Abstract
Purpose
The aim of the study was to evaluate the relationship between changes in hemoglobin A1c (HbA1c) and exercise levels in type 2 diabetes mellitus (T2DM) patients when performing various types of exercise.
Methods
The inclusion criteria were randomized controlled trials involving adults with T2DM, intervention involving exercise alone, the overall duration of intervention ≥12 weeks, and reporting HbA1c. Weighted mean difference (WMD) was defined as the mean difference between the intervention group and the control group weighted by the inverse of the squared standard error for each study, and all WMDs were pooled as overall effects. A meta-regression analysis was performed to evaluate the relationship between the exercise level and the WMD in HbA1c.
Results
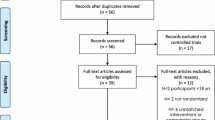
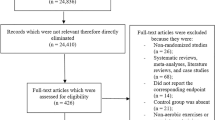
Forty-eight studies (2395 subjects) were analyzed. The pooled WMD in HbA1c decreased significantly (−0.5% [95% confidence intervals: −0.6 to −0.4]) but contained significant heterogeneity (Q = 103.8, P < 0.01; I2 = 36.6%). A meta-regression analysis showed that the intensity (metabolic equivalents [METs]), time (min/session), or frequency (sessions/week) of the exercise was not associated with the HbA1c. However, the overall duration of exercise (weeks) was significantly associated with the WMD in HbA1c (meta-regression coefficient: 0.01 [95% confidence intervals: 0.002−0.016]; R2 = 70.0%), and that result did not contain significant heterogeneity (P > 0.05; I2 = 14.7%).
Conclusions
The exercise intervention decreases HbA1c in T2DM patients. In addition, exercise for an extended duration was associated with an increase in HbA1c, so the effects of exercise may be evident early on, but results suggested that exercise for a prolonged period alone may increase HbA1c.


Similar content being viewed by others
Data availability
All data are available in submitted paper or as electronic supplementary material.
References
International Diabetes Federation: IDF Diabetes Atlas 9th (eds.). https://www.diabetesatlas.org (2019). Accessed: 15 June 2021
M. Fujishima, Y. Kiyohara, I. Kato, et al., Diabetes and cardiovascular disease in a prospective population survey in Japan: The Hisayama Study. Diabetes 45, S14–S16 (1996). https://doi.org/10.2337/diab.45.3.s14
I.M. Stratton, A.I. Adler, H.A. Neil, et al., Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ 321, 405–412 (2000). https://doi.org/10.1136/bmj.321.7258.405
A.K. Wright, E. Kontopantelis, R. Emsley, et al., Cardiovascular risk and risk factor management in type 2 diabetes mellitus. Circulation 139, 2742–2753 (2019). https://doi.org/10.1161/CIRCULATIONAHA.118.039100
C.J. Currie, J.R. Peters, A. Tynan, et al., Survival as a function of HbA(1c) in people with type 2 diabetes: a retrospective cohort study. Lancet 375, 481–489 (2010). https://doi.org/10.1016/S0140-6736(09)61969-3
J.I. Chiang, P. Hanlon, T.C. Li, et al., Multimorbidity, mortality, and HbA1c in type 2 diabetes: a cohort study with UK and Taiwanese cohorts. PLoS Med. 17, e1003094 (2020). https://doi.org/10.1371/journal.pmed.1003094
E. Selvin, S. Marinopoulos, G. Berkenblit, et al., Meta-analysis: glycosylated hemoglobin and cardiovascular disease in diabetes mellitus. Ann. Intern. Med. 141, 421–431 (2004). https://doi.org/10.7326/0003-4819-141-6-200409210-00007
Z. Shan, Y. Li, G. Zong, et al., Rotating night shift work and adherence to unhealthy lifestyle in predicting risk of type 2 diabetes: results from two large US cohorts of female nurses. BMJ 363, k4641 (2018). https://doi.org/10.1136/bmj.k4641
T. Honda, H. Kishimoto, N. Mukai, et al., Objectively measured sedentary time and diabetes mellitus in a general Japanese population: The Hisayama Study. J. Diabetes Investig. 10, 809–816 (2019). https://doi.org/10.1111/jdi.12968
