Abstract
Autoimmune uveitis (AIU) is among the leading causes of preventable blindness. It can be isolated, precede, or appear in the course of a systemic autoimmune inflammatory disease. When suspected, AIU should be promptly referred to an ophthalmologist for proper anatomic classification and local treatment. In recurrent and chronic forms, systemic treatment should be started, usually with corticosteroids and immunesuppressors. In cases of lack of efficacy or intolerance, biologic agents such as monoclonal antibodies anti-TNF (infliximab and adalimumab) and others (abatacept and tocilizumab) are being used. The clinical diseases associated to AIU and the experimental models have helped in the understanding of the pathogenic mechanism. The treatment schemes have improved, and recent advances in basic knowledge are leading to even more effective targeted therapies.
Similar content being viewed by others
References
Gery I, Nussenblatt RB, Chan CC, Caspi RR (2002) Autoimmune diseases of the eye. In: Theofilopoulos AN, Bona CA (eds) The Molecular Pathology of Autoimmune Diseases. Taylor and Francis, New York, pp 978–998
Ali A, Samson CM (2007) Seronegative spondyloarthropathies and the eye. Curr Opin Ophthalmol 18(6):476–480
Grassi A, Corona F, Casellato A, Carnelli V, Bardare M (2007) Prevalence and outcome of juvenile idiopathic arthritis-associated uveitis and relation to articular disease. J Rheumatol 34(5):1139–1145
Damico FM, Kiss S, Young LH (2005) Vogt-Koyanagi-Harada disease. Semin Ophthalmol 20(3):183–190
Romanelli RG, La Villa G, Almerigogna F, Vizzutti F, Di Pietro E, Fedi V, Gentilini P, Laffi G (2006) Uveitis in autoimmune hepatitis: a case report. World J Gastroenterol 12(10):1637–1640
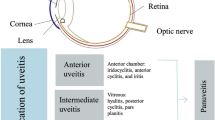
Khairallah M (2010) Are the Standardization of the Uveitis Nomenclature (SUN) Working Group criteria for Codifying the Site of Inflammation Appropriate for All Uveitis Problems? Limitations of the SUN Working Group Classification. Ocul Immunol Inflamm 18(1):2–4, Serial online
Jabs DA, Nussenblatt RB, Rosenbaum JT, Standardization of Uveitis Nomenclature (SUN) Working Group (2005) Standardization of uveitis nomenclature for reporting clinical data. Results of the First International Workshop. Am J Ophthalmol 140(3):509–516
Srivastava A, Rajappa M, Kaur J (2010) Uveitis: Mechanisms and recent advances in therapy. Clin Chim Acta 411:1165–1171
Banares A, Hernández-García C, Fernández-Gutiérrez B, Jover JA (1998) Eye involvement in the spondyloarthropathies. Rheum Dis Clin North Am 24:771–784
Braun J, Baraliakos X, Listing J, Sieper J (2005) Decreased incidence of anterior uveitis in patients with ankylosing spondylitis treated with the anti-tumor necrosis factor agents infliximab and etanercept. Arthritis Rheum 52(8):2447–2451
Rudwaleit M, Rodevand E, Holck P, Vanhoof J, Kron M, Kary S, Kupper H (2009) Adalimumab effectively reduces the rate of anterior uveitis flares in patients with active ankylosing spondylitis: results of a prospective open-label study. Ann Rheum Dis 68(5):696–701
Demiroglu H, Dundar S (1997) Effects of age, sex, and initial presentation on the clinical course of Behçet's syndrome. S Med J 90:567
Takamoto M, Kaburaki T, Numaga J, Fujino Y, Kawashima H (2007) Long-term infliximab treatment for Behçet’s disease. Jap J Ophthalmol 51:239–240
Silva Freitas S, Dionello CF, Rezende LS, Serratto VA, Baumle ACB, Rachid Filho A (2005) Infliximab treatment for refractory posterior uveitis in Behçet’s disease. Rev Bras Reumatol 45(2):94–97
