Abstract
Background
Lipohypertrophy (LHT) has been suggested as an outcome of the adipogenic effects of insulin injection-related tissue trauma. It commonly occurs in the clinical setting, but the current understanding of LHT by the medical staff and diabetes patients remains insufficient; moreover, it has not garnered attention as a research topic.
Objective
To investigate the ultrasound characterization of LHT, to identify the factors associated with LHT development by assessing the prevalence of LHT and compare the accuracy of clinical palpation with that of ultrasonography in LHT detection, and to further evaluate the possible impact of LHT on patients’ blood glucose fluctuations.
Method
A cross-sectional study was conducted in 120 patients with type 2 diabetes. Patients’ general information were obtained using a questionnaire, and the patients were evaluated for LHT by ultrasonography and clinical palpation of the abdomen. The patients were instructed to inject equal amounts of insulin in tissues with LHT and in normal adipose tissues (NATs) in two non-consecutive d in a selected week; the possible effect of LHT on patients’ blood glucose fluctuations was assessed using a continuous glucose monitoring system.
Results
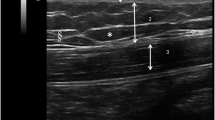
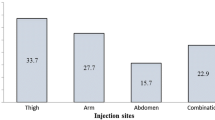
LHT has characteristic ultrasonic signs. We found a high rate of missed LHT detection on clinical palpation compared with that on ultrasonography (P < 0.05). The duration of insulin treatment, rotation of injection sites, frequency of needle reuse, and number of insulin injections per day were the primary factors influencing the development of LHT (P < 0.05). Compared with NATs, LHT tissues showed extremely elevated amplitude of glycemic excursion, mean blood glucose levels, standard deviation of blood glucose levels and postprandial glucose excursion, and large fluctuations in blood glucose levels (P < 0.05).
Conclusion
Ultrasonography can more accurately detect LHT than can clinical palpation. LHT development is associated with several factors and can lead to significant fluctuations in blood glucose levels; thus, sufficient attention should be paid to investigating the underlying mechanism of LHT.


Similar content being viewed by others
References
S. Famulla, U. Hövelmann, A. Fischer et al. Insulin Injection Into Lipohypertrophic Tissue: Blunted and More Variable Insulin Absorption and Action and Impaired Postprandial Glucose Control.[J]. Diabetes Care 39, 1486–92 (2016)
D. Luo, Y. Shi, M. Zhu et al. Subclinical lipohypertrophy–Easily ignored complications of insulin therapy.[J]. J. Diabetes Complications 35, 107806 (2021)
G.H. Abu, R. Hashem, A. Forbes et al. A Systematic Review of Ultrasound-Detected Lipohypertrophy in Insulin-Exposed People with Diabetes.[J]. Diabetes Ther. 9, 1741–1756 (2018)
S. Gentile, F. Strollo, G. Guarino et al. Why are so huge differences reported in the occurrence rate of skin lipohypertrophy? Does it depend on method defects or on lack of interest?[J]. Diabetes Metab. Syndr. 13, 682–686 (2019)
M.D. Pavlović, T. Milenković, M. Dinić et al. The prevalence of cutaneous manifestations in young patients with type 1 diabetes.[J]. Diabetes Care 30, 1964–7 (2007)
F.F. Li, S.M. Fu, Z.P. Liu et al. Injection sites lipohypertrophy among 736 patients with type 2 diabetes of different-grade hospitals[J]. J. Clin. Exp. Med. 9, 13178–13183 (2016).
A. Barola, P. Tiwari, A. Bhansali et al. Insulin-Related Lipohypertrophy: Lipogenic Action or Tissue Trauma?[J]. Front. Endocrinol. (Lausanne) 9, 638 (2018)
