Abstract
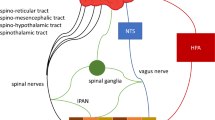
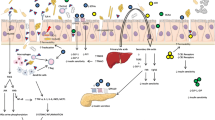
Type 2 diabetes mellitus (T2DM) has become one of the most serious public healthcare challenges, contributing to increased mortality and disability. In the past decades, significant progress has been made in understanding the pathogenesis of T2DM. Mounting evidence suggested that gut microbiota (GM) plays a significant role in the development of T2DM. Communication between the GM and the brain is a complex bidirectional connection, known as the “gut-brain axis,” via the nervous, neuroendocrine, and immune systems. Gut-brain axis has an essential impact on various physiological processes, including glucose metabolism, food intake, gut motility, etc. In this review, we provide an outline of the gut-brain axis. We also highlight how the dysbiosis of the gut-brain axis affects glucose homeostasis and even results in T2DM.



Similar content being viewed by others
References
H. Sun, P. Saeedi, S. Karuranga, M. Pinkepank, K. Ogurtsova, B.B. Duncan, C. Stein, A. Basit, J.C.N. Chan, J.C. Mbanya, M.E. Pavkov, A. Ramachandaran, S.H. Wild, S. James, W.H. Herman, P. Zhang, C. Bommer, S. Kuo, E.J. Boyko, D.J. Magliano, IDF diabetes atlas: global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res. Clin. Pr. 183, 109119 (2022). https://doi.org/10.1016/j.diabres.2021.109119
M.N. Huda, M. Kim, B.J. Bennett, Modulating the microbiota as a therapeutic intervention for type 2 diabetes. Front. Endocrinol. 12, 632335 (2021). https://doi.org/10.3389/fendo.2021.632335
S. Chatterjee, K. Khunti, M.J. Davies, Type 2 diabetes. Lancet 389(10085), 2239–2251 (2017). https://doi.org/10.1016/s0140-6736(17)30058-2
M. Gurung, Z. Li, H. You, R. Rodrigues, D.B. Jump, A. Morgun, N. Shulzhenko, Role of gut microbiota in type 2 diabetes pathophysiology. EBioMedicine 51, 102590 (2020). https://doi.org/10.1016/j.ebiom.2019.11.051
M. Zhao, J. Chu, S. Feng, C. Guo, B. Xue, K. He, L. Li, Immunological mechanisms of inflammatory diseases caused by gut microbiota dysbiosis: A review. Biomed. Pharmacother. 164, 114985 (2023). https://doi.org/10.1016/j.biopha.2023.114985
A. Jais, J.C. Brüning, Arcuate nucleus-dependent regulation of metabolism-pathways to obesity and diabetes mellitus. Endocr. Rev. 43(2), 314–328 (2022). https://doi.org/10.1210/endrev/bnab025
W.R. Wikoff, A.T. Anfora, J. Liu, P.G. Schultz, S.A. Lesley, E.C. Peters, G. Siuzdak, Metabolomics analysis reveals large effects of gut microflora on mammalian blood metabolites. Proc. Natl Acad. Sci. USA 106(10), 3698–3703 (2009). https://doi.org/10.1073/pnas.0812874106
J.M. Yano, K. Yu, G.P. Donaldson, G.G. Shastri, P. Ann, L. Ma, C.R. Nagler, R.F. Ismagilov, S.K. Mazmanian, E.Y. Hsiao, Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell 161(2), 264–276 (2015). https://doi.org/10.1016/j.cell.2015.02.047
B.S. Samuel, A. Shaito, T. Motoike, F.E. Rey, F. Backhed, J.K. Manchester, R.E. Hammer, S.C. Williams, J. Crowley, M. Yanagisawa, J.I. Gordon, Effects of the gut microbiota on host adiposity are modulated by the short-chain fatty-acid binding G protein-coupled receptor, Gpr41. Proc. Natl Acad. Sci. USA 105(43), 16767–16772 (2008). https://doi.org/10.1073/pnas.0808567105
P.V. Bauer, S.C. Hamr, F.A. Duca, Regulation of energy balance by a gut-brain axis and involvement of the gut microbiota. Cell Mol. Life Sci. 73(4), 737–755 (2016). https://doi.org/10.1007/s00018-015-2083-z
C. Lee, H. Lee, J.C. Park, S.H. Im, Microbial components and effector molecules in T Helper cell differentiation and function. Immune Netw. 23(1), e7 (2023). https://doi.org/10.4110/in.2023.23.e7
J. Qin, R. Li, J. Raes, M. Arumugam, K.S. Burgdorf, C. Manichanh, T. Nielsen, N. Pons, F. Levenez, T. Yamada, D.R. Mende, J. Li, J. Xu, S. Li, D. Li, J. Cao, B. Wang, H. Liang, H. Zheng, Y. Xie, J. Tap, P. Lepage, M. Bertalan, J.M. Batto, T. Hansen, D. Le Paslier, A. Linneberg, H.B. Nielsen, E. Pelletier, P. Renault, T. Sicheritz-Ponten, K. Turner, H. Zhu, C. Yu, S. Li, M. Jian, Y. Zhou, Y. Li, X. Zhang, S. Li, N. Qin, H. Yang, J. Wang, S. Brunak, J. Doré, F. Guarner, K. Kristiansen, O. Pedersen, J. Parkhill, J. Weissenbach, P. Bork, S.D. Ehrlich, J. Wang, A human gut microbial gene catalogue established by metagenomic sequencing. Nature 464(7285), 59–65 (2010). https://doi.org/10.1038/nature08821
C. de Weerth, Do bacteria shape our development? Crosstalk between intestinal microbiota and HPA axis. Neurosci. Biobehav. Rev. 83, 458–471 (2017). https://doi.org/10.1016/j.neubiorev.2017.09.016
A. El-Sayed, L. Aleya, M. Kamel, Microbiota’s role in health and diseases. Environ. Sci. Pollut. Res. Int. 28(28), 36967–36983 (2021). https://doi.org/10.1007/s11356-021-14593-z
H. Ullah, S. Arbab, Y. Tian, C.Q. Liu, Y. Chen, L. Qijie, M.I.U. Khan, I.U. Hassan, K. Li, The gut microbiota-brain axis in neurological disorder. Front. Neurosci. 17, 1225875 (2023). https://doi.org/10.3389/fnins.2023.1225875
P.B. Eckburg, E.M. Bik, C.N. Bernstein, E. Purdom, L. Dethlefsen, M. Sargent, S.R. Gill, K.E. Nelson, D.A. Relman, Diversity of the human intestinal microbial flora. Science 308(5728), 1635–1638 (2005). https://doi.org/10.1126/science.1110591
