg Psychiatsry. 2003;74(6):760–4.
Lauritzen M, Dreier JP, Fabricius M, Hartings JA, Graf R, Strong AJ. Clinical relevance of cortical spreading depression in neurological disorders: migraine, malignant stroke, subarachnoid and intracranial hemorrhage, and traumatic brain injury. J Cereb Blood Flow Metab. 2011;31(1):17–35. https://doi.org/10.1038/jcbfm.2010.191.
Aarabi B, Hesdorffer DC, Ahn ES, Aresco C, Scalea TM, Eisenberg HM. Outcome following decompressive craniectomy for malignant swelling due to severe head injury. J Neurosurg. 2006;104(4):469–79. https://doi.org/10.3171/jns.2006.104.4.469.
Kang SK, Murphy RK, Hwang SW, Lee SM, Harburg DV, Krueger NA, Shin J, Gamble P, Cheng H, Yu S, Liu Z, McCall JG, Stephen M, Ying H, Kim J, Park G, Webb RC, Lee CH, Chung S, Wie DS, Gujar AD, Vemulapalli B, Kim AH, Lee KM, Cheng J, Huang Y, Lee SH, Braun PV, Ray WZ, Rogers JA. Bioresorbable silicon electronic sensors for the brain. Nature. 2016;530(7588):71–6. https://doi.org/10.1038/nature16492.
Rovlias A, Kotsou S. The influence of hyperglycemia on neurological outcome in patients with severe head injury. Neurosurgery. 2000;46(2):335–42. https://doi.org/10.1097/00006123-200002000-00015.
Polderman KH. Application of therapeutic hypothermia in the intensive care unit. Intensive Care Med. 2004;30(5):757–69. https://doi.org/10.1007/s00134-003-2151-y.
Manley G. Hypotension, hypoxia, and head injury: frequency, duration, and consequences. Arch Surg. 2001;136(10):1118. https://doi.org/10.1007/s00134-003-2151-y.
Stiefel MF, Spiotta A, Gracias VH, Garuffe AM, Guillamondegui O, Maloney-Wilensky E, Bloom S, Grady MS, LeRoux PD. Reduced mortality rate in patients with severe traumatic brain injury treated with brain tissue oxygen monitoring. J Neurosurg. 2005;103(5):805–11. https://doi.org/10.3171/jns.2005.103.5.0805.
Vespa PM, Miller C, McArthur D, Eliseo M, Etchepare M, Hirt D, Glenn TC, Martin N, Hovda D. Nonconvulsive electrographic seizures after traumatic brain injury result in a delayed, prolonged increase in intracranial pressure and metabolic crisis. Crit Care Med. 2007;35(12):2830–6. https://doi.org/10.1097/00003246-200712000-00023.
Aries MJ, Czosnyka M, Budohoski KP, Steiner LA, Lavinio A, Kolias AG, Hutchinson PJ, Brady KM, Menon DK, Pickard JD, Smielewski P. Continuous determination of optimal cerebral perfusion pressure in traumatic brain injury. Crit Care Med. 2012;40(8):2456–63. https://doi.org/10.1097/CCM.0b013e3182514eb6.
Bulger EM, Nathens AB, Rivara FP, Moore M, MacKenzie EJ, Jurkovich GJ. Management of severe head injury: institutional variations in care and effect on outcome. Crit Care Med. 2002;30(8):1870–6. https://doi.org/10.1097/00003246-200208000-00033.
Geeraerts T, Launey Y, Martin L, Pottecher J, Vigué B, Duranteau J, Benhamou D. Ultrasonography of the optic nerve sheath may be useful for detecting raised intracranial pressure after severe brain injury. Intensive Care Med. 2007;33(10):1704–11. https://doi.org/10.1007/s00134-007-0797-6.
