Abstract
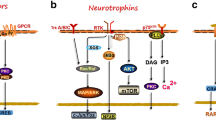
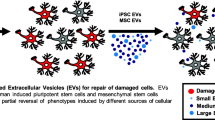
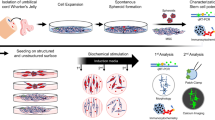
Advances in stem cell (SC) technology allow the generation of cellular models that recapitulate the histological, molecular and physiological properties of humanized in vitro three dimensional (3D) models, as well as production of cell-derived therapeutics such as extracellular vesicles (EVs). Improvements in organ-on-chip platforms and human induced pluripotent stem cells (hiPSCs) derived neural/glial cells provide unprecedented systems for studying 3D personalized neural tissue modeling with easy setup and fast output. Here, we highlight the key points in differentiation procedures for neurons, astrocytes, oligodendrocytes and microglia from single origin hiPSCs. Additionally, we present a well-defined humanized neural tissue-on-chip model composed of differentiated cells with the same genetic backgrounds, as well as the therapeutic potential of bone marrow mesenchymal stem cells (BMSCs)-derived extracellular vesicles to propose a novel treatment for neuroinflammation derived diseases. Around 100 nm CD9 + EVs promote a more anti-inflammatory and pro-remodeling of cell–cell interaction cytokine responses on tumor necrosis factor-α (TNF-α) induced neuroinflammation in neural tissue-on-chip model which is ideal for modeling authentic neural-glial patho-physiology.
Graphical Abstract






Similar content being viewed by others
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code Availability
Not applicable.
References
Cakmak, B., Beceren, G., Saglam-metiner, P., Yesil-Celiktas, O., & Zhang, Y. S. (2022). A 3D in vitro co-culture model for evaluating biomaterial-mediated modulation of foreign-body responses. Bio-Design and Manufacturing, 5(3), 465–480. https://doi.org/10.1007/s42242-022-00198-z
Hendriksen, E., van Bergeijk, D., Oosting, R. S., & Redegeld, F. A. (2017). Mast cells in neuroinflammation and brain disorders. Neuroscience and Biobehavioral Reviews, 79(May), 119–133. https://doi.org/10.1016/j.neubiorev.2017.05.001
Companys-Alemany, J., Turcu, A. L., Vázquez, S., Pallàs, M., & Griñán-Ferré, C. (2022). Glial cell reactivity and oxidative stress prevention in Alzheimer’s disease mice model by an optimized NMDA receptor antagonist. Scientific Reports, 12(1), 1–15. https://doi.org/10.1038/s41598-022-22963-x
Rauf, A., Badoni, H., Abu-Izneid, T., Olatunde, A., Rahman, M. M., Painuli, S., … Mubarak, M. S. (2022). Neuroinflammatory Markers: Key Indicators in the Pathology of Neurodegenerative Diseases. Molecules, 27(10), 1–25. https://doi.org/10.3390/molecules27103194
Errede, M., Annese, T., Petrosino, V., Longo, G., Girolamo, F., de Trizio, I., … Virgintino, D. (2022). Microglia-derived CCL2 has a prime role in neocortex neuroinflammation. Fluids and Barriers of the CNS, 19(1), 1–25. https://doi.org/10.1186/s12987-022-00365-5
Dong, H., Zhang, X., & Qian, Y. (2014). Mast cells and neuroinflammation. Medical Science Monitor Basic Research, 20, 200–206. https://doi.org/10.12659/MSMBR.893093
Sharma, N., Sharma, S., & Nehru, B. (2017). Curcumin protects dopaminergic neurons against inflammation-mediated damage and improves motor dysfunction induced by single intranigral lipopolysaccharide injection. Inflammopharmacology, 25(3), 351–368. https://doi.org/10.1007/s10787-017-0346-z
Peng, Z., Peng, S., Lin, K., Zhao, B., Wei, L., Tuo, Q., … Shi, Z. (2022). Chronic stress-induced depression requires the recruitment of peripheral Th17 cells into the brain. Journal of Neuroinflammation, 19(1), 1–14. https://doi.org/10.1186/s12974-022-02543-6