C. Barrio, S. Arias-Sánchez, I. Martín-Monzón, The gut microbiota-brain axis, psychobiotics and its influence on brain and behaviour: a systematic review. Psychoneuroendocrinology 137, 105640 (2022). https://doi.org/10.1016/j.psyneuen.2021.105640
C.S. Oriach, R.C. Robertson, C. Stanton, J.F. Cryan, T.G. Dinan, Food for thought: the role of nutrition in the microbiota–gut–brain axis. Clin. Nutr. Exp. 6, 25–38 (2016). https://doi.org/10.1016/j.yclnex.2016.01.003
Y. Chen, J. Zhou, L. Wang, Role and mechanism of gut microbiota in human disease. Front. Cell Infect. Microbiol. 11, 625913 (2021). https://doi.org/10.3389/fcimb.2021.625913
A. Varesi, L.I.M. Campagnoli, F. Fahmideh, E. Pierella, M. Romeo, G. Ricevuti, M. Nicoletta, S. Chirumbolo, and A. Pascale, The interplay between gut microbiota and Parkinson’s disease: implications on diagnosis and treatment. Int. J. Mol. Sci. 23(20), (2022). https://doi.org/10.3390/ijms232012289
A. Varesi, L.I.M. Campagnoli, S. Chirumbolo, B. Candiano, A. Carrara, G. Ricevuti, C. Esposito, A. Pascale, The brain-gut-microbiota interplay in depression: a key to design innovative therapeutic approaches. Pharm. Res. 192, 106799 (2023). https://doi.org/10.1016/j.phrs.2023.106799
L.I.M. Campagnoli, N. Marchesi, M. Vairetti, A. Pascale, A. Ferrigno, and A. Barbieri, Age-related NAFLD: the use of probiotics as a supportive therapeutic intervention. Cells 11(18), (2022). https://doi.org/10.3390/cells11182827
F. Suriano, S. Vieira-Silva, G. Falony, M. Roumain, A. Paquot, R. Pelicaen, M. Régnier, N.M. Delzenne, J. Raes, G.G. Muccioli, M. Van Hul, P.D. Cani, Novel insights into the genetically obese (ob/ob) and diabetic (db/db) mice: two sides of the same coin. Microbiome 9(1), 147 (2021). https://doi.org/10.1186/s40168-021-01097-8
F. Yu, W. Han, G. Zhan, S. Li, X. Jiang, L. Wang, S. Xiang, B. Zhu, L. Yang, A. Luo, F. Hua, C. Yang, Abnormal gut microbiota composition contributes to the development of type 2 diabetes mellitus in db/db mice. Aging 11(22), 10454–10467 (2019). https://doi.org/10.18632/aging.102469
P.P. Zhang, L.L. Li, X. Han, Q.W. Li, X.H. Zhang, J.J. Liu, Y. Wang, Fecal microbiota transplantation improves metabolism and gut microbiome composition in db/db mice. Acta Pharm. Sin. 41(5), 678–685 (2020). https://doi.org/10.1038/s41401-019-0330-9
N. Larsen, F.K. Vogensen, F.W. van den Berg, D.S. Nielsen, A.S. Andreasen, B.K. Pedersen, W.A. Al-Soud, S.J. Sørensen, L.H. Hansen, M. Jakobsen, Gut microbiota in human adults with type 2 diabetes differs from non-diabetic adults. PLoS One 5(2), e9085 (2010). https://doi.org/10.1371/journal.pone.0009085
J. Qin, Y. Li, Z. Cai, S. Li, J. Zhu, F. Zhang, S. Liang, W. Zhang, Y. Guan, D. Shen, Y. Peng, D. Zhang, Z. Jie, W. Wu, Y. Qin, W. Xue, J. Li, L. Han, D. Lu, P. Wu, Y. Dai, X. Sun, Z. Li, A. Tang, S. Zhong, X. Li, W. Chen, R. Xu, M. Wang, Q. Feng, M. Gong, J. Yu, Y. Zhang, M. Zhang, T. Hansen, G. Sanchez, J. Raes, G. Falony, S. Okuda, M. Almeida, E. LeChatelier, P. Renault, N. Pons, J.M. Batto, Z. Zhang, H. Chen, R. Yang, W. Zheng, S. Li, H. Yang, J. Wang, S.D. Ehrlich, R. Nielsen, O. Pedersen, K. Kristiansen, J. Wang, A metagenome-wide association study of gut microbiota in type 2 diabetes. Nature 490(7418), 55–60 (2012). https://doi.org/10.1038/nature11450
Q. Li, Y. Chang, K. Zhang, H. Chen, S. Tao, Z. Zhang, Implication of the gut microbiome composition of type 2 diabetic patients from northern China. Sci. Rep. 10(1), 5450 (2020). https://doi.org/10.1038/s41598-020-62224-3
F.H. Karlsson, V. Tremaroli, I. Nookaew, G. Bergström, C.J. Behre, B. Fagerberg, J. Nielsen, F. Bäckhed, Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature 498(7452), 99–103 (2013). https://doi.org/10.1038/nature12198
P.C. Chen, Y.W. Chien, S.C. Yang, The alteration of gut microbiota in newly diagnosed type 2 diabetic patients. Nutrition 63-64, 51–56 (2019). https://doi.org/10.1016/j.nut.2018.11.019
K.H. Allin, V. Tremaroli, R. Caesar, B.A.H. Jensen, M.T.F. Damgaard, M.I. Bahl, T.R. Licht, T.H. Hansen, T. Nielsen, T.M. Dantoft, A. Linneberg, T. Jørgensen, H. Vestergaard, K. Kristiansen, P.W. Franks, T. Hansen, F. Bäckhed, O. Pedersen, Aberrant intestinal microbiota in individuals with prediabetes. Diabetologia 61(4), 810–820 (2018). https://doi.org/10.1007/s00125-018-4550-1
T. Xu, Y. Ge, H. Du, Q. Li, X. Xu, H. Yi, X. Wu, T. Kuang, G. Fan, Y. Zhang, Berberis kansuensis extract alleviates type 2 diabetes in rats by regulating gut microbiota composition. J. Ethnopharmacol. 273, 113995 (2021). https://doi.org/10.1016/j.jep.2021.113995
J. Xu, R. Liang, W. Zhang, K. Tian, J. Li, X. Chen, T. Yu, Q. Chen, Faecalibacterium prausnitzii-derived microbial anti-inflammatory molecule regulates intestinal integrity in diabetes mellitus mice via modulating tight junction protein expression. J. Diabetes 12(3), 224–236 (2020). https://doi.org/10.1111/1753-0407.12986
S. Singh, R.K. Sharma, S. Malhotra, R. Pothuraju, U.K. Shandilya, Lactobacillus rhamnosus NCDC17 ameliorates type-2 diabetes by improving gut function, oxidative stress and inflammation in high-fat-diet fed and streptozotocintreated rats. Benef. Microbes 8(2), 243–255 (2017). https://doi.org/10.3920/bm2016.0090
S. Westfall, N. Lomis, I. Kahouli, S.Y. Dia, S.P. Singh, S. Prakash, Microbiome, probiotics, and neurodegenerative diseases: deciphering the gut-brain axis. Cell Mol. Life Sci. 74(20), 3769–3787 (2017). https://doi.org/10.1007/s00018-017-2550-9