E.G. Wilmot, C.L. Edwardson, F.A. Achana, et al., Sedentary time in adults and the association with diabetes, cardiovascular disease and death: systematic review and meta-analysis. Diabetologia 55, 2895–2905 (2012). https://doi.org/10.1007/s00125-012-2677-z
B.E. Ainsworth, W.L. Haskell, M.C. Whitt, et al., Compendium of physical activities: an update of activity codes and MET intensities. Med. Sci. Sports Exerc. 32, S498–S504 (2000). https://doi.org/10.1097/00005768-200009001-00009
American Diabetes Association: Standards of Medical Care in Diabetes-2019, Abridged for primary care providers. Clin. Diabetes 37, 11–34 (2019). https://doi.org/10.2337/cd18-0105
H. Sone, S. Tanaka, S. Tanaka, et al., Leisure-time physical activity is a significant predictor of stroke and total mortality in Japanese patients with type 2 diabetes: analysis from the Japan Diabetes Complications Study (JDCS). Diabetologia 56, 1021–1030 (2013). https://doi.org/10.1007/s00125-012-2810-z
K. Okada, T. Hayashi, K. Tsumura, C. Suematsu, G. Endo, S. Fujii, Leisure-time physical activity at weekends and the risk of type 2 diabetes mellitus in Japanese men: the Osaka Health Survey. Diabet. Med. 17, 53–58 (2000). https://doi.org/10.1046/j.1464-5491.2000.00229.x
J.E. Manson, E.B. Rimm, M.J. Stampfer, et al., Physical activity and incidence of non-insulin-dependent diabetes mellitus in women. Lancet 338, 774–778 (1991). https://doi.org/10.1016/0140-6736(91)90664-b
J.E. Manson, D.M. Nathan, A.S. Krolewski, M.J. Stampfer, W.C. Willett, C.H. Hennekens, A prospective study of exercise and incidence of diabetes among US male physicians. JAMA 268, 63–67 (1992). https://doi.org/10.1001/jama.1992.03490010065031
P. Huai, H. Han, K.H. Reilly, X. Guo, J. Zhang, A. Xu, Leisure-time physical activity and risk of type 2 diabetes: a meta-analysis of prospective cohort studies. Endocrine 52, 226–230 (2016). https://doi.org/10.1007/s12020-015-0769-5
Y. Zhang, X.F. Pan, J. Chen, et al., Combined lifestyle factors and risk of incident type 2 diabetes and prognosis among individuals with type 2 diabetes: a systematic review and meta-analysis of prospective cohort studies. Diabetologia 63, 21–33 (2020). https://doi.org/10.1007/s00125-019-04985-9
R.S. Delevatti, C.G. Bracht, S.D.C. Lisboa, et al., The role of aerobic training variables progression on glycemic control of patients with type 2 diabetes: a systematic review with meta-analysis. Sports Med. Open 5, 22 (2019). https://doi.org/10.1186/s40798-019-0194-z
S. Qiu, X. Cai, U. Schumann, M. Velders, Z. Sun, J.M. Steinacker, Impact of walking on glycemic control and other cardiovascular risk factors in type 2 diabetes: a meta-analysis. PLoS One 9, e109767 (2014). https://doi.org/10.1371/journal.pone.0109767
S. Qiu, X. Cai, X. Chen, B. Yang, Z. Sun, Step counter use in type 2 diabetes: a meta-analysis of randomized controlled trials. BMC Med. 12, 36 2014). https://doi.org/10.1186/1741-7015-12-36
Y. Liu, W. Ye, Q. Chen, Y. Zhang, C.H. Kuo, M. Korivi, Resistance exercise intensity is correlated with attenuation of HbA1c and insulin in patients with type 2 diabetes: a systematic review and meta-analysis. Int. J. Environ. Res. Public Health 16, 140 (2019). https://doi.org/10.3390/ijerph16010140
P. Acosta-Manzano, M. Rodriguez-Ayllon, F.M. Acosta, D. Niederseer, J. Niebauer, Beyond general resistance training. Hypertrophy versus muscular endurance training as therapeutic interventions in adults with type 2 diabetes mellitus: a systematic review and meta-analysis. Obes. Rev. 21, e13007 (2020). https://doi.org/10.1111/obr.13007
J.X. Liu, L. Zhu, P.J. Li, N. Li, Y.B. Xu, Effectiveness of high-intensity interval training on glycemic control and cardiorespiratory fitness in patients with type 2 diabetes: a systematic review and meta-analysis. Aging Clin. Exp. Res. 31, 575–593 (2019). https://doi.org/10.1007/s40520-018-1012-z
D. Umpierre, P.A. Ribeiro, B.D. Schaan, J.P. Ribeiro, Volume of supervised exercise training impacts glycaemic control in patients with type 2 diabetes: a systematic review with meta-regression analysis. Diabetologia 56, 242–251 (2013). https://doi.org/10.1007/s00125-012-2774-z