Yaldiz, B., Saglam-Metiner, P., & Yesil-Celiktas, O. (2022). Decellularised extracellular matrix-based biomaterials for repair and regeneration of central nervous system. Expert Reviews in Molecular Medicine, 23(e25), 1–11. https://doi.org/10.1017/erm.2021.22
Shaker, T., Chattopadhyaya, B., Amilhon, B., Cristo, G. Di, & Weil, A. G. (2021). Transduction of inflammation from peripheral immune cells to the hippocampus induces neuronal hyperexcitability mediated by Caspase-1 activation. Neurobiology of Disease, 160. https://doi.org/10.1016/j.nbd.2021.105535
Lon, H. K., Liu, D., & Jusko, W. J. (2012). Pharmacokinetic/pharmacodynamic modeling in inflammation. Critical Reviews in Biomedical Engineering, 40(4), 295–312. https://doi.org/10.1615/CritRevBiomedEng.v40.i4.50
Ingber, D. E. (2020). Is it time for reviewer 3 to request human organ chip experiments instead of animal validation studies? Advanced Science, 7(22), 1–15. https://doi.org/10.1002/advs.202002030
Cecen, B., Saygili, E., Zare, I., Nejati, O., Khorsandi, D., Zarepour, A., … Bal-Öztürk, A. (2023). Biosensor integrated brain-on-a-chip platforms: Progress and prospects in clinical translation. Biosensors and Bioelectronics, 225(January). https://doi.org/10.1016/j.bios.2023.115100
Zhu, Y., Zhang, X., Sun, L., Wang, Y., & Zhao, Y. (2023). Engineering Human Brain Assembloids by Microfluidics. Advanced Materials, 2210083, 1–8. https://doi.org/10.1002/adma.202210083
Yesil-Celiktas, O., Hassan, S., Miri, A. K., Maharjan, S., Al-kharboosh, R., Quiñones-Hinojosa, A., & Zhang, Y. S. (2018). Mimicking human pathophysiology in organ-on-chip devices. Advanced Biosystems, 2(10), 1–25. https://doi.org/10.1002/adbi.201800109
Pediaditakis, I., Kodella, K. R., Manatakis, D. V., Le, C. Y., Hinojosa, C. D., Tien-Street, W., … Karalis, K. (2021). Modeling alpha-synuclein pathology in a human brain-chip to assess blood-brain barrier disruption. Nature Communications, 12(1), 1–17. https://doi.org/10.1038/s41467-021-26066-5
Freundt, E. C., Maynard, N., Clancy, E. K., Roy, S., Bousset, L., Sourigues, Y., … Michel Brahic, M. (2012). Neuron-to-neuron transmission of α-synuclein fibrils through axonal transport. Bone, 23(1), 1–7. https://doi.org/10.1002/ana.23747.Neuron-to-neuron
Takeda, S., Wegmann, S., Cho, H., Devos, S. L., Commins, C., Roe, A. D., … Hyman, B. T. (2015). Neuronal uptake and propagation of a rare phosphorylated high-molecular-weight tau derived from Alzheimer’s disease brain. Nature Communications, 6. https://doi.org/10.1038/ncomms9490
Calafate, S., Buist, A., Miskiewicz, K., Vijayan, V., Daneels, G., de Strooper, B., … Moechars, D. (2015). Synaptic contacts enhance cell-to-cell tau pathology propagation. Cell Reports, 11(8), 1176–1183. https://doi.org/10.1016/j.celrep.2015.04.043
Brahic, M., Bousset, L., Bieri, G., Melki, R., & Gitler, A. D. (2016). Axonal transport and secretion of fibrillar forms of α-synuclein, Aβ42 peptide and HTTExon 1. Acta Neuropathologica, 131(4), 539–548. https://doi.org/10.1007/s00401-016-1538-0
Katsikoudi, A., Ficulle, E., Cavallini, A., Sharman, G., Guyot, A., Zagnoni, M., … Bose, S. (2020). Quantitative propagation of assembled human Tau from Alzheimer’s disease brain in microfluidic neuronal cultures. Journal of Biological Chemistry, 295(37), 13079–13093. https://doi.org/10.1074/jbc.RA120.013325
Ghasemi, M., Roshandel, E., Mohammadian, M., Farhadihosseinabadi, B., Akbarzadehlaleh, P., & Shamsasenjan, K. (2023). Mesenchymal stromal cell-derived secretome-based therapy for neurodegenerative diseases: Overview of clinical trials. Stem cell research & therapy, 14(1), 122. https://doi.org/10.1186/s13287-023-03264-0