C. Long-Smith, K.J. O’Riordan, G. Clarke, C. Stanton, T.G. Dinan, J.F. Cryan, Microbiota-gut-brain axis: new therapeutic opportunities. Annu. Rev. Pharm. Toxicol. 60, 477–502 (2020). https://doi.org/10.1146/annurev-pharmtox-010919-023628
H.R. Wachsmuth, S.N. Weninger, F.A. Duca, Role of the gut-brain axis in energy and glucose metabolism. Exp. Mol. Med. 54(4), 377–392 (2022). https://doi.org/10.1038/s12276-021-00677-w
M. Rao, M.D. Gershon, The bowel and beyond: the enteric nervous system in neurological disorders. Nat. Rev. Gastroenterol. Hepatol. 13(9), 517–528 (2016). https://doi.org/10.1038/nrgastro.2016.107
A.M. Goldstein, R.M. Hofstra, A.J. Burns, Building a brain in the gut: development of the enteric nervous system. Clin. Genet 83(4), 307–316 (2013). https://doi.org/10.1111/cge.12054
B. Niesler, S. Kuerten, I.E. Demir, K.H. Schäfer, Disorders of the enteric nervous system - a holistic view. Nat. Rev. Gastroenterol. Hepatol. 18(6), 393–410 (2021). https://doi.org/10.1038/s41575-020-00385-2
L.M.T. Dicks, Gut Bacteria and Neurotransmitters. Microorganisms 10(9), (2022). https://doi.org/10.3390/microorganisms10091838
M. Schemann, Control of gastrointestinal motility by the “gut brain”–the enteric nervous system. J. Pediatr. Gastroenterol. Nutr. 41 Suppl 1, S4–S6 (2005). https://doi.org/10.1097/01.scs.0000180285.51365.55
J.F. Cryan, K.J. O’Riordan, C.S.M. Cowan, K.V. Sandhu, T.F.S. Bastiaanssen, M. Boehme, M.G. Codagnone, S. Cussotto, C. Fulling, A.V. Golubeva, K.E. Guzzetta, M. Jaggar, C.M. Long-Smith, J.M. Lyte, J.A. Martin, A. Molinero-Perez, G. Moloney, E. Morelli, E. Morillas, R. O’Connor, J.S. Cruz-Pereira, V.L. Peterson, K. Rea, N.L. Ritz, E. Sherwin, S. Spichak, E.M. Teichman, M. van de Wouw, A.P. Ventura-Silva, S.E. Wallace-Fitzsimons, N. Hyland, G. Clarke, T.G. Dinan, The microbiota-gut-brain axis. Physiol. Rev. 99(4), 1877–2013 (2019). https://doi.org/10.1152/physrev.00018.2018
S. Breit, A. Kupferberg, G. Rogler, G. Hasler, Vagus nerve as modulator of the brain-gut axis in psychiatric and inflammatory disorders. Front. Psychiatry 9, 44 (2018). https://doi.org/10.3389/fpsyt.2018.00044
H. Ahmed, Q. Leyrolle, V. Koistinen, O. Kärkkäinen, S. Layé, N. Delzenne, K. Hanhineva, Microbiota-derived metabolites as drivers of gut-brain communication. Gut Microbes 14(1), 2102878 (2022). https://doi.org/10.1080/19490976.2022.2102878
S. Fried, E. Wemelle, P.D. Cani, C. Knauf, Interactions between the microbiota and enteric nervous system during gut-brain disorders. Neuropharmacology 197, 108721 (2021). https://doi.org/10.1016/j.neuropharm.2021.108721
A. Bessac, P.D. Cani, E. Meunier, G. Dietrich, C. Knauf, Inflammation and gut-brain axis during type 2 diabetes: focus on the crosstalk between intestinal immune cells and enteric nervous system. Front. Neurosci. 12, 725 (2018). https://doi.org/10.3389/fnins.2018.00725
A. Abot, A. Lucas, T. Bautzova, A. Bessac, A. Fournel, S. Le-Gonidec, P. Valet, C. Moro, P.D. Cani, C. Knauf, Galanin enhances systemic glucose metabolism through enteric nitric oxide synthase-expressed neurons. Mol. Metab. 10, 100–108 (2018). https://doi.org/10.1016/j.molmet.2018.01.020
B. Chandrasekharan, S. Srinivasan, Diabetes and the enteric nervous system. Neurogastroenterol. Motil. 19(12), 951–960 (2007). https://doi.org/10.1111/j.1365-2982.2007.01023.x
H. Iwasaki, M. Kajimura, S. Osawa, S. Kanaoka, T. Furuta, M. Ikuma, A. Hishida, A deficiency of gastric interstitial cells of Cajal accompanied by decreased expression of neuronal nitric oxide synthase and substance P in patients with type 2 diabetes mellitus. J. Gastroenterol. 41(11), 1076–1087 (2006). https://doi.org/10.1007/s00535-006-1909-8
S.S. Yarandi, S. Srinivasan, Diabetic gastrointestinal motility disorders and the role of enteric nervous system: current status and future directions. Neurogastroenterol. Motil. 26(5), 611–624 (2014). https://doi.org/10.1111/nmo.12330
A. Fournel, A. Drougard, T. Duparc, A. Marlin, S.M. Brierley, J. Castro, S. Le-Gonidec, B. Masri, A. Colom, A. Lucas, P. Rousset, N. Cenac, N. Vergnolle, P. Valet, P.D. Cani, C. Knauf, Apelin targets gut contraction to control glucose metabolism via the brain. Gut 66(2), 258–269 (2017). https://doi.org/10.1136/gutjnl-2015-310230
F. De Vadder, E. Grasset, L. Mannerås Holm, G. Karsenty, A.J. Macpherson, L.E. Olofsson, F. Bäckhed, Gut microbiota regulates maturation of the adult enteric nervous system via enteric serotonin networks. Proc. Natl Acad. Sci. USA 115(25), 6458–6463 (2018). https://doi.org/10.1073/pnas.1720017115
T.M.Z. Waise, H.J. Dranse, T.K.T. Lam, The metabolic role of vagal afferent innervation. Nat. Rev. Gastroenterol. Hepatol. 15(10), 625–636 (2018). https://doi.org/10.1038/s41575-018-0062-1
B. Bonaz, T. Bazin, S. Pellissier, The vagus nerve at the interface of the microbiota-gut-brain axis. Front. Neurosci. 12, 49 (2018). https://doi.org/10.3389/fnins.2018.00049
E.K. Williams, R.B. Chang, D.E. Strochlic, B.D. Umans, B.B. Lowell, S.D. Liberles, Sensory neurons that detect stretch and nutrients in the digestive system. Cell 166(1), 209–221 (2016). https://doi.org/10.1016/j.cell.2016.05.011
L.H. Morais, H.L.T. Schreiber, S.K. Mazmanian, The gut microbiota-brain axis in behaviour and brain disorders. Nat. Rev. Microbiol. 19(4), 241–255 (2021). https://doi.org/10.1038/s41579-020-00460-0
