Abstract
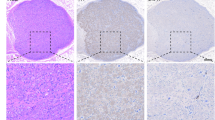
One of the hypothesized mechanisms of sudden cardiac death in humans is an arrhythmia precipitated by increased sympathetic outflow to a compromised heart. The stellate ganglia provide the main sympathetic innervation to the heart, where the left stellate ganglion appears to play a role in arrhythmogenesis. Case reports of sudden cardiac death have described left stellate ganglion inflammation but no larger studies have been performed. Thus, we have specifically assessed whether the left stellate ganglion was inflamed in those dying from sudden cardiac death versus other causes of death. Thirty-one left stellate ganglia were resected from cadavers diagnosed with sudden cardiac deaths and compared with 18 ganglia from cadavers diagnosed with non-sudden cardiac deaths. Ganglia were stained with hematoxylin and eosin and lymphocytic aggregates compared. The proportion of left stellate ganglion inflammation (77%) was significantly higher in deaths from sudden cardiac deaths than non-sudden cardiac deaths (33%). This study provides information on a previously recognized, but understudied, structure that may help understand sudden cardiac death. We found high prevalence of stellate ganglion inflammation and propose that this may trigger sympathetic storms.


Similar content being viewed by others
References
Kuriachan VPMD, Sumner GLMD, Mitchell LBMD. Sudden cardiac death. Curr Probl Cardiol. 2015;40(4):133–200.
Hayashi M, Shimizu W, Albert CM. The spectrum of epidemiology underlying sudden cardiac death. Circ Res. 2015;116(12):1887–906.
Smith SA, Mitchell JH, Garry MG. The mammalian exercise pressor reflex in health and disease. Exp Physiol. 2006;91(1):89–102.
Rajendran PS, Challis RC, Fowlkes CC, Hanna P, Tompkins JD, Jordan MC, et al. Identification of peripheral neural circuits that regulate heart rate using optogenetic and viral vector strategies. Nature Commun. 2019;10(1).
Mitchell JH. Abnormal cardiovascular response to exercise in hypertension: contribution of neural factors. Am J Physiology-Regulatory, Integrative and Comparative Physiol. 2017;312(6):R851–63.
Schwartz PJ, Stone HL. Left stellectomy in the prevention of ventricular fibrillation caused by acute myocardial ischemia in conscious dogs with anterior myocardial infarction. Circulation. 1980;62(6):1256–65.
Rizzo S, Basso C, Troost D, Aronica E, Frigo AC, Driessen AHG, et al. T-cell–mediated inflammatory activity in the stellate ganglia of patients with ion-channel disease and severe ventricular arrhythmias. Circulation: Arrhythmia and Electrophysiology. 2014;7(2):224–9.
Ajijola OA, Yagishita D, Reddy NK, Yamakawa K, Vaseghi M, Downs AM, et al. Remodeling of stellate ganglion neurons after spatially targeted myocardial infarction: neuropeptide and morphologic changes. Heart rhythm : the official j Heart Rhythm Soc. 2015;12(5):1027–35.
Ajijola OA, Hoover DB, Simerly TM, Brown TC, Yanagawa J, Biniwale RM, et al. Inflammation, oxidative stress, and glial cell activation characterize stellate ganglia from humans with electrical storm. JCI Insight. 2017;2(18).
Bardsley EN, Davis H, Ajijola OA, Buckler KJ, Ardell JL, Shivkumar K, et al. RNA sequencing reveals novel transcripts from sympathetic stellate ganglia during cardiac sympathetic hyperactivity. Sci Rep. 2018;8(1).
Zhou S, Jung B-C, Tan AY, Trang VQ, Gholmieh G, Han S-W, et al. Spontaneous stellate ganglion nerve activity and ventricular arrhythmia in a canine model of sudden death. Heart rhythm : the official journal of the Heart Rhythm Society. 2008;5(1):131–9.
Wang Z, Li S, Lai H, Zhou L, Meng G, Wang M, et al. Interaction between endothelin-1 and left stellate ganglion activation: a potential mechanism of malignant ventricular arrhythmia during myocardial ischemia. Oxid Med Cell Longev. 2019;2019:6508328.
Duffy M, Garland J, Ondruschka B, Paton JFR, Bardsley EN, Wong CX, et al. Stellate ganglionitis in sudden cardiac death: a case report. Auton Neurosci. 2021;234:102837.
