Abstract
Background
Endoplasmic reticulum stress (ERS) plays a vital role in mediating apoptosis in the brain following cardiac arrest (CA). Studies have shown that therapeutic hypothermia (TH) provides neuroprotection through anti-apoptosis; however, the effects of temperature variability in TH on the brain remain unclear. In this study, we investigated the different effects of temperature variability through extracorporeal membrane oxygenation on apoptosis and ERS in the brain following CA.
Methods
Eighteen male domestic pigs underwent 6-min duration of no-flow induced by ventricular fibrillation. Extracorporeal cardiopulmonary resuscitation was then performed, and the return of spontaneous circulation (ROSC) was achieved. The animals were randomly assigned to the following groups: normothermia, non-temperature variability, and temperature variability. TH (core temperature, 33–35 °C) was maintained for 24 h post-ROSC, and the animals were rewarmed for 8 h. Quantitative real-time polymerase chain reaction (qRT-PCR) and immunohistochemistry for Bax and Bcl-2 transcripts and proteins, respectively, were used to investigate apoptosis in the cerebral cortex. Expression levels of the ERS molecules, GRP78 and CHOP, were also detected by qRT-PCR, and cellular morphology was evaluated using transmission electron microscopy.
Results
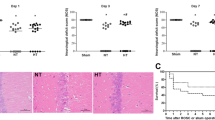
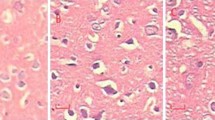
qRT-PCR and immunohistochemistry results revealed that TH significantly increased the expression levels of Bcl-2 and GRP78 and decreased that of Bax and CHOP than under normothermia conditions. Compared to the non-temperature variability group, temperature variability did not decrease the expression levels of Bcl-2 and GRP78 and not increase the levels of Bax and CHOP. Endoplasmic reticulum ultrastructural changes were significantly improved under TH. No statistical difference was observed between the temperature variability and non-temperature variability groups.
Conclusion
TH can reduce neuronal apoptosis by ERS, while temperature variability does not attenuate this beneficial effect.






Similar content being viewed by others
Abbreviations
- ERS:
-
Endoplasmic reticulum stress
- CA:
-
Cardiac arrest
- TH:
-
Therapeutic hypothermia
- ECMO:
-
Extracorporeal membrane oxygenation
- VF:
-
Ventricular fibrillation
- ECPR:
-
Extracorporeal cardiopulmonary resuscitation
- ROSC:
-
Return of spontaneous circulation
- qRT-PCR:
-
Quantitative real-time polymerase chain reaction
References
Lemiale V, Dumas F, Mongardon N, et al. Intensive care unit mortality after cardiac arrest: the relative contribution of shock and brain injury in a large cohort. Intensive Care Med. 2013;39(11):1972–80.
Callaway CW, Donnino MW, Fink EL, et al. Part 8: post-Cardiac Arrest Care: 2015 American Heart Association Guidelines Update For Cardiopulmonary Resuscitation And Emergency Cardiovascular Care. Circulation. 2015;132(18 Suppl 2):S465–82.
Mackowiak PA. Drug fever: mechanisms, maxims and misconceptions. Am J Med Sci. 1987;294(4):275–86.
Gaussorgues P, Gueugniaud PY, Vedrinne JM, et al. Bacteremia following cardiac arrest and cardiopulmonary resuscitation. Intensive Care Med. 1988;14(5):575–7.
Tommasi E, Lazzeri C, Bernardo P, et al. Cooling techniques in mild hypothermia after cardiac arrest. J Cardiovasc Med (Hagerstown). 2017;18(7):459–66.
Suffoletto B, Peberdy MA, van der Hoek T, et al. Body temperature changes are associated with outcomes following in-hospital cardiac arrest and return of spontaneous circulation. Resuscitation. 2009;80(12):1365–70.
Shinozaki K, Oda S, Sadahiro T, et al. Duration of well-controlled core temperature correlates with neurological outcome in patients with post-cardiac arrest syndrome. Am J Emerg Med. 2012;30(9):1838–44.
Nobile L, Lamanna I, Fontana V, et al. Greater temperature variability is not associated with a worse neurological outcome after cardiac arrest. Resuscitation. 2015;96:268–74.
Nayeri A, Bhatia N, Holmes B, et al. Temperature variability during targeted temperature management is not associated with neurological outcomes following cardiac arrest. Am J Emerg Med. 2017;35(6):889–92.
Pinichjindasup A, Homvises B, Muengtaweepongsa S. Therapeutic hypothermia with extracorporeal membrane oxygenation (ECMO) and surface cooling in post-cardiac arrest patients: 4 case reports. J Med Assoc Thail. 2014;97:S223–7.