M.S. Vohra, K. Benchoula, C.J. Serpell, W.E. Hwa, AgRP/NPY and POMC neurons in the arcuate nucleus and their potential role in treatment of obesity. Eur. J. Pharm. 915, 174611 (2022). https://doi.org/10.1016/j.ejphar.2021.174611
Z. Mirzadeh, C.L. Faber, M.W. Schwartz, Central nervous system control of glucose homeostasis: a therapeutic target for type 2 diabetes. Annu. Rev. Pharm. Toxicol. 62, 55–84 (2022). https://doi.org/10.1146/annurev-pharmtox-052220-010446
A. Plamboeck, S. Veedfald, C.F. Deacon, B. Hartmann, A. Wettergren, L.B. Svendsen, S. Meisner, C. Hovendal, F.K. Knop, T. Vilsbøll, J.J. Holst, Characterisation of oral and i.v. glucose handling in truncally vagotomised subjects with pyloroplasty. Eur. J. Endocrinol. 169(2), 187–201 (2013). https://doi.org/10.1530/eje-13-0264
S.C. Payne, G. Ward, J.B. Fallon, T. Hyakumura, J.B. Prins, S. Andrikopoulos, R.J. MacIsaac, J. Villalobos, Blood glucose modulation and safety of efferent vagus nerve stimulation in a type 2 diabetic rat model. Physiol. Rep. 10(8), e15257 (2022). https://doi.org/10.14814/phy2.15257
D. Borgmann, E. Ciglieri, N. Biglari, C. Brandt, A.L. Cremer, H. Backes, M. Tittgemeyer, F.T. Wunderlich, J.C. Brüning, H. Fenselau, Gut-brain communication by distinct sensory neurons differently controls feeding and glucose metabolism. Cell Metab. 33(7), 1466–1482.e7 (2021). https://doi.org/10.1016/j.cmet.2021.05.002
P.Y. Wang, L. Caspi, C.K. Lam, M. Chari, X. Li, P.E. Light, R. Gutierrez-Juarez, M. Ang, G.J. Schwartz, T.K. Lam, Upper intestinal lipids trigger a gut-brain-liver axis to regulate glucose production. Nature 452(7190), 1012–1016 (2008). https://doi.org/10.1038/nature06852
L. Du, Q. Li, H. Yi, T. Kuang, Y. Tang, G. Fan, Gut microbiota-derived metabolites as key actors in type 2 diabetes mellitus. Biomed. Pharmacother. 149, 112839 (2022). https://doi.org/10.1016/j.biopha.2022.112839
D. Parada Venegas, M.K. De la Fuente, G. Landskron, M.J. González, R. Quera, G. Dijkstra, H.J.M. Harmsen, K.N. Faber, M.A. Hermoso, Short Chain Fatty Acids (SCFAs)-mediated gut epithelial and immune regulation and its relevance for inflammatory bowel diseases. Front. Immunol. 10, 277 (2019). https://doi.org/10.3389/fimmu.2019.00277
L. Liu, J.R. Huh, K. Shah, Microbiota and the gut-brain-axis: Implications for new therapeutic design in the CNS. EBioMedicine 77, 103908 (2022). https://doi.org/10.1016/j.ebiom.2022.103908
B. van der Hee, J.M. Wells, Microbial regulation of host physiology by short-chain fatty acids. Trends Microbiol. 29(8), 700–712 (2021). https://doi.org/10.1016/j.tim.2021.02.001
X. Li, Y. Shimizu, I. Kimura, Gut microbial metabolite short-chain fatty acids and obesity. Biosci. Microbiota Food Health 36(4), 135–140 (2017). https://doi.org/10.12938/bmfh.17-010
R. Corrêa-Oliveira, J.L. Fachi, A. Vieira, F.T. Sato, M.A. Vinolo, Regulation of immune cell function by short-chain fatty acids. Clin. Transl. Immunol. 5(4), e73 (2016). https://doi.org/10.1038/cti.2016.17
J.C. McNelis, Y.S. Lee, R. Mayoral, R. van der Kant, A.M. Johnson, J. Wollam, J.M. Olefsky, GPR43 potentiates β-cell function in obesity. Diabetes 64(9), 3203–3217 (2015). https://doi.org/10.2337/db14-1938
A. Veprik, D. Laufer, S. Weiss, N. Rubins, M.D. Walker, GPR41 modulates insulin secretion and gene expression in pancreatic β-cells and modifies metabolic homeostasis in fed and fasting states. Faseb J. 30(11), 3860–3869 (2016). https://doi.org/10.1096/fj.201500030R
M. Thangaraju, G.A. Cresci, K. Liu, S. Ananth, J.P. Gnanaprakasam, D.D. Browning, J.D. Mellinger, S.B. Smith, G.J. Digby, N.A. Lambert, P.D. Prasad, V. Ganapathy, GPR109A is a G-protein-coupled receptor for the bacterial fermentation product butyrate and functions as a tumor suppressor in colon. Cancer Res. 69(7), 2826–2832 (2009). https://doi.org/10.1158/0008-5472.Can-08-4466
R.G. Xiong, D.D. Zhou, S.X. Wu, S.Y. Huang, A. Saimaiti, Z.J. Yang, A. Shang, C.N. Zhao, R.Y. Gan, and H.B. Li, Health benefits and side effects of short-chain fatty acids. Foods 11(18), (2022). https://doi.org/10.3390/foods11182863
E.E. Canfora, J.W. Jocken, E.E. Blaak, Short-chain fatty acids in control of body weight and insulin sensitivity. Nat. Rev. Endocrinol. 11(10), 577–591 (2015). https://doi.org/10.1038/nrendo.2015.128
L. Jiang, B.I. Gulanski, H.M. De Feyter, S.A. Weinzimer, B. Pittman, E. Guidone, J. Koretski, S. Harman, I.L. Petrakis, J.H. Krystal, G.F. Mason, Increased brain uptake and oxidation of acetate in heavy drinkers. J. Clin. Invest. 123(4), 1605–1614 (2013). https://doi.org/10.1172/jci65153
G. Frost, M.L. Sleeth, M. Sahuri-Arisoylu, B. Lizarbe, S. Cerdan, L. Brody, J. Anastasovska, S. Ghourab, M. Hankir, S. Zhang, D. Carling, J.R. Swann, G. Gibson, A. Viardot, D. Morrison, E. Louise Thomas, J.D. Bell, The short-chain fatty acid acetate reduces appetite via a central homeostatic mechanism. Nat. Commun. 5, 3611 (2014). https://doi.org/10.1038/ncomms4611
A. Psichas, M.L. Sleeth, K.G. Murphy, L. Brooks, G.A. Bewick, A.C. Hanyaloglu, M.A. Ghatei, S.R. Bloom, G. Frost, The short-chain fatty acid propionate stimulates GLP-1 and PYY secretion via free fatty acid receptor 2 in rodents. Int J. Obes. 39(3), 424–429 (2015). https://doi.org/10.1038/ijo.2014.153
