Abstract
Purpose
Somatotroph adenomas are obviously heterogeneous in clinical characteristics, imaging performance, pathological diagnosis and therapeutic effect. The heterogeneity of the tumors, especially for SG and DG type adenomas, have attracted great interest in identifying the specific pathological markers and therapeutic targets of them. However, previous analyses of the molecular characteristics of the subtypes of somatotroph adenomas were performed at genomic and transcriptome level. The proteomic differences between the two subtypes of somatotroph adenomas are still unknown.
Methods
Tumor samples were surgically removed from 10 sporadic pituitary somatotroph adenoma patients and grouped according to the pathological type. Tandem mass tag (TMT)-based quantitative proteomic analysis was employed to analyze the proteomic differences between SG and DG tumors.
Results
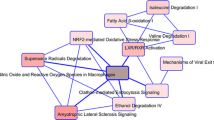
In total, 228 differentially expressed proteins were identified between SG adenomas and DG adenomas. They were enriched mainly in extracellular matrix (ECM)-receptor interaction, leukocyte transendothelial migration, arrhythmogenic right ventricular cardiomyopathy and DNA replication pathways. Protein-protein interaction (PPI) network analysis indicated that Cadherin-1 and Catenin beta-1 were the most important key proteins in the differences between SG and DG adenomas. Immunohistochemistry (IHC) confirmed the expression levels of the key proteins.
Conclusions
This study provides large-scale proteome molecular characteristics of distinct granulation subtypes of somatotroph adenomas. Compared with DG adenomas, The differential protein of SG adenomas mostly enrich in invasive and proliferative functions and pathways at the proteomic level. Cadherin-1 and Catenin beta-1 play key roles in the different biological characteristics of the two tumor subtypes.





Similar content being viewed by others
References
C. Capatina, J.A. Wass, 60 years of neuroendocrinology: acromegaly. J. Endocrinol. 226(2), T141–160 (2015). https://doi.org/10.1530/joe-15-0109
S. Melmed, Acromegaly pathogenesis and treatment. J. Clin. Invest. 119(11), 3189–3202 (2009). https://doi.org/10.1172/jci39375
O.M. Dekkers, N.R. Biermasz, A.M. Pereira, J.A. Romijn, J.P. Vandenbroucke, Mortality in acromegaly: a metaanalysis. J. Clin. Endocrinol. Metab. 93(1), 61–67 (2008). https://doi.org/10.1210/jc.2007-1191
A. Ben-Shlomo, S. Melmed, Acromegaly. Endocrinol. Metab. Clin. North Am. 37(1), 101–122 (2008). https://doi.org/10.1016/j.ecl.2007.10.002. viii
S.L. Asa, W. Kucharczyk, S. Ezzat, Pituitary acromegaly: not one disease. Endocr. Relat. Cancer 24(3), C1–c4 (2017). https://doi.org/10.1530/erc-16-0496
K. Kiseljak-Vassiliades, N.E. Carlson, M.T. Borges, B.K. Kleinschmidt-DeMasters, K.O. Lillehei, J.M. Kerr, M.E. Wierman, Growth hormone tumor histological subtypes predict response to surgical and medical therapy. Endocrine 49(1), 231–241 (2015). https://doi.org/10.1007/s12020-014-0383-y
B. Mayr, R. Buslei, M. Theodoropoulou, G.K. Stalla, M. Buchfelder, C. Schöfl, Molecular and functional properties of densely and sparsely granulated GH-producing pituitary adenomas. Eur. J. Endocrinol. 169(4), 391–400 (2013). https://doi.org/10.1530/eje-13-0134
S.L. Asa, S. Ezzat, The pathogenesis of pituitary tumors. Annu. Rev. Pathol. 4, 97–126 (2009). https://doi.org/10.1146/annurev.pathol.4.110807.092259
I. Potorac, P. Petrossians, A.F. Daly, O. Alexopoulou, S. Borot, M. Sahnoun-Fathallah, F. Castinetti, F. Devuyst, M.L. Jaffrain-Rea, C. Briet, F. Luca, M. Lapoirie, F. Zoicas, I. Simoneau, A.M. Diallo, A. Muhammad, F. Kelestimur, E. Nazzari, R.G. Centeno, S.M. Webb, M.L. Nunes, V. Hana, V. Pascal-Vigneron, I. Ilovayskaya, F. Nasybullina, S. Achir, D. Ferone, S.J. Neggers, B. Delemer, J.M. Petit, C. Schöfl, G. Raverot, B. Goichot, P. Rodien, B. Corvilain, T. Brue, F. Schillo, L. Tshibanda, D. Maiter, J.F. Bonneville, A. Beckers, T2-weighted MRI signal predicts hormone and tumor responses to somatostatin analogs in acromegaly. Endocr. Relat. Cancer 23(11), 871–881 (2016). https://doi.org/10.1530/erc-16-0356
