Abstract
Purpose
This study aims to review all published cases on the association between thyrotoxicosis and Takutsubo Syndrome by describing clinical characteristics, diagnostic work-up, treatment, and outcome.
Methods
We searched PubMed and Embase databases from inception to the 17th of February 2022 for case reports or series reporting the above-mentioned association. We extracted data on demographic characteristics, clinical features, diagnostic work-up, treatment, and clinical outcomes. Cases were stratified into groups based on the presumed cause of the thyrotoxicosis (iatrogenic vs non-iatrogenic and Graves’ diseases vs non-Graves’ disease, respectively).
Results
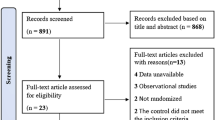
We identified 25 cases from 24 articles. The mean age was 61.7 years (+/− SD 14.5). Most patients were women (88%). Graves’ disease (52%) was the leading cause of thyrotoxicosis. Previous cancer was significantly more common in patients with iatrogenic thyrotoxicosis (P = 0.03). The most common symptoms were respiratory symptoms (68%), chest pain (56%), and palpitations (40%). The most common ECG characteristics were T-wave abnormalities (48%) and ST-elevations (36%). Elevated troponin levels were found in 92% of the cases. Patients with Graves’s disease and Takutsubo Syndrome had higher plasma levels of serum thyroxine (P = 0.03) and were more often treated with beta-blockers (P = 0.01) compared to patients with thyrotoxicosis of other origins. Notably, 40% of cases experienced in-hospital complications. No deaths were reported. All patients had improved cardiac function within a median follow-up of 42 days.
Conclusion
Evidence-based on current case reports suggests an increased risk of Takutsubo Syndrome and subsequently increased risk of in-hospital complications in patients with thyrotoxicosis.


Similar content being viewed by others
References
H. Sato, H. Taiteishi, T. Uchida, Takotsubo-type cardiomyopathy due to multivessel spasm. Clinical aspect of myocardial injury: from ischemia to heart failure: From Ischemia to Heart Failure, Kagakuhyouronsya, Tokyo, 56–64 (1990)
K. Dote, H. Sato, H. Tateishi, T. Uchida, et al. Myocardial stunning due to simultaneous multivessel coronary spasms: a review of 5 cases. J. Cardiol. 21, 203–214 (1991)
J.-R. Ghadri, I.S. Wittstein, A. Prasad, S. Sharkey, et al. International expert consensus document on Takotsubo Syndrome (Part I): Clinical characteristics, diagnostic criteria, and pathophysiology. Eur. Heart J. 39, 2032–2046 (2018). https://doi.org/10.1093/eurheartj/ehy076
D.C. Scantlebury, A. Prasad, Diagnosis of Takotsubo Cardiomyopathy:—Mayo Clinic Criteria. Circ. J. 78, 2129–2139 (2014). https://doi.org/10.1253/circj.CJ-14-0859
A. Garmendia Madariaga, S. Santos Palacios, F. Guillén-Grima, J.C. Galofré, The incidence and prevalence of thyroid dysfunction in Europe: A meta-analysis. J. Clin. Endocrinol. Metab. 99, 923–931 (2014). https://doi.org/10.1210/jc.2013-2409
J.G. Hollowell, N.W. Staehling, W.D. Flanders, W.H. Hannon, et al. Serum TSH, T 4, and thyroid antibodies in the United States population (1988 to 1994): National Health and Nutrition Examination Survey (NHANES III). J. Clin. Endocrinol. Metab. 87, 489–499 (2002). https://doi.org/10.1210/jcem.87.2.8182
S.W. Bahouth, Thyroid hormones transcriptionally regulate the beta 1-adrenergic receptor gene in cultured ventricular myocytes. J. Biol. Chem. 266, 15863–15869 (1991). https://doi.org/10.1016/S0021-9258(18)98488-7
S.W. Bahouth, X. Cui, M.J. Beauchamp, E.A. Park, Thyroid hormone Inducesβ1-adrenergic receptor gene transcription through a direct repeat separated by five nucleotides. J. Mol. Cell. Cardiol. 29, 3223–3237 (1997). https://doi.org/10.1006/jmcc.1997.0549
