Abstract
Purpose
The study aimed to disclose mortality pattern and quantitatively evaluate risks for cause-specific mortality among thyroid cancer survivors.
Methods
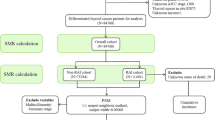
We included 173,710 patients from the Surveillance, Epidemiology, and End Results (SEER) database with thyroid cancer diagnosed between 1975 and 2015. Standardized mortality ratio (SMR) was calculated using general US population as the reference. Cumulative incidence function curves were constructed to elaborate crude cause-specific mortality by histology. Cox proportional hazards regression model was adopted to identify predictors for cause-specific mortality, expressed as hazard ratio (HR) and 95% confidence interval (CI).
Results
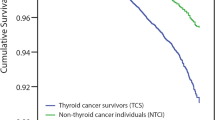
After a median follow-up of 101 months, 23,040 (13.3%) deaths occurred, of which 29.1% and 21.7% were attributable to thyroid cancer and cardiovascular disease (CVD), respectively. CVD SMRs were 1.14, 1.47, 1.21, and 5.66 in patients with follicular, Hürthle cell, medullary and anaplastic histology, respectively. The adjusted HRs of thyroid cancer-specific mortality were 1.59 (95% CI: 1.46–1.74), 1.87 (95% CI: 1.65–2.12), 3.66 (95% CI: 3.31–4.05), and 12.65 (95% CI: 11.50–13.92) for follicular, Hürthle cell, medullary, and anaplastic histology, respectively, as compared with papillary histology; HRs of CVD-specific mortality were 1.23 (95% CI: 1.12–1.34), 1.27 (95% CI: 1.11–1.46), 1.13 (95% CI: 0.96–1.33), and 1.60 (95% CI: 1.19–2.16), respectively. Older age, male sex, nonwhite race, unmarried status, and advanced stage were independent predictors of CVD-specific mortality, while receiving surgery and radiotherapy were protective against CVD-specific mortality.
Conclusions
We disclosed distinct mortality patterns by histology and identified predictors of CVD-specific mortality in thyroid cancer survivors, supporting CVD intervention for aggressive thyroid cancer.


Similar content being viewed by others
Data availability
The data that support the findings of this study are openly available in the Surveillance, Epidemiology, and End Results Program at https://seer.cancer.gov.
References
R.L. Siegel, K.D. Miller, A. Jemal, Cancer statistics, 2020. CA Cancer J. Clin. 70(1), 7–30 (2020). https://doi.org/10.3322/caac.21590
H. Lim, S.S. Devesa, J.A. Sosa, D. Check, C.M. Kitahara, Trends in thyroid cancer incidence and mortality in the United States, 1974-2013. JAMA 317(13), 1338–1348 (2017). https://doi.org/10.1001/jama.2017.2719
L.G. Morris, R.M. Tuttle, L. Davies, Changing trends in the incidence of thyroid cancer in the United States. JAMA Otolaryngol Head Neck Surg 142(7), 709–711 (2016). https://doi.org/10.1001/jamaoto.2016.0230
U.S. Cancer Statistics Working Group. U.S. Cancer Statistics Data Visualizations Tool, based on November 2018 submission data (1999-2016): U.S. Department of Health and Human Services (Centers for Disease Control and Prevention and National Cancer Institute, 2019). www.cdc.gov/cancer/dataviz
B.E. Blackburn, P.A. Ganz, K. Rowe, J. Snyder, Y. Wan, V. Deshmukh, M. Newman, A. Fraser, K. Smith, K. Herget, J. Kim, A.C. Kirchhoff, C. Porucznik, H. Hanson, M. Monroe, M. Hashibe, Aging-related disease risks among young thyroid cancer survivors. Cancer Epidemiol. Biomark. Prev. 26(12), 1695–1704 (2017). https://doi.org/10.1158/1055-9965.EPI-17-0623
E.N. Klein Hesselink, M.S. Klein Hesselink, G.H. de Bock, R.T. Gansevoort, S.J. Bakker, E.J. Vredeveld, A.N. van der Horst-Schrivers, I.C. van der Horst, P.W. Kamphuisen, J.T. Plukker, T.P. Links, J.D. Lefrandt, Long-term cardiovascular mortality in patients with differentiated thyroid carcinoma: an observational study. J. Clin. Oncol. 31(32), 4046–4053 (2013). https://doi.org/10.1200/JCO.2013.49.1043
