Abstract
Purpose
To evaluate whether the clinical, biochemical and radiological features of patients with primary aldosteronism (PA) can predict both main subtypes of PA.
Methods
A retrospective multicenter study of PA patients followed in 27 Spanish tertiary hospitals (SPAIN-ALDO Register). Only patients with confirmed unilateral or bilateral PA based on adrenal venous sampling (AVS) and/or postsurgical biochemical cure after adrenalectomy were included. Supervised regression techniques were used for model development.
Results
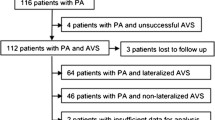
328 patients [270 unilateral PA (UPA), 58 bilateral PA (BPA)] were included. The area under the curve (AUC) for aldosterone/potassium ratio and aldosterone responses following saline infusion test were 0.602 [95%CI 0.520 to 0.684] and 0.574 [95% CI 0.446–0.701], respectively, to differentiate UPA from BPA. The AUC was 0.825 [95% 0.764–0.886] when the prediction model with seven parameters – comorbidities (dyslipidemia, cerebrovascular disease, sleep apnea syndrome [SAS]), systolic blood pressure (SBP), plasma aldosterone levels (PAC), hypokalemia and unilateral adrenal nodule >1 cm and normal contralateral adrenal gland on CT/MRI – was used. In patients without comorbidities, hypokalemia, SBP > 160 mmHg, PAC > 40 ng/dL, and unilateral adrenal lesions were associated with a likelihood of having a UPA of 98.5%. The chance of BPA was higher in individuals with comorbidities, SBP < 140 mmHg, normokalemia, low PAC levels, and no adrenal tumors on the CT/MRI (91.5%).
Conclusion
A combination of high PAC, SBP > 160 mmHg, low serum potassium, a unilateral adrenal nodule>1 cm and no comorbidities could predict a UPA with a 98.5% accuracy.


Similar content being viewed by others
References
J.W. Funder, R.M. Carey, C. Fardella, C.E. Gomez-Sanchez, F. Mantero, M. Stowasser, W.F. Young Jr, V.M. Montori, Case detection, diagnosis, and treatment of patients with primary aldosteronism: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 93(9 Sep), 3266–81 (2008). https://doi.org/10.1210/jc.2008-0104.
P. Mulatero, S. Monticone, J. Deinum, L. Amar, A. Prejbisz, M.C. Zennaro, F. Beuschlein, G.P. Rossi, T. Nishikawa, A. Morganti, T.M. Seccia, Y.H. Lin, F. Fallo, J. Widimsky, Genetics, prevalence, screening and confirmation of primary aldosteronism: a position statement and consensus of the Working Group on Endocrine Hypertension of The European Society of Hypertension. J. Hypertens. 38(10 Oct), 1919–1928 (2020). https://doi.org/10.1097/HJH.0000000000002510.
T. Nishikawa, M. Omura, F. Satoh, H. Shibata, K. Takahashi, N. Tamura, A. Tanabe; Task Force Committee on Primary Aldosteronism, The Japan Endocrine Society, Guidelines for the diagnosis and treatment of primary aldosteronism–the Japan Endocrine Society 2009. Endocr. J. 58(9), 711–21 (2011). https://doi.org/10.1507/endocrj.ej11-0133.
L. Amar, J.P. Baguet, S. Bardet, P. Chaffanjon, B. Chamontin, C. Douillard, P. Durieux, X. Girerd, P. Gosse, A. Hernigou, D. Herpin, P. Houillier, X. Jeunemaitre, F. Joffre, J.L. Kraimps, H. Lefebvre, F. Ménégaux, C. Mounier-Véhier, J. Nussberger, J.Y. Pagny, A. Pechère, P.F. Plouin, Y. Reznik, O. Steichen, A. Tabarin, M.C. Zennaro, F. Zinzindohoue, O. Chabre, SFE/SFHTA/AFCE primary aldosteronism consensus: Introduction and handbook. Ann. Endocrinol. (Paris) 77(3 Jul), 179–86 (2016). https://doi.org/10.1016/j.ando.2016.05.001.
G.P. Rossi, R.J. Auchus, M. Brown, J.W. Lenders, M. Naruse, P.F. Plouin, F. Satoh, W.F. Young Jr, An expert consensus statement on use of adrenal vein sampling for the subtyping of primary aldosteronism. Hypertension 63(1 Jan), 151–60 (2014). https://doi.org/10.1161/HYPERTENSIONAHA.113.02097.
W.F. Young, A.W. Stanson, G.B. Thompson, C.S. Grant, D.R. Farley, J.A. van Heerden, Role for adrenal venous sampling in primary aldosteronism. Surgery 136(6 Dec), 1227–35 (2004). https://doi.org/10.1016/j.surg.2004.06.051.
