Abstract
Objective
Polycystic ovary syndrome (PCOS) is one of the risk factors for cardiovascular diseases (CVDs). However, the possible association between PCOS and common CVDs remains inconclusive. The aim of this study was to explore the potential relationship between PCOS and CVDs using genetic polymorphisms.
Methods
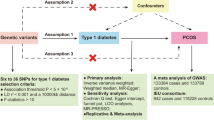
We conducted two-sample Mendelian randomization (MR) analyses. In our study, 14 single nucleotide polymorphisms (SNPs) in Europeans and another 13 SNPs in Asians were applied as instrumental variables for PCOS. The largest published meta-genome-wide association studies of European ancestry and the BioBank Japan Project of Asian ancestry were used to collect the outcome data. MR analysis was performed using inverse variance weighting as the primary method. Several sensitivity analyses and instrumental variable strength evaluations were also performed to verify the reliability of results.
Results
Our analysis revealed that any potential causal association between genetically-predicted PCOS and the risk of CVDs do not exist. These CVDs include peripheral artery disease, atrial fibrillation, arrhythmia, cardiovascular diseases, heart failure, peripheral vascular disease, hypertension, ischemic stroke, myocardial infarction and venous thromboembolisms. Associations could not be found even after the SNPs linked to these possible confounders (body mass index, waist-to-hip ratio, and serum testosterone) were deleted. Sensitivity analysis demonstrated no presence of horizontal pleiotropy or heterogeneity.
Conclusion
The present mendelian randomization study suggests that genetically-predicted PCOS may not be associated with the risk of CVDs.




Similar content being viewed by others
Data availability
Publicly available data were analyzed in this study, which can be found here: https://www.ebi.ac.uk/gwas/, https://gwas.mrcieu.ac.uk/datasets/. The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
References
H.F. Escobar-Morreale, Polycystic ovary syndrome: definition, aetiology, diagnosis and treatment. Nat Rev Endocrinol 14(5), 270–284 (2018)
M.A. Brower et al. Bidirectional Mendelian randomization to explore the causal relationships between body mass index and polycystic ovary syndrome. Hum Reprod 34(1), 127–136 (2019)
C. Riestenberg et al. Health care-related economic burden of polycystic ovary syndrome in the United States: pregnancy-related and long-term health consequences. J Clin Endocrinol Metab 107(2), 575–585 (2022)
J.V. Lazarus et al. Advancing the global public health agenda for NAFLD: a consensus statement. Nat Rev Gastroenterol Hepatol 19(1), 60–78 (2022)
C.W. Tsao et al. Heart disease and stroke statistics-2022 update: a report from the American Heart Association. Circulation 145(8), e153–e639 (2022)
A. Dokras, Cardiovascular disease risk in women with PCOS. Steroids. 78(8), 773–776 (2013)
R.E. Harvey et al. Women-specific factors to consider in risk, diagnosis and treatment of cardiovascular disease. Womens Health (Lond) 11(2), 239–257 (2015)
C. Oliver-Williams et al. Polycystic ovary syndrome as a novel risk factor for atrial fibrillation: results from a national Danish registry cohort study. Eur J Prev Cardiol 28(12), e20–e22 (2020)
R. Zehir et al. Assessment of atrial conduction time in patients with polycystic ovary syndrome. J Interv Card Electrophysiol 41(2), 137–143 (2014)
E. Gazi et al. Relationship of QT dispersion with sex hormones and insulin in young women with polycystic ovary syndrome: an observational study. Anadolu Kardiyol Derg 13(8), 772–777 (2013)
S. Zahid et al. Trends, predictors, and outcomes of cardiovascular complications associated with polycystic ovary syndrome during delivery hospitalizations: a national inpatient sample analysis (2002–2019). J Am Heart Assoc 11(16), e025839 (2022)