P. Louis, H.J. Flint, Diversity, metabolism and microbial ecology of butyrate-producing bacteria from the human large intestine. FEMS Microbiol. Lett. 294(1), 1–8 (2009). https://doi.org/10.1111/j.1574-6968.2009.01514.x
C. Alexander, K.S. Swanson, G.C. Fahey, K.A. Garleb, Perspective: physiologic importance of short-chain fatty acids from nondigestible carbohydrate fermentation. Adv. Nutr. 10(4), 576–589 (2019). https://doi.org/10.1093/advances/nmz004
S.S. Pedersen, M. Prause, C. Sørensen, J. Størling, T. Moritz, E. Mariño, and N. Billestrup, Targeted delivery of butyrate improves glucose homeostasis, reduces hepatic lipid accumulation and inflammation in db/db mice. Int. J. Mol. Sci. 24(5), (2023). https://doi.org/10.3390/ijms24054533
H. Wu, V. Tremaroli, C. Schmidt, A. Lundqvist, L.M. Olsson, M. Krämer, A. Gummesson, R. Perkins, G. Bergström, F. Bäckhed, The gut microbiota in prediabetes and diabetes: a population-based cross-sectional study. Cell Metab. 32(3), 379–390.e3 (2020). https://doi.org/10.1016/j.cmet.2020.06.011
K. Ray, Gut microbiota: microbial metabolites feed into the gut-brain-gut circuit during host metabolism. Nat. Rev. Gastroenterol. Hepatol. 11(2), 76 (2014). https://doi.org/10.1038/nrgastro.2014.8
R. Li, S. Andreu-Sánchez, F. Kuipers, J. Fu, Gut microbiome and bile acids in obesity-related diseases. Best. Pr. Res Clin. Endocrinol. Metab. 35(3), 101493 (2021). https://doi.org/10.1016/j.beem.2021.101493
M.S. Trabelsi, M. Daoudi, J. Prawitt, S. Ducastel, V. Touche, S.I. Sayin, A. Perino, C.A. Brighton, Y. Sebti, J. Kluza, O. Briand, H. Dehondt, E. Vallez, E. Dorchies, G. Baud, V. Spinelli, N. Hennuyer, S. Caron, K. Bantubungi, R. Caiazzo, F. Reimann, P. Marchetti, P. Lefebvre, F. Bäckhed, F.M. Gribble, K. Schoonjans, F. Pattou, A. Tailleux, B. Staels, S. Lestavel, Farnesoid X receptor inhibits glucagon-like peptide-1 production by enteroendocrine L cells. Nat. Commun. 6, 7629 (2015). https://doi.org/10.1038/ncomms8629
M.M. Holter, M.K. Chirikjian, V.N. Govani, and B.P. Cummings, TGR5 signaling in hepatic metabolic health. Nutrients 12(9), (2020). https://doi.org/10.3390/nu12092598
M. Watanabe, S.M. Houten, C. Mataki, M.A. Christoffolete, B.W. Kim, H. Sato, N. Messaddeq, J.W. Harney, O. Ezaki, T. Kodama, K. Schoonjans, A.C. Bianco, J. Auwerx, Bile acids induce energy expenditure by promoting intracellular thyroid hormone activation. Nature 439(7075), 484–489 (2006). https://doi.org/10.1038/nature04330
C. Thomas, A. Gioiello, L. Noriega, A. Strehle, J. Oury, G. Rizzo, A. Macchiarulo, H. Yamamoto, C. Mataki, M. Pruzanski, R. Pellicciari, J. Auwerx, K. Schoonjans, TGR5-mediated bile acid sensing controls glucose homeostasis. Cell Metab. 10(3), 167–177 (2009). https://doi.org/10.1016/j.cmet.2009.08.001
J.Y.L. Chiang, J.M. Ferrell, Bile acids as metabolic regulators and nutrient sensors. Annu. Rev. Nutr. 39, 175–200 (2019). https://doi.org/10.1146/annurev-nutr-082018-124344
K.K. Ryan, R. Kohli, R. Gutierrez-Aguilar, S.G. Gaitonde, S.C. Woods, R.J. Seeley, Fibroblast growth factor-19 action in the brain reduces food intake and body weight and improves glucose tolerance in male rats. Endocrinology 154(1), 9–15 (2013). https://doi.org/10.1210/en.2012-1891
C.R. Martin, V. Osadchiy, A. Kalani, E.A. Mayer, The brain-gut-microbiome axis. Cell Mol. Gastroenterol. Hepatol. 6(2), 133–148 (2018). https://doi.org/10.1016/j.jcmgh.2018.04.003
G. Marcelin, Y.H. Jo, X. Li, G.J. Schwartz, Y. Zhang, N.J. Dun, R.M. Lyu, C. Blouet, J.K. Chang, S. Chua Jr., Central action of FGF19 reduces hypothalamic AGRP/NPY neuron activity and improves glucose metabolism. Mol. Metab. 3(1), 19–28 (2014). https://doi.org/10.1016/j.molmet.2013.10.002
P. Pathak, C. Xie, R.G. Nichols, J.M. Ferrell, S. Boehme, K.W. Krausz, A.D. Patterson, F.J. Gonzalez, J.Y.L. Chiang, Intestine farnesoid X receptor agonist and the gut microbiota activate G-protein bile acid receptor-1 signaling to improve metabolism.Hepatology 68(4), 1574–1588 (2018). https://doi.org/10.1002/hep.29857
S. Moehn, P.B. Pencharz, R.O. Ball, Lessons learned regarding symptoms of tryptophan deficiency and excess from animal requirement studies. J. Nutr. 142(12), 2231s–2235s (2012). https://doi.org/10.3945/jn.112.159061
K. Gao, C.L. Mu, A. Farzi, W.Y. Zhu, Tryptophan metabolism: a link between the gut microbiota and brain. Adv. Nutr. 11(3), 709–723 (2020). https://doi.org/10.1093/advances/nmz127
D.Y. Kim, M. Camilleri, Serotonin: a mediator of the brain-gut connection. Am. J. Gastroenterol. 95(10), 2698–2709 (2000). https://doi.org/10.1111/j.1572-0241.2000.03177.x
T. Mazda, H. Yamamoto, M. Fujimura, M. Fujimiya, Gastric distension-induced release of 5-HT stimulates c-fos expression in specific brain nuclei via 5-HT3 receptors in conscious rats. Am. J. Physiol. Gastrointest. Liver Physiol. 287(1), G228–G235 (2004). https://doi.org/10.1152/ajpgi.00373.2003
L.A. Jones, E.W. Sun, A.M. Martin, D.J. Keating, The ever-changing roles of serotonin. Int. J. Biochem. Cell Biol. 125, 105776 (2020). https://doi.org/10.1016/j.biocel.2020.105776
N. Mou, Z. Duan, P. Ma, R. Fu, D. Fan, Study on the hypnotic effect of rare protopanaxadiol-type and protopanaxatriol-type ginsenosides. RSC Adv. 9(35), 20483–20491 (2019). https://doi.org/10.1039/c9ra01549c