S. Melmed, Pathogenesis of pituitary tumors. Nat. Rev. Endocrinol. 7(5), 257–266 (2011). https://doi.org/10.1038/nrendo.2011.40
A. Obari, T. Sano, K. Ohyama, E. Kudo, Z.R. Qian, A. Yoneda, N. Rayhan, M. Mustafizur Rahman, S. Yamada, Clinicopathological features of growth hormone-producing pituitary adenomas: difference among various types defined by cytokeratin distribution pattern including a transitional form. Endocr. Pathol. 19(2), 82–91 (2008). https://doi.org/10.1007/s12022-008-9029-z
F. Langlois, R. Woltjer, J.S. Cetas, M. Fleseriu, Silent somatotroph pituitary adenomas: an update. Pituitary 21(2), 194–202 (2018). https://doi.org/10.1007/s11102-017-0858-y
M.H. Schernthaner-Reiter, G. Trivellin, C.A. Stratakis, MEN1, MEN4, and carney complex: pathology and molecular genetics. Neuroendocrinology 103(1), 18–31 (2016). https://doi.org/10.1159/000371819
J. Trouillas, F. Labat-Moleur, N. Sturm, M. Kujas, M.F. Heymann, D. Figarella-Branger, M. Patey, M. Mazucca, E. Decullier, B. Vergès, O. Chabre, A. Calender, Pituitary tumors and hyperplasia in multiple endocrine neoplasia type 1 syndrome (MEN1): a case-control study in a series of 77 patients versus 2509 non-MEN1 patients. Am. J. Surg. Pathol. 32(4), 534–543 (2008). https://doi.org/10.1097/PAS.0b013e31815ade45
D. Iacovazzo, R. Caswell, B. Bunce, S. Jose, B. Yuan, L.C. Hernández-Ramírez, S. Kapur, F. Caimari, J. Evanson, F. Ferraù, M.N. Dang, P. Gabrovska, S.J. Larkin, O. Ansorge, C. Rodd, M.L. Vance, C. Ramírez-Renteria, M. Mercado, A.P. Goldstone, M. Buchfelder, C.P. Burren, A. Gurlek, P. Dutta, C.S. Choong, T. Cheetham, G. Trivellin, C.A. Stratakis, M.B. Lopes, A.B. Grossman, J. Trouillas, J.R. Lupski, S. Ellard, J.R. Sampson, F. Roncaroli, M. Korbonits, Germline or somatic GPR101 duplication leads to X-linked acrogigantism: a clinico-pathological and genetic study. Acta Neuropathol. Commun. 4(1), 56 (2016). https://doi.org/10.1186/s40478-016-0328-1
S. Salenave, A.M. Boyce, M.T. Collins, P. Chanson, Acromegaly and McCune-Albright syndrome. J. Clin. Endocrinol. Metab. 99(6), 1955–1969 (2014). https://doi.org/10.1210/jc.2013-3826
Eva, H, Kalman, K, Pathology of acromegaly. Neuroendocrinology (2006).
Y. Bakhtiar, H. Hirano, K. Arita, S. Yunoue, S. Fujio, A. Tominaga, T. Sakoguchi, K. Sugiyama, K. Kurisu, J. Yasufuku-Takano, K. Takano, Relationship between cytokeratin staining patterns and clinico-pathological features in somatotropinomae. Eur. J. Endocrinol. 163(4), 531–539 (2010). https://doi.org/10.1530/eje-10-0586
O. Mete, M.B. Lopes, Overview of the 2017 WHO classification of pituitary tumors. Endocr. Pathol. 28(3), 228–243 (2017). https://doi.org/10.1007/s12022-017-9498-z
S.L. Fougner, O. Casar-Borota, A. Heck, J.P. Berg, J. Bollerslev, Adenoma granulation pattern correlates with clinical variables and effect of somatostatin analogue treatment in a large series of patients with acromegaly. Clin. Endocrinol. 76(1), 96–102 (2012). https://doi.org/10.1111/j.1365-2265.2011.04163.x
K. Kiseljak-Vassiliades, T.S. Mills, Y. Zhang, M. Xu, K.O. Lillehei, B.K. Kleinschmidt-DeMasters, M.E. Wierman, Elucidating the role of the desmosome protein p53 apoptosis effector related to PMP-22 in growth hormone tumors. Endocrinology 158(5), 1450–1460 (2017). https://doi.org/10.1210/en.2016-1841
T. Xie, Y. Tang, R. Luo, X. Zhang, S. Wu, Y. Gu, T. Liu, F. Hu, GPR64 promotes cAMP pathway in tumor aggressiveness in sparsely granulated growth hormone cell adenomas. Endocrine (2020). https://doi.org/10.1007/s12020-020-02263-y
P. Kahn, From genome to proteome: looking at a cell’s proteins. Science 270(5235), 369–370 (1995). https://doi.org/10.1126/science.270.5235.369
J. Zecha, S. Satpathy, T. Kanashova, S.C. Avanessian, M.H. Kane, K.R. Clauser, P. Mertins, S.A. Carr, B. Kuster, TMT labeling for the masses: a robust and cost-efficient, in-solution labeling approach. Mol. Cell. Proteom. 18(7), 1468–1478 (2019). https://doi.org/10.1074/mcp.TIR119.001385
