Abstract
Purpose
We aimed to investigate the characteristics of kidney disease in severely obese Japanese patients with type 2 diabetes mellitus (T2DM).
Methods
This was a cross-sectional study of severely obese patients (body mass index ≥35 kg/m2) with T2DM treated at Jinnouchi Hospital, Kumamoto, Japan.
Results
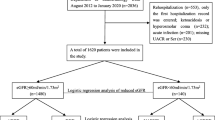
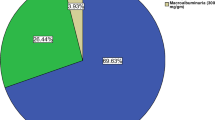
A total of 3128 T2DM patients visited the hospital during the survey period, of whom 55 patients (1.7%) were severely obese and 50 patients were enrolled. In terms of diabetic nephropathy (DN), twenty-five patients were stage 1 (non-DN, 50.0%), sixteen were stage 2 (32.0%), five were stage 3 (10.0%), and four were stage 4 (8.0%). There were significant differences in the presence of urinary occult blood (P = 0.01) and history of cardiovascular disease (CVD) (P = 0.04) between patients with DN (stages 2–4) and those without DN (stage 1). The presence of urinary occult blood (odds ratio [OR], 4.96; 95% confidence interval, 1.32–18.6; P = 0.02) was significantly associated with the presence of DN according to multivariate logistic regression analysis with forced inclusion of age, sex, and CVD history.
Conclusions
Urinary occult blood may be a significant independent factor associated with the presence of nephropathy in severely obese Japanese patients with T2DM. The presence of urinary occult blood could thus be an important pathogenic factor in obesity-related nephropathy in patients with T2DM.


Similar content being viewed by others
References
National Institutes of Diabetes DaKD, The National Institutes of Health. U. S. Renal Data System: USRDS 2006 annual data report. NIDDK The National Institutes of Health, 2006
S.P. Salvatore, J.M. Chevalier, S.F. Kuo, P.F. Audia, S.V. Seshan, Kidney disease in patients with obesity: It is not always obesity-related glomerulopathy alone. Obes. Res Clin. Pract. 11(5), 597–606 (2017)
A. Jauregui, D.H. Mintz, P. Mundel, A. Fornoni, Role of altered insulin signaling pathways in the pathogenesis of podocyte malfunction and microalbuminuria. Curr. Opin. Nephrol. Hypertens. 18(6), 539–545 (2009)
I.H. de Boer, S.D. Sibley, B. Kestenbaum et al. Central obesity, incident microalbuminuria, and change in creatinine clearance in the epidemiology of diabetes interventions and complications study. J. Am. Soc. Nephrol. 18(1), 235–243 (2007)
W.B. Eijkelkamp, Z. Zhang, G. Remuzzi et al. Albuminuria is a target for renoprotective therapy independent from blood pressure in patients with type 2 diabetic nephropathy: post hoc analysis from the Reduction of Endpoints in NIDDM with the Angiotensin II Antagonist Losartan (RENAAL) trial. J. Am. Soc. Nephrol. 18(5), 1540–1546 (2007)
K. Iseki, Y. Ikemiya, K. Kinjo, T. Inoue, C. Iseki, S. Takishita, Body mass index and the risk of development of end-stage renal disease in a screened cohort. Kidney Int. 65(5), 1870–1876 (2004)
C.Y. Hsu, C.E. McCulloch, C. Iribarren, J. Darbinian, A.S. Go, Body mass index and risk for end-stage renal disease. Ann. Intern. Med. 144(1), 21–28 (2006)
A.V. Mathew, S. Okada, K. Sharma, Obesity related kidney disease. Curr. Diabetes Rev. 7(1), 41–49 (2011)
N. Kambham, G.S. Markowitz, A.M. Valeri, J. Lin, V.D. D’Agati, Obesity-related glomerulopathy: an emerging epidemic. Kidney Int. 59(4), 1498–1509 (2001)
P.K. Chandie Shaw, S.P. Berger, M. Mallat, M. Frölich, F.W. Dekker, T.J. Rabelink, Central obesity is an independent risk factor for albuminuria in nondiabetic South Asian subjects. Diabetes Care 30(7), 1840–1844 (2007)
A. Chang, B.C. Batch, H.L. McGuire, W.M. Vollmer, L.P. Svetkey, C.C. Tyson et al. Association of a reduction in central obesity and phosphorus intake with changes in urinary albumin excretion: the PREMIER study. Am. J. Kidney Dis. 62(5), 900–907 (2013)
M. Haneda, K. Utsunomiya, D. Koya, T. Babazono, T. Moriya, H. Makino et al. A new classification of Diabetic Nephropathy 2014: a report from Joint Committee on Diabetic Nephropathy. J. Diabetes Investig. 6(2), 242–246 (2015)