Oveili, E., Vafaei, S., Bazavar, H., Eslami, Y., Mamaghanizadeh, E., Yasamineh, S., & Gholizadeh, O. (2023). The potential use of mesenchymal stem cells-derived exosomes as microRNAs delivery systems in different diseases. Cell Communication and Signaling, 21(1), 1–26. https://doi.org/10.1186/s12964-022-01017-9
Yu, F., Wang, Y., Huang, C.-Q., Lin, S.-J., Gao, R.-X., & Wu, R.-Y. (2023). Neuroprotective effect of mesenchymal stem cell-derived extracellular vesicles on optic nerve injury in chronic ocular hypertension. Neural Regeneration Research. https://doi.org/10.4103/1673-5374.369121
Kimiz-Gebologlu, I., & Oncel, S. S. (2022). Exosomes: Large-scale production, isolation, drug loading efficiency, and biodistribution and uptake. Journal of Controlled Release, 347(May), 533–543. https://doi.org/10.1016/j.jconrel.2022.05.027
Brosseau, C., Colas, L., Magnan, A., & Brouard, S. (2018). CD9 tetraspanin: A new pathway for the regulation of inflammation? Frontiers in Immunology, 9(OCT), 1–12. https://doi.org/10.3389/fimmu.2018.02316
Shi, Y., Kang, X., Wang, Y., Bian, X., He, G., Zhou, M., & Tang, K. (2020). Exosomes derived from bone marrow stromal cells (BMSCs) enhance tendon-bone healing by regulating macrophage polarization. Medical Science Monitor, 26. https://doi.org/10.12659/MSM.923328
Yuan, Y., Sun, J., You, T., Shen, W., Xu, W., Dong, Q., & Cui, M. (2022). Extracellular vesicle-based therapeutics in neurological disorders. Pharmaceutics, 14(12), 1–15. https://doi.org/10.3390/pharmaceutics14122652
Casajuana Ester, M., & Day, R. M. (2023). Production and utility of extracellular vesicles with 3D culture methods. Pharmaceutics, 15(2). https://doi.org/10.3390/pharmaceutics15020663
Zhang, Z. X., Zhou, Y. J., Gu, P., Zhao, W., Chen, H. X., Wu, R. Y., ... & An, S. J. (2023). Exosomes derived from human umbilical cord mesenchymal stem cells alleviate Parkinson’s disease and neuronal damage through inhibition of microglia. Neural Regeneration Research, 18(10), 2291–2300. https://doi.org/10.4103/1673-5374.368300
Sheng, X., Zhao, J., Li, M., Xu, Y., Zhou, Y., Xu, J., … Hu, J. (2021). Bone marrow mesenchymal stem cell-derived exosomes accelerate functional recovery after spinal cord ınjury by promoting the phagocytosis of macrophages to clean myelin debris. Frontiers in Cell and Developmental Biology, 9(November), 1–19. https://doi.org/10.3389/fcell.2021.772205
Nguyen, V. V. T., Witwer, K. W., Verhaar, M. C., Strunk, D., & van Balkom, B. W. M. (2020). Functional assays to assess the therapeutic potential of extracellular vesicles. Journal of Extracellular Vesicles, 10(1). https://doi.org/10.1002/jev2.12033
Deliloglu-gurhan, S. I., Vatansever, H. S., Ozdal-kurt, F., & Tuglu, I. (2006). Characterization of osteoblasts derived from bone marrow stromal cells in a modified cell culture system, 108. https://doi.org/10.1016/j.acthis.2005.11.001
Yurtsever, M. C., Science, A., Cakmak, S., & Sen, B. H. (2012). Random / aligned electrospun PCL / PCL-collagen nanofibrous membranes : Comparison of neural differentiation of rat AdMSCs and BMSCs Random / aligned electrospun PCL / PCL-collagen nanofibrous membranes : comparison of neural differentiation of rat AdMSCs, (August). https://doi.org/10.1088/1748-6041/7/4/045013
Yaldiz, B., Saglam-Metiner, P., Cakmak, B., Kaya, E., Deliogullari, B., & Yesil-Celiktas, O. (2022). Essential Oil and Supercritical Carbon Dioxide Extract of Grapefruit Peels Formulated for Candida albicans Infections: Evaluation by an in Vitro Model to Study Fungal-Host Interactions. ACS Omega, 7(42), 37427–37435. https://doi.org/10.1021/acsomega.2c04189