S. Gupta, P. Goyal, S. Idrees, S. Aggarwal, et al. Association of endocrine conditions with takotsubo cardiomyopathy: a comprehensive review. J. Am. Heart Assoc. 7, e009003 (2018). https://doi.org/10.1161/JAHA.118.009003
M.J. Page, J.E. McKenzie, P.M. Bossuyt, I. Boutron, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. n71 (2021). https://doi.org/10.1136/bmj.n71
Z. Munn, T.H. Barker, S. Moola, C. Tufanaru, et al. Methodological quality of case series studies: an introduction to the JBI critical appraisal tool. JBI Evid. Synth. 18, 2127–2133 (2020). https://doi.org/10.11124/JBISRIR-D-19-00099
A.S.M. Zuhdi, Z.H. Yaakob, M.A. Sadiq, M.D. Ismail, A.W. Undok, W.A.W. Ahmad, Takotsubo cardiomyopathy in association with hyperthyroidism. Medicine 47, 219–221 (2011)
N.W.C.J. van de Donk, Y.G.C.J. America, P.M.J. Zelissen, B.J.B. Hamer, Takotsubo cardiomyopathy following radioiodine therapy for toxic multinodular goitre. Neth. J. Med. 67, 350–352 (2009)
M. Ugurlucan, Y. Zorman, G. Ates, A. Arslan, Y. Yildiz, A. Zor, S. Cicek, Takotsubo cardiomyopathy in a patient with multiple autoimmune disorders and hyperthyroidism. Res. Cardiovasc. Med. 2, 145 (2013). https://doi.org/10.5812/cardiovascmed.10023
A.M. Saleh, S. Kramer, C. Kleinecke, M. Duecker, et al. Tako-tsubo cardiomyopathy during a thyroid storm; a critical intersection. Clinical cases from the ESC Cardiologists of Tomorrow, 1218 (2015)
T. Sakaki, Y. Fujioka, T. Akagami, M. Masai, et al. Cardiac wall motion abnormalities observed in a patient with transient hyperthyroidism. Jpn Heart J. 45, 1071–1077 (2004). https://doi.org/10.1536/jhj.45.1071
D. Rueda, R. Aguirre, D. Contardo, P. Finocchietto, et al. Takotsubo myocardiopathy and hyperthyroidism: a case report and literature review. Am. J. Case Rep. 18, 865–870 (2017). https://doi.org/10.12659/AJCR.905121
A.M. Rossor, S.H.S. Pearce, P.C. Adams, Left ventricular apical ballooning (Takotsubo Cardiomyopathy) in Thyrotoxicosis. Thyroid 17, 181–182 (2007). https://doi.org/10.1089/thy.2006.0102
A. Radhakrishnan, J.E. Granato, An association between Takotsubo cardiomyopathy and thyroid storm. Postgrad. Med. 121, 126–130 (2009). https://doi.org/10.3810/pgm.2009.05.2012
M.J. Perkins, D.T. Schachter, Biventricular Takotsubo cardiomyopathy in Graves hyperthyroidism. J. Invasive Cardiol. 26, E35–E36 (2014)
K. Patel, G.T. Griffing, P.J. Hauptman, J.M. Stolker, Recurrent Takotsubo cardiomyopathy related to recurrent thyrotoxicosis. Tex. Heart Inst. J. 43, 152–155 (2016). https://doi.org/10.14503/THIJ-15-5046
S. Omar, E. Ali, H. Mazek, T. Mahmood, et al. Takotsubo Cardiomyopathy associated with hyperthyroidism treated with thyroidectomy. Bayl. Univ. Med. Cent. Proc. 28, 194–195 (2015). https://doi.org/10.1080/08998280.2015.11929227
D. Murdoch, W. O’Callaghan, E. Reda, S. Niranjan, Takotsubo Cardiomyopathy associated with primary hyperthyroidism secondary to toxic multinodular goiter. Int J. Angiol. 25, e121–e122 (2015). https://doi.org/10.1055/s-0035-1548548
S. Miyazaki, T. Kamiishi, N. Hosokawa, M. Komura, et al. Reversible left ventricular dysfunction “takotsubo” cardiomyopathy associated with hyperthyroidism. Jpn Heart J. 45, 889–894 (2004). https://doi.org/10.1536/jhj.45.889
C.S. Martin, L.N. Ionescu, C.G. Barbu, A.E. Sirbu, et al. Takotsubo cardiomyopathy and transient thyrotoxicosis during combination therapy with interferon-alpha and ribavirin for chronic hepatitis C. BMC Endocr. Disord. 14, 10 (2014). https://doi.org/10.1186/1472-6823-14-10