Niccoli L, Nannini C, Benucci M, Chindamo D, Cassarà E, Salvarani C, Cimino L, Gini G, Lenzetti I, Cantini F (2007) Long-term efficacy of infliximab in refractory posterior uveitis of Behcet's disease: a 24-month follow-up study. Rheumatol Oxf 46(7):1161–1164
Deuter CM, Zierhut M, Möhle A, Vonthein R, Stöbiger N, Kötter I (2010) Long-term remission after cessation of interferon-alpha treatment in patients with severe uveitis due to Behçet's disease. Arthritis Rheum 62(9):2796–2805
Hamuryudan V, Ozyazgan Y, Fresko Y, Mat C, Yurdakul S, Yazici H (2002) Interferon alfa combined with azathioprine for the uveitis of Behcet’s disease: an open study. Isr Med Assoc J 4(11):928–930
Commodaro AG, Peron JPS, Genre J, Arslanian C, Sanches L, Muccioli C, Rizzo LV, Belfort R Jr (2010) IL-10 and TGF-β immunoregulatory cytokines rather than natural regulatory T cells are associated with the resolution phase of Vogt-Koyanagi-Harada (VKH) syndrome. Scan J Immunol 72:31–37
Li F, Yang P, Liu X, Wang C, Hou S, Kijlstra A (2010) Upregulation of interleukin 21 and promotion of interleukin 17 production in chronic or recurrent Vogt-Koyanagi-Harada disease. Arch Ophthalmol 128(11):1449–1454
Newman LS, Rose CS, Maier LA (1997) Sarcoidosis. N Engl J Med 336:1224–1234
Khalatbari D, Stinnett S, McCallum RM, Jaffe GJ (2004) Demographic-related variations in posterior segment ocular sarcoidosis. Ophthalmology 111(2):357–362
Saligan LN, Levy-Clarke G, Wu T, Faia LJ, Wroblewski K, Yeh S, Nussenblatt RB, Sen HN (2010) Quality of life in sarcoidosis: comparing the impact of ocular and non-ocular involvement of the disease. Ophthalmic Epidemiol 17(4):217–224
Herbort CP, Rao NA, Mochizuki M, members of Scientific Committee of First International Workshop on Ocular Sarcoidosis (2009) International criteria for the diagnosis of ocular sarcoidosis: results of the first International Workshop On Ocular Sarcoidosis (IWOS). Ocul Immunol Inflamm 17(3):160–169
Wakefield D, Zierhut M (2010) Controversy: ocular sarcoidosis. Ocul Immunol Inflamm 18(1):5–9
Heiligenhaus A, Wefelmeyer D, Wefelmeyer E, Rösel M, Schrenk M (2010) The eye as a common site for the early clinical manifestation of sarcoidosis. Ophthalmic Res 46(1):9–12
Rosenbaum JT, Hessellund A, Phan I, Planck SR, Wilson DJ (2010) The expression of STAT-1 and phosphorylated STAT-1 in conjunctival granulomas. Ocul Immunol Inflamm 18(4):261–264
Baughman RP, Lower EE, Kaufman AH (2010) Ocular sarcoidosis. Semin Respir Crit Care Med 31(4):452–462
Ravelli A, Martini A (2007) Juvenile idiopathic arthritis. Lancet 369(9563):767–778
Heiligenhaus A, Niewerth M, Ganser G, Heinz C, Minden K, German Uveitis in Childhood Study Group* (2007) Prevalence and complications of uveitis in juvenile idiopathic arthritis in a population-based nation-wide study in Germany: suggested modification of the current screening guidelines. Rheumatol Oxf 46(6):1015–1019
Edelsten C, Lee V, Bentley CR, Kanski JJ, Graham EM (2002) An evaluation of baseline risk factors predicting severity in juvenile idiopathic arthritis associated uveitis and other chronic anterior uveitis in early childhood. Br J Ophthalmol 86:51–56
Cassidy J, Kivlin J, Lindsley C, Nocton J (2006) Ophthalmologic examinations in children with juvenile rheumatoid arthritis. Pediatrics 117(5):1843–1845
Reininga JKL, Los I, Wulffraat NM, Armbrust W (2008) The evaluation of uveitis in juvenile idiopathic arthritis (JIA) patients: are current ophthalmologic screening guidelines adequate? Clin Exp Rheumatol 26(2):367–372
Foeldvari I, Wierk A (2005) Methotrexate is an effective treatment for chronic uveitis associated with juvenile idiopathic arthritis. J Rheumatol 32(2):362–365