S. Mike, C. Linda, S. Kenneth, UK lipohypertrophy interventional study.[J]. Diabetes Res Clin Pract 126, 248–253 (2017).
U. Hovelmann, S. Famulla, L. Hermanski et al. Insulin injection into regions with lipohypertrophy (LHT) worsens postprandial (PP) blood glucose (BG) versus injections into normal adipose tissue (NAT) [J]. Diabetes 64(suppl 1), A254–A5 (2015)
L. Ji, Z. Sun, Q. Li et al. Lipohypertrophy in China: Prevalence, Risk Factors, Insulin Consumption, and Clinical Impact.[J]. Diabetes Technol. Ther. 19, 61–67 (2017)
Chinese Diabetes Journal Guide and Consensus Writing Committee, Chinese guideline on diabetes drug injection technology (2016 edition). Chin. J. Diabetes Metab. 9(2), 79–105 (2017)
B. F, M. E, B. E et al. Ultrasound characterization of insulin induced lipohypertrophy in type 1 diabetes mellitus [J]. J. Endocrinol. Investig. 40(10), 1107–13 (2017)
N. Volkova, I. Davidenko, J. Rudakova, et al. Insulin-induced lipohypertrophy diagnostics in diabetic patients: subcutaneous fat ultrasonography[J]. Endocr. Abstracts (2015).
F. J, F. M, Y. S et al. Insulin-induced lipohypertrophy: report of a case with histopathology [J]. Endocr. J. 52(5), 623–8 (2005)
S. Gentile, G. Guarino, A. Giancaterini et al. A suitable palpation technique allows to identify skin lipohypertrophic lesions in insulin-treated people with diabetes.[J]. Springerplus 5, 563 (2016)
W. Wang, R. Huang, Y. Chen et al. Values of ultrasound for diagnosis and management of insulin-induced lipohypertrophy: A prospective cohort study in China.[J]. Med. (Baltim.) 100, e26743 (2021)
H. Mulnier et al. Subcutaneous tissue changes and dermal inflammation at insulin injections sites: a feasibility study using ultrasound to describe characterise and grade lipohypertrophy. Diabetologia 60(1 Suppl 1), S90 (2017)
J. Kapeluto et al. Criteria for the detection of insulin-induced lipohypertrophy using ultrasonography. Can. J. Diabetes 39(6), 534 (2015)
M. Blanco, M.T. Hernández, K.W. Strauss et al. Prevalence and risk factors of lipohypertrophy in insulin-injecting patients with diabetes.[J]. Diabetes Metab. 39, 445–53 (2013)
M.A. Omar, A.A. El-Kafoury, R.I. El-Araby, Lipohypertrophy in children and adolescents with type 1 diabetes and the associated factors.[J]. BMC Res. Notes 4, 290 (2011)
A.N. AlJaber, I. Sales, T.H. Almigbal et al. The prevalence of lipohypertrophy and its associated factors among Saudi patients with type 2 diabetes mellitus.[J]. J. Taibah Univ. Med. Sci. 15, 224–231 (2020)
J. Overland, L. Molyneaux, S. Tewari et al. Lipohypertrophy: does it matter in daily life? A study using a continuous glucose monitoring system.[J]. Diabetes Obes. Metab. 11, 460–3 (2009)
G. Grassi, P. Scuntero, R. Trepiccioni et al. Optimizing insulin injection technique and its effect on blood glucose control.[J]. J. Clin. Transl. Endocrinol. 1, 145–150 (2014)
U.-B. Johansson, S. Amsberg, L. Hannerz et al. Impaired absorption of insulin aspart from lipohypertrophic injection sites.[J]. Diabetes Care 28, 2025–7 (2005)
S. Gentile, Metabolic consequences of incorrect insulin administration technique: Lypohypertrophy[J]. G. Ital. di Diabetologia e Metab. 30(3), 97–99 (2010)
T.A. Chowdhury, Poor glycaemic control caused by insulin induced lipohypertrophy[J]. Bmj 327(7411), 383–384 (2003)
L. Chen, Q. Xing, L.I. Jing et al. 337-OR: Injection Technique (IT) Training in Subjects Injecting into Lipohypertrophy (LH)—The Tianjin Randomized Controlled Trial (RCT)[J]. Diabetes 68(Supplement 1), 337-OR (2019)
Author information
Authors and Affiliations
Contributions
Y.L. contributed to the conception of the study and paper. L.L. and W.W. performed the experiments and analyzed the data. J.H. contributed to perform the experiments. H.Z. contributed to the conception of the study and paper preparation.
Funding
This work was supported by the Guide Project of FuJian Province of China (2019Y0072).
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lin, Y., Lin, L., Wang, W. et al. Insulin-related lipohypertrophy: ultrasound characteristics, risk factors, and impact of glucose fluctuations. Endocrine 75, 768–775 (2022). https://doi.org/10.1007/s12020-021-02904-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02904-w