Abstract
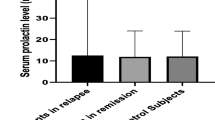
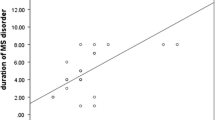
An association between prolactinemia with disability, clinical forms, and sex of patients with multiple sclerosis (MS) remains unclear. The aim of this study was to evaluate the association of prolactin with clinical forms and accumulating disability over time in patients with MS. A longitudinal study was carried out with 101 patients with relapsing–remitting MS (RRMS) and 19 with progressive forms of MS (ProgMS). The disability over time, as well as prolactin and ferritin serum levels were evaluated at baseline (T0), 8-month follow-up (T8), and 16-month follow-up. The disability at T0, T8, and T16 was higher among patients with ProgMS than those with RRMS. Prolactin and ferritin levels did not differ over time between both groups. Initially, prolactin was associated with MS disability. After introducing age and sex, the effects of prolactin on disability were no longer significant. Prolactin was associated with age and sex, whereby age was positively associated with disability. In the same way, after introducing age and sex, the effects of diagnosis on prolactin levels, as well as the association between prolactin and ferritin, were no longer significant (P = 0.563 and P = 0.599, respectively). Moreover, 21.6% of the variance in the disability was predicted by age (P < 0.001), and sex (P = 0.049), while prolactin was not significant. In conclusion, the effects of prolactin on the disability and clinical forms of MS patients may be spurious results because those correlations reflect the positive associations of age with the disability and the negative association of age with prolactin.
Similar content being viewed by others
References
Academia Brasileira De Neurologia. (2016). Recomendações no tratamento da Esclerose Múltipla e Neuromielite Óptica (2nd ed.). São Paulo: Omnifarma.
Alberti, K. G., Eckel, R. H., Grundy, S. M., et al. (2009). Harmonizing the metabolic syndrome: A joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation,120(16), 1640–1645.
Azar, S. T., & Yamout, B. (1999). Prolactin secretion is increased in patients with multiple sclerosis. Endocrine Research,25(2), 207–214. https://doi.org/10.1080/07435809909066142.
Borba, V. V., Zandman-Goddard, G., & Shoenfeld, Y. (2018). Prolactin and autoimmunity. Frontiers in Immunology,9, 1–8.
Borchers, A. T., Naguwa, S. M., Keen, C. L., & Gershwin, M. E. (2010). The implications of autoimmunity and pregnancy. Journal of Autoimmunity,34(3), 287–299. https://doi.org/10.1016/j.jaut.2009.11.015.
Correale, J., Farez, M. F., & Ysrraelit, M. C. (2014). Role of prolactin in B cell regulation in multiple sclerosis. Journal of Neuroimmunology,269(1–2), 76–86. https://doi.org/10.1016/j.jneuroim.2014.02.007.
Cottrell, D. A., Kremenchutzky, M., Rice, G. P., et al. (1999). The natural history of multiple sclerosis: A geographically based study. 5. The clinical features and natural history of primary progressive multiple sclerosis. Brain,122(Pt 4), 625–639.
Da Costa, R., Szyper-Kravitz, M., Szekanecz, Z., et al. (2011). Ferritin and prolactin levels in multiple sclerosis. Israel Medical Association Journal,13(2), 91–95.
De Giglio, L., Marinelli, F., Prosperini, L., et al. (2015). Relationship between prolactin plasma levels and white matter volume in women with multiple sclerosis. Mediators of Inflammation,2015, 732539. https://doi.org/10.1155/2015/732539.
Devi, Y. S., & Halperin, J. (2014). Reproductive actions of prolactin mediated through short and long receptor isoforms. Molecular and Cellular Endocrinology,382(1), 400–410. https://doi.org/10.1016/j.mce.2013.09.016.