Jaw SP, Su DD, Truong DD. Expression of Bcl-2 and Bax in the frontoparietal cortex of the rat following cardiac arrest. Brain Res Bull. 1995;38(6):577–80.
Nozari A, Safar P, Stezoski SW, et al. Critical time window for intra-arrest cooling with cold saline flush in a dog model of cardiopulmonary resuscitation. Circulation. 2006;113(23):2690–6.
Gong P, Hua R, Zhang Y, et al. Hypothermia-induced neuroprotection is associated with reduced mitochondrial membrane permeability in a swine model of cardiac arrest. J Cereb Blood Flow Metab. 2013;33(6):928–34.
Suh GJ, Kwon WY, Kim KS, et al. Prolonged therapeutic hypothermia is more effective in attenuating brain apoptosis in a Swine cardiac arrest model. Crit Care Med. 2014;42(2):e132–42.
Gong P, Li CS, Hua R, et al. Mild hypothermia attenuates mitochondrial oxidative stress by protecting respiratory enzymes and upregulating MnSOD in a pig model of cardiac arrest. PLoS ONE. 2012;7(4):e35313.
Stuss DT, Levine B. Adult clinical neuropsychology: lessons from studies of the frontal lobes. Annu Rev Psychol. 2002;53:401–33.
Püttgen HA, Geocadin R. Predicting neurological outcome following cardiac arrest. J Neurol Sci. 2007;261(1–2):108–17.
Tahsili-Fahadan P, Farrokh S, Geocadin RG. Hypothermia and brain inflammation after cardiac arrest. Brain Circ. 2018;4(1):1–13.
Wu L, Sun HL, Gao Y, et al. Therapeutic hypothermia enhances cold-inducible RNA-binding protein expression and inhibits mitochondrial apoptosis in a rat model of cardiac arrest. Mol Neurobiol. 2017;54(4):2697–705.
Nguyen TP, Chen MH, Li N, et al. PD98059 protects brain against cells death resulting from ROS/ERK activation in a cardiac arrest rat model. Oxid Med Cell Longev. 2016;2016:3723762.
Rasheva VI, Domingos PM. Cellular responses to endoplasmic reticulum stress and apoptosis. Apoptosis. 2009;14(8):996–1007.
Kim I, Xu W, Reed JC. Cell death and endoplasmic reticulum stress: disease relevance and therapeutic opportunities. Nat Rev Drug Discov. 2008;7(12):1013–30.
Walter P, Ron D. The unfolded protein response: from stress pathway to homeostatic regulation. Science. 2011;334(6059):1081–6.
Zhang K, Kaufman RJ. From endoplasmic-reticulum stress to the inflammatory response. Nature. 2008;454(7203):455–62.
Marciniak SJ, Yun CY, Oyadomari S, et al. CHOP induces death by promoting protein synthesis and oxidation in the stressed endoplasmic reticulum. Genes Dev. 2004;18(24):3066–77.
Liu X, Wang M, Chen H, et al. Hypothermia protects the brain from transient global ischemia/reperfusion by attenuating endoplasmic reticulum response-induced apoptosis through CHOP. PLoS ONE. 2013;8(1):e53431.
Cordoza M, Thompson H, Bridges E, et al. Association between target temperature variability and neurologic outcomes for patients receiving targeted temperature management at 36 C after cardiac arrest: a retrospective cohort study. Ther Hypothermia Temp Manag. 2020. https://doi.org/10.1089/ther.2020.0005.
Yannopoulos D, Zviman M, Castro V, et al. Intra-cardiopulmonary resuscitation hypothermia with and without volume loading in an ischemic model of cardiac arrest. Circulation. 2009;120(14):1426–35.
Nielsen N, Wetterslev J, Cronberg T, et al. Targeted temperature management at 33 °C versus 36 °C after cardiac arrest. N Engl J Med. 2013;369(23):2197–206.
Acknowledgements
We gratefully acknowledge the support of National Natural Science Foundation of China for this research, Grant Number 81927808, grant recipient Wenkui Yu. We would like to thank Editage (www.editage.cn) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Source of support
We received the support of National Natural Science Foundation of China for this research, grant number 81927808.
Conflicts of interest
The authors declare that they have no conflict of interest.
Human and Animal Rights
All applicable institutional and/or national guidelines for the care and use of animals were followed. The experiment was conducted in conformity with the guidance suggestions for the care and use of laboratory animals formulated by the Ministry of Science and Technology of the People’s Republic of China.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, B., Gu, Q., Chen, X. et al. Temperature Variability Does Not Attenuate the Beneficial Effects of Therapeutic Hypothermia on Cellular Apoptosis and Endoplasmic Reticulum Stress in the Cerebral Cortex of a Swine Cardiac Arrest Model. Neurocrit Care 34, 769–780 (2021). https://doi.org/10.1007/s12028-020-01083-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-01083-2