Abstract
Purpose
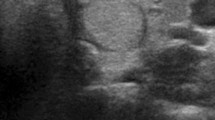
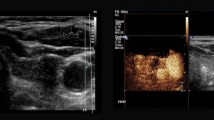
Nonhomogenous and ill-defined hypoechoic areas are typical ultrasonographic features of subacute thyroiditis (SAT). Evaluating a thyroid nodule accurately in this heterogeneous paranchime may be troublesome. This study aims to compare thyroid nodules, their characteristics, and European Thyroid Imaging and Reporting Data System (EU-TIRADS) categories at the time of the diagnosis and in the remission of SAT.
Methods
Ultrasonographic features of SAT and characteristics and EU-TIRADS categories of thyroid nodules in the initial and control ultrasonography (US) of 350 patients with SAT have been evaluated in this retrospective observational study. Fine needle aspiration biopsy (FNAB) results and postsurgical data, if performed, have been estimated.
Results
A hundred patients (28.6%) with SAT had thyroid nodules at the time of the diagnosis, while 152 (43.4%) patients had a nodule in remission US (p < 0.001). The number of thyroid nodules was found to be higher in the control US as against the initial US (p = 0.001). EU-TIRADS scores of the nodules in the remission US were significantly higher than the scores at the time of the diagnosis (p < 0.001). FNAB was performed in 23% of nodules observed in the remission US, and the rate of thyroid carcinoma within them was 3.3%.
Conclusion
Thyroid nodules, malignancy suspected features, and EU-TIRADS categories of them may not be appropriately evaluated due to heterogenous paranchime of SAT. Performing a control US examination after resolution of hypoechoic areas may be beneficial to avoid missing clinically significant nodules with high EU-TIRADS scores.


Similar content being viewed by others
References
E. Nishihara, H. Ohye, N. Amino, K. Takata, T. Arishima, T. Kudo et al. Clinical characteristics of 852 patients with subacute thyroiditis before treatment. Inter. Med. 47, 725–729 (2008). https://doi.org/10.2169/internalmedicine.47.0740
S. Hepsen, P. Akhanli, M.E. Sencar, H. Duger, D. Sakiz, M. Kizilgul et al. The evaluation of low- and high-dose steroid treatments in subacute thyroiditis: a retrospective observational study. Endocr. Pract. 27, 594–600 (2021). https://doi.org/10.1016/j.eprac.2020.11.009
S.Y. Park, E.-K. Kim, M.J. Kim, B.M. Kim, K.K. Oh, S.W. Hong et al. Ultrasonographic characteristics of subacute granulomatous thyroiditis. Korean J. Radiol. 7, 229 (2006). https://doi.org/10.3348/kjr.2006.7.4.229
M.C. Frates, E. Marqusee, C.B. Benson, E.K. Alexander, Subacute granulomatous (de Quervain) thyroiditis. J. Ultrasound Med. 32, 505–511 (2013). https://doi.org/10.7863/jum.2013.32.3.505
B. Ucan, T. Delibasi, E. Cakal, M.S. Arslan, N.C. Bozkurt, T. Demirci et al. Papillary thyroid cancer case masked by subacute thyroiditis. Arq. Bras. Endocrinol. Metabol. 58, 851–854 (2014). https://doi.org/10.1590/0004-2730000003222
N. Gül, A.K. Üzüm, Ö.S. Selçukbiricik, G. Yegen, R. Tanakol, F. Aral, Prevalence of papillary thyroid cancer in subacute thyroiditis patients may be higher than it is presumed: retrospective analysis of 137 patients. Radiol. Oncol. 52, 257–262 (2018). https://doi.org/10.2478/raon-2018-0027
E. Nishihara, M. Hirokawa, H. Ohye, M. Ito, S. Kubota, S. Fukata et al. Papillary carcinoma obscured by complication with subacute thyroiditis: sequential ultrasonographic and histopathological findings in five cases. Thyroid 18, 1221–1225 (2008). https://doi.org/10.1089/thy.2008.0096
E. Nishihara, T. Kudo, M. Ito, S. Fukata, M. Nishikawa, H. Nakamura et al. Papillary thyroid carcinomas are highly obscured by inflammatory hypoechoic regions caused by subacute thyroiditis: a longitudinal evaluation of 710 patients using ultrasonography. Endocr. J. 67, 569–574 (2020). https://doi.org/10.1507/endocrj.EJ19-0597
G. Russ, S.J. Bonnema, M.F. Erdogan, C. Durante, R. Ngu, L. Leenhardt, European thyroid association guidelines for ultrasound malignancy risk stratification of thyroid nodules in adults: The EU-TIRADS. Eur. Thyroid J. 6, 225–237 (2017). https://doi.org/10.1159/000478927