Rossi L. Cardioneuropathy and extracardiac neural disease. J Am Coll Cardiol. 1985;5(6):66B-70B.
James TN, Zipes DP, Finegan RE, Eisele JW, Carter JE. Cardiac ganglionitis associated with sudden unexpected death. Ann Intern Med. 1979;91(5):727–30.
James TN, Imamura K. Virus-like particles associated with intracardiac ganglionitis in 2 cases of sudden unexpected death. Jpn Heart J. 1981;22(3):447–54.
Thiene G. Sudden cardiac death and cardiovascular pathology: from anatomic theater to double helix. Am J Cardiol. 2014;114(12):1930–6.
Adabag AS, Luepker RV, Roger VL, Gersh BJ. Sudden cardiac death: epidemiology and risk factors. Nat Rev Cardiol. 2010;7(4):216–25.
Finocchiaro G, Papadakis M, Dhutia H, Cole D, Behr ER, Tome M, et al. Obesity and sudden cardiac death in the young: clinical and pathological insights from a large national registry. Eur J Prev Cardiol. 2018;25(4):395–401.
Rosenberg MA, Lopez FL, Bůžková P, Adabag S, Chen LY, Sotoodehnia N, et al. Height and risk of sudden cardiac death: the Atherosclerosis Risk in Communities and Cardiovascular Health studies. Ann Epidemiol. 2014;24(3):174-9.e2.
Dahlberg ST. Gender difference in the risk factors for sudden cardiac death. Cardiology. 1990;77(Suppl 2):31–40.
Ellulu MS, Patimah I, Khaza’Ai H, Rahmat A, Abed Y. Obesity and inflammation: the linking mechanism and the complications. Archives of Med Sci. 2017;4:851–63.
Chung HY, Kim DH, Lee EK, Chung KW, Chung S, Lee B, et al. Redefining chronic inflammation in aging and age-related diseases: proposal of the senoinflammation concept. Aging Dis. 2019;10(2):367–82.
Schwartz PJ, Motolese M, Pollavini G, Lotto A, Ruberti U, Trazzi R, et al. Prevention of sudden cardiac death after a first myocardial infarction by pharmacologic or surgical antiadrenergic interventions. J Cardiovasc Electrophysiol. 1992;3(1):2–16.
Vestergaard V, Drostrup DH, Thomsen JL. Sudden unexpected death associated with lymphocytic thyroiditis. Med Sci Law. 2007;47(2):125–33.
Edston E. Three sudden deaths in men associated with undiagnosed chronic thyroiditis. Int J Legal Med. 1996;109(2):94–7.
Collins KA, Hutchins GM. An introduction to autopsy technique. 2nd ed. Illinois: College of Am Pathol. 2005.
Collins KA. Special Austopsy Dissection. 1st ed. Illinois: CAP Press; 2010.
Tan CMJ, Green P, Tapoulal N, Lewandowski AJ, Leeson P, Herring N. The role of neuropeptide Y in cardiovascular health and disease. Front Physiol. 2018;9:1281-.
Kalla M, Hao G, Tapoulal N, Tomek J, Liu K, Woodward L, et al. The cardiac sympathetic co-transmitter neuropeptide Y is pro-arrhythmic following ST-elevation myocardial infarction despite beta-blockade. Eur Heart J. 2020;41(23):2168–79.
Herring N, Tapoulal N, Kalla M, Ye X, Borysova L, Lee R, et al. Neuropeptide-Y causes coronary microvascular constriction and is associated with reduced ejection fraction following ST-elevation myocardial infarction. Eur Heart J. 2019;40(24):1920–9.
Shaker T, Chattopadhyaya B, Amilhon B, Cristo GD, Weil AG. Transduction of inflammation from peripheral immune cells to the hippocampus induces neuronal hyperexcitability mediated by Caspase-1 activation. Neurobiol Dis. 2021;160:105535.
Acknowledgements
The authors would like to thank the forensic technicians for their dissection expertise, and doctors Kilak Kesha, Charley Glenn, and Paul Morrow in assisting in the preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tse, R., Garland, J., McCarthy, S. et al. Sudden cardiac deaths have higher proportion of left stellate ganglionitis. Forensic Sci Med Pathol 18, 156–164 (2022). https://doi.org/10.1007/s12024-022-00466-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-022-00466-5