Patel, D. B., Gray, K. M., Santharam, Y., Lamichhane, T. N., Stroka, K. M., & Jay, S. M. (2017). Impact of cell culture parameters on production and vascularization bioactivity of mesenchymal stem cell-derived extracellular vesicles. Bioengineering & Translational Medicine, 2(2), 170–179. https://doi.org/10.1002/btm2.10065
Karttunen, J., Heiskanen, M., Joki, T., Hyysalo, A., Navarro-Ferrandis, V., Miettinen, S., … Pitkänen, A. (2022). Effect of cell culture media on extracellular vesicle secretion from mesenchymal stromal cells and neurons. European Journal of Cell Biology, 101(4). https://doi.org/10.1016/j.ejcb.2022.151270
Akbari, S., Sevinç, G. G., Ersoy, N., Basak, O., Kaplan, K., Sevinç, K., … Erdal, E. (2019). Robust, long-term culture of endoderm-derived hepatic organoids for disease modeling. stem cell reports, 13(4), 627–641. https://doi.org/10.1016/j.stemcr.2019.08.007
Saglam-metiner, P., Devamoglu, U., Filiz, Y., Akbari, S., Beceren, G., Goker, B., … Yesil-celiktas, O. (2023). Spatio-temporal dynamics enhance cellular diversity, neuronal function and further maturation of human cerebral organoids. Communications Biology, 6(173). https://doi.org/10.1038/s42003-023-04547-1
Yaldiz, B., Saglam-metiner, P., Cam, S. B., Korkusuz, P., & Yesil-celiktas, O. (2021). Effect of sterilization methods on the mechanical stability and extracellular matrix constituents of decellularized brain tissues. The Journal of Supercritical Fluids, 175(May), 105299. https://doi.org/10.1016/j.supflu.2021.105299
Verkhratsky, A., & Butt, A. (2013). Glial physiology and pathophysiology. Wiley-Blackwell.
Neniskyte, U., Vilalta, A., & Brown, G. C. (2014). Tumour necrosis factor alpha-induced neuronal loss is mediated by microglial phagocytosis. FEBS Letters, 588(17), 2952–2956. https://doi.org/10.1016/j.febslet.2014.05.046
Gupta, D., Zickler, A. M., & El Andaloussi, S. (2021). Dosing extracellular vesicles. Advanced Drug Delivery Reviews, 178, 113961. https://doi.org/10.1016/j.addr.2021.113961
Maldonado, V. V., Patel, N. H., Smith, E. E., Barnes, C. L., Gustafson, M. P., Rao, R. R., & Samsonraj, R. M. (2023). Clinical utility of mesenchymal stem/stromal cells in regenerative medicine and cellular therapy. Journal of Biological Engineering, 17(1), 1–22. https://doi.org/10.1186/s13036-023-00361-9
Yaldiz, B., Saglam-Metiner, P., Cam, S. B., Korkusuz, P., & Yesil-Celiktas, O. (2021). Effect of sterilization methods on the mechanical stability and extracellular matrix constituents of decellularized brain tissues. Journal of Supercritical Fluids, 175(January), 105299. https://doi.org/10.1016/j.supflu.2021.105299
Pediaditakis, I., Kodella, K. R., Manatakis, D. V., Le, C. Y., Barthakur, S., Sorets, A., … Karalis, K. (2022). A microengineered Brain-Chip to model neuroinflammation in humans. iScience, 25(8), 104813. https://doi.org/10.1016/j.isci.2022.104813
Jayaraman, A., Htike, T. T., James, R., Picon, C., & Reynolds, R. (2021). TNF-mediated neuroinflammation is linked to neuronal necroptosis in Alzheimer’s disease hippocampus. Acta Neuropathologica Communications, 9(1), 1–21. https://doi.org/10.1186/s40478-021-01264-w
Galderisi, U., Peluso, G., & Di Bernardo, G. (2022). Clinical trials based on mesenchymal stromal cells are exponentially increasing: where are we in recent years? Stem Cell Reviews and Reports, 18(1), 23–36. https://doi.org/10.1007/s12015-021-10231-w
Galipeau, J., & Sensébé, L. (2018). Mesenchymal stromal cells: clinical challenges and therapeutic opportunities. Cell Stem Cell, 22(6), 824–833. https://doi.org/10.1016/j.stem.2018.05.004
