Abstract
Background
Early cerebral hypoperfusion and ischemia occur after subarachnoid hemorrhage (SAH) and influence clinical prognosis. Pathophysiological mechanisms possibly involve inflammatory mediators. TNF-α has been associated with complications and prognosis after SAH. We investigated the relation of perfusion parameters and ischemic lesions, with levels of TNF-α main receptor, TNF-R1, after SAH, and their association with prognosis.
Methods
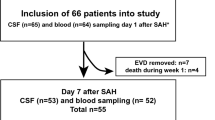
We included consecutive SAH patients admitted within the first 72 h of SAH onset. Blood samples were simultaneously collected from a peripheral vein and from the parent artery of the aneurysm. Levels of TNF-R1 were measured using ELISA (R&D Systems Inc., USA). CT perfusion and MRI studies were performed in the first 72 h. Correlation and logistic regression analysis were used to identify outcome predictors.
Results
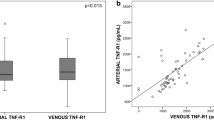
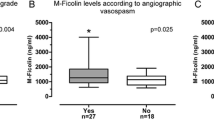
We analyzed 41 patients. Increased levels of TNF-R1 correlated with increased Tmax (arterial: r = −0.37, p = 0.01) and prolonged MTT (arterial: r = 0.355, p = 0.012; venous: r = 0.306, p = 0.026). Increased levels of both arterial and venous TNF-R1 were associated with increased number of lesions on DWI (p = 0.006). In multivariate analysis, venous TNFR1 levels > 1742.2 pg/mL (OR 1.78; 95%CI 1.18–2.67; p = 0.006) and DWI lesions (OR 14.01; 95%CI 1.19–165.3; p = 0.036) were both independent predictors of poor outcome (mRS ≥ 3) at 6 months.
Conclusion
Increased levels of TNF-R1 in arterial and venous blood correlate with worse cerebral perfusion and with increased burden of acute ischemic lesions in the first 72 h after SAH. Venous levels of TNF-R1 and DWI lesions were associated with poor outcome at 6 months. These results highlight the pathophysiological role of TNF-α pathways in SAH and suggest a possible role of combined imaging and laboratorial markers in determining prognosis in acute SAH.

Similar content being viewed by others
References
Hop JW, Rinkel GJE, Algra A, van Gijn J. Case-fatality rates and functional outcome after subarachnoid hemorrhage: a systematic review. Stroke. 1997;28(3):660–4.
Rosengart AJ, Schultheiss KE, Tolentino J, Macdonald RL. Prognostic factors for outcome in patients with aneurysmal subarachnoid hemorrhage. Stroke. 2007;38(8):2315–21.
Vergouwen MDI, Ilodigwe D, MacDonald RL. Cerebral infarction after subarachnoid hemorrhage contributes to poor outcome by vasospasm-dependent and -independent effects. Stroke. 2011;42(4):924–9.
Dumont AS, Dumont RJ, Chow MM, et al. Cerebral vasospasm after subarachnoid hemorrhage: putative role of inflammation. Neurosurgery. 2003;53(1):123–5.
Hong CM, Tosun C, Kurland DB, Gerzanich V. Biomarkers as outcome predictors in subarachnoid hemorrhage—a systematic review. Biomarkers. 2014;19(2):95–108.
Jordan JD, Nyquist P. Biomarkers and vasospasm after aneurysmal subarachnoid hemorrhage. Neurosurg Clin N Am. 2010;21(2):381–91.
Chou SH, Feske SK, Atherton J, et al. Early elevation of serum TNFα is associated with poor outcome in subarachnoid hemorrhage. J Investig Med. 2012;60(7):1054–8.
Mathiesen T, Edner G, Ulfarsson E, Andersson B. Cerebrospinal fluid interleukin-1 receptor antagonist and tumor necrosis factor-alpha following subarachnoid hemorrhage. J Neurosurg. 1997;87(2):215–20.
Vikman P, Beg S, Khurana TS, Khurana T, Hansen-Schwartz J, Edvinsson L. Gene expression and molecular changes in cerebral arteries following subarachnoid hemorrhage in the rat. J Neurosurg. 2006;105(3):438–44.
Young AMH, Karri SK, You W, Ogilvy CS. Specific TNF-alpha inhibition in cerebral aneurysm formation and subarachnoid hemorrhage. Curr Drug Saf. 2012;7(3):190–6.
Fragata I, Bustamante A, Penalba A, et al. Venous and arterial TNF-R1 predicts outcome and complications in acute subarachnoid hemorrhage. Neurocrit Care. 2019;31(1):107–15.