F. Lumachi, M. Ermani, S.M. Basso, D. Armanini, M. Iacobone, G. Favia, Long-term results of adrenalectomy in patients with aldosterone-producing adenomas: multivariate analysis of factors affecting unresolved hypertension and review of the literature. Am. Surg. 71(10 Oct), 864–9 (2005).
E.M. Küpers, L. Amar, A. Raynaud, P.F. Plouin, O. Steichen, A clinical prediction score to diagnose unilateral primary aldosteronism. J. Clin. Endocrinol. Metab. 97(10 Oct), 3530–7 (2012). https://doi.org/10.1210/jc.2012-1917.
J. Burrello, A. Burrello, J. Pieroni, E. Sconfienza, V. Forestiero, P. Rabbia, C. Adolf, M. Reincke, F. Veglio, T.A. Williams, S. Monticone, P. Mulatero, Development and validation of prediction models for subtype diagnosis of patients with primary aldosteronism. J. Clin. Endocrinol. Metab. 105(10 Oct), dgaa379 (2020). https://doi.org/10.1210/clinem/dgaa379.
H. Kobayashi, M. Abe, M. Soma, Y. Takeda, I. Kurihara, H. Itoh, H. Umakoshi, M. Tsuiki, T. Katabami, T. Ichijo, N. Wada, T. Yoshimoto, Y. Ogawa, J. Kawashima, M. Sone, N. Inagaki, K. Takahashi, M. Watanabe, Y. Matsuda, H. Shibata, K. Kamemura, T. Yanase, M. Otsuki, Y. Fujii, K. Yamamoto, A. Ogo, K. Nanba, A. Tanabe, T. Suzuki, M. Naruse, Development and validation of subtype prediction scores for the workup of primary aldosteronism. J. Hypertens. 36(11 Nov), 2269–2276 (2018). https://doi.org/10.1097/HJH.0000000000001855.
K. Nanba, M. Tsuiki, K. Nakao, A. Nanba, T. Usui, T. Tagami, Y. Hirokawa, H. Okuno, T. Suzuki, T. Shimbo, A. Shimatsu, M. Naruse, A subtype prediction score for primary aldosteronism. J. Hum. Hypertens. 28(12 Dec), 716–20 (2014). https://doi.org/10.1038/jhh.2014.20.
N. Wada, A. Miyoshi, H. Usubuchi, S. Terae, Y. Shibayama, B. Takahashi, S. Baba, H. Sugawara, S. Obara, Prediction of unilateral hyperaldosteronism on adrenal vein sampling using captopril challenge test in patients with primary aldosteronism. Endocr. J. 68(1 Jan), 45–51 (2021). https://doi.org/10.1507/endocrj.EJ20-0329.
H. Nagano, T. Kono, A. Saiga, Y. Kubota, M. Fujimoto, S.J.A. Felizola, K. Ishiwata, A. Tamura, S. Higuchi, I. Sakuma, N. Hashimoto, S. Suzuki, H. Koide, N. Takeshita, S. Sakamoto, T. Ban, K. Yokote, Y. Nakamura, T. Ichikawa, T. Uno, T. Tanaka, Aldosterone reduction rate after saline infusion test may be a novel prediction in patients with primary aldosteronism. J. Clin. Endocrinol. Metab. 105(3 Mar), dgz092 (2020). https://doi.org/10.1210/clinem/dgz092.
T. Kocjan, G. Vidmar, P. Popović, M. Stanković, Validation of three novel clinical prediction tools for primary aldosteronism subtyping. Endocr. Connect 11(5 May), e210532 (2022). https://doi.org/10.1530/EC-21-0532.
H. Umakoshi, M. Tsuiki, Y. Takeda, I. Kurihara, H. Itoh, T. Katabami, T. Ichijo, N. Wada, T. Yoshimoto, Y. Ogawa, J. Kawashima, M. Sone, N. Inagaki, K. Takahashi, M. Watanabe, Y. Matsuda, H. Kobayashi, H. Shibata, K. Kamemura, M. Otsuki, Y. Fujii, K. Yamamto, A. Ogo, T. Yanase, T. Suzuki, M. Naruse; JPAS Study Group, Significance of computed tomography and serum potassium in predicting subtype diagnosis of primary aldosteronism. J. Clin. Endocrinol. Metab. 103(3 Mar), 900–908 (2018). https://doi.org/10.1210/jc.2017-01774.
T.H. Puar, W.J. Loh, D.S. Lim, L.M. Loh, M. Zhang, R.S. Foo, L. Lee, D.S. Swee, J. Khoo, D. Tay, J.W. Kam, T. Dekkers, M. Velema, J. Deinum, P.C. Kek, Aldosterone-potassium ratio predicts primary aldosteronism subtype. J. Hypertens. 38(7 Jul), 1375–1383 (2020). https://doi.org/10.1097/HJH.0000000000002348.