N. Stallard, Practical statistics for medical research by D. G. Altman. J. R. Stat. Soc. 49(4), 179–361 (2000).
S.C.Y. Leung, T.O. Nielsen, L.A. Zabaglo, I. Arun, S.S. Badve, A.L. Bane, J.M.S. Bartlett, S. Borgquist, M.C. Chang, A. Dodson, A. Ehinger, S. Fineberg, C.M. Focke, D. Gao, A.M. Gown, C. Gutierrez, J.C. Hugh, Z. Kos, A.V. Laenkholm, M.G. Mastropasqua, T. Moriya, S. Nofech-Mozes, C.K. Osborne, F.M. Penault-Llorca, T. Piper, T. Sakatani, R. Salgado, J. Starczynski, T. Sugie, B. van der Vegt, G. Viale, D.F. Hayes, L.M. McShane, M. Dowsett, Analytical validation of a standardised scoring protocol for Ki67 immunohistochemistry on breast cancer excision whole sections: an international multicentre collaboration. Histopathology 75(2), 225–235 (2019). https://doi.org/10.1111/his.13880
M. Li, X. Wu, J. Wang, Y. Pan, Towards the identification of protein complexes and functional modules by integrating PPI network and gene expression data. BMC Bioinform. 13, 109 (2012). https://doi.org/10.1186/1471-2105-13-109
G.D. Bader, C.W.V. Hogue, An automated method for finding molecular complexes in large protein interaction networks. BMC Bioinform. 4, 2 (2003)
L. Katznelson, E.R. Laws Jr, S. Melmed, M.E. Molitch, M.H. Murad, A. Utz, J.A. Wass, Acromegaly: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 99(11), 3933–3951 (2014). https://doi.org/10.1210/jc.2014-2700
T. Xie, T. Liu, X. Zhang, L. Chen, R. Luo, W. Sun, F. Hu, Y. Yu, Y. Gu, Z. Lu, Time to revive the value of the pseudocapsule in endoscopic endonasal transsphenoidal surgery for growth hormone adenomas. World Neurosurg. 89, 65–71 (2016). https://doi.org/10.1016/j.wneu.2016.01.036
A. Giustina, G. Barkhoudarian, A. Beckers, A. Ben-Shlomo, N. Biermasz, B. Biller, C. Boguszewski, M. Bolanowski, J. Bollerslev, V. Bonert, M. Bronstein, M. Buchfelder, F. Casanueva, P. Chanson, D. Clemmons, M. Fleseriu, A. Formenti, P. Freda, M. Gadelha, E. Geer, M. Gurnell, A. Heaney, K. Ho, A. Ioachimescu, S. Lamberts, E. Laws, M. Losa, P. Maffei, A. Mamelak, M. Mercado, M. Molitch, P. Mortini, A. Pereira, S. Petersenn, K. Post, M. Puig-Domingo, R. Salvatori, S. Samson, I. Shimon, C. Strasburger, B. Swearingen, P. Trainer, M. Vance, J. Wass, M. Wierman, K. Yuen, M. Zatelli, S. Melmed, Multidisciplinary management of acromegaly: a consensus. Rev. Endocr. Metab. Disord. 21(4), 667–678 (2020). https://doi.org/10.1007/s11154-020-09588-z
A.M. Abu Dabrh, K. Mohammed, N. Asi, W.H. Farah, Z. Wang, M.H. Farah, L.J. Prokop, L. Katznelson, M.H. Murad, Surgical interventions and medical treatments in treatment-naive patients with acromegaly: systematic review and meta-analysis. J. Clin. Endocrinol. Metab. 99(11), 4003–4014 (2014). https://doi.org/10.1210/jc.2014-2900
S. Petersenn, Management of aggressive pituitary tumors - a 2019 update. Horm. Metab. Res. 51(12), 755–764 (2019). https://doi.org/10.1055/a-1060-1883
A. Colao, R.S. Auriemma, G. Lombardi, R. Pivonello, Resistance to somatostatin analogs in acromegaly. Endocr. Rev. 32(2), 247–271 (2011). https://doi.org/10.1210/er.2010-0002
S. Larkin, R. Reddy, N. Karavitaki, S. Cudlip, J. Wass, O. Ansorge, Granulation pattern, but not GSP or GHR mutation, is associated with clinical characteristics in somatostatin-naive patients with somatotroph adenomas. Eur. J. Endocrinol. 168(4), 491–499 (2013). https://doi.org/10.1530/eje-12-0864