Riazifar, M., M. Rezaa Mohammadi, E. J. P., Yeri, A., Segaliny, C. L. A. I., McIntyre, L. L., Shelke, G. V., … Zhao, W. (2017). Stem Cell-Derived Exosomes as Nanotherapeutics for Autoimmune and Neurodegenerative Disorders. Physiology & behavior, 176(3), 139–148.https://doi.org/10.1053/j.gastro.2016.08.014.CagY
Lehrich, B. M., Liang, Y., & Fiandaca, M. S. (2021). Foetal bovine serum influence on in vitro extracellular vesicle analyses. Journal of Extracellular Vesicles, 10(3). https://doi.org/10.1002/jev2.12061
Shall, G., Menosky, M., Decker, S., Nethala, P., Welchko, R., Leveque, X., … Dunbar, G. (2018). Effects of passage number and differentiation protocol on the generation of dopaminergic neurons from rat bone marrow-derived mesenchymal stem cells. International Journal of Molecular Sciences, 19(3). https://doi.org/10.3390/ijms19030720
O’Neill, C. P., Gilligan, K. E., & Dwyer, R. M. (2019). Role of extracellular vesicles (EVs) in cell stress response and resistance to cancer therapy. Cancers, 11(2), 1–14. https://doi.org/10.3390/cancers11020136
Sikora, M., Śmieszek, A., & Marycz, K. (2021). Bone marrow stromal cells (BMSCs CD45-/CD44+/CD73+/CD90+) isolated from osteoporotic mice SAM/P6 as a novel model for osteoporosis investigation. Journal of Cellular and Molecular Medicine, 25(14), 6634–6651. https://doi.org/10.1111/jcmm.16667
Mehmet, K., & Gupta, R. (2018). Physical characterization and profiling of airway epithelial derived exosomes using light scattering. Physiology & behavior, 176(5), 139–148. https://doi.org/10.4049/jimmunol.1801473.The
Sitar, S., Kejžar, A., Pahovnik, D., Kogej, K., Tušek-Žnidarič, M., Lenassi, M., & Žagar, E. (2015). Size characterization and quantification of exosomes by asymmetrical-flow field-flow fractionation. Analytical Chemistry, 87(18), 9225–9233. https://doi.org/10.1021/acs.analchem.5b01636
Lyu, T. S., Ahn, Y., Im, Y. J., Kim, S. S., Lee, K. H., Kim, J., … Cho, J. A. (2021). The characterization of exosomes from fibrosarcoma cell and the useful usage of Dynamic Light Scattering (DLS) for their evaluation. PLoS ONE, 16(1 1), 1–14. https://doi.org/10.1371/journal.pone.0231994
Doyle, L. M., & Zhuo Wang, M. (2019). Overview of extracellular vesicles, their origin, composition, purpose, and methods for exosome isolation and analysis. Cells, 8(7), 727. https://doi.org/10.3390/cells8070727
Kalluri, R., & LeBleu, V. S. (2020). The biology, function, and biomedical applications of exosomes. Science, 367(6478). https://doi.org/10.1126/science.aau6977
Akagi, T., Iida, Y., Nakanishi, H., Terada, N., Morooka, S., Yamada, H., Hasegawa, T., Yokota, S., Yoshikawa, M., N. Y. (2016). Microvascular density in glaucomatous eyes with hemifield visual field defects: an optical coherence tomography angiography study. American Journal of Ophthalmology.https://doi.org/10.1016/j.ajo.2016.06.009
Böker, K. O., Lemus-Diaz, N., Rinaldi Ferreira, R., Schiller, L., Schneider, S., & Gruber, J. (2018). The Impact of the CD9 Tetraspanin on Lentivirus Infectivity and Exosome Secretion. Molecular Therapy, 26(2), 634–647. https://doi.org/10.1016/j.ymthe.2017.11.008
Brzozowski, J. S., Bond, D. R., Jankowski, H., Goldie, B. J., Burchell, R., Naudin, C., … Weidenhofer, J. (2018). Extracellular vesicles with altered tetraspanin CD9 and CD151 levels confer increased prostate cell motility and invasion. Scientific Reports, 8(1), 1–13. https://doi.org/10.1038/s41598-018-27180-z
Maia, J., Batista, S., Couto, N., Gregório, A. C., Bodo, C., Elzanowska, J., … Costa-Silva, B. (2020). Employing flow cytometry to extracellular vesicles sample microvolume analysis and quality control. Frontiers in Cell and Developmental Biology, 8(October), 1–15. https://doi.org/10.3389/fcell.2020.593750