J. Park, B.E. Blackburn, P.A. Ganz, K. Rowe, J. Snyder, Y. Wan, V. Deshmukh, M. Newman, A. Fraser, K. Smith, K. Herget, A.C. Kirchhoff, D. Abraham, J. Kim, M. Monroe, M. Hashibe, Risk factors for cardiovascular disease among thyroid cancer survivors: findings from the Utah Cancer Survivors Study. J. Clin. Endocrinol. Metab. 103(7), 2468–2477 (2018). https://doi.org/10.1210/jc.2017-02629
G. Mercuro, M.G. Panzuto, A. Bina, M. Leo, R. Cabula, L. Petrini, F. Pigliaru, S. Mariotti, Cardiac function, physical exercise capacity, and quality of life during long-term thyrotropin-suppressive therapy with levothyroxine: effect of individual dose tailoring. J. Clin. Endocrinol. Metab. 85(1), 159–164 (2000). https://doi.org/10.1210/jcem.85.1.6298
R.W. Flynn, S.R. Bonellie, R.T. Jung, T.M. MacDonald, A.D. Morris, G.P. Leese, Serum thyroid-stimulating hormone concentration and morbidity from cardiovascular disease and fractures in patients on long-term thyroxine therapy. J. Clin. Endocrinol. Metab. 95(1), 186–193 (2010). https://doi.org/10.1210/jc.2009-1625
H.S. Park, S. Lloyd, R.H. Decker, L.D. Wilson, J.B. Yu, Overview of the surveillance, epidemiology, and end results database: evolution, data variables, and quality assurance. Curr. Probl. Cancer 36(4), 183–190 (2012). https://doi.org/10.1016/j.currproblcancer.2012.03.007
Surveillance, Epidemiology, and End Results (SEER) Program (www.seer.cancer.gov). SEER*Stat Database: Incidence. SEER 18 Regs Research Data, Nov 2018 Sub (1975-2016 varying) “Katrina/Rita Population Adjustment”—Linked To County Attributes—Total U.S., 1969-2017 Counties, National Cancer Institute, DCCPS, Surveillance Research Program, based on the November 2018 submission (2019)
A.R. Shaha, TNM classification of thyroid carcinoma. World J. Surg. 31(5), 879–887 (2007). https://doi.org/10.1007/s00268-006-0864-0
Surveillance, Epidemiology, and End Results (SEER) Program (www.seer.cancer.gov). SEER*Stat Database: Mortality. All COD, Aggregated With State, Total U.S. (1969-2017) “Katrina/Rita Population Adjustment”, National Cancer Institute, DCCPS, Surveillance Research Program. Underlying mortality data provided by NCHS (2019). www.cdc.gov/nchs
K.J. Rothman, S. Greenland, T.L. Lash. Modern Epidemiology, 3rd edn. (Lippincott Williams & WIlkins, Philadelphia, PA, 2008)
L. Davies, H.G. Welch, Current thyroid cancer trends in the United States. JAMA Otolaryngol. Head Neck Surg. 140(4), 317–322 (2014). https://doi.org/10.1001/jamaoto.2014.1
B. Xu, R. Ghossein, Evolution of the histologic classification of thyroid neoplasms and its impact on clinical management. Eur. J. Surg. Oncol. 44(3), 338–347 (2018). https://doi.org/10.1016/j.ejso.2017.05.002
T. Ibrahimpasic, R. Ghossein, J.P. Shah, I. Ganly, Poorly differentiated carcinoma of the thyroid gland: current status and future prospects. Thyroid 29(3), 311–321 (2019). https://doi.org/10.1089/thy.2018.0509
R.C. Smallridge, J.A. Copland, Anaplastic thyroid carcinoma: pathogenesis and emerging therapies. Clin. Oncol. (R. Coll. Radiol.) 22(6), 486–497 (2010). https://doi.org/10.1016/j.clon.2010.03.013
G. Grani, L. Lamartina, C. Durante, S. Filetti, D.S. Cooper, Follicular thyroid cancer and Hurthle cell carcinoma: challenges in diagnosis, treatment, and clinical management. Lancet Diabetes Endocrinol. 6(6), 500–514 (2018). https://doi.org/10.1016/S2213-8587(17)30325-X
H. Joensuu, P.J. Klemi, R. Paul, J. Tuominen, Survival and prognostic factors in thyroid carcinoma. Acta Radiol. Oncol. 25(4-6), 243–248 (1986). https://doi.org/10.3109/02841868609136413
R. Sciuto, L. Romano, S. Rea, F. Marandino, I. Sperduti, C.L. Maini, Natural history and clinical outcome of differentiated thyroid carcinoma: a retrospective analysis of 1503 patients treated at a single institution. Ann. Oncol. 20(10), 1728–1735 (2009). https://doi.org/10.1093/annonc/mdp050