S.T. Breisch, F.P. Zemlan, B.G. Hoebel, Hyperphagia and obesity following serotonin depletion by intraventricular p-chlorophenylalanine. Science 192(4237), 382–385 (1976). https://doi.org/10.1126/science.130678
Y. Cai, X. Li, H. Zhou, J. Zhou, The serotonergic system dysfunction in diabetes mellitus. Front. Cell Neurosci. 16, 899069 (2022). https://doi.org/10.3389/fncel.2022.899069
L. Zhou, G.M. Sutton, J.J. Rochford, R.K. Semple, D.D. Lam, L.J. Oksanen, Z.D. Thornton-Jones, P.G. Clifton, C.Y. Yueh, M.L. Evans, R.J. McCrimmon, J.K. Elmquist, A.A. Butler, L.K. Heisler, Serotonin 2C receptor agonists improve type 2 diabetes via melanocortin-4 receptor signaling pathways. Cell Metab. 6(5), 398–405 (2007). https://doi.org/10.1016/j.cmet.2007.10.008
H. Ahlman, Nilsson, The gut as the largest endocrine organ in the body. Ann. Oncol. 12 Suppl 2, S63–S68 (2001). https://doi.org/10.1093/annonc/12.suppl_2.s63
R. Latorre, C. Sternini, R. De Giorgio, B. Greenwood-Van Meerveld, Enteroendocrine cells: a review of their role in brain-gut communication. Neurogastroenterol. Motil. 28(5), 620–630 (2016). https://doi.org/10.1111/nmo.12754
C. Sternini, L. Anselmi, E. Rozengurt, Enteroendocrine cells: a site of ‘taste’ in gastrointestinal chemosensing. Curr. Opin. Endocrinol. Diabetes Obes. 15(1), 73–78 (2008). https://doi.org/10.1097/MED.0b013e3282f43a73
S.Z. Wang, Y.J. Yu, and K. Adeli, Role of gut microbiota in neuroendocrine regulation of carbohydrate and lipid metabolism via the microbiota-gut-brain-liver axis. Microorganisms 8(4), (2020). https://doi.org/10.3390/microorganisms8040527
G.J. Dockray, Enteroendocrine cell signalling via the vagus nerve. Curr. Opin. Pharm. 13(6), 954–958 (2013). https://doi.org/10.1016/j.coph.2013.09.007
M.M. Kaelberer, K.L. Buchanan, M.E. Klein, B.B. Barth, M.M. Montoya, X. Shen, and D.V. Bohórquez, A gut-brain neural circuit for nutrient sensory transduction. Science 361(6408), (2018). https://doi.org/10.1126/science.aat5236
K.G. Margolis, J.F. Cryan, E.A. Mayer, The microbiota-gut-brain axis: from motility to mood. Gastroenterology 160(5), 1486–1501 (2021). https://doi.org/10.1053/j.gastro.2020.10.066
S.F. Mehdi, S. Pusapati, M.S. Anwar, D. Lohana, P. Kumar, S.A. Nandula, F.K. Nawaz, K. Tracey, H. Yang, D. LeRoith, M.J. Brownstein, J. Roth, Glucagon-like peptide-1: a multi-faceted anti-inflammatory agent. Front. Immunol. 14, 1148209 (2023). https://doi.org/10.3389/fimmu.2023.1148209
T.D. Müller, B. Finan, S.R. Bloom, D. D’Alessio, D.J. Drucker, P.R. Flatt, A. Fritsche, F. Gribble, H.J. Grill, J.F. Habener, J.J. Holst, W. Langhans, J.J. Meier, M.A. Nauck, D. Perez-Tilve, A. Pocai, F. Reimann, D.A. Sandoval, T.W. Schwartz, R.J. Seeley, K. Stemmer, M. Tang-Christensen, S.C. Woods, R.D. DiMarchi, M.H. Tschöp, Glucagon-like peptide 1 (GLP-1). Mol. Metab. 30, 72–130 (2019). https://doi.org/10.1016/j.molmet.2019.09.010
S. Trapp, D.I. Brierley, Brain GLP-1 and the regulation of food intake: GLP-1 action in the brain and its implications for GLP-1 receptor agonists in obesity treatment. Br. J. Pharm. 179(4), 557–570 (2022). https://doi.org/10.1111/bph.15638
C. Knauf, P.D. Cani, C. Perrin, M.A. Iglesias, J.F. Maury, E. Bernard, F. Benhamed, T. Grémeaux, D.J. Drucker, C.R. Kahn, J. Girard, J.F. Tanti, N.M. Delzenne, C. Postic, R. Burcelin, Brain glucagon-like peptide-1 increases insulin secretion and muscle insulin resistance to favor hepatic glycogen storage. J. Clin. Invest. 115(12), 3554–3563 (2005). https://doi.org/10.1172/jci25764
E.S. Bliss, E. Whiteside, The gut-brain axis, the human gut microbiota and their integration in the development of obesity. Front. Physiol. 9, 900 (2018). https://doi.org/10.3389/fphys.2018.00900
L. Jia, S. Huang, B. Sun, Y. Shang, C. Zhu, Pharmacomicrobiomics and type 2 diabetes mellitus: a novel perspective towards possible treatment. Front. Endocrinol.14, 1149256 (2023). https://doi.org/10.3389/fendo.2023.1149256
L. Wang, P. Li, Z. Tang, X. Yan, B. Feng, Structural modulation of the gut microbiota and the relationship with body weight: compared evaluation of liraglutide and saxagliptin treatment. Sci. Rep. 6, 33251 (2016). https://doi.org/10.1038/srep33251
A.A. Greenwell, J.J. Chahade, J.R. Ussher, Cardiovascular biology of the GIP receptor. Peptides 125, 170228 (2020). https://doi.org/10.1016/j.peptides.2019.170228
C.W. Chia, J.M. Egan, Incretins in obesity and diabetes. Ann. N. Y Acad. Sci. 1461(1), 104–126 (2020). https://doi.org/10.1111/nyas.14211
J. Dupre, S.A. Ross, D. Watson, J.C. Brown, Stimulation of insulin secretion by gastric inhibitory polypeptide in man. J. Clin. Endocrinol. Metab. 37(5), 826–828 (1973). https://doi.org/10.1210/jcem-37-5-826
P. Richards, N.A. Thornberry, S. Pinto, The gut-brain axis: identifying new therapeutic approaches for type 2 diabetes, obesity, and related disorders. Mol. Metab. 46, 101175 (2021). https://doi.org/10.1016/j.molmet.2021.101175
A.E. Adriaenssens, E.K. Biggs, T. Darwish, J. Tadross, T. Sukthankar, M. Girish, J. Polex-Wolf, B.Y. Lam, I. Zvetkova, W. Pan, D. Chiarugi, G.S.H. Yeo, C. Blouet, F.M. Gribble, F. Reimann, Glucose-dependent insulinotropic polypeptide receptor-expressing cells in the hypothalamus regulate food intake. Cell Metab. 30(5), 987–996.e6 (2019). https://doi.org/10.1016/j.cmet.2019.07.013
