Abstract
Background
Except conventional treatments, research on medical approach for radioiodine-refractory differentiated thyroid cancer (RR-DTC) was considered particularly challenging. Sorafenib, a novel biological agent, has been widely studied in the treatment of RR-DTC for years. We performed a systematic review and meta-analysis to explore the efficiency and safety of treating RR-DTC patients with sorafenib.
Methods
An electronic search on PubMed/Medline and Embase was carried out to search associated articles. Fixed-effects or random-effects models were chose according to the heterogeneity.
Results
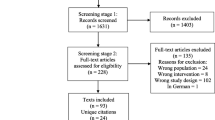
A total of 15 eligible studies (636 patients) were included. As shown by the only randomised clinical trial-DECISION, sorafenib significantly improved progression-free survival (PFS) compared with placebo in patients with progressive RR-DTC. The pooled analysis indicated that there were 26% patients (95% CI: 0.19–0.34) achieved partial response (PR), and 44% patients (98% CI: 0.39–0.48) achieved stable disease (SD). The most frequent adverse effects (AEs) observed included hand-foot syndrome (HFS), diarrhoea, fatigue, alopecia, weight loss (WS) and rash, the incidence of all grades AEs for which were 71%, 60%, 59%, 55%, 51% and 50%, respectively. There were 68% patients (252/368), who had a dose reduction because of the drug toxicities and AEs.
Conclusions
Sorafenib could improve PFS in patients with progressive RR-DTC, comparing with placebo. Due to the resistance to conventional treatments, sorafenib is considered as a promising treatment for RR-DTC by most physicians specialised in this field. However, the use of sorafenib should be cautious due to a high incidence of AEs caused by the agent. More effective agents with less toxicities are warranted.



Similar content being viewed by others
References
C. Eheman, S.J. Henley, R. Ballard-Barbash, E.J. Jacobs, M.J. Schymura, A.M. Noone, L. Pan, R.N. Anderson, J.E. Fulton, B.A. Kohler, A. Jemal, E. Ward, M. Plescia, L.A. Ries, B.K. Edwards, Annual Report to the Nation on the status of cancer, 1975–2008, featuring cancers associated with excess weight and lack of sufficient physical activity. Cancer 118(9), 2338–2366 (2012). https://doi.org/10.1002/cncr.27514
B.R. Haugen, 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: What is new and what has changed? Cancer 123(3), 372–381 (2017). https://doi.org/10.1002/cncr.30360
R. Dadu, M.E. Cabanillas, Optimizing therapy for radioactive iodine-refractory differentiated thyroid cancer: current state of the art and future directions. Minerva Endocrinol. 37(4), 335–356 (2012)
C. Durante, N. Haddy, E. Baudin, S. Leboulleux, D. Hartl, J.P. Travagli, B. Caillou, M. Ricard, J.D. Lumbroso, F. De Vathaire, M. Schlumberger, Long-term outcome of 444 patients with distant metastases from papillary and follicular thyroid carcinoma: benefits and limits of radioiodine therapy. J. Clin. Endocrinol. Metab. 91(8), 2892–2899 (2006). https://doi.org/10.1210/jc.2005-2838
M. Schlumberger, M. Brose, R. Elisei, S. Leboulleux, M. Luster, F. Pitoia, F. Pacini, Definition and management of radioactive iodine-refractory differentiated thyroid cancer. Lancet Diabetes Endocrinol. 2(5), 356–358 (2014). https://doi.org/10.1016/S2213-8587(13)70215-8
B.R. Haugen, E.K. Alexander, K.C. Bible, G.M. Doherty, S.J. Mandel, Y.E. Nikiforov, F. Pacini, G.W. Randolph, A.M. Sawka, M. Schlumberger, K.G. Schuff, S.I. Sherman, J.A. Sosa, D.L. Steward, R.M. Tuttle, L. Wartofsky, 2015 American Thyroid Association Management Guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: The American Thyroid Association Guidelines Task Force on thyroid nodules and differentiated thyroid cancer. Thyroid. 26(1), 1–133 (2016). https://doi.org/10.1089/thy.2015.0020
F. Albarel, B. Conte-Devolx, C. Oliver, From nodule to differentiated thyroid carcinoma: contributions of molecular analysis in 2012. Ann. Endocrinol. 73(3), 155–164 (2012). https://doi.org/10.1016/j.ando.2012.03.002