Ferreira, K. P. Z., Oliveira, S. R., Kallaur, A. P., et al. (2017). Disease progression and oxidative stress are associated with higher serum ferritin levels in patients with multiple sclerosis. Journal of the Neurological Sciences,15(373), 236–241. https://doi.org/10.1016/j.jns.2016.12.039.
Gregg, C. (2009). Pregnancy, prolactin and white matter regeneration. J Neurological Sciences,285, 22–27.
Gregg, C., Shikar, V., Larsen, P., et al. (2007). White matter plasticity and enhanced remyelination in the maternal CNS. Journal of Neuroscience,21, 1812–1823.
Heesen, C., Gold, S. M., Bruhn, M., Mönch, A., & Schulz, K. H. (2002). Prolactin stimulation in multiple sclerosis—An indicator of disease subtypes and activity? Endocrine Research,28(1–2), 9–18.
Huitinga, I., Erkut, Z. A., Van Beurden, D., et al. (2004). Impaired hypothalamus-pituitary-adrenal axis activity and more severe multiple sclerosis with hypothalamic lesions. Annals of Neurology,55, 37–45.
James, P. A., Oparil, S., Carter, B. L., et al. (2014). Evidence-based guideline for the management of high blood pressure in adults: Report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA,311(5), 507–520.
Kira, J., Harada, M., Yamaguchi, Y., et al. (1991). Hyperprolactinemia in multiple sclerosis. Journal of the Neurological Sciences,102, 61–66.
Koch, M., Mostert, J., Arutjunyan, A. V., et al. (2007). Plasma lipid peroxidation and progression of disability in multiple sclerosis. European Journal of Neurology,14, 529–533.
Kurtzke, J. F. (1983). Rating neurologic impairment in multiple sclerosis: An expanded disability status scale (EDSS). Neurology,33, 1444–1452.
Langer-Gould, A., Huang, S. M., & Gupta, R. (2009). Exclusive breastfeeding and the risk of postpartum relapses in women with multiple sclerosis. Archives of Neurology,66, 958–963.
Lassmann, H., van Horssen, J., & Mahad, D. (2012). Progressive multiple sclerosis: Pathology and pathogenesis. Nature Reviews Neurology,8, 647–656.
Lennartsson, A. K., & Jonsdottir, I. H. (2011). Prolactin in response to acute psychosocial stress in healthy men and women. Psychoneuroendocrinology,36, 1530–1539.
Lublin, F. D., & Reingold, S. C. (1996). Defining the clinical course of multiple sclerosis: Results of an international survey. National Multiple Sclerosis Society (USA) Advisory Committee on Clinical Trials of New Agents in Multiple Sclerosis. Neurology,46, 907–911.
Lublin, F. D., Reingold, S. C., Cohen, J. A., Cutter, G. R., Sørensen, P. S., Thompson, A. J., et al. (2014). Defining the clinical course of multiple sclerosis: The 2013 revisions. Neurology,83(3), 278–286.
Mackern-Oberti, J. P., Jara, E. L., Riedel, C. A., & Kalergis, A. M. (2011). Hormonal modulation of dendritic cells differentiation, maturation and function: Implications for the initiation and progress of systemic autoimmunity. Archivum immunolgiae et therapiae experimentalis,65(2), 123–136. https://doi.org/10.1007/s00005-016-0418-6.
Majumdar, A., & Mangal, N. S. (2013). Hyperprolactinemia. Journal of Human Reproductive Sciences,6(3), 168–175. https://doi.org/10.4103/0974-1208.121400.
Mellai, M., Giordano, M., D’Alfonso, S., et al. (2003). Prolactin and prolactin receptor gene polymorphisms in multiple sclerosis and systemic lupus erythematosus. Human Immunology,64(2), 274–284. https://doi.org/10.1016/s0198-8859(02)00804-2.
Moshirzadeh, S., Ghareghozli, K., Harandi, A. A., & Pakdaman, H. (2012). Serum prolactin level in patients with relapsing-remitting multiple sclerosis during relapse. Journal of Clinical Neuroscience,19(4), 622–623. https://doi.org/10.1016/j.jocn.2011.07.032.