Heinz C, Heiligenhaus A, Kümmerle-Deschner J, Foeldvari I (2010) Uveitis in juvenile idiopathic arthritis. Z Rheumatol 69(5):411–418
Foeldvari I, Nielsen S, Kummerle-Deschner J, Espada G, Horneff G, Bica B, Olivieri AN, Wierk A, Saurenmann RK (2007) Tumor necrosis factor-alpha blocker in treatment of juvenile idiopathic arthritis-associated uveitis refractory to second-line agents: Results of a multinational survey. J Rheumatol 34(5):1146–1150
Kenawy N, Cleary G, Mewar D, Beare N, Chandna A, Pearce I (2011) Abatacept: a potential therapy in refractory cases of juvenile idiopathic arthritis-associated uveitis. Graefes Arch Clin Exp Ophthalmol 249(2):297–300
Zulian F, Balzarin M, Flacini F, Martini G, Alessio M, Cimaz R, Cimino L, Zannin ME (2010) Abatacept for severe anti-tumor necrosis factor alpha refractory juvenile idiopathic arthritis-related uveitis. Arthritis Care Res Hoboken 62(6):821–825
Simonini G, Cantarini L, Bresci C, Lorusso M, Galeazzi M, Cimaz R (2010) Current therapeutic approaches to autoimmune chronic uveitis in children. Autoimmun Rev 9(10):674–683
Venaille A, Palombi K, Templier I, Bouillet L, Pagnier A, Debillon T, Bourdat-Michel G (2011) Vogt-Koyanagi-Harada syndrome: a serious and rare emergency in children. Arch Pediatr 18(1):33–36, French
Mackensen F (2009) Tubulointerstitial nephritis and uveitis syndrome. Curr Opin Ophthalmol 20(6):525–531
Langer-Gould A, Albers KB, Van Den Eeden SK, Nelson LM (2010) Autoimmune diseases prior to the diagnosis of multiple sclerosis: a population-based case-control study. Mult Scler 16(7):855–861
Hikita ST, Vistica BP, Jones HR, Keswani JR, Watson MM, Ericson VR, Ayoub GS, Gery I, Clegg DO (2006) Osteopontin is proinflammatory in experimental autoimmune uveitis. Investig Ophthalmol Vis Sci 47:4435–4443
Gregerson DS, Torseth JW, McPherson SW, Roberts JP, Shinohara T, Zack DJ (1999) Retinal expression of a neo-self antigen, beta-galactosidase, is not tolerogenic and creates a target for autoimmune uveoretinitis. J Immunol 163(2):1073–1080
Gregerson DS, Heuss ND, Lehmann U, McPherson SW (2009) Peripheral induction of tolerance by retinal antigen expression. J Immunol 183(2):814–822
Bora NS, Sohn JH, Kang SG, Cruz JM, Nishihori H, Suk HJ, Wang Y, Kaplan HJ, Bora PS (2004) Type I collagen is the autoantigen in experimental anterior uveitis. J Immunol 172:7086–7094
Kim Y, Caberoy NB, Alvarado G, Davis JL, Feuer WJ, Li W (2011) Identification of Hnrph3 as an autoantigen for acute anterior uveitis. Clin Immunol 138(1):60–66
Caspi RR (2010) A look at autoimmunity and inflammation in the eye. J Clin Invest 120(9):3073–3083
Commodaro AG, Bueno V, Belfort R Jr, Rizzo LV (2011) Autoimmune uveitis: the associated proinflammatory molecules and the search for immunoregulation. Autoimmun Rev 10(4):205–209
Chan CC, Caspi RR, Ni M, Leake WC, Wiggert B, Chader GJ, Nussenblatt RB (1990) Pathology of experimental autoimmune uveoretinitis in mice. J Autoimmun 3:247–255
Caspi RR, Chan CC, Wiggert B, Chader GJ, Nussenblatt RB (1990) The mouse as a model of experimental autoimmune uveoretinitis (EAU). Curr Eye Res s9:169–174
Jiang HR, Lumsden L, Forrester JV (1999) Macrophages and dendritic cells in IRBP- induced experimental autoimmune uveoretinitis in B10.RIII mice. Investig Ophthalmol Vis Sci 40:3177–3185
Takeuchi M, Yokoi H, Tsukahara R, Sakai J, Usui M (2001) Differentiation of Th1 and Th2 cells in lymph nodes and spleens of mice during experimental autoimmune uveoretinitis. Jpn J Ophthalmol 45:463–469