S.-A. Kwon, J.H. Yang, M.-K. Kim, S.W. Park, et al. A case of Takotsubo cardiomyopathy in a patient with Iatrogenic thyrotoxicosis. Int. J. Cardiol. 145, e111–e113 (2010). https://doi.org/10.1016/j.ijcard.2009.06.040
O. Kuboyama, T. Tokunaga, K. Kobayashi, T. Iwai, et al. A case of asymptomatic patient with hyperthyroidism documented the onset of Takotsubo cardiomyopathy by holter monitoring. Int. J. Cardiol. 151, e82–e84 (2011). https://doi.org/10.1016/j.ijcard.2010.05.055
D.C. Hutchings, D. Adlam, V. Ferreira, T.D. Karamitsos, et al. Takotsubo cardiomyopathy in association with endogenous and exogenous thyrotoxicosis. QJM 104, 433–435 (2011). https://doi.org/10.1093/qjmed/hcq099
J.S. Gundara, J.C. Lee, J. Ip, S.B. Sidhu, Takotsubo cardiomyopathy complicating thyroidectomy for graves’ disease. Thyroid 22, 975–976 (2012). https://doi.org/10.1089/thy.2012.0101
M. Eliades, D. El-Maouche, C. Choudhary, B. Zinsmeister, et al. Takotsubo cardiomyopathy associated with thyrotoxicosis: a case report and review of the literature. Thyroid 24, 383–389 (2014). https://doi.org/10.1089/thy.2012.0384
A. Dimakopoulou, K. Vithian, D. Gannon, A. Harkness, Stress cardiomyopathy (Takotsubo) following radioactive iodine therapy. Endocrinology, Diabetes & Metabolism Case Reports. 2015, (2015). https://doi.org/10.1530/EDM-15-0053
E. Cervilla-Muñoz, M. Bringas-Beranek, P. Demelo-Rodríguez, Iatrogenic hyperthyroidism can be a triggering factor for takotsubo cardiomyopathy. Med. Clínica 155, 42–43 (2020). https://doi.org/10.1016/j.medcli.2019.02.014
I. Capel, E. Tasa-Vinyals, A. Cano-Palomares, I. Bergés-Raso, et al. Takotsubo cardiomyopathy in amiodarone-induced hyperthyroidism. Endocrinology, Diabetes & Metabolism Case Reports. 2017, (2017). https://doi.org/10.1530/EDM-16-0116
E. Bird-Lake, Severe transient left ventricular dysfunction induced by thyrotoxicosis. Neth. Heart J. 19, 352–354 (2011). https://doi.org/10.1007/s12471-011-0113-5
F. Alidjan, M. Ezzhati, W. Bruggeling, C. van Guldener, Takotsubo cardiomyopathy precipitated by thyrotoxicosis. Thyroid 20, 1427–1428 (2010). https://doi.org/10.1089/thy.2009.0444
A. Al-Salameh, J. Allain, P. Meimoun, T. Benali, et al. Takotsubo cardiomyopathy can occur in patients with apathetic hyperthyroidism. Thyroid 24, 400–401 (2014). https://doi.org/10.1089/thy.2013.0354
S. Aggarwal, R. Papani, V. Gupta, Can thyroid break your heart? Role of thyroid in Takotsubo cardiomyopathy: A single center retrospective study. Int. J. Cardiol. 184, 545–546 (2015). https://doi.org/10.1016/j.ijcard.2015.02.058
A. Aweimer, I. El‐Battrawy, I. Akin, M. Borggrefe, et al. Abnormal thyroid function is common in takotsubo syndrome and depends on two distinct mechanisms: results of a multicentre observational study. J. Intern. Med. 289, 675–687 (2021). https://doi.org/10.1111/joim.13189
Y.J. Akashi, K. Nakazawa, M. Sakakibara, F. Miyake, et al. 123I-MIBG myocardial scintigraphy in patients with “takotsubo” cardiomyopathy. J. Nucl. Med. 45, 1121–1127 (2004)
G.S. Levey, I. Klein, Catecholamine-thyroid hormone interactions and the cardiovascular manifestations of hyperthyroidism. Am. J. Med. 88, 642–646 (1990). https://doi.org/10.1016/0002-9343(90)90533-J
R. Vassy, Y.L. Yin, G.Y. Perret, Acute effect of T3 on beta-Adrenoceptors of Cultured Chick Cardiac Myocyte. In: Braverman LE, Eber O, Langsteger W, eds. Heart and Thyroid. Wien: Blackwell-MZV, 165–168 (1994)
B.D. Hoit, S.F. Khoury, Y. Shao, M. Gabel, et al. Effects of thyroid hormone on cardiac β-adrenergic responsiveness in conscious baboons. Circulation 96, 592–598 (1997). https://doi.org/10.1161/01.CIR.96.2.592