M. Araujo-Castro, M. Paja Fano, M. González Boillos, B. Pla Peris, E. Pascual-Corrales, A.M. García Cano, P. Parra Ramírez, P.M. Rojas-Marcos, J.G. Ruiz-Sanchez, A. Vicente Delgado, E. Gómez Hoyos, R. Ferreira, I. García Sanz, M. Recasens Sala, R. Barahona San Millan, M.J. Picón César, P. Díaz Guardiola, J.J. García González, C.M. Perdomo, L. Manjón Miguélez, R. García Centeno, J.C. Percovich, Á. Rebollo Román, P. Gracia Gimeno, C. Robles Lázaro, M. Morales-Ruiz, F.A. Hanzu, Adrenal venous sampling in primary aldosteronism: experience of a Spanish multicentric study (Results from the SPAIN-ALDO Register). Endocrine 78(2 Nov), 363–372 (2022). https://doi.org/10.1007/s12020-022-03122-8.
M. Araujo-Castro, M. Paja Fano, M. González Boillos, B. Pla Peris, E. Pascual-Corrales, A.M. García Cano, P. Parra Ramírez, P.M. Rojas-Marcos, J.G. Ruiz-Sanchez, A. Vicente Delgado, E. Gómez Hoyos, R. Ferreira, I. García Sanz, P. Díaz Guardiola, J.J. García González, C.M. Perdomo, M. Morales, F.A. Hanzu, Evolution of the cardiometabolic profile of primary hyperaldosteronism patients treated with adrenalectomy and with mineralocorticoid receptor antagonists: results from the SPAIN-ALDO registry. Endocrine 76(3 Jun), 687–696 (2022). https://doi.org/10.1007/s12020-022-03029-4.
P.A. Harris, R. Taylor, B.L. Minor, V. Elliott, M. Fernandez, L. O’Neal, L. McLeod, G. Delacqua, F. Delacqua, J. Kirby, S.N. Duda, The REDCap consortium: Building an international community of software platform partners. J. Biomed. Inf. 95(Jul), 103208 (2019). https://doi.org/10.1016/j.jbi.2019.103208.
P.A. Harris, R. Taylor, R. Thielke, J. Payne, N. Gonzalez, J.G. Conde, Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inf. 42(2 Apr), 377–81 (2009). https://doi.org/10.1016/j.jbi.2008.08.010.
T.A. Williams, J.W.M. Lenders, P. Mulatero, J. Burrello, M. Rottenkolber, C. Adolf, F. Satoh, L. Amar, M. Quinkler, J. Deinum, F. Beuschlein, K.K. Kitamoto, U. Pham, R. Morimoto, H. Umakoshi, A. Prejbisz, T. Kocjan, M. Naruse, M. Stowasser, T. Nishikawa, W.F. Young Jr, C.E. Gomez-Sanchez, J.W. Funder, M. Reincke; Primary Aldosteronism Surgery Outcome (PASO) investigators, Outcomes after adrenalectomy for unilateral primary aldosteronism: an international consensus on outcome measures and analysis of remission rates in an international cohort. Lancet Diabetes Endocrinol. 5(9 Sep), 689–699 (2017). https://doi.org/10.1016/S2213-8587(17)30135-3.
S.H. Kim, J.H. Ahn, H.C. Hong, H.Y. Choi, Y.J. Kim, N.H. Kim, H.J. Yoo, H.Y. Kim, J.A. Seo, N.H. Kim, S.G. Kim, K.M. Choi, S.H. Baik, D.S. Choi, Changes in the clinical manifestations of primary aldosteronism. Korean J. Intern Med 29(2 Mar), 217–25 (2014). https://doi.org/10.3904/kjim.2014.29.2.217.
D.A. Heinrich, C. Adolf, L.C. Rump, I. Quack, M. Quinkler, S. Hahner, A. Januszewicz, J. Seufert, H.S. Willenberg, N. Nirschl, L. Sturm, F. Beuschlein, M. Reincke, Primary aldosteronism: key characteristics at diagnosis: a trend toward milder forms. Eur. J. Endocrinol. 178(6 Jun), 605–611 (2018). https://doi.org/10.1530/EJE-17-0978.
Z. Zhang, Q. Luo, T. Tuersun, G. Wang, T. Wu, D. Zhang, M. Wang, K. Zhou, L. Sun, N. Yue, N. Li, Higher prevalence of metabolic disorders in patients with bilateral primary aldosteronism than unilateral primary aldosteronism. Clin. Endocrinol. (Oxf.) 94(1 Jan), 3–11 (2021). https://doi.org/10.1111/cen.14318.