Sun M, Yang P, Du L, Zhou H, Ren X, Kijlstra A (2010) Contribution of CD4+CD25+T cells to the regression phase of experimental autoimmune uveoretinitis. Investig Ophthalmol Vis Sci 51:383–389
Pennesi G, Mattapallil MJ, Sun SH, Avichezer D, Silver PB, Karabekian Z, David CS, Hargrave PA, McDowell JH, Smith WC, Wiggert B, Donoso LA, Chan CC, Caspi RR (2003) A humanized model of experimental autoimmune uveitis in HLA class II transgenic mice. J Clin Invest 111(8):1171–1180
Keino H, Watanabe T, Sato Y, Okada AA (2010) Anti-inflammatory effect of retinoic acid on experimental autoimmune uveoretinitis. Br J Ophthalmol 94:802–807
Pacheco PA, Taylor SR, Cuchacovich MT, Diaz GV (2008) Azathioprine in the management of autoimmune uveitis. Ocul Immunol Inflamm 16(4):161–165
Ayuso VK, Van de Winkel EL, Rothova A, de Boer JH (2011) Relapse rate of uveitis post-methotrexate treatment in juvenile idiopathic arthritis. Am J Ophthalmol 151(1):217–222
Yeh S, Nussenblatt RB (2008) Fluocinolone acetonide for the treatment of uveitis: weighing the balance between local and systemic immunosuppression. Arch Ophthalmol 126(9):1287–1289
Kurup S, Lew J, Byrnes G, Yeh S, Nussenblatt R, Levy-Clarke G (2009) Therapeutic efficacy of intravitreal bevacizumab on posterior uveitis complicated by neovascularization. Acta Ophthalmol 87(3):349–352
Diebold Y, Calonge M (2010) Applications of nanoparticles in ophthalmology. Prog Retin Eye Res 29(6):596–609
Yoshimura T, Sonoda KH, Ohguro N, Ohsugi Y, Ishibashi T, Cua DJ, Kobayashi T, Yoshida H, Yoshimura A (2009) Involvement of Th17 cells and the effect of anti-IL-6 therapy in autoimmune uveitis. Rheumatol Oxf 48(4):347–354
Chi W, Yang P, Li B, Wu C, Jin H, Zhu X, Chen L, Zhou H, Huang X, Kijlstra A (2007) IL-23 promotes CD4+ T cells to produce IL-17 in Vogt–Koyanagi–Harada disease. J Allergy Clin Immunol 119:1218–1224
Liu L, Xu Y, Wang j, Li H (2009) Upregulated IL-21 and IL-21 receptor expression is involved in experimental autoimmune uveitis (EAU). Mol Vis 15:2938–2944
Hueber W, Patel DD, Dryja T, Wright AM, Koroleva I, Bruin G, Antoni C, Draelos Z, Gold MH, Psoriasis Study Group, Durez P, Tak PP, Gomez-Reino JJ, Rheumatoid Arthritis Study Group, Foster CS, Kim RY, Samson CM, Falk NS, Chu DS, Callanan D, Nguyen QD, Uveitis Study Group, Rose K, Haider A, Di Padova F (2010) Effects of AIN457, a fully human antibody to interleukin-17A, on psoriasis, rheumatoid arthritis, and uveitis. Sci Transl Med 6(52):52–72
Ke Y (2009) Anti-inflammatory role of IL-17 in experimental autoimmune uveitis. J Immunol 182(5):3183–3190
Sugita S, Yamada Y, Kaneko S, Horie S, Mochizuki M (2011) Induction of regulatory T cells by infliximab in Behcet's disease. Invest Ophthalmol Vis Sci 52(2):476–484
Sen HN, Levy-Clarke G, Faia LJ, Li Z, Yeh S, Barron KS, Ryan JG, Hammel K, Nussenblatt RB (2009) High-dose daclizumab for the treatment of juvenile idiopathic arthritis-associated active anterior uveitis. Am J Ophthalmol 148(5):696–703
Pato E, Muñoz-Fernández S, Francisco F, Abad MA, Maese J, Ortiz A, Carmona L, Uveitis Working Group from Spanish Society of Rheumatology (2011) Systematic review on the effectiveness of immunosuppressants and biological therapies in the treatment of autoimmune posterior uveitis. Semin Arthritis Rheum 40(4):314–323
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Levy, R.A., de Andrade, F.A. & Foeldvari, I. Cutting-Edge Issues in Autoimmune Uveitis. Clinic Rev Allerg Immunol 41, 214–223 (2011). https://doi.org/10.1007/s12016-011-8267-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12016-011-8267-x