Abstract
Background and Objective
Malignant cerebral edema (MCE) is a well-known complication in patients with acute ischemic stroke with core infarcts ≥ 80 mL caused by large-vessel occlusions. MCE can also develop in patients with smaller infarcts with moderate -to-large volume of tissue at risk who do not achieve successful revascularization with endovascular thrombectomy (ET). Features that predict the development of MCE in this population are not well-described. We aim to identify predictors of MCE and 90-day functional outcome in stroke patients with an anterior circulation large vessel occlusion (LVO) and a < 80 mL ischemic core who do not achieve complete reperfusion.
Methods
We reviewed our institutional stroke registry and included patients who achieved unsuccessful revascularization, mTICI 0-2a, after ET and whose baseline imaging was notable for a core infarct < 80 mL, a Tmax > 6 s volume ≥ 80 mL, and a mismatch ratio ≥ 1.8. MCE was defined as ≥ 5 mm of midline shift on follow-up imaging, obtained 6–48 h after the pre-ET perfusion scan.
Results
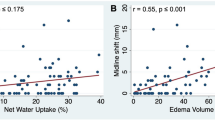
Thirty-six patients met inclusion criteria. Unadjusted analysis demonstrated that younger age, higher systolic blood pressure, larger core volume, and higher hypoperfusion intensity ratio (HIR) were associated with MCE (all p < 0.02). In multivariate logistic regression analysis, age, HIR, and core infarct volume were independent predictors of MCE. The optimal HIR threshold to predict MCE was ≥ 0.54 (OR 14.7, 95% CI 2.4–78.0, p = 0.003). HIR was also associated with 3-month mRS (HIR ≥ 0.54 for mRS of 3–6: OR 10.8, 95% CI 1.9–44.0, p = 0.02).
Conclusions
Younger age, larger core infarct volume, and higher HIR are predictive of MCE in patients with anterior circulation LVO, moderate-to-large tissue at risk, and suboptimal revascularization. HIR is correlated with three-month functional outcomes.





Similar content being viewed by others
References
Thomalla G, Hartmann F, Juettler E, et al. Prediction of malignant middle cerebral artery infarction by magnetic resonance imaging within 6 hours of symptom onset: a prospective multicenter observational study. Ann Neurol. 2010;68:435–45.
Mlynash M, Lansberg MG, De Silva DA, et al. Refining the definition of the malignant profile: insights from the DEFUSE-EPITHET pooled data set. Stroke. 2011;42:1270–5.
Arenillas JF, Rovira A, Molina CA, Grive E, Montaner J, Alvarez-Sabin J. Prediction of early neurological deterioration using diffusion- and perfusion-weighted imaging in hyperacute middle cerebral artery ischemic stroke. Stroke. 2002;33:2197–203.
Wijdicks EF, Sheth KN, Carter BS, et al. Recommendations for the management of cerebral and cerebellar infarction with swelling: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2014;45:1222–38.
Huang X, Yang Q, Shi X, et al. Predictors of malignant brain edema after mechanical thrombectomy for acute ischemic stroke. J Neurointerv Surg. 2019;11:994–8.
Kimberly WT, Dutra BG, Boers AMM, et al. Association of reperfusion with brain Edema in Patients with acute ischemic stroke: a secondary analysis of the MR CLEAN trial. JAMA Neurol. 2018;75:453–61.
Irvine HJ, Ostwaldt AC, Bevers MB, et al. Reperfusion after ischemic stroke is associated with reduced brain edema. J Cereb Blood Flow Metab. 2018;38:1807–17.
Goyal M, Menon BK, van Zwam WH, et al. Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet. 2016;387:1723–31.
Nogueira RG, Jadhav AP, Haussen DC, et al. Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med. 2018;378:11–21.
Marks MP, Heit JJ, Lansberg MG, et al. Endovascular treatment in the DEFUSE 3 study. Stroke. 2018;49:2000–3.
Bang OY, Saver JL, Alger JR, et al. Determinants of the distribution and severity of hypoperfusion in patients with ischemic stroke. Neurology. 2008;71:1804–11.
Nicoli F, Lafaye de Micheaux P, Girard N. Perfusion-weighted imaging-derived collateral flow index is a predictor of MCA M1 recanalization after i.v. thrombolysis. AJNR Am J Neuroradiol. 2013;34:107–14.
Wheeler HM, Mlynash M, Inoue M, et al. Early diffusion-weighted imaging and perfusion-weighted imaging lesion volumes forecast final infarct size in DEFUSE 2. Stroke. 2013;44:681–5.
Olivot JM, Mlynash M, Inoue M, et al. Hypoperfusion intensity ratio predicts infarct progression and functional outcome in the DEFUSE 2 Cohort. Stroke. 2014;45:1018–23.
Campbell BC, Mitchell PJ, Kleinig TJ, et al. Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med. 2015;372:1009–18.
Albers GW, Marks MP, Kemp S, et al. Thrombectomy for Stroke at 6 to 16 Hours with Selection by Perfusion Imaging. N Engl J Med. 2018;378:708–18.
Ong CJ, Gluckstein J, Laurido-Soto O, Yan Y, Dhar R, Lee JM. Enhanced detection of edema in malignant anterior circulation stroke (EDEMA) score: a risk prediction tool. Stroke. 2017;48:1969–72.
von Kummer R, Broderick JP, Campbell BC, et al. The Heidelberg bleeding classification: classification of bleeding events after ischemic stroke and reperfusion therapy. Stroke. 2015;46:2981–6.
Saver JL. Time is brain–quantified. Stroke. 2006;37:263–6.
Oppenheim C, Samson Y, Manai R, et al. Prediction of malignant middle cerebral artery infarction by diffusion-weighted imaging. Stroke. 2000;31:2175–81.
Lee SJ, Lee KH, Na DG, et al. Multiphasic helical computed tomography predicts subsequent development of severe brain edema in acute ischemic stroke. Arch Neurol. 2004;61:505–9.
Ryoo JW, Na DG, Kim SS, et al. Malignant middle cerebral artery infarction in hyperacute ischemic stroke: evaluation with multiphasic perfusion computed tomography maps. J Comput Assist Tomogr. 2004;28:55–62.
Dittrich R, Kloska SP, Fischer T, et al. Accuracy of perfusion-CT in predicting malignant middle cerebral artery brain infarction. J Neurol. 2008;255:896–902.
Funding
The study was not funded.
Author information
Authors and Affiliations
Contributions
This manuscript complies with all instructions to authors. The authorship requirements have been met and the final manuscript was approved by all authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed Consent
This study complied with the Health Insurance Portability and Accountability Act and was approved by our Institutional Review Board, which waived the need for written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Murray, N.M., Culbertson, C.J., Wolman, D.N. et al. Hypoperfusion Intensity Ratio Predicts Malignant Edema and Functional Outcome in Large-Vessel Occlusive Stroke with Poor Revascularization. Neurocrit Care 35, 79–86 (2021). https://doi.org/10.1007/s12028-020-01152-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-01152-6