K. Miyawaki, Y. Yamada, N. Ban, Y. Ihara, K. Tsukiyama, H. Zhou, S. Fujimoto, A. Oku, K. Tsuda, S. Toyokuni, H. Hiai, W. Mizunoya, T. Fushiki, J.J. Holst, M. Makino, A. Tashita, Y. Kobara, Y. Tsubamoto, T. Jinnouchi, T. Jomori, Y. Seino, Inhibition of gastric inhibitory polypeptide signaling prevents obesity. Nat. Med. 8(7), 738–742 (2002). https://doi.org/10.1038/nm727
T. Min, S.C. Bain, The role of tirzepatide, dual GIP and GLP-1 receptor agonist, in the management of type 2 diabetes: The SURPASS clinical trials. Diabetes Ther. 12(1), 143–157 (2021). https://doi.org/10.1007/s13300-020-00981-0
M.K. Thomas, A. Nikooienejad, R. Bray, X. Cui, J. Wilson, K. Duffin, Z. Milicevic, A. Haupt, D.A. Robins, Dual GIP and GLP-1 receptor agonist tirzepatide improves beta-cell function and insulin sensitivity in type 2 diabetes. J. Clin. Endocrinol. Metab. 106(2), 388–396 (2021). https://doi.org/10.1210/clinem/dgaa863
M. Dufresne, C. Seva, D. Fourmy, Cholecystokinin and gastrin receptors. Physiol. Rev. 86(3), 805–847 (2006). https://doi.org/10.1152/physrev.00014.2005
L.I. Larsson, J.F. Rehfeld, Localization and molecular heterogeneity of cholecystokinin in the central and peripheral nervous system. Brain Res. 165(2), 201–218 (1979). https://doi.org/10.1016/0006-8993(79)90554-7
R. Chandra, R.A. Liddle, Cholecystokinin. Curr. Opin. Endocrinol. Diabetes Obes. 14(1), 63–67 (2007). https://doi.org/10.1097/MED.0b013e3280122850
G.W. Cheung, A. Kokorovic, C.K. Lam, M. Chari, T.K. Lam, Intestinal cholecystokinin controls glucose production through a neuronal network. Cell Metab. 10(2), 99–109 (2009). https://doi.org/10.1016/j.cmet.2009.07.005
W. Fan, K.L. Ellacott, I.G. Halatchev, K. Takahashi, P. Yu, R.D. Cone, Cholecystokinin-mediated suppression of feeding involves the brainstem melanocortin system. Nat. Neurosci. 7(4), 335–336 (2004). https://doi.org/10.1038/nn1214
B. Ahrén, J.J. Holst, S. Efendic, Antidiabetogenic action of cholecystokinin-8 in type 2 diabetes. J. Clin. Endocrinol. Metab. 85(3), 1043–1048 (2000). https://doi.org/10.1210/jcem.85.3.6431
K. Kasarello, A. Cudnoch-Jedrzejewska, K. Czarzasta, Communication of gut microbiota and brain via immune and neuroendocrine signaling. Front. Microbiol. 14, 1118529 (2023). https://doi.org/10.3389/fmicb.2023.1118529
L.D. Godoy, M.T. Rossignoli, P. Delfino-Pereira, N. Garcia-Cairasco, E.H. de Lima Umeoka, A comprehensive overview on stress neurobiology: basic concepts and clinical implications. Front. Behav. Neurosci. 12, 127 (2018). https://doi.org/10.3389/fnbeh.2018.00127
C.J. Hoogendoorn, J.F. Roy, J.S. Gonzalez, Shared dysregulation of homeostatic brain-body pathways in depression and type 2 diabetes. Curr. Diabetes Rep. 17(10), 90 (2017). https://doi.org/10.1007/s11892-017-0923-y
L.M. Frankiensztajn, E. Elliott, O. Koren, The microbiota and the hypothalamus-pituitary-adrenocortical (HPA) axis, implications for anxiety and stress disorders. Curr. Opin. Neurobiol. 62, 76–82 (2020). https://doi.org/10.1016/j.conb.2019.12.003
Y. Lin, Z. Zhang, S. Wang, J. Cai, J. Guo, Hypothalamus-pituitary-adrenal Axis in Glucolipid metabolic disorders. Rev. Endocr. Metab. Disord. 21(4), 421–429 (2020). https://doi.org/10.1007/s11154-020-09586-1
I. Kokkinopoulou, A. Diakoumi, and P. Moutsatsou, Glucocorticoid receptor signaling in diabetes. Int. J. Mol. Sci. 22(20), (2021). https://doi.org/10.3390/ijms222011173
U. Smith, Abdominal obesity: a marker of ectopic fat accumulation. J. Clin. Invest. 125(5), 1790–1792 (2015). https://doi.org/10.1172/jci81507
B. Misiak, I. Łoniewski, W. Marlicz, D. Frydecka, A. Szulc, L. Rudzki, J. Samochowiec, The HPA axis dysregulation in severe mental illness: Can we shift the blame to gut microbiota?. Prog. Neuropsychopharmacol. Biol. Psychiatry 102, 109951 (2020). https://doi.org/10.1016/j.pnpbp.2020.109951
K. Manohar, F.M. Mesfin, J. Liu, W.C. Shelley, J.P. Brokaw, T.A. Markel, Gut-Brain cross talk: the pathogenesis of neurodevelopmental impairment in necrotizing enterocolitis. Front. Pediatr. 11, 1104682 (2023). https://doi.org/10.3389/fped.2023.1104682
J.R. Kelly, P.J. Kennedy, J.F. Cryan, T.G. Dinan, G. Clarke, N.P. Hyland, Breaking down the barriers: the gut microbiome, intestinal permeability and stress-related psychiatric disorders. Front. Cell Neurosci. 9, 392 (2015). https://doi.org/10.3389/fncel.2015.00392
D.A. Winer, H. Luck, S. Tsai, S. Winer, The intestinal immune system in obesity and insulin resistance. Cell Metab. 23(3), 413–426 (2016). https://doi.org/10.1016/j.cmet.2016.01.003
K.Y. Hur, M.S. Lee, Gut microbiota and metabolic disorders. Diabetes Metab. J. 39(3), 198–203 (2015). https://doi.org/10.4093/dmj.2015.39.3.198
P.D. Cani, J. Amar, M.A. Iglesias, M. Poggi, C. Knauf, D. Bastelica, A.M. Neyrinck, F. Fava, K.M. Tuohy, C. Chabo, A. Waget, E. Delmée, B. Cousin, T. Sulpice, B. Chamontin, J. Ferrières, J.F. Tanti, G.R. Gibson, L. Casteilla, N.M. Delzenne, M.C. Alessi, R. Burcelin, Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes 56(7), 1761–1772 (2007). https://doi.org/10.2337/db06-1491
K. de Punder, L. Pruimboom, Stress induces endotoxemia and low-grade inflammation by increasing barrier permeability. Front. Immunol. 6, 223 (2015). https://doi.org/10.3389/fimmu.2015.00223
S. Mohammad, C. Thiemermann, Role of metabolic endotoxemia in systemic inflammation and potential interventions. Front. Immunol. 11, 594150 (2020). https://doi.org/10.3389/fimmu.2020.594150