S. Wilhelm, C. Carter, M. Lynch, T. Lowinger, J. Dumas, R.A. Smith, B. Schwartz, R. Simantov, S. Kelley, Discovery and development of sorafenib: a multikinase inhibitor for treating cancer. Nat. Rev. Drug Discov. 5(10), 835–844 (2006). https://doi.org/10.1038/nrd2130
M.S. Brose, C.M. Nutting, B. Jarzab, R. Elisei, S. Siena, L. Bastholt, C. de la Fouchardiere, F. Pacini, R. Paschke, Y.K. Shong, S.I. Sherman, J.W. Smit, J. Chung, C. Kappeler, C. Pena, I. Molnar, M.J. Schlumberger, Sorafenib in radioactive iodine-refractory, locally advanced or metastatic differentiated thyroid cancer: a randomised, double-blind, phase 3 trial. Lancet. 384(9940), 319–328 (2014). https://doi.org/10.1016/s0140-6736(14)60421-9
V. Gupta-Abramson, A.B. Troxel, A. Nellore, K. Puttaswamy, M. Redlinger, K. Ransone, S.J. Mandel, K.T. Flaherty, L.A. Loevner, P.J. O’Dwyer, M.S. Brose, Phase II trial of sorafenib in advanced thyroid cancer. J. Clin. Onco.l 26(29), 4714–4719 (2008). https://doi.org/10.1200/jco.2008.16.3279
D. Moher, A. Liberati, J. Tetzlaff, D.G. Altman, P. Group, Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J. Clin. Epidemiol. 62(10), 1006–1012 (2009). https://doi.org/10.1016/j.jclinepi.2009.06.005
J.P. Higgins, S.G. Thompson, Quantifying heterogeneity in a meta-analysis. Stat. Med. 21(11), 1539–1558 (2002). https://doi.org/10.1002/sim.1186
C.B. Begg, M. Mazumdar, Operating characteristics of a rank correlation test for publication bias. Biometrics. 50(4), 1088–1101 (1994)
M. Ahmed, Y. Barbachano, A. Riddell, J. Hickey, K.L. Newbold, A. Viros, K.J. Harrington, R. Marais, C.M. Nutting, Analysis of the efficacy and toxicity of sorafenib in thyroid cancer: a phase II study in a UK based population. Eur. J. Endocrinol. 165(2), 315–322 (2011). https://doi.org/10.1530/eje-11-0129
M. Benekli, S. Yalcin, M. Ozkan, E.T. Elkiran, A. Sevinc, D. Cabuk, H.S. Coskun, B. Oksuzoglu, B. Bayar, A. Akbulat, A. Ozet, Efficacy of sorafenib in advanced differentiated and medullary thyroid cancer: experience in a Turkish population. OncoTargets Ther. 8, 1–5 (2015). https://doi.org/10.2147/ott.S70670
J. Capdevila, L. Iglesias, I. Halperin, A. Segura, J. Martinez-Trufero, M.A. Vaz, J. Corral, G. Obiols, E. Grande, J.J. Grau, J. Tabernero, Sorafenib in metastatic thyroid cancer. Endoc. Relat. Cancer 19(2), 209–216 (2012). https://doi.org/10.1530/erc-11-0351
L. Chen, Y. Shen, Q. Luo, Y. Yu, H. Lu, R. Zhu, Response to sorafenib at a low dose in patients with radioiodine-refractory pulmonary metastases from papillary thyroid carcinoma. Thyroid. 21(2), 119–124 (2011). https://doi.org/10.1089/thy.2010.0199
R. Dadu, S.G. Waguespack, S.I. Sherman, M.I. Hu, N.L. Busaidy, C. Jimenez, M.A. Habra, A.K. Ying, R.L. Bassett, M.E. Cabanillas, Efficacy and tolerability of different starting doses of sorafenib in patients with differentiated thyroid cancer. Oncologist 19(5), 477–482 (2014). https://doi.org/10.1634/theoncologist.2013-0409
M. Gallo, F. Michelon, A. Castiglione, F. Felicetti, A.A. Viansone, A. Nervo, C. Zichi, G. Ciccone, A. Piovesan, E. Arvat, Sorafenib treatment of radioiodine-refractory advanced thyroid cancer in daily clinical practice: a cohort study from a single center. Endocrine 49(3), 726–734 (2015). https://doi.org/10.1007/s12020-014-0481-x
H. Hoftijzer, K.A. Heemstra, H. Morreau, M.P. Stokkel, E.P. Corssmit, H. Gelderblom, K. Weijers, A.M. Pereira, M. Huijberts, E. Kapiteijn, J.A. Romijn, J.W. Smit, Beneficial effects of sorafenib on tumor progression, but not on radioiodine uptake, in patients with differentiated thyroid carcinoma. Eur. J. Endocrinol. 161(6), 923–931 (2009). https://doi.org/10.1530/eje-09-0702
M. Kim, T.H. Kim, D.Y. Shin, D.J. Lim, E.Y. Kim, W.B. Kim, J.H. Chung, Y.K. Shong, B.H. Kim, W.G. Kim, Tertiary care experience of sorafenib in the treatment of progressive radioiodine-refractory differentiated thyroid carcinoma: a Korean Multicenter Study. Thyroid. 28(3), 340–348 (2018). https://doi.org/10.1089/thy.2017.0356
R.T. Kloos, M.D. Ringel, M.V. Knopp, N.C. Hall, M. King, R. Stevens, J. Liang, P.E. Wakely Jr., V.V. Vasko, M. Saji, J. Rittenberry, L. Wei, D. Arbogast, M. Collamore, J.J. Wright, M. Grever, M.H. Shah, Phase II trial of sorafenib in metastatic thyroid cancer. J. Clin. Oncol. 27(10), 1675–1684 (2009). https://doi.org/10.1200/jco.2008.18.2717