Orbach, H., Zandman-Goddard, G., Amital, H., Barak, V., Szekanecz, Z., Szucs, G., et al. (2007). Novel biomarkers in autoimmune diseases: Prolactin, ferritin, vitamin D, and TPA levels in autoimmune diseases. Annals of the New York Academy of Sciences,1109, 385–400.
Ortona, E., Pierdominici, M., Maselli, A., Veroni, C., Aloisi, F., & Shoenfeld, Y. (2016). Sex-based differences in autoimmune diseases. Annali dell Istituto Superiore di Sanita,52(2), 205–212. https://doi.org/10.4415/ann_16_02_12.
Peeva, E., & Zouali, M. (2005). Spotlight on the role of hormonal factors in the emergence of autoreactive B-lymphocytes. Immunology Letters,101(2), 123–143. https://doi.org/10.1016/j.imlet.2005.05.014.
Pereira Suarez, A. L., Lopez-Rincon, G., Martinez Neri, P. A., & Estrada-Chavez, C. (2015). Prolactin in inflammatory response. Advances in Experimental Medicine and Biology,846, 243–264. https://doi.org/10.1007/978-3-319-12114-7_11.
Polman, C. H., Reingold, S. C., Banwell, B., et al. (2011). Diagnostic criteria for multiple sclerosis: 2010 Revisions to the McDonald criteria. Annals of Neurology,69, 292–302. https://doi.org/10.1002/ana.22366.
Ringle, C. M., Wende, S., Becker, J.-M. SmartPLS 3. Bönningstedt: SmartPLS, 2015. Retrieved from http://www.smartpls.com.
Sinha, Y. (1995). Structural variants of prolactin: Occurrence and physiological significance. Endocrine Reviews,16, 354–369.
Sospedra, M., & Martin, R. (2016). Immunology of multiple sclerosis. Seminars in Neurology,36, 115–127.
Vera-Lastra, O., Jara, L. J., & Espinoza, L. R. (2002). Prolactin and autoimmunity. Autoimmunity Reviews,1(6), 360–364. https://doi.org/10.1016/S1568-9972(02)00081-2.
Vukusic, S., Hutchinson, M., & Hours, M. (2004). Pregnancy and multiple sclerosis (the PRIMS study): Clinical predictors of postpartum relapse. Brain,127, 1353–1360.
Yamasaki, K., Horiuchi, I., Minohara, M., et al. (2000). Hyperprolactinemia in optico-spinal multiple sclerosis. Internal Medicine,39, 296–299.
Zhornitsky, S., Yong, V. W., Weiss, S., & Metz, L. M. (2012). Prolactin in multiple sclerosis. Multiple Sclerosis Journal,19(1), 15–23. https://doi.org/10.1177/1352458512458555.
Funding
This study was partially supported by Novartis Biosciences S.A. for the development of the research according to the Researcher’s Initiative Study CFTY720DBR07T. The authors do not receive any reimbursement or financial benefits and declare that they have no competing interests. Novartis Biosciences S.A. played no role in the design, methods, data management or analysis or in the decision to publish. The study was also supported by grants from Coordination for the Improvement of Higher Level of Education Personnel (CAPES) of Brazilian Ministry of Education; Institutional Program for Scientific Initiation Scholarship (PIBIC) of the National Council for Scientific and Technological Development (CNPq).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
The protocol was approved by the Institutional Research Ethics Committees of University of Londrina, Paraná, Brazil (CAAE: 22290913.9.0000.5231) and all of the individuals invited were informed in detail about the research and gave written Informed Consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Carvalho Jennings Pereira, W.L., Flauzino, T., Alfieri, D.F. et al. Prolactin is Not Associated with Disability and Clinical Forms in Patients with Multiple Sclerosis. Neuromol Med 22, 73–80 (2020). https://doi.org/10.1007/s12017-019-08565-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12017-019-08565-3