Abstract
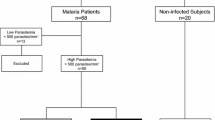
The persistence of residual infection is one of the major factors in failure of the Global Programme to Eliminate Lymphatic Filariasis (GPELF). The present study aims to explore the status of sheath antibody and regulatory T cells (Tregs) known to play key roles in clearance of parasite and patent filarial infection, in individuals with residual infection after MDA. A total of 61 microfilaremic (Mf) individuals were followed up after at least 6 rounds of MDA. Infection status of subjects was assessed through the detection of Mf and circulating filarial antigen (CFA). Antibodies to Mf sheath were determined by immuno-peroxidase assay (IPA). The expression of Tregs was measured by a flow cytometer. IL-10 and IFN-γ were evaluated using the commercially available ELISA kit. The sheath antibody was present in subjects who have cleared both Mf and CFA and absent in individuals who were found to be Mf /CFA positive. Further individuals carrying infection have significantly high levels of Tregs and IL-10. A positive correlation was observed between Tregs, IL-10, and CFA in infected individuals. In contrast, a negative correlation was observed between IFN-γ and IL-10 in both infected and uninfected subjects. Our study reveals that the absence of a sheath antibody and a high level of Tregs and IL-10 are the hallmarks of the persistence of residual filarial infection.






Similar content being viewed by others
Data availability
All data pertaining to this study is published in the paper or included in the Supplemental Materials.
References
Achary KG, Mandal NN, Mishra S, Mishra R, Sarangi SS, Satapathy AK, et al. In utero sensitization modulates IgG isotype, IFN-γ and IL-10 responses of neonates in bancroftian filariasis. Parasite Immunol. 2014;36(10):485–93. https://doi.org/10.1111/pim.12121.
Achary KG, Mandal NN, Mishra S, Sarangi SS, Kar SK, Satapathy AK, et al. Maternal filarial infection: association of anti-sheath antibody responses with plasma levels of IFN-γ and IL-10. Parasitol. 2013;140(5):598–03. https://doi.org/10.1017/S0031182012002144.
Babu S, Nutman TB. Immunology of lymphatic filariasis. Parasite Immunol. 2014;36(8):338–46. https://doi.org/10.1111/pim.12081.
Babu S, Ganley M, Klei TR, Shultz LD, Rajan TV. Role of gamma interferon and interleukin-4 in host defense against the human filarial parasite Brugia malayi. Infect Immun. 2000;68(5):3034–5. https://doi.org/10.1128/iai.68.5.3034-3035.2000.
Bal M, Ranjit M, Achary KG, Satapathy AK. Maternal filarial infection influences the development of regulatory T cells in children from infancy to early childhood. PLoS Negl Trop Dis. 2016;10(11):e0005144. https://doi.org/10.1371/journal.pntd.0005144.
Biritwum NK, Yikpotey P, Marfo BK., Odoom S, Mensah EO, Asiedu O, Alomatu B, Hervie ET, ,Yeboah A, Ade S. Hinderaker SG, Reid A, Takarinda KC, Koudou B, Koroma J B. Persistent ‘hotspots’ of lymphatic filariasis microfilaraemia despite 14 years of mass drug administration in Ghana. Trans R Soc Trop Med Hyg, 2017; 110(12): 690-695. https://doi.org/10.1093/trstmh/trx007
De Souza DK, Ansumana R, Sessay S, Conteh A, Koudou B, Rebollo MP, et al. The impact of residual infections on Anopheles-transmitted Wuchereria bancrofti after multiple rounds of mass drug administration. Parasit Vectors. 2015;8(1):488. https://doi.org/10.1186/s13071-015-1091-z.
Gillan V, Devaney E. Regulatory T cells modulate Th2 responses induced by Brugia pahangi third-stage larvae. Infect Immun. 2005;73(7):4034–42. https://doi.org/10.1128/iai.73.7.4034-4042.2005.
Jawaharlal JP, Madhumathi J, Prince RP, Kaliraj P. Repeat region of Brugia malayi sheath protein (Shp-1) carries Dominant B epitopes recognized in filarial endemic population. Acta Parasitol. 2014;(3):454–8. https://doi.org/10.2478/s11686-014-0270-y.