E. Horvath, K. Kovacs, Pathology of acromegaly. Neuroendocrinology 83(3-4), 161–165 (2006). https://doi.org/10.1159/000095524
S. Murphy, P. Dowling, K. Ohlendieck, Comparative skeletal muscle proteomics using two-dimensional gel electrophoresis. Proteomes 4(3) (2016). https://doi.org/10.3390/proteomes4030027
L.E. Scott, S.H. Weinberg, C.A. Lemmon, Mechanochemical signaling of the extracellular matrix in epithelial-mesenchymal transition. Front Cell Dev. Biol. 7, 135 (2019). https://doi.org/10.3389/fcell.2019.00135
D.I. Bellovin, R.C. Bates, A. Muzikansky, D.L. Rimm, A.M. Mercurio, Altered localization of p120 catenin during epithelial to mesenchymal transition of colon carcinoma is prognostic for aggressive disease. Cancer Res. 65(23), 10938–10945 (2005). https://doi.org/10.1158/0008-5472.Can-05-1947
F.X. Bosch, C. Andl, U. Abel, J. Kartenbeck, E-cadherin is a selective and strongly dominant prognostic factor in squamous cell carcinoma: a comparison of E-cadherin with desmosomal components. Int. J. Cancer 114(5), 779–790 (2005). https://doi.org/10.1002/ijc.20782
W. Yu, L. Yang, T. Li, Y. Zhang, Cadherin signaling in cancer: its functions and role as a therapeutic target. Front. Oncol. 9, 989 (2019). https://doi.org/10.3389/fonc.2019.00989
M. Takeichi, Multiple functions of α-catenin beyond cell adhesion regulation. Curr. Opin. Cell Biol. 54, 24–29 (2018). https://doi.org/10.1016/j.ceb.2018.02.014
P.D. McCrea, C.J. Gottardi, Beyond β-catenin: prospects for a larger catenin network in the nucleus. Nat. Rev. Mol. Cell Biol. 17(1), 55–64 (2016). https://doi.org/10.1038/nrm.2015.3
I.S. Gul, P. Hulpiau, Y. Saeys, F. van Roy, Evolution and diversity of cadherins and catenins. Exp. Cell Res. 358(1), 3–9 (2017). https://doi.org/10.1016/j.yexcr.2017.03.001
P.D. McCrea, D. Gu, The catenin family at a glance. J. Cell Sci. 123(Pt 5), 637–642 (2010). https://doi.org/10.1242/jcs.039842
N. Ishiyama, R. Sarpal, M.N. Wood, S.K. Barrick, T. Nishikawa, H. Hayashi, A.B. Kobb, A.S. Flozak, A. Yemelyanov, R. Fernandez-Gonzalez, S. Yonemura, D.E. Leckband, C.J. Gottardi, U. Tepass, M. Ikura, Force-dependent allostery of the α-catenin actin-binding domain controls adherens junction dynamics and functions. Nat. Commun. 9(1), 5121 (2018). https://doi.org/10.1038/s41467-018-07481-7
D. Ollech, T. Pflästerer, A. Shellard, C. Zambarda, J.P. Spatz, P. Marcq, R. Mayor, R. Wombacher, E.A. Cavalcanti-Adam, An optochemical tool for light-induced dissociation of adherens junctions to control mechanical coupling between cells. Nat. Commun. 11(1), 472 (2020). https://doi.org/10.1038/s41467-020-14390-1
I. Kaszak, O. Witkowska-Piłaszewicz, Z. Niewiadomska, B. Dworecka-Kaszak, F. Ngosa Toka, P. Jurka, Role of cadherins in cancer—a review. Int. J. Mol. Sci. 21(20) (2020). https://doi.org/10.3390/ijms21207624
G. Berx, F. Van Roy, The E-cadherin/catenin complex: an important gatekeeper in breast cancer tumorigenesis and malignant progression. Breast Cancer Res. 3(5), 289–293 (2001). https://doi.org/10.1186/bcr309
R. Aamodt, J. Bondi, S.N. Andersen, A. Bakka, G. Bukholm, I.R. Bukholm, The prognostic impact of protein expression of e-cadherin-catenin complexes differs between rectal and colon carcinoma. Gastroenterol. Res. Pract. 2010 (2010). https://doi.org/10.1155/2010/616023