Marchetto, M. C. N., Carromeu, C., Acab, A., Yu, D., Yeo, G. W., Mu, Y., … Muotri, A. R. (2010). A model for neural development and treatment of rett syndrome using human ınduced pluripotent stem cells. Cell, 143(4), 527–539. https://doi.org/10.1016/j.cell.2010.10.016
Saglam-Metiner, P., Gulce-Iz, S., & Biray-Avci, C. (2019). Bioengineering-inspired three-dimensional culture systems: Organoids to create tumor microenvironment. Gene, 686(November 2018), 203–212. https://doi.org/10.1016/j.gene.2018.11.058
Takahashi, K., & Yamanaka, S. (2006). Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors, 2, 663–676.https://doi.org/10.1016/j.cell.2006.07.024
Johnson, M. A., Weick, J. P., Pearce, R. A., & Zhang, S. (2007). functional neural development from human embryonic stem cells : accelerated synaptic activity via astrocyte coculture, 27(12), 3069–3077.https://doi.org/10.1523/JNEUROSCI.4562-06.2007
Kang, S., Chen, X., Gong, S., Yu, P., Yau, S., Su, Z., & Zhou, L. (2017). Characteristic analyses of a neural differentiation model from iPSC- derived neuron according to morphology , physiology , and global gene expression pattern. Scientific Reports, (February), 1–11. https://doi.org/10.1038/s41598-017-12452-x
Bell, S., & Nuwan C. Hettige, Heika Silveira, Huashan Peng, Hanrong Wu, Malvin Jefri, Lilit Antonyan, Ying Zhang, X. Z., & C. E. (2019). Differentiation of human ınduced pluripotent stem cells (ipscs) into an effective model of forebrain neural progenitor cells and mature neurons, 9, 1–18. https://doi.org/10.21769/BioProtoc.3188
Krencik, R., & Zhang, S. (2011). Directed differentiation of functional astroglial subtypes from human pluripotent stem cells. Nature Protocols, 6(11), 1710–1717. https://doi.org/10.1038/nprot.2011.405
Tcw, J., Wang, M., Pimenova, A. A., Bowles, K. R., Hartley, B. J., Lacin, E., … Brennand, K. J. (2017). An efficient platform for astrocyte differentiation from human ınduced pluripotent stem cells julia. Stem Cell Reports, 9(2), 600–614. https://doi.org/10.1016/j.stemcr.2017.06.018
Ogawa, S., Tokumoto, Y., Miyake, J., & Nagamune, T. (2011). Induction of oligodendrocyte differentiation from adult human fibroblast-derived induced pluripotent stem cells, 464–469. https://doi.org/10.1007/s11626-011-9435-2
Wang, S., Bates, J., Li, X., Schanz, S., Chandler-militello, D., Levine, C., … Goldman, S. A. (2013). Human iPSC-derived oligodendrocyte progenitor cells can myelinate and rescue a mouse model of congenital hypomyelination. Stem Cell, 12(2), 252–264. https://doi.org/10.1016/j.stem.2012.12.002
Abud, E. M., Ramirez, R. N., Martinez, E. S., Carson, M. J., Poon, W. W., Blurton-jones, M., … Newman, S. A. (2017). iPSC-derived human microglia-like cells to study neurological diseases. Neuron, 94(2), 278–293.e9. https://doi.org/10.1016/j.neuron.2017.03.042
Douvaras, P., Sun, B., Wang, M., Kruglikov, I., Lallos, G., Zimmer, M., … Fossati, V. (2017). Directed differentiation of human pluripotent stem cells to microglia panagiotis. Stem Cell Reports, 8(6), 1516–1524. https://doi.org/10.1016/j.stemcr.2017.04.023
Haenseler, W., Sansom, S. N., Buchrieser, J., Newey, S. E., Moore, C. S., Nicholls, F. J., … Cowley, S. A. (2017). A highly efficient human pluripotent stem cell microglia model displays a neuronal-co-culture-specific expression profile and ınflammatory response. Stem Cell Reports, 8(6), 1727–1742. https://doi.org/10.1016/j.stemcr.2017.05.017