H. Ninomiya, N. Katakami, T.A. Matsuoka, M. Takahara, H. Nishizawa, N. Maeda et al. Association between poor psychosocial conditions and diabetic nephropathy in Japanese type 2 diabetes patients: A cross-sectional study. J. Diabetes Investig. 9(1), 162–172 (2018)
N. Kurinami, S. Sugiyama, H. Nishimura, A. Morita, A. Yoshida et al. Clinical factors associated with initial decrease in body-fat percentage induced by add-on sodium-glucose co-transporter 2 inhibitors in patients with type 2 diabetes mellitus. Clin. Drug Invest. 38, 19–27 (2018)
N. Kurinami, S. Sugiyama, A. Yoshida, K. Hieshima, F. Miyamoto et al. Dapagliflozin significantly reduced liver fat accumulation associated with a decrease in abdominal subcutaneous fat in patients with inadequately controlled type 2 diabetes mellitus. Diabetes Res. Clin. Pract. 142, 254–263 (2018)
K. Cha, G.M. Chertow, J. Gonzalez, J.M. Lazarus, D.W. Wilmore, Multifrequency bioelectrical impedance estimates the distribution of body water. J. Appl. Physiol. 79, 1316–1319 (1995)
K. Cha, S. Shin, C. Shon, S. Choi, D.W. Wilmore, Evaluation of segmental bioelectrical impedance analysis (SIBA) for measuring muscle distribution. J. ICHPER SD-ASIA. 11–14 (1997)
H. Yokoyama, K. Kawai, M. Kobayashi, Japan Diabetes Clinical Data Management Study Group., Microalbuminuria is common in Japanese type 2 diabetic patients: a nationwide survey from the Japan Diabetes Clinical Data Management Study Group (JDDM 10). Diabetes Care 30(4), 989–992 (2007)
K. Iseki, Y. Ikemiya, C. Iseki, S. Takishita, Proteinuria and the risk of developing end-stage renal disease. Kidney Int. 63(4), 1468–1474 (2003)
S. Sugiyama, H. Jinnouchi, A. Yoshida, K. Hieshima, N. Kurinami, K. Jinnouchi et al. Renoprotective effects of additional SGLT2 inhibitor therapy in patients with type 2 diabetes mellitus and chronic kidney disease stages 3b-4: a real world report from a Japanese specialized diabetes care center. J. Clin. Med. Res. 11(4), 267–274 (2019)
S.P. Marso, G.H. Daniels, K. Brown-Frandsen, P. Kristensen, J.F. Mann, M.A. Nauck et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N. Engl. J. Med. 375(4), 311–322 (2016)
E.C. Hagen, C.A. Stegeman, J. D’Amaro, G.M. Schreuder, S.P. Lems, J.W. Tervaert et al. Decreased frequency of HLA-DR13DR6 in Wegener’s granulomatosis. Kidney Int. 48(3), 801–805 (1995)
T. Moriya, Y. Suzuki, S. Inomata, M. Iwano, M. Kanauchi, M. Haneda, Renal histological heterogeneity and functional progress in normoalbuminuric and microalbuminuric Japanese patients with type 2 diabetes. BMJ Open Diabetes Res. Care 2(1), e000029 (2014)
V.D. D’Agati, A. Chagnac, A.P. de Vries, M. Levi, E. Porrini, M. Herman-Edelstein, M. Praga, Obesity-related glomerulopathy: clinical and pathologic characteristics and pathogenesis. Nat. Rev. Nephrol. 12(8), 453–471 (2016)
Acknowledgements
We thank Susan Furness, PhD, from Edanz Group (https://en-author-services.edanzgroup.com/) for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
HJ has received honoraria from Novo Nordisk, Sanofi, AstraZeneca Pharmaceuticals, Astellas Pharma, Boehringer Ingelheim, Daiichi-Sankyo, Eli Lilly, Takeda, and Novartis Pharmaceuticals. SS has received honoraria from MSD, AstraZeneca Pharmaceuticals, Ono Pharmaceutical, Bayer Yakuhin, Ltd., and Novo Nordisk. There are no other potential conflicts of interest relevant to this article.
Ethics approval
The article does not contain any studies with animals performed by any of the authors. The study was conducted in accordance with the Declaration of Helsinki and the study protocol was approved by the Human Ethics Review Committee of Jinnouchi Hospital.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kurinami, N., Sugiyama, S., Ijima, H. et al. Characteristics of nephropathy in severely obese Japanese patients complicated with type 2 diabetes mellitus: a cross-sectional cohort study. Endocrine 70, 509–516 (2020). https://doi.org/10.1007/s12020-020-02462-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02462-7