C. Salon, S. Lantuejoul, B. Eymin, S. Gazzeri, C. Brambilla, E. Brambilla, The E-cadherin-beta-catenin complex and its implication in lung cancer progression and prognosis. Future Oncol. 1(5), 649–660 (2005). https://doi.org/10.2217/14796694.1.5.649
N. Chauvet, N. Romanò, A.C. Meunier, E. Galibert, P. Fontanaud, M.N. Mathieu, G. Osterstock, P. Osterstock, E. Baccino, V. Rigau, H. Loiseau, S. Bouillot-Eimer, A. Barlier, P. Mollard, N. Coutry, Combining cadherin expression with molecular markers discriminates invasiveness in growth hormone and prolactin pituitary adenomas. J. Neuroendocrinol. 28(2), 12352 (2016). https://doi.org/10.1111/jne.12352
B. Xu, T. Sano, K. Yoshimoto, S. Yamada, Downregulation of E-cadherin and its undercoat proteins in pituitary growth hormone cell adenomas with prominent fibrous bodies. Endocr. Pathol. 13(4), 341–351 (2002). https://doi.org/10.1385/ep:13:4:341
T. Sano, Q.Z. Rong, N. Kagawa, S. Yamada, Down-regulation of E-cadherin and catenins in human pituitary growth hormone-producing adenomas. Front. Horm. Res. 32, 127–132 (2004). https://doi.org/10.1159/000079041
R.A. Laskey, M.A. Madine, A rotary pumping model for helicase function of MCM proteins at a distance from replication forks. EMBO Rep. 4(1), 26–30 (2003). https://doi.org/10.1038/sj.embor.embor706
J.M. Bailis, S.L. Forsburg, MCM proteins: DNA damage, mutagenesis and repair. Curr. Opin. Genet. Dev. 14(1), 17–21 (2004). https://doi.org/10.1016/j.gde.2003.11.002
C.U. Köhler, A. Kreuter, M.C. Rozynkowski, T. Rahmel, W. Uhl, A. Tannapfel, W.E. Schmidt, J.J. Meier, Validation of different replication markers for the detection of beta-cell proliferation in human pancreatic tissue. Regul. Pept. 162(1–3), 115–121 (2010). https://doi.org/10.1016/j.regpep.2009.12.021
T. Hallén, D.S. Olsson, C. Hammarstrand, C. Örndal, A. Engvall, O. Ragnarsson, T. Skoglund, G. Johannsson, MCM7 as a marker of postsurgical progression in non-functioning pituitary adenomas. Eur. J. Endocrinol. 184(4), 521–531 (2021). https://doi.org/10.1530/eje-20-1086
A. Coli, S.L. Asa, G. Fadda, D. Scannone, S. Chiloiro, L. De Marinis, L. Lauretti, F.O. Ranelletti, L. Lauriola, Minichromosome maintenance protein 7 as prognostic marker of tumor aggressiveness in pituitary adenoma patients. Eur. J. Endocrinol. 174(3), 307–314 (2016). https://doi.org/10.1530/eje-15-0586
C.M. Dallago, L.M. Barbosa-Coutinho, N.P. Ferreira, R. Meurer, J.F. Pereira-Lima, C. Oliveira Mda, Determination of cell proliferation using Mcm2 antigen and evaluation of apoptosis and TGF-beta1 expression in GH-secreting or clinically nonfunctioning pituitary adenomas. Endocr. Pathol. 21(1), 32–39 (2010). https://doi.org/10.1007/s12022-010-9107-x
Acknowledgements
We thank and acknowledge all of the participants in the study.
Funding
Foundation of Science and Technology Commission of Shanghai Municipality (19ZR1409800).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Tang, Y., Xie, T., Wu, S. et al. Quantitative proteomics revealed the molecular characteristics of distinct types of granulated somatotroph adenomas. Endocrine 74, 375–386 (2021). https://doi.org/10.1007/s12020-021-02767-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02767-1