Holloway KL, Barnes T, Choi S, Bullock R, Marshall LF, Eisenberg HM, Jane JA, Ward JD, Young HF, Marmarou A. Ventriculostomy infections: the effect of monitoring duration and catheter exchange in 584 patients. J Neurosurg. 1996;85(3):419–24. https://doi.org/10.3171/jns.1996.85.3.0419.
Rosenfeld JV, Maas AI, Bragge P, Morganti-Kossmann MC, Manley GT, Gruen RL. Early management of severe traumatic brain injury. Lancet. 2012;380(9847):1088–98. https://doi.org/10.1016/S0140-6736(12)60864-2.
Timofeev I, Carpenter KL, Nortje J, Al-Rawi PG, O’Connell MT, Czosnyka M, Smielewski P, Pickard JD, Menon DK, Kirkpatrick PJ, Gupta AK, Hutchinson PJ. Cerebral extracellular chemistry and outcome following traumatic brain injury: a microdialysis study of 223 patients. Brain. 2011;134(2):484–94. https://doi.org/10.1093/brain/awq353.
Bouma G, Muizelaar J, Bandoh K, Marmarou A. Blood pressure and intracranial pressure-volume dynamics in severe head injury: relationship with cerebral blood flow. J Neurosurg. 1992;77(1):15–9. https://doi.org/10.3171/jns.1992.77.1.0015.
Le Roux P, Menon DK, Citerio G, Vespa P, Bader MK, Brophy GM, Diringer MN, Stocchetti N, Videtta W, Armonda R, Badjatia N, Böesel J, Chesnut R, Chou S, Claassen J, Czosnyka M, De Georgia M, Figaji A, Fugate J, Helbok R, Horowitz D, Hutchinson P, Kumar M, McNett M, Miller C, Naidech A, Oddo M, Olson D, O'Phelan K, Provencio JJ, Puppo C, Riker R, Robertson C, Schmidt M, Taccone F. Consensus summary statement of the international multidisciplinary consensus conference on multimodality monitoring in neurocritical care. Neurocrit Care. 2014;21(S2):1–26. https://doi.org/10.1007/s12028-014-0041-5
Carney N, Totten AM, O’Reilly C, et al. Guidelines for the Management of Severe Traumatic Brain Injury, 4th Edition. Brain Trauma Foundation. 2016. https://braintrauma.org/uploads/03/12/Guidelines_for_Management_of_Severe_TBI_4th_Edition.pdf.
Funding
No funding was received for our study.
Author information
Authors and Affiliations
Contributions
MK: conceptualization, investigation, writing original draft, methodology, writing review, and editing. AB: conceptualization, investigation; writing original draft, methodology, formal analysis, visualization, writing review, and editing. CG: conceptualization, validation, writing review, and editing. TK: writing review and editing. CV: writing review and editing. GS: writing review and editing. KF: conceptualization, writing review, editing, project administration, and supervision. All contributing authors have approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of Interest
I would like to declare that no conflict of interest, financial or any ethical issue resulting from the publication of this manuscript exists.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
12028_2021_1428_MOESM2_ESM.tiff
Figure 2. Three larger and three smaller groups were recognized in the co-word analysis network, according to the author’s keyword co-occurrence. (TIFF 2990 kb)
12028_2021_1428_MOESM4_ESM.png
Figure 4. A schematic representation of the significant international collaborations between institutions (top figure) and between countries (bottom figure) regarding the usage of neuromonitoring in sTBI patients. (PNG 862 kb)
12028_2021_1428_MOESM5_ESM.png
Figure 5. A schematic representation demonstrating a dense co-work analysis network according to the author’s co-citation analysis. (PNG 868 kb)
Rights and permissions
About this article
Cite this article
Karagianni, M.D., Brotis, A.G., Gatos, C. et al. Neuromonitoring in Severe Traumatic Brain Injury: A Bibliometric Analysis. Neurocrit Care 36, 1044–1052 (2022). https://doi.org/10.1007/s12028-021-01428-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-021-01428-5