J. Brunn, U. Block, G. Ruf, I. Bos, W.P. Kunze, P.C. Scriba, Volumetrie der Schilddrüsenlappen mittels Real-time-Sonographie * 1. DMW. Dtsch Med. Wochenschr 106, 1338–1340 (2008). https://doi.org/10.1055/s-2008-1070506
J.E. Park, S.M. Hwang, J.-Y. Hwang, J.H. Moon, I. Yang, J.Y. Woo et al. The relationship between ultrasound findings and thyroid function in children and adolescent autoimmune diffuse thyroid diseases. Sci. Rep. 11, 19709 (2021). https://doi.org/10.1038/s41598-021-99016-2
C. Marcocci, P. Vitti, F. Cetani, F. Catalano, R. Concetti, A. Pinchera, Thyroid ultrasonography helps to identify patients with diffuse lymphocytic thyroiditis who are prone to develop hypothyroidism. J. Clin. Endocrinol. Metab. 72, 209–213 (1991). https://doi.org/10.1210/jcem-72-1-209
E.S. Cibas, S.Z. Ali, The 2017 Bethesda system for reporting thyroid cytopathology. Thyroid 27, 1341–1346 (2017). https://doi.org/10.1089/thy.2017.0500
B.R. Haugen, E.K. Alexander, K.C. Bible, G.M. Doherty, S.J. Mandel, Y.E. Nikiforov et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid 26, 1–133 (2016). https://doi.org/10.1089/thy.2015.0020
Y.-K. Chen, C.-L. Lin, Y.-J. Chang, F.T.-F. Cheng, C.-L. Peng, F.-C. Sung et al. Cancer Risk in Patients with Graves’ Disease: A Nationwide Cohort Study. Thyroid 23, 879–884 (2013). https://doi.org/10.1089/thy.2012.0568
K. Gul, A. Dirikoc, G. Kiyak, P.E. Ersoy, N.S. Ugras, R. Ersoy et al. The Association Between Thyroid Carcinoma and Hashimoto’s Thyroiditis: The Ultrasonographic and Histopathologic Characteristics of Malignant Nodules. Thyroid 20, 873–878 (2010). https://doi.org/10.1089/thy.2009.0118
J.P. Brito, M.R. Gionfriddo, A. Al Nofal, K.R. Boehmer, A.L. Leppin, C. Reading et al. The accuracy of thyroid nodule ultrasound to predict thyroid cancer: systematic review and meta-analysis. J. Clin. Endocrinol. Metab. 99, 1253–1263 (2014). https://doi.org/10.1210/jc.2013-2928
L.R. Remonti, C.K. Kramer, C.B. Leitão, L.C.F. Pinto, J.L. Gross, Thyroid ultrasound features and risk of carcinoma: a systematic review and meta-analysis of observational studies. Thyroid 25, 538–550 (2015). https://doi.org/10.1089/thy.2014.0353
W.-J. Moon, S.L. Jung, J.H. Lee, D.G. Na, J.-H. Baek, Y.H. Lee et al. Benign and malignant thyroid nodules: US differentiation—multicenter retrospective study. Radiology 247, 762–770 (2008). https://doi.org/10.1148/radiol.2473070944
J.Y. Lee, D.G. Na, S.J. Yoon, H.Y. Gwon, W. Paik, T. Kim et al. Ultrasound malignancy risk stratification of thyroid nodules based on the degree of hypoechogenicity and echotexture. Eur. Radiol 30, 1653–1663 (2020). https://doi.org/10.1007/s00330-019-06527-8
Y. Ito, A. Miyauchi, H. Inoue, M. Fukushima, M. Kihara, T. Higashiyama et al. An observational trial for papillary thyroid microcarcinoma in Japanese Patients. World J. Surg. 34, 28–35 (2010). https://doi.org/10.1007/s00268-009-0303-0
Y.S. Lee, B.-J. Lee, H.J. Hong, K.-D. Lee, Current trends of practical issues concerning micropapillary thyroid carcinoma. Medicine 96, e8596 (2017). https://doi.org/10.1097/MD.0000000000008596
J.P. Brito, N. Singh-Ospina, M.R. Gionfriddo, S. Maraka, A. Espinosa De Ycaza, R. Rodriguez-Gutierrez et al. Restricting ultrasound thyroid fine needle aspiration biopsy by nodule size: which tumors are we missing? A population-based study. Endocrine 51, 499–505 (2016). https://doi.org/10.1007/s12020-015-0713-8
Author contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by S.H., H.B., P.A., M.E.S., M.K., O.O., and B.U.. The first draft of the manuscript was written by S.H. and all authors commented on previous versions of the manuscript. E.C. supervised the study. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of University of Health Sciences, Diskapi Yildirim Beyazit Training and Research Hospital (Date: 28.06.2019/No:66/13).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hepsen, S., Bostan, H., Akhanli, P. et al. Subacute thyroiditis paranchime heterogeneity may mask thyroid nodules and higher EU-TIRADS scores. Endocrine 77, 291–296 (2022). https://doi.org/10.1007/s12020-022-03069-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-022-03069-w