S.M. Chow, S.C. Law, S.K. Au, T.W. Leung, P.T. Chan, W.M. Mendenhall, W.H. Lau, Differentiated thyroid carcinoma: comparison between papillary and follicular carcinoma in a single institute. Head Neck 24(7), 670–677 (2002). https://doi.org/10.1002/hed.10080
E.M. Aboelnaga, R.A. Ahmed, Difference between papillary and follicular thyroid carcinoma outcomes: an experience from Egyptian institution. Cancer Biol. Med. 12(1), 53–59 (2015). https://doi.org/10.7497/j.issn.2095-3941.2015.0005
A.P. Kiess, N. Agrawal, J.D. Brierley, U. Duvvuri, R.L. Ferris, E. Genden, R.J. Wong, R.M. Tuttle, N.Y. Lee, G.W. Randolph, External-beam radiotherapy for differentiated thyroid cancer locoregional control: a statement of the American Head and Neck Society. Head Neck 38(4), 493–498 (2016). https://doi.org/10.1002/hed.24357
E. Ruel, S. Thomas, M. Dinan, J.M. Perkins, S.A. Roman, J.A. Sosa, Adjuvant radioactive iodine therapy is associated with improved survival for patients with intermediate-risk papillary thyroid cancer. J. Clin. Endocrinol. Metab. 100(4), 1529–1536 (2015). https://doi.org/10.1210/jc.2014-4332
Y. Sun, J. Gong, B. Guo, J. Shang, Y. Cheng, H. Xu, Association of adjuvant radioactive iodine therapy with survival in node-positive papillary thyroid cancer. Oral Oncol. 87, 152–157 (2018). https://doi.org/10.1016/j.oraloncology.2018.10.041
T.J. Pugh, A. Ballonoff, K.E. Rusthoven, R. McCammon, B. Kavanagh, F. Newman, R. Rabinovitch, Cardiac mortality in patients with stage I and II diffuse large B-cell lymphoma treated with and without radiation: a surveillance, epidemiology, and end-results analysis. Int. J. Radiat. Oncol. Biol. Phys. 76(3), 845–849 (2010). https://doi.org/10.1016/j.ijrobp.2009.02.045
H. Abuamsha, A.N. Kadri, A.V. Hernandez, Cardiovascular mortality among patients with non-Hodgkin lymphoma: differences according to lymphoma subtype. Hematol. Oncol. 37(3), 261–269 (2019). https://doi.org/10.1002/hon.2607
J. Weberpals, L. Jansen, O.J. Muller, H. Brenner, Long-term heart-specific mortality among 347 476 breast cancer patients treated with radiotherapy or chemotherapy: a registry-based cohort study. Eur. Heart J. 39(43), 3896–3903 (2018). https://doi.org/10.1093/eurheartj/ehy167
J.L. la Cour, U.B. Andersen, C.H. Sorensen, B. Nygaard, L.T. Jensen, Radioiodine therapy does not change the atherosclerotic burden of the carotid arteries. Thyroid 26(7), 965–971 (2016). https://doi.org/10.1089/thy.2015.0538
I. Klein, S. Danzi, Thyroid disease and the heart. Circulation 116(15), 1725–1735 (2007). https://doi.org/10.1161/CIRCULATIONAHA.106.678326
E. Ryodi, S. Metso, H. Huhtala, M. Valimaki, A. Auvinen, P. Jaatinen, Cardiovascular morbidity and mortality after treatment of hyperthyroidism with either radioactive iodine or thyroidectomy. Thyroid 28(9), 1111–1120 (2018). https://doi.org/10.1089/thy.2017.0461
C.E. Palme, Z. Waseem, S.N. Raza, S. Eski, P. Walfish, J.L. Freeman, Management and outcome of recurrent well-differentiated thyroid carcinoma. Arch. Otolaryngol. Head Neck Surg. 130(7), 819–824 (2004). https://doi.org/10.1001/archotol.130.7.819
S. Naing, B.J. Collins, A.B. Schneider, Clinical behavior of radiation-induced thyroid cancer: factors related to recurrence. Thyroid 19(5), 479–485 (2009). https://doi.org/10.1089/thy.2008.0343
E. Ron, J.H. Lubin, R.E. Shore, K. Mabuchi, B. Modan, L.M. Pottern, A.B. Schneider, M.A. Tucker, J.D. Boice Jr, Thyroid cancer after exposure to external radiation: a pooled analysis of seven studies. Radiat. Res. 141(3), 259–277 (1995)
R.C. Smallridge, K.B. Ain, S.L. Asa, K.C. Bible, J.D. Brierley, K.D. Burman, E. Kebebew, N.Y. Lee, Y.E. Nikiforov, M.S. Rosenthal, M.H. Shah, A.R. Shaha, R.M. Tuttle,American Thyroid Association Anaplastic Thyroid Cancer Guidelines Taskforce, American Thyroid Association guidelines for management of patients with anaplastic thyroid cancer. Thyroid 22(11), 1104–1139 (2012). https://doi.org/10.1089/thy.2012.0302