W. He, O. Rebello, R. Savino, R. Terracciano, C. Schuster-Klein, B. Guardiola, K. Maedler, TLR4 triggered complex inflammation in human pancreatic islets. Biochim. Biophys. Acta Mol. Basis Dis. 1865(1), 86–97 (2019). https://doi.org/10.1016/j.bbadis.2018.09.030
X. Li, Y. Cai, Z. Zhang, J. Zhou, Glial and vascular cell regulation of the blood-brain barrier in diabetes. Diabetes Metab. J. 46(2), 222–238 (2022). https://doi.org/10.4093/dmj.2021.0146
M.T. Herrero, C. Estrada, L. Maatouk, S. Vyas, Inflammation in Parkinson’s disease: role of glucocorticoids. Front. Neuroanat. 9, 32 (2015). https://doi.org/10.3389/fnana.2015.00032
D. Erny, A.L. Hrabě de Angelis, D. Jaitin, P. Wieghofer, O. Staszewski, E. David, H. Keren-Shaul, T. Mahlakoiv, K. Jakobshagen, T. Buch, V. Schwierzeck, O. Utermöhlen, E. Chun, W.S. Garrett, K.D. McCoy, A. Diefenbach, P. Staeheli, B. Stecher, I. Amit, M. Prinz, Host microbiota constantly control maturation and function of microglia in the CNS. Nat. Neurosci. 18(7), 965–977 (2015). https://doi.org/10.1038/nn.4030
A. Parker, S. Fonseca, S.R. Carding, Gut microbes and metabolites as modulators of blood-brain barrier integrity and brain health. Gut Microbes 11(2), 135–157 (2020). https://doi.org/10.1080/19490976.2019.1638722
V. Braniste, M. Al-Asmakh, C. Kowal, F. Anuar, A. Abbaspour, M. Tóth, A. Korecka, N. Bakocevic, L.G. Ng, P. Kundu, B. Gulyás, C. Halldin, K. Hultenby, H. Nilsson, H. Hebert, B.T. Volpe, B. Diamond, S. Pettersson, The gut microbiota influences blood-brain barrier permeability in mice. Sci. Transl. Med. 6(263), 263ra158 (2014). https://doi.org/10.1126/scitranslmed.3009759
X. Peng, Z. Luo, S. He, L. Zhang, Y. Li, Blood-brain barrier disruption by lipopolysaccharide and sepsis-associated encephalopathy. Front Cell Infect. Microbiol. 11, 768108 (2021). https://doi.org/10.3389/fcimb.2021.768108
M. Kalyan, A.H. Tousif, S. Sonali, C. Vichitra, T. Sunanda, S.S. Praveenraj, B. Ray, V.R. Gorantla, W. Rungratanawanich, A.M. Mahalakshmi, M.W. Qoronfleh, T.M. Monaghan, B.J. Song, M.M. Essa, and S.B. Chidambaram, Role of endogenous lipopolysaccharides in neurological disorders. Cells 11(24), (2022). https://doi.org/10.3390/cells11244038
Z.H. Li, Y.Y. Jiang, C.Y. Long, Q. Peng, R.S. Yue, The gut microbiota-astrocyte axis: Implications for type 2 diabetic cognitive dysfunction. CNS Neurosci. Ther. 29 Suppl 1(Suppl 1), 59–73 (2023). https://doi.org/10.1111/cns.14077
A.M. Stranahan, S. Hao, A. Dey, X. Yu, B. Baban, Blood-brain barrier breakdown promotes macrophage infiltration and cognitive impairment in leptin receptor-deficient mice. J. Cereb. Blood Flow. Metab. 36(12), 2108–2121 (2016). https://doi.org/10.1177/0271678x16642233
T.P.M. Scheithauer, E. Rampanelli, M. Nieuwdorp, B.A. Vallance, C.B. Verchere, D.H. van Raalte, H. Herrema, Gut microbiota as a trigger for metabolic inflammation in obesity and type 2 diabetes. Front. Immunol. 11, 571731 (2020). https://doi.org/10.3389/fimmu.2020.571731
Y. Date, M. Kojima, H. Hosoda, A. Sawaguchi, M.S. Mondal, T. Suganuma, S. Matsukura, K. Kangawa, M. Nakazato, Ghrelin, a novel growth hormone-releasing acylated peptide, is synthesized in a distinct endocrine cell type in the gastrointestinal tracts of rats and humans. Endocrinology 141(11), 4255–4261 (2000). https://doi.org/10.1210/endo.141.11.7757
G. Pradhan, S.L. Samson, Y. Sun, Ghrelin: much more than a hunger hormone. Curr. Opin. Clin. Nutr. Metab. Care 16(6), 619–624 (2013). https://doi.org/10.1097/MCO.0b013e328365b9be
Q. Zeng, L. Ou, W. Wang, D.Y. Guo, Gastrin, cholecystokinin, signaling, and biological activities in cellular processes. Front. Endocrinol. 11, 112 (2020). https://doi.org/10.3389/fendo.2020.00112
M. Liguz-Lecznar, G. Dobrzanski, and M. Kossut, Somatostatin and somatostatin-containing interneurons-from plasticity to pathology. Biomolecules 12(2), (2022). https://doi.org/10.3390/biom12020312
Y. Wu, H. He, Z. Cheng, Y. Bai, X. Ma, The role of neuropeptide Y and peptide YY in the development of obesity via gut-brain axis. Curr. Protein Pept. Sci. 20(7), 750–758 (2019). https://doi.org/10.2174/1389203720666190125105401
A. De Silva, S.R. Bloom, Gut hormones and appetite control: a focus on PYY and GLP-1 as therapeutic targets in obesity. Gut Liver 6(1), 10–20 (2012). https://doi.org/10.5009/gnl.2012.6.1.10
K.C. Coate, S.A. Kliewer, D.J. Mangelsdorf, SnapShot: hormones of the gastrointestinal tract. Cell 159(6), 1478.e1 (2014). https://doi.org/10.1016/j.cell.2014.11.026
Acknowledgements
We thank all the peer reviewers for their opinions and suggestions.
Funding
This work was supported by the Key R&D Plan Social Development Project of Jiangsu Province (SBE2023741128), the National Natural Science Foundation of Jiangsu Province (SBK2023022865), the sixth phase 333 high-level talent training project of Jiangsu Province (tackling bottleneck technology) (BRA2022008).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by T.B., X.D., and J.J. The first draft of the manuscript was written by Y.P. and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pan, Y., Bu, T., Deng, X. et al. Gut microbiota and type 2 diabetes mellitus: a focus on the gut-brain axis. Endocrine 84, 1–15 (2024). https://doi.org/10.1007/s12020-023-03640-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-023-03640-z