Krencik, R., Seo, K., Asperen, J. V. Van, Basu, N., Cvetkovic, C., Barlas, S., … Ullian, E. M. (2017). Systematic three-dimensional coculture rapidly recapitulates ınteractions between human neurons and astrocytes. Stem Cell Reports, 9(6), 1745–1753. https://doi.org/10.1016/j.stemcr.2017.10.026
Schafer, S. T., Mansour, A. A., Schlachetzki, J. C. M., Glass, C. K., Nimmerjahn, A., & Gage, F. H. (2023). Article An in vivo neuroimmune organoid model to study human microglia phenotypes ll ll An in vivo neuroimmune organoid model to study human microglia phenotypes. Cell, 186(10), 2111-2126.e20. https://doi.org/10.1016/j.cell.2023.04.022
Perriot, S., Canales, M., & Mathias, A. (2021). Protocol Differentiation of functional astrocytes from human-induced pluripotent stem cells in chemically defined media Differentiation of functional astrocytes from human- induced pluripotent stem cells in chemically defined media. STAR Protocols, 2(4), 100902. https://doi.org/10.1016/j.xpro.2021.100902
Kuhn, S., Gritti, L., Crooks, D., & Dombrowski, Y. (2017). Oligodendrocytes in development, myelin generation and beyond sarah. Oral and Maxillofacial Surgery Clinics of North America, 29(1), ix. https://doi.org/10.1016/j.coms.2016.10.001
Behrangi, N., Lorenz, P., Kipp, M., & Kipp, M. (2021). Oligodendrocyte lineage marker expression in egfp ‑ gfap transgenic mice. Journal of Molecular Neuroscience, 2237–2248. https://doi.org/10.1007/s12031-020-01771-w
Maguire, E., Connor-Robson, N., Shaw, B., O’Donoghue, R., Stöberl, N., & Hall-Roberts, H. (2022). Assaying microglia functions In Vitro. Cells, 11(21). https://doi.org/10.3390/cells11213414
Caldeira, C., Oliveira, A. F., Cunha, C., Vaz, A. R., Falcão, A. S., Fernandes, A., & Brites, D. (2014). Microglia change from a reactive to an age-like phenotype with the time in culture. Frontiers in Cellular Neuroscience, 8(JUN), 1–16. https://doi.org/10.3389/fncel.2014.00152
Cui, L., Luo, W., Jiang, W., Li, H., Xu, J., Liu, X., … Chen, G. (2022). Human umbilical cord mesenchymal stem cell-derived exosomes promote neurological function recovery in rat after traumatic brain injury by inhibiting the activation of microglia and astrocyte. Regenerative Therapy, 21, 282–287. https://doi.org/10.1016/j.reth.2022.07.005
Zhang, C., Huang, Y., Ouyang, F., Su, M., Li, W., Chen, J., & Xiao, H. (2022). Extracellular vesicles derived from mesenchymal stem cells alleviate neuroinflammation and mechanical allodynia in interstitial cystitis rats by inhibiting NLRP3 inflammasome activation. Journal of Neuroinflammation, 1–14. https://doi.org/10.1186/s12974-022-02445-7
Brifault, C., Gras, M., Liot, D., May, V., Vaudry, D., & Wurtz, O. (2014). Delayed pituitary adenylate cyclase – activating polypeptide delivery after brain stroke ımproves functional recovery, 520–528. https://doi.org/10.1161/STROKEAHA.114.006864
Gordon, S., & Martinez, F. O. (2010). Review alternative activation of macrophages : mechanism and functions. Immunity, 32(5), 593–604. https://doi.org/10.1016/j.immuni.2010.05.007
Hu, L., Si, L., Dai, X., Dong, H., Ma, Z., Sun, Z., & Zhang, Z. (2021). Exosomal miR-409–3p secreted from activated mast cells promotes microglial migration, activation and neuroinflammation by targeting Nr4a2 to activate the NF- κ B pathway. Journal of Neuroinflammation, 18(1), 68. https://doi.org/10.1186/s12974-021-02110-5
Zong, L., Huang, P., Song, Q., & Kang, Y. (2021). Bone marrow mesenchymal stem cells-secreted exosomal H19 modulates lipopolysaccharides-stimulated microglial M1 / M2 polarization and alleviates inflammation-mediated neurotoxicity. American Journal of Translational Research, 13(3), 935–951.