D. Umpierre, P.A. Ribeiro, C.K. Kramer, et al., Physical activity advice only or structured exercise training and association with HbA1c levels in type 2 diabetes: a systematic review and meta-analysis. JAMA 305, 1790–1799 (2011). https://doi.org/10.1001/jama.2011.576
M. Chao, C. Wang, X. Dong, M. Ding, The effects of tai chi on type 2 diabetes mellitus: a meta-analysis. J. Diabetes Res. 2018, 7350567 (2018). https://doi.org/10.1155/2018/7350567
R. Ramamoorthi, D. Gahreman, T. Skinner, S. Moss, The effect of yoga practice on glycemic control and other health parameters in the prediabetic state: a systematic review and meta-analysis. PLoS One 14, e0221067 (2019). https://doi.org/10.1371/journal.pone.0221067
T. Xia, Y. Yang, W. Li, et al., Meditative movements for patients with type 2 diabetes: a systematic review and meta-analysis. Evid. Based Complement. Alternat. Med. 2020, 5745013 (2020). https://doi.org/10.1155/2020/5745013
L.W. Pai, T.C. Li, Y.J. Hwu, S.C. Chang, L.L. Chen, P.Y. Chang, The effectiveness of regular leisure-time physical activities on long-term glycemic control in people with type 2 diabetes: A systematic review and meta-analysis. Diabetes Res. Clin. Pract. 113, 77–85 (2016). https://doi.org/10.1016/j.diabres.2016.01.011
J.L. Rees, S.T. Johnson, N.G. Boulé, Aquatic exercise for adults with type 2 diabetes: a meta-analysis. Acta. Diabetol. 54, 895–904 (2017). https://doi.org/10.1007/s00592-017-1023-9
L. Shamseer, D. Moher, M. Clarke, et al., Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ 350, g7647 (2015). https://doi.org/10.1136/bmj.g7647
PROSPERO: International Prospective Register of Systematic Reviews (Centre for reviews and dissemination, University of York, 2011), https://www.crd.york.ac.uk/prospero. Accessed: 15 June 2021.
American Diabetes Association, 6. Glycemic targets: standards of medical care in diabetes-2020. Diabetes Care 43, S66–S76 (2020). https://doi.org/10.2337/dc20-S006
Cochrane Skin Group: Data collection forms for intervention reviews: RCTs only, version 3. https://skin.cochrane.org/resources (2014). Accessed: 15 June 2021
L. Vanhees, N. Geladas, D. Hansen, et al., Importance of characteristics and modalities of physical activity and exercise in the management of cardiovascular health in individuals with cardiovascular risk factors: recommendations from the EACPR. Part II. Eur. J. Prev. Cardiol. 19, 1005–1033 (2012). https://doi.org/10.1177/1741826711430926
J.A.C. Sterne, J. Savović, M.J. Page, et al., RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366, l4898 (2019). https://doi.org/10.1136/bmj.l4898
Y. Igarashi, Y. Nogami, Running to lower resting blood pressure: a systematic review and meta-analysis. Sports Med. 50, 531–541 (2020). https://doi.org/10.1007/s40279-019-01209-3
R.M. Harbord, J.P.T. Higgins, Meta-regression in Stata. Stata J. 8, 493–519 (2008). https://doi.org/10.1177/1536867X0800800403
R.J. Hardy, S.G. Thompson, A likelihood approach to meta-analysis with random effects. Stat. Med. 15, 619–629 (1996). https://doi.org/10.1002/(SICI)1097-0258(19960330)15:63.0.CO;2-A
D. Langan, J.P.T. Higgins, D. Jackson, et al., A comparison of heterogeneity variance estimators in simulated random-effects meta-analyses. Res. Synth. Methods 10, 83–98 (2019). https://doi.org/10.1002/jrsm.1316
A.M. Aloe, B.J. Becker, T.D. Pigott, An alternative to R(2) for assessing linear models of effect size. Res. Synth. Methods 1, 272–283 (2010). https://doi.org/10.1002/jrsm.23
J.P. Higgins, S.G. Thompson, J.J. Deeks, D.G. Altman, Measuring inconsistency in meta-analyses. BMJ 327, 557–560 (2003). https://doi.org/10.1136/bmj.327.7414.557
M. Egger, S.G. Davey, M. Schneider, C. Minder, Bias in meta-analysis detected by a simple, graphical test. BMJ 315, 629–634 (1997). https://doi.org/10.1136/bmj.315.7109.629
S. Duval, R. Tweedie, Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56, 455–463 (2000). https://doi.org/10.1111/j.0006-341x.2000.00455.x