Kalimuthu M, Sunish IP, Nagaraj J, Munirathinam A, Kumar VA, Arunachalam N, et al. Residual microfilaraemia in rural pockets of South India after five rounds of DEC plus albendazole administration as part of the LF elimination campaign. J Vector Borne Dis. 2015;52(2):182–4.
Kar SK, Dwibedi B, Kerketa AS, Maharana A, Panda SS, Mohanty PC, et al. A randomized controlled trial of increased dose and frequency of albendazole with standard dose DEC for treatment of Wuchereria bancrofti microfilaremics in Odisha, India. PLoS Negl Trop Dis. 2015;9(3):e0003583. https://doi.org/10.1371/journal.pntd.0003583.
King CL, Mahanty S, Kumaraswami V, Abrams JS, Regunathan J, Jayaraman K, et al. Cytokine control of parasite-specific anergy in human lymphatic filariasis. Preferential induction of a regulatory T helper type 2 lymphocyte subset. J Clin Invest. 1993;92(4):1667–73. https://doi.org/10.1172/jci116752.
Lau CL, Sheridan S, Ryan S, Roineau M, Andreosso A, Fuimaono S, et al. Detecting and confirming residual hotspots of lymphatic filariasis transmission in American Samoa 8 years after stopping mass drug administration. PLoS Negl Trop Dis. 2017;11(9):e0005914. https://doi.org/10.1371/journal.pntd.
Mahanty S, Mollis SN, Ravichandran M, Abrams JS, Kumaraswami V, Jayaraman K, et al. High levels of spontaneous and parasite antigen-driven interleukin-10 production are associated with antigen-specific hyporesponsiveness in human lymphatic filariasis. J Infect Dis. 1996;173(3):769–73. https://doi.org/10.1093/infdis/173.3.769.
Metenou S, Nutman TB. Regulatory T cell subsets in filarial infection and their function. Front Immunol. 2013;4:305. https://doi.org/10.3389/fimmu.2013.00305.
Metenou S, Dembele B, Konate S, Dolo H, Coulibaly SY, Coulibaly YI, et al. At homeostasis filarial infections have expanded adaptive T regulatory but not classical Th2 cells. J Immunol. 2010;184(9):5375. https://doi.org/10.4049/jimmunol.0904067.
Molyneux DH. Advancing toward the elimination of lymphatic filariasis. N Engl J Med. 2018;379(19):1871–2. https://doi.org/10.1056/NEJMe1811455.
Pi-Bans S, Osei JHN, Frempong KK, Elhassan E, Akuoko OK, Agyemang D, et al. Potential factors influencing lymphatic filariasis transmission in “hotspot” and “control” areas in Ghana: the importance of vectors. Infect Dis Poverty. 2019;8(1):9. https://doi.org/10.1186/s40249-019-0520-.
Ramaiah KD, Ottesen EA. Progress and Impact of 13 Years of the Global Programme to Eliminate Lymphatic Filariasis on Reducing the Burden of Filarial Disease. PLoS Negl Trop Dis. 2014;8(11):e3319. https://doi.org/10.1371/journal.pntd.0003319.
Ravindran B, Satapathy AK, Sahoo PK, Babu Geddam JJ. Protective immunity in human Bancroftian filariasis: inverse relationship between antibodies to microfilarial sheath and circulating filarial antigens. Parasite Immunol. 2000;22(12):633–7.
Ravindran B, Satapathy AK, Sahoo PK, Mohanty MC. Protective immunity in human lymphatic filariasis: problems and prospects. Med Microbiol Immunol. 2003;192(1):41–6. https://doi.org/10.1007/s00430-002-0157-7.
Ravindran B, Satapathy AK, Sahoo PK. Bancroftian filariasis-differential reactivity of anti-sheath antibodies in microfilariae carriers. Parasite Immunol. 1994;16(6):321–3. https://doi.org/10.1111/j.1365-3024.1994.tb00355.x.
Rebollo MP, Bockarie MJ. Toward the elimination of lymphatic filariasis by 2020: treatment update and impact assessment for the endgame. Expert Rev Anti-Infect Ther. 2013;11(7):723–31. https://doi.org/10.1586/14787210.2013.811841.