L. Davies, H.G. Welch, Increasing incidence of thyroid cancer in the United States, 1973-2002. JAMA 295(18), 2164–2167 (2006). https://doi.org/10.1001/jama.295.18.2164
F.C. Pampel, P.M. Krueger, J.T. Denney, Socioeconomic disparities in health behaviors. Annu. Rev. Sociol. 36, 349–370 (2010). https://doi.org/10.1146/annurev.soc.012809.102529
W.M. Schultz, H.M. Kelli, J.C. Lisko, T. Varghese, J. Shen, P. Sandesara, A.A. Quyyumi, H.A. Taylor, M. Gulati, J.G. Harold, J.H. Mieres, K.C. Ferdinand, G.A. Mensah, L.S. Sperling, Socioeconomic status and cardiovascular outcomes: challenges and interventions. Circulation 137(20), 2166–2178 (2018). https://doi.org/10.1161/CIRCULATIONAHA.117.029652
N. Li, X.L. Du, L.R. Reitzel, L. Xu, E.M. Sturgis, Impact of enhanced detection on the increase in thyroid cancer incidence in the United States: review of incidence trends by socioeconomic status within the surveillance, epidemiology, and end results registry, 1980-2008. Thyroid 23(1), 103–110 (2013). https://doi.org/10.1089/thy.2012.0392
R. Manfredini, A. De Giorgi, R. Tiseo, B. Boari, R. Cappadona, R. Salmi, M. Gallerani, F. Signani, F. Manfredini, D.P. Mikhailidis, F. Fabbian, Marital status, cardiovascular diseases, and cardiovascular risk factors: a review of the evidence. J. Womens Health 26(6), 624–632 (2017). https://doi.org/10.1089/jwh.2016.6103
A.A. Aizer, M.H. Chen, E.P. McCarthy, M.L. Mendu, S. Koo, T.J. Wilhite, P.L. Graham, T.K. Choueiri, K.E. Hoffman, N.E. Martin, J.C. Hu, P.L. Nguyen, Marital status and survival in patients with cancer. J. Clin. Oncol. 31(31), 3869–3876 (2013). https://doi.org/10.1200/JCO.2013.49.6489
B.R. Haugen, E.K. Alexander, K.C. Bible, G.M. Doherty, S.J. Mandel, Y.E. Nikiforov, F. Pacini, G.W. Randolph, A.M. Sawka, M. Schlumberger, K.G. Schuff, S.I. Sherman, J.A. Sosa, D.L. Steward, R.M. Tuttle, L. Wartofsky, 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the american thyroid association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 26(1), 1–133 (2016). https://doi.org/10.1089/thy.2015.0020
B. Biondi, D.S. Cooper, Benefits of thyrotropin suppression versus the risks of adverse effects in differentiated thyroid cancer. Thyroid 20(2), 135–146 (2010). https://doi.org/10.1089/thy.2009.0311
T.Y. Goraya, S.J. Jacobsen, P.G. Belau, S.A. Weston, T.E. Kottke, V.L. Roger, Validation of death certificate diagnosis of out-of-hospital coronary heart disease deaths in Olmsted County, Minnesota. Mayo Clin. Proc. 75(7), 681–687 (2000). https://doi.org/10.4065/75.7.681
C.M. Kitahara, R.M. Pfeiffer, J.A. Sosa, M.S. Shiels, Impact of overweight and obesity on U.S. papillary thyroid cancer incidence trends (1995-2015). J. Natl. Cancer Inst. (2019). https://doi.org/10.1093/jnci/djz202
Y.K. Lee, N. Hong, S.H. Park, D.Y. Shin, C.R. Lee, S.W. Kang, J. Lee, J.J. Jeong, K.H. Nam, W.Y. Chung, E.J. Lee, The relationship of comorbidities to mortality and cause of death in patients with differentiated thyroid carcinoma. Sci Rep. 9(1), 11435 (2019). https://doi.org/10.1038/s41598-019-47898-8
Funding
This study was funded by the Henan Province Health Planning Technology Talents Overseas Research Project (formerly 5451 Project, Grant no. HWYX2019045).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was considered exempt from local ethics committee approval because all data are de-identified for public use.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Du, B., Wang, F., Wu, L. et al. Cause-specific mortality after diagnosis of thyroid cancer: a large population-based study. Endocrine 72, 179–189 (2021). https://doi.org/10.1007/s12020-020-02445-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02445-8