G.H. Guyatt, A.D. Oxman, R. Kunz, et al., What is “quality of evidence” and why is it important to clinicians?. BMJ 336, 995–998 (2008). https://doi.org/10.1136/bmj.39490.551019.BE
G. Jabardo-Camprubí, R. Donat-Roca, M. Sitjà-Rabert, R. Milà-Villarroel, J. Bort-Roig, Drop-out ratio between moderate to high-intensity physical exercise treatment by patients with, or at risk of, type 2 diabetes mellitus: a systematic review and meta-analysis. Physiol. Behav. 215, 112786 (2020). https://doi.org/10.1016/j.physbeh.2019.112786
R.E. Ashton, G.A. Tew, J.J. Aning, S.E. Gilbert, L. Lewis, J.M. Saxton, Effects of short-term, medium-term and long-term resistance exercise training on cardiometabolic health outcomes in adults: systematic review with meta-analysis. Br. J. Sports Med. 54, 341–348 (2020). https://doi.org/10.1136/bjsports-2017-098970
G.A. Silverii, L. Botarelli, I. Dicembrini, et al., Low-carbohydrate diets and type 2 diabetes treatment: a meta-analysis of randomized controlled trials. Acta. Diabetol. 57, 1375–1382 (2020). https://doi.org/10.1007/s00592-020-01568-8
L.J. Orozco, A.M. Buchleitner, G. Gimenez-Perez, M.R.I. Figuls, B. Richter, D. Mauricio, Exercise or exercise and diet for preventing type 2 diabetes mellitus. Cochrane Database Syst. Rev. 2008, CD003054 (2008). https://doi.org/10.1002/14651858.CD003054.pub3
K.I. Stanford, L.J. Goodyear, Exercise and type 2 diabetes: molecular mechanisms regulating glucose uptake in skeletal muscle. Adv. Physiol. Educ. 38, 308–314 (2014). https://doi.org/10.1152/advan.00080.2014
H. Ohnishi, S. Saitoh, S. Takagi, et al., Incidence of insulin resistance in obese subjects in a rural Japanese population: the Tanno and Sobetsu study. Diabetes Obes. Metab. 7, 83–87 (2005). https://doi.org/10.1111/j.1463-1326.2004.00381.x
T. Okura, R. Nakamura, Y. Fujioka, et al., Body mass index ≥23 is a risk factor for insulin resistance and diabetes in Japanese people: a brief report. PLoS One 13, e0201052 (2018). https://doi.org/10.1371/journal.pone.0201052
Y. Hayashino, J.L. Jackson, T. Hirata, et al., Effects of exercise on C-reactive protein, inflammatory cytokine, and adipokine in patients with type 2 diabetes: a meta-analysis of randomized controlled trials. Metabolism 63, 431–440 (2014). https://doi.org/10.1016/j.metabol.2013.08.018
T. Suzuki, J. Imai, T. Yamada, et al., Interleukin-6 enhances glucose-stimulated insulin secretion from pancreatic beta-cells: potential involvement of the PLC-IP3-dependent pathway. Diabetes 60, 537–547 (2011). https://doi.org/10.2337/db10-0796
R.J.S. Costa, R.M.J. Snipe, C.M. Kitic, P.R. Gibson, Systematic review: exercise-induced gastrointestinal syndrome-implications for health and intestinal disease. Aliment. Pharmacol. Ther. 46, 246–265 (2017). https://doi.org/10.1111/apt.14157
Acknowledgements
The authors wish to sincerely thank the staff of Osaka City University Media Center Library Service for collecting the articles used in this analysis and to thank the staff of Toin University of Yokohama Library, National Museum of Ethnology, and National Institute of Public Health for facilitating a search of the literature in electronic databases.
Author contributions
Y.I. conceived the study, conducted a literature search, analyzed the data, and drafted the paper. N.A. conducted a literature search, analyzed the data, and drafted the paper. S.M. conceived the study and drafted the paper. All authors have approved the final paper and agree with its submission to the journal.
Funding
No sources of funding were used to assist in the preparation of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Igarashi, Y., Akazawa, N. & Maeda, S. The relationship between the level of exercise and hemoglobin A1c in patients with type 2 diabetes mellitus: a systematic review and meta-analysis. Endocrine 74, 546–558 (2021). https://doi.org/10.1007/s12020-021-02817-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02817-8