R. Holaj, P. Waldauf, D. Wichterle, J. Kvasnička, T. Zelinka, O. Petrák, Z. Krátká, L. Forejtová, J. Kaván, J. Widimský Jr, Adrenal venous sampling could be omitted before surgery in patients with conn’s adenoma confirmed by computed tomography and higher normal aldosterone concentration after saline infusion test. Diagnostics (Basel) 12(7 Jul), 1718 (2022). https://doi.org/10.3390/diagnostics12071718.
Z. Somlóová, J. Widimský Jr, J. Rosa, D. Wichterle, B. Strauch, O. Petrák, T. Zelinka, J. Vlková, M. Masek, J. Dvoráková, R. Holaj, The prevalence of metabolic syndrome and its components in two main types of primary aldosteronism. J. Hum. Hypertens. 24(10 Oct), 625–30 (2010). https://doi.org/10.1038/jhh.2010.65.
F.J. Zuo, X.H. Zhou, Y. Ren, T. Chen, H.M. Tian, [Clinical characteristics of aldosterone producing adenoma and idiopathic hyperaldosteronism with obstructive sleep apnea hypopnea syndrome]. Sichuan Da Xue Xue Bao Yi Xue Ban. 51(3 May), 298–303 (2020). https://doi.org/10.12182/20200560602.
F. Buffolo, Q. Li, S. Monticone, D.A. Heinrich, A. Mattei, J. Pieroni, M. Mei, S. Yang, Y.H. Hu, M.C. Yang, C. Sabbadin, F. Pizzolo, G. Giacchetti, F. Fallo, F. Veglio, M. Reincke, V.C. Wu, P. Mulatero, Primary aldosteronism and obstructive sleep apnea: a cross-sectional multi-ethnic study. Hypertension 74(6 Dec), 1532–1540 (2019). https://doi.org/10.1161/HYPERTENSIONAHA.119.13833.
Y. Song, S. Yang, W. He, J. Hu, Q. Cheng, Y. Wang, T. Luo, L. Ma, Q. Zhen, S. Zhang, M. Mei, Z. Wang, H. Qing, D. Bruemmer, B. Peng, Q. Li; Chongqing Primary Aldosteronism Study (CONPASS) Group†, Confirmatory tests for the diagnosis of primary aldosteronism: a prospective diagnostic accuracy study. Hypertension 71(1 Jan), 118–124 (2018). https://doi.org/10.1161/HYPERTENSIONAHA.117.10197.
S. Wu, J. Yang, J. Hu, Y. Song, W. He, S. Yang, R. Luo, Q. Li, Confirmatory tests for the diagnosis of primary aldosteronism: a systematic review and meta-analysis. Clin. Endocrinol. (Oxf.) 90(5 May), 641–648 (2019). https://doi.org/10.1111/cen.13943.
M.J. Kempers, J.W. Lenders, L. van Outheusden, G.J. van der Wilt, L.J. Schultze Kool, A.R. Hermus, J. Deinum, Systematic review: diagnostic procedures to differentiate unilateral from bilateral adrenal abnormality in primary aldosteronism. Ann. Intern Med 151(5 Sep), 329–37 (2009). https://doi.org/10.7326/0003-4819-151-5-200909010-00007.
T. Dekkers, A. Prejbisz, L.J.S. Kool, H.J.M.M. Groenewoud, M. Velema, W. Spiering, S. Kołodziejczyk-Kruk, M. Arntz, J. Kądziela, J.F. Langenhuijsen, M.N. Kerstens, A.H. van den Meiracker, B.J. van den Born, F.C.G.J. Sweep, A.R.M.M. Hermus, A. Januszewicz, A.F. Ligthart-Naber, P. Makai, G.J. van der Wilt, J.W.M. Lenders, J. Deinum, Adrenal vein sampling versus CT scan to determine treatment in primary aldosteronism: an outcome-based randomised diagnostic trial. Lancet Diabetes Endocrinol. 4(9 Sep), 739–746 (2016). https://doi.org/10.1016/S2213-8587(16)30100-0.
Funding
This research was funded by Sociedad Española de Endocrinología y Nutrición (SEEN).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Ethics Committee of the Hospital Universitario Ramón y Cajal. Madrid. Spain (approval date: 10th November 2020, code: ACTA 401).
Informed consent
Patient consent was waived due to the retrospective nature of the study. Only for patients who continued follow-up or prospectively included the informed consent was requested.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Parra Ramírez, P., Martín Rojas-Marcos, P., Paja Fano, M. et al. Is adrenal venous sampling always necessary to differentiate between unilateral and bilateral primary aldosteronism? Lesson from the SPAIN-ALDO register. Endocrine 84, 683–693 (2024). https://doi.org/10.1007/s12020-023-03609-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-023-03609-y