Mir DI, Gupta A, Dunning A, et al. CT perfusion for detection of delayed cerebral ischemia in aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis. AJNR Am J Neuroradiol. 2014;35(5):866–71.
Cremers CHP, van der Schaaf IC, Wensink E, et al. CT perfusion and delayed cerebral ischemia in aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis. J Cereb Blood Flow Metab. 2014;34(2):200–7.
Rosenstein J, Suzuki M, Symon L, Redmond S. Clinical use of a portable bedside cerebral blood flow machine in the management of aneurysmal subarachnoid hemorrhage. Neurosurgery. 1984;15(4):519–25.
Honda M, Sase S, Yokota K, et al. Early cerebral circulatory disturbance in patients suffering subarachnoid hemorrhage prior to the delayed cerebral vasospasm stage: xenon computed tomography and perfusion computed tomography study. Neurol Med Chir (Tokyo). 2012;52(7):488–94.
Rodriguez-Régent C, Hafsa M, Turc G, et al. Early quantitative CT perfusion parameters variation for prediction of delayed cerebral ischemia following aneurysmal subarachnoid hemorrhage. Eur Radiol. 2016;26(9):2956–63.
Sanelli PC, Jou A, Gold R, et al. Using CT perfusion during the early baseline period in aneurysmal subarachnoid hemorrhage to assess for development of vasospasm. Neuroradiology. 2011;53(6):425–34.
van Gijn J, Hijdra A, Wijdicks EF, Vermeulen M, van Crevel H. Acute hydrocephalus after aneurysmal subarachnoid hemorrhage. J Neurosurg. 1985;63(3):355–62.
Frontera JA, Claassen J, Schmidt JM, et al. Prediction of symptomatic vasospasm after subarachnoid hemorrhage: the modified fisher scale. Neurosurgery. 2006;59(1):21–7.
Hijdra A, Brouwers PJ, Vermeulen M, van Gijn J. Grading the amount of blood on computed tomograms after subarachnoid hemorrhage. Stroke. 1990;21(8):1156–61.
Frontera JA, Fernandez A, Schmidt JM, et al. Defining vasospasm after subarachnoid hemorrhage: what is the most clinically relevant definition? Stroke. 2009;40(6):1963–8.
Vergouwen MDI, Vermeulen M, Muizelaar JP, et al. Definition of delayed cerebral ischemia after aneurysmal subarachnoid hemorrhage as an outcome event in clinical trials and observational studies proposal of a multidisciplinary research group. Stroke. 2010;41:2391–5.
Janssen PM, Visser NA, Dorhout Mees SM, Klijn CJM, Algra A, Rinkel GJE. Comparison of telephone and face-to-face assessment of the modified Rankin Scale. Cerebrovasc Dis. 2010;29(2):137–9.
Kudo K, Sasaki M, Ogasawara K, Terae S, Ehara S, Shirato H. Difference in tracer delay-induced effect among deconvolution algorithms in CT perfusion analysis: quantitative evaluation with digital phantoms. Radiology. 2009;251(1):241–9.
Rodríguez-Rodríguez A, Egea-Guerrero JJ, Ruiz De Azúa-López Z, Murillo-Cabezas F. Biomarkers of vasospasm development and outcome in aneurysmal subarachnoid hemorrhage. J Neurol Sci. 2014;341:1–2.
Lucke-Wold BP, Logsdon AF, Manoranjan B, et al. Aneurysmal subarachnoid hemorrhage and neuroinflammation: a comprehensive review. Int J Mol Sci. 2016;17(4):1–17.
Pantoni L, Sarti C, Inzitari D. Cytokines and cell adhesion molecules in cerebral ischemia: experimental bases and therapeutic perspectives. Arterioscler Thromb Vasc Biol. 1998;18(4):503–13.
Grell M, Zimmermann G, Hülser D, Pfizenmaier K, Scheurich P. TNF receptors TR60 and TR80 can mediate apoptosis via induction of distinct signal pathways. J Immunol. 1994;153(5):1963–72.
Frontera JA, Ahmed W, Zach V, et al. Acute ischaemia after subarachnoid haemorrhage, relationship with early brain injury and impact on outcome: a prospective quantitative MRI study. J Neurol Neurosurg Psychiatry. 2015;86(1):71–8.
Mckeating EG, Andrews PJD, Signorini DF, Mascia L. Transcranial cytokine gradients in patients requiring intensive care after acute brain injury. Br J Anaesth. 1997;78(5):520–3.
Elkind MS, McClure LA, Luna JM, Del Brutto OH, Pikula A, Benavente OR. Abstract 219: tumor necrosis factor receptor 1 and subclinical cerebrovascular disease: the levels of inflammatory markers in treatment of stroke Study. Stroke. 2016;47(suppl_1):A219–A219.