H. Mori, S. Ishikawa, S. Kojima, J. Hayashi, et al. Increased responsiveness of left ventricular apical myocardium to adrenergic stimuli. Cardiovasc. Res. 27, 192–198 (1993). https://doi.org/10.1093/cvr/27.2.192
A.R. Lyon, P.S. Rees, S. Prasad, P.A. Poole-Wilson, S.E. Harding, Stress (Takotsubo) cardiomyopathy—a novel pathophysiological hypothesis to explain catecholamine-induced acute myocardial stunning. Nat. Rev. Cardiol. 5, 22–29 (2008). https://doi.org/10.1038/ncpcardio1066
E.S. Bachman, T.G. Hampton, H. Dhillon, I. Amende, et al. The metabolic and cardiovascular effects of hyperthyroidism are largely independent of β-adrenergic stimulation. Endocrinology 145, 2767–2774 (2004). https://doi.org/10.1210/en.2003-1670
M. Cakir, Takotsubo cardiomyopathy in thyrotoxicosis. Int. J. Cardiol. 145, 499–500 (2010). https://doi.org/10.1016/j.ijcard.2009.10.041
J. Brenes-Salazar, Takotsubo cardiomyopathy associated with severe hypothyroidism in an elderly female. Heart Views 17, 72 (2016). https://doi.org/10.4103/1995-705X.185119
T. Micallef, M. Gruppetta, A. Cassar, S. Fava, Takotsubo cardiomyopathy and severe hypothyroidism. J. Cardiovasc. Med. 12, 824–827 (2011). https://doi.org/10.2459/JCM.0b013e3283403454
J.-R. Ghadri, I.S. Wittstein, A. Prasad, S. Sharkey, et al. International expert consensus document on Takotsubo Syndrome (Part II): diagnostic workup, outcome, and management. Eur. Heart J. 39, 2047–2062 (2018). https://doi.org/10.1093/eurheartj/ehy077
D.S. Ross, H.B. Burch, D.S. Cooper, M.C. Greenlee, et al. 2016 American Thyroid Association Guidelines for diagnosis and management of hyperthyroidism and other causes of thyrotoxicosis. Thyroid 26, 1343–1421 (2016). https://doi.org/10.1089/thy.2016.0229
G.J. Kahaly, L. Bartalena, L. Hegedüs, L. Leenhardt, K. Poppe, S.H. Pearce, 2018 European Thyroid Association Guideline for the Management of Graves’ Hyperthyroidism. Eur. Thyroid J. 7, 167–186 (2018). https://doi.org/10.1159/000490384
T.A. McDonagh, M. Metra, M. Adamo, R.S. Gardner, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. ehab368 (2021). https://doi.org/10.1093/eurheartj/ehab368
C. Templin, J.R. Ghadri, J. Diekmann, L.C. Napp, et al. Clinical features and outcomes of Takotsubo (Stress) Cardiomyopathy. N. Engl. J. Med. 373, 929–938 (2015). https://doi.org/10.1056/NEJMoa1406761
Author contributions
A.M.: conceptualization(lead), methodology (lead), investigation (lead), formal analysis (lead), writing-original draft (lead), writing-review and editing (equal), final approval of manuscript (equal), project administration (lead). T.B.: conceptualization(lead), methodology (lead), investigation (lead), formal analysis (lead), writing-original draft (lead), writing-review and editing (equal), final approval of manuscript (equal), project administration (lead). M.O.: writing-review and editing (equal), final approval of manuscript (equal). N.A.: writing-review and editing (equal), final approval of manuscript (equal). S.B.: conceptualization (supporting), writing-review and editing (equal), final approval of manuscript (equal), supervision (lead).
Funding
A.M.: no funding to declare. T.B.: no funding to declare. M.O.: no funding to declare. N.A.: no funding to declare. S.J.B.: received grant from Desirée and Niels Ydes Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohamed, A.A., Basaran, T., Othman, M.H. et al. The association between Takotsubo cardiomyopathy and thyrotoxicosis: A systematic review. Endocrine 78, 418–428 (2022). https://doi.org/10.1007/s12020-022-03174-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-022-03174-w