Y. Luo, Y. Shi, P. Xing, L. Wang, Y. Feng, X. Han, X. He, Sorafenib in metastatic radioactive iodine-refractory differentiated thyroid cancer: a pilot study. Mol. Clin. Oncol. 2(1), 87–92 (2014). https://doi.org/10.3892/mco.2013.199
V. Marotta, V. Ramundo, L. Camera, M. Del Prete, R. Fonti, R. Esposito, G. Palmieri, M. Salvatore, M. Vitale, A. Colao, A. Faggiano, Sorafenib in advanced iodine-refractory differentiated thyroid cancer: efficacy, safety and exploratory analysis of role of serum thyroglobulin and FDG-PET. Clin. Endocrinol. 78(5), 760–767 (2013). https://doi.org/10.1111/cen.12057
F. Pitoia, Response to sorafenib treatment in advanced metastatic thyroid cancer. Arq. Bras. Endocrinol. Metabol. 58(1), 37–41 (2014)
T.C. Schneider, R.M. Abdulrahman, E.P. Corssmit, H. Morreau, J.W. Smit, E. Kapiteijn, Long-term analysis of the efficacy and tolerability of sorafenib in advanced radio-iodine refractory differentiated thyroid carcinoma: final results of a phase II trial. Eur. J. Endocrinol. 167(5), 643–650 (2012). https://doi.org/10.1530/eje-12-0405
C.T. Shen, Z.L. Qiu, Q.Y. Luo, Sorafenib in the treatment of radioiodine-refractory differentiated thyroid cancer: a meta-analysis. Endocr. Relat. cancer 21(2), 253–261 (2014). https://doi.org/10.1530/erc-13-0438
R. Elisei, C. Ugolini, D. Viola, C. Lupi, A. Biagini, R. Giannini, C. Romei, P. Miccoli, A. Pinchera, F. Basolo, BRAF(V600E) mutation and outcome of patients with papillary thyroid carcinoma: a 15-year median follow-up study. J. Clin. Endocrinol. Metab. 93(10), 3943–3949 (2008). https://doi.org/10.1210/jc.2008-0607
A.L. Smith, M.D. Williams, J. Stewart, W.L. Wang, S. Krishnamurthy, M.E. Cabanillas, S. Roy-Chowdhuri, Utility of the BRAF p.V600E immunoperoxidase stain in FNA direct smears and cell block preparations from patients with thyroid carcinoma. Cancer Cytopathol. 126(6), 406–413 (2018). https://doi.org/10.1002/cncy.21992
M. Xing, Prognostic utility of BRAF mutation in papillary thyroid cancer. Mol. Cell. Endocrinol. 321(1), 86–93 (2010). https://doi.org/10.1016/j.mce.2009.10.012
M. Xing, B.R. Haugen, M. Schlumberger, Progress in molecular-based management of differentiated thyroid cancer. Lancet 381(9871), 1058–1069 (2013). https://doi.org/10.1016/S0140-6736(13)60109-9
C. Gouveia, N.T. Can, A. Bostrom, J.P. Grenert, A. van Zante, L.A. Orloff, Lack of association of BRAF mutation with negative prognostic indicators in papillary thyroid carcinoma: the University of California, San Francisco, experience. JAMA Otolaryngol. Head. Neck Surg. 139(11), 1164–1170 (2013). https://doi.org/10.1001/jamaoto.2013.4501
L.E. Henke, J.D. Pfeifer, C. Ma, S.M. Perkins, T. DeWees, S. El-Mofty, J.F. Moley, B. Nussenbaum, B.H. Haughey, T.J. Baranski, J.K. Schwarz, P.W. Grigsby, BRAF mutation is not predictive of long-term outcome in papillary thyroid carcinoma. Cancer Med. 4(6), 791–799 (2015). https://doi.org/10.1002/cam4.417
Author information
Authors and Affiliations
Contributions
J.Z. designed the research. G.F. searched and independently assessed the eligibility of all potential publications. G.F. and Q.Z. conducted data extraction according to the PRISMA statement. J.X. carried out the statistical analyses. G.F. wrote the manuscript, supervised by J.Z. All authors contributed to the revising the article, and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All the studies included in the meta-analysis were conducted in accordance with the ethical standards of the institutional and/or national research committee, and obtained written informed consent from all participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Feng, G., Luo, Y., Zhang, Q. et al. Sorafenib and radioiodine-refractory differentiated thyroid cancer (RR-DTC): a systematic review and meta-analysis. Endocrine 68, 56–63 (2020). https://doi.org/10.1007/s12020-019-02167-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-019-02167-6