Zheng R, Qin L, Li S, Xu K, Geng H. CT perfusion-derived mean transit time of cortical brain has a negative correlation with the plasma level of Nitric Oxide after subarachnoid hemorrhage. Acta Neurochir (Wien). 2014;156(3):527–33.
Dankbaar JW, de Rooij NK, Rijsdijk M, et al. Diagnostic threshold values of cerebral perfusion measured with computed tomography for delayed cerebral ischemia after aneurysmal subarachnoid hemorrhage. Stroke. 2010;41(9):1927–32.
Rijsdijk M, van der Schaaf IC, Velthuis BK, Wermer MJ, Rinkel GJE. Global and focal cerebral perfusion after aneurysmal subarachnoid hemorrhage in relation with delayed cerebral ischemia. Neuroradiology. 2008;50(9):813–20.
Murphy A, de Oliveira Manoel AL, Burgers K, et al. Early CT perfusion changes and blood-brain barrier permeability after aneurysmal subarachnoid hemorrhage. Neuroradiology. 2015;57(8):767–73.
Murphy A, Leonardo A, Manoel DO, et al. Changes in cerebral perfusion with induced hypertension in aneurysmal subarachnoid hemorrhage: a pilot and feasibility study. Neurocrit Care. 2017;27(1):3–10.
Etminan N, Beseoglu K, Heiroth HJ, Turowski B, Steiger HJ, Hänggi D. Early perfusion computerized tomography imaging as a radiographic surrogate for delayed cerebral ischemia and functional outcome after subarachnoid hemorrhage. Stroke. 2013;44(5):1260–6.
Friedrich B, Müller F, Feiler S, Schöller K, Plesnila N. Experimental subarachnoid hemorrhage causes early and long-lasting microarterial constriction and microthrombosis: an in vivo microscopy study. J Cereb Blood Flow Metab. 2012;32(3):447–55.
Cossu G, Messerer M, Oddo M, Daniel RT. To look beyond vasospasm in aneurysmal subarachnoid haemorrhage. Biomed Res Int. 2014;2014:628597. https://doi.org/10.1155/2014/628597.
Provencio JJ, Vora N. Subarachnoid hemorrhage and inflammation: Bench to bedside and back. Semin Neurol. 2005;25(4):435–44.
Liu C, Tang J. Expression levels of tumor necrosis factor-alpha and the corresponding receptors are correlated with trauma severity. Oncol Lett. 2014;8(6):2747–51.
Claassen J, Albers D, Schmidt JM, et al. Nonconvulsive seizures in subarachnoid hemorrhage link inflammation and outcome. Ann Neurol. 2014;75(5):771–81.
Noto C, Gadelha A, Belangero SI, et al. Circulating levels of sTNFR1 as a marker of severe clinical course in schizophrenia. J Psychiatr Res. 2013;47(4):467–71.
Claassen J, Carhuapoma JR, Kreiter KT, Du EY, Connolly ES, Mayer SA. Global cerebral edema after subarachnoid hemorrhage: frequency, predictors, and impact on outcome. Stroke. 2002;33(5):1225–32.
Fragata I, Canto-Moreira N, Canhão P. Comparison of cerebral perfusion in perimesencephalic subarachnoid hemorrhage and aneurysmal subarachnoid hemorrhage. Neuroradiology. 2018;60(6):609–16. https://doi.org/10.1007/s00234-018-1997-1.
Fragata I, Canto-Moreira N, Canhão P. Ischemic lesions in acute and subacute perimesencephalic subarachnoid hemorrhage. Am J Roentgenol. 2018;212(2):418–24.
Acknowledgements
We thank the Clinical Pathology Laboratory of Hospital São José, CHLC, for careful preparation of the blood samples.
Funding
Dr Fragata was supported by Sociedade Portuguesa de AVC/Tecnifar. Dr Bustamante is supported by a Juan Rodes research contract (JR16/00008) from Instituto de Salud Carlos III.
Author information
Authors and Affiliations
Contributions
IF, AB, PC, JM contributed to project design; IF, AB, AP, PF, APN contributed to data collection; AB, IF performed data analysis; IF, AB, JM, PC contributed to writing. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
Institutional review board approval was obtained for this study. Informed consent obtained from patient or legal representative.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fragata, I., Bustamante, A., Penalba, A. et al. TNF-R1 Correlates with Cerebral Perfusion and Acute Ischemia Following Subarachnoid Hemorrhage. Neurocrit Care 33, 679–687 (2020). https://doi.org/10.1007/s12028-020-01082-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-01082-3