D. Glintborg et al. Morbidity and medicine prescriptions in a nationwide Danish population of patients diagnosed with polycystic ovary syndrome. Eur J Endocrinol 172(5), 627–638 (2015)
H. Mani et al. Diabetes and cardiovascular events in women with polycystic ovary syndrome: a 20-year retrospective cohort study. Clin Endocrinol (Oxf) 78(6), 926–934 (2013)
J. Mehilli, P. Presbitero, Coronary artery disease and acute coronary syndrome in women. Heart 106(7), 487–492 (2020)
R. Hart, D.A. Doherty, The potential implications of a PCOS diagnosis on a woman’s long-term health using data linkage. J Clin Endocrinol Metab 100(3), 911–919 (2015)
C. Meun et al. High androgens in postmenopausal women and the risk for atherosclerosis and cardiovascular disease: the Rotterdam study. J Clin Endocrinol Metab 103(4), 1622–1630 (2018)
R. Perini, Heart rate variability in normal-weight patients with polycystic ovary syndrome. Anatol J Cardiol 17(5), 410–411 (2017)
E.M. Okoroh et al. Assessing the intersection of cardiovascular disease, venous thromboembolism, and polycystic ovary syndrome. Thromb Res 136(6), 1165–1168 (2015)
D.C. Ding et al. Coronary artery disease risk in young women with polycystic ovary syndrome. Oncotarget 9(9), 8756–8764 (2018)
C.A. Emdin et al. Mendelian randomization. Jama 318(19), 1925–1926 (2017)
G. Davey Smith et al. When will Mendelian randomization become relevant for clinical practice and public health? Jama 317(6), 589–591 (2017)
S.W. Van Der Laan et al. Cystatin C and cardiovascular disease: a Mendelian randomization study. J Am Coll Cardiol 68(9), 934–945 (2016)
B.L. Pierce, S. Burgess, Efficient design for Mendelian randomization studies: subsample and 2-sample instrumental variable estimators. Am J Epidemiol 178(7), 1177–1184 (2013)
P. Simons et al. Causal relationship between polycystic ovary syndrome and coronary artery disease: a Mendelian randomisation study. Clin Endocrinol (Oxf) 96(4), 599–604 (2022)
T. Zhu et al. Polycystic ovary syndrome and risk of type 2 diabetes, coronary heart disease, and stroke. Diabetes 70(2), 627–637 (2021)
F. Day et al. Large-scale genome-wide meta-analysis of polycystic ovary syndrome suggests shared genetic architecture for different diagnosis criteria. PLoS Genet 14(12), e1007813 (2018)
F.P. Hartwig et al. Two-sample Mendelian randomization: avoiding the downsides of a powerful, widely applicable but potentially fallible technique. Int J Epidemiol 45(6), 1717–1726 (2016)
Y. Shi et al. Genome-wide association study identifies eight new risk loci for polycystic ovary syndrome. Nat Genet 44(9), 1020–1025 (2012)
Z.J. Chen et al. Genome-wide association study identifies susceptibility loci for polycystic ovary syndrome on chromosome 2p16.3, 2p21 and 9q33.3. Nat Genet 43(1), 55–59 (2011)
J. Bowden et al. Consistent estimation in Mendelian randomization with some invalid instruments using a weighted median estimator. Genet Epidemiol 40(4), 304–314 (2016)
S. Burgess, S.G. Thompson, Avoiding bias from weak instruments in Mendelian randomization studies. Int J Epidemiol 40(3), 755–764 (2011)
D.A. Lawlor et al. Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med 27(8), 1133–1163 (2008)
J. Bowden et al. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol 44(2), 512–525 (2015)
F.P. Hartwig et al. Robust inference in summary data Mendelian randomization via the zero modal pleiotropy assumption. Int J Epidemiol 46(6), 1985–1998 (2017)
M. Verbanck et al. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet 50(5), 693–698 (2018)
C.J. Lavie et al. Obesity and cardiovascular disease: risk factor, paradox, and impact of weight loss. J Am Coll Cardiol 53(21), 1925–1932 (2009)
E.D. Bode et al. Cardiovascular disease risk factors by BMI and age in United States firefighters. Obesity (Silver Spring) 29(7), 1186–1194 (2021)