Ritter M, Osei-Mensah J, Debrah LB, Kwarteng A, Mubarik Y, Debrah AY, et al. Wuchereria bancrofti-infected individuals harbour distinct IL-10-producing regulatory B and T cell subsets which are affected by anti-filarial treatment. PLoS Negl Trop Dis. 2019;13(5):e0007436.
Sheel M, Sheridan S, Gass K, Won K, Fuimaono S, Kirk M, et al. Identifying residual transmission of lymphatic filariasis after mass drug administration: comparing school-based versus community-based surveillance - American Samoa, 2016. PLoS Negl Trop Dis. 2018;12(7):e0006583. https://doi.org/10.1371/journal.pntd.0006583.
Simonsen PE, Meyrowitsch DW, Jaoko WG, Malecela MN, Michael E. Immunoepidemiology of Wuchereria bancrofti infection in two East African communities: antibodies to the microfilarial sheath and their role in regulating host microfilaraemia. Acta Trop. 2008;106(3):200–6. https://doi.org/10.1016/j.actatropica.2008.03.008.
Stolk WA, ten Bosch QA, de Vlas SJ, Fischer PU, Weil GJ, Goldman AS. Modeling the impact and costs of semiannual mass drug administration for accelerated elimination of lymphatic filariasis. PLoS Negl Trop Dis. 2013;7(1):e1984. https://doi.org/10.1371/journal.pntd.0001984.
Taylor MD, LeGoff L, Harris A, Malone E. Allen JE and Maizels RMRemoval of regulatory T cell activity reverses hyporesponsiveness and leads to filarial parasite clearance in vivo. J Immunol. 2005;174(8):4924–33. https://doi.org/10.4049/jimmunol.174.8.492.
Wammes LJ, Hamid F, Wiria AE, Wibowo H, Sartono E, Maizels RM, et al. Regulatory T cells in human lymphatic filariasis: stronger functional activity in microfilaremics. PLoS Negl Trop Dis. 2012;6(5):e1655. https://doi.org/10.1371/journal.pntd.0001655.
World Health Organization. Western Pacific Region. Congratulations, Tonga! Pacific island state eliminates lymphatic filariasisas a public health problem. 2017. [7 September 2017]. http://www.wpro.who.int/mediacentre/releases/2017/20170731/en/
World Health Organization. Monitoring and epidemiological assessment of mass drug administration in the global programme to eliminate lymphatic filariasis: a manual for national elimination programmes. 2011.
Acknowledgments
We are grateful to all the participants of this study for their sincere cooperation throughout this study. We thankfully acknowledge the technical assistance rendered by Mr Minaketan Barik, Mr KC Parichha, and Mr Niranjan Sahu of the institute during the study. We express our gratitude to the village chiefs, field workers, and community members for their support during the study.
Funding
This work was supported by the Indian Council of Medical Research, New Delhi, India.
Author information
Authors and Affiliations
Contributions
Conceptualization: Madhusmita Bal; methodology: Madhusmita Bal, Manoranjan Ranjit, and Bhagirathi Dwibedi; formal analysis and investigation: Madhusmita Bal, K. GopinathAchary, and Hemanta K. Khuntia; writing—original draft preparation: Madhusmita Bal; writing—review and editing: Manoranjan Ranjit and Madhusmita Bal; funding acquisition: Sanghamitra Pati; resources: Ashok K. Satapathy; supervision: Madhusmita Bal
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest
Ethics approval
The Indian Council of Medical Research has granted the proposal and Human Ethical Committee of ICMR-Regional Medical Research Centre Bhubaneswar, Odisha, has approved the study.
Consent to participate
Informed written consent has been taken from all participants.
Code availability
Not applicable
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Fig. 1
Lymphocytes were analyzed by flow cytometry after staining with anti-human CD4-FITC and anti-human CD25-PE. Figure shows the gating strategy of regulatory T Cells (CD4+ T cells expressing the highest level of CD25 i,e CD4+ CD25hi). % of Tregs frequencies were calculated from total lymphocyte gated (TIFF 757 kb)
Rights and permissions
About this article
Cite this article
Bal, M., Ranjit, M., Khuntia, H.K. et al. High Tregs and systemic IL-10 expressions linked to the absence of sheath antibodies in lymphatic filariasis: implications on the persistence of residual infection. Immunol Res 69, 90–99 (2021). https://doi.org/10.1007/s12026-021-09175-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12026-021-09175-7