B.C. Lam et al. Comparison of body mass index (BMI), body adiposity index (BAI), waist circumference (WC), waist-to-hip ratio (WHR) and waist-to-height ratio (WHtR) as predictors of cardiovascular disease risk factors in an adult population in Singapore. PLoS One 10(4), e0122985 (2015)
P. Kaminski et al. Cardiovascular risk and the use of oral contraceptives. Neuro Endocrinol Lett 34(7), 587–589 (2013)
D. Macut et al. Cardiovascular risk factors and events in women with androgen excess. J Endocrinol Invest 38(3), 295–301 (2015)
I.P. Blagojevic et al. Women with polycystic ovary syndrome and risk of cardiovascular disease. J Med Biochem 36(3), 259–269 (2017)
J.R. Staley et al. PhenoScanner: a database of human genotype-phenotype associations. Bioinformatics. 32(20), 3207–3209 (2016)
G. Hemani et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife. 7, e34408 (2018)
V. Wekker et al. Long-term cardiometabolic disease risk in women with PCOS: a systematic review and meta-analysis. Hum Reprod Update 26(6), 942–960 (2020)
J. Zhang et al. Risk of cardiovascular and cerebrovascular events in polycystic ovarian syndrome women: a meta-analysis of cohort studies. Front Cardiovasc Med 7, 552421 (2020)
S. Wild et al. Cardiovascular disease in women with polycystic ovary syndrome at long-term follow-up: a retrospective cohort study. Clin Endocrinol (Oxf) 52(5), 595–600 (2000)
S. Iftikhar et al. Risk of cardiovascular events in patients with polycystic ovary syndrome. Neth J Med 70(2), 74–80 (2012)
J.C. Lo et al. Epidemiology and adverse cardiovascular risk profile of diagnosed polycystic ovary syndrome. J Clin Endocrinol Metab 91(4), 1357–1363 (2006)
F. Ramezani Tehrani et al. Cardiovascular events among reproductive and menopausal age women with polycystic ovary syndrome: a systematic review and meta-analysis. Gynecol Endocrinol 36(1), 12–23 (2020)
E. Carmina, R.A. Lobo, Is there really increased cardiovascular morbidity in women with polycystic ovary syndrome? J Womens Health (Larchmt) 27(11), 1385–1388 (2018)
R. Azziz, Does the risk of diabetes and heart disease in women with polycystic ovary syndrome lessen with age? Fertil Steril 108(6), 959–960 (2017)
K.S. Ruth et al. Using human genetics to understand the disease impacts of testosterone in men and women. Nat Med 26(2), 252–258 (2020)
T. Mandviwala et al. Obesity and cardiovascular disease: a risk factor or a risk marker? Curr Atheroscler Rep 18(5), 21 (2016)
S. Marini et al. Mendelian randomization study of obesity and cerebrovascular disease. Ann Neurol 87(4), 516–524 (2020)
S.S. Venkatesh et al. Obesity and risk of female reproductive conditions: a Mendelian randomisation study. PLoS Med 19(2), e1003679 (2022)
T. Zhu, M.O. Goodarzi, Causes and consequences of polycystic ovary syndrome: insights from Mendelian randomization. J Clin Endocrinol Metab 107(3), e899–e911 (2022)
D. Lizneva et al. Criteria, prevalence, and phenotypes of polycystic ovary syndrome. Fertil Steril 106(1), 6–15 (2016)
Acknowledgements
The authors acknowledge all GWAS participants and investigators for their contribution to the summary statistic data. The authors thank all investigators for sharing these data.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. XZ and ZH conducted data acquisition and performed data analysis. XZ and SW performed manuscript revision. Informed consent was obtained from all individual participants included in the study.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, X., Huangfu, Z. & Wang, S. No association effect of genetic polymorphism was observed between polycystic ovary syndrome and cardiovascular diseases risk: a mendelian randomization study. Endocrine 82, 695–706 (2023). https://doi.org/10.1007/s12020-023-03467-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-023-03467-8