Heo, J. S., & Kim, S. (2022). Human adipose mesenchymal stem cells modulate inflammation and angiogenesis through exosomes. Scientific Reports, 0123456789, 1–11. https://doi.org/10.1038/s41598-022-06824-1
Michetti, F. (2019). The S100B story: from biomarker to active factor in neural injury, 168–187. https://doi.org/10.1111/jnc.14574
Clarkson, B. D. S., Grund, E., David, K., Johnson, R. K., & Howe, C. L. (2022). ISGylation is induced in neurons by demyelination driving ISG15 - dependent microglial activation. Journal of Neuroinflammation, 4, 1–23. https://doi.org/10.1186/s12974-022-02618-4
Liu, M., Yang, Y., Zhao, B., Yang, Y., Wang, J., Shen, K., & Givogri, M. I. (2021). exosomes derived from adipose-derived mesenchymal stem cells ameliorate radiation-ınduced brain ınjury by activating the SIRT1 pathway, 9(July), 1–14. https://doi.org/10.3389/fcell.2021.693782
Esen, N., & Kielian, T. (2007). Diverse pathogen-associated molecular patterns ( PAMPs ), 18, 1–18. https://doi.org/10.1186/1742-2094-4-10
Wang, G., Li, H., Long, H., Gong, X., Hu, S., & Gong, C. (2022). Exosomes derived from mouse adipose-derived mesenchymal stem cells alleviate benzalkonium chloride-ınduced mouse dry eye model via ınhibiting nlrp3 ınflammasome, 40–51. https://doi.org/10.1159/000519458
Ou, W., Yang, J., Simanauskaite, J., Choi, M., Castellanos, D. M., Chang, R., … Sumbria, R. K. (2021). Biologic TNF ‑ α inhibitors reduce microgliosis , neuronal loss , and tau phosphorylation in a transgenic mouse model of tauopathy. Journal of Neuroinflammation, 1–19. https://doi.org/10.1186/s12974-021-02332-7
Yang, E. S., Jin, M. U., Hong, J. H., Kim, Y. S., Choi, S. Y., Kim, T. H., … Bae, Y. C. (2014). Expression of vesicular glutamate transporters VGLUT1 and VGLUT2 in the rat dental pulp and trigeminal ganglion following ınflammation, 9(10). https://doi.org/10.1371/journal.pone.0109723
Xu, Y., Jiang, Y., Wang, L., Huang, J., & Wen, J. (2019). Thymosin Alpha-1 Inhibits Complete Freund’s Adjuvant-Induced Pain and Production of Microglia-Mediated Pro-inflammatory Cytokines in Spinal Cord. Neuroscience Bulletin, 35(4), 637–648. https://doi.org/10.1007/s12264-019-00346-z
Du, X., Li, J., Li, M., Yang, X., Qi, Z., Xu, B., … Deng, Y. (2020). Research progress on the role of type I vesicular glutamate transporter ( VGLUT1 ) in nervous system diseases. Cell & Bioscience, 1–10. https://doi.org/10.1186/s13578-020-00393-4
Gábriel, R., Wilhelm, M., & Straznicky, C. (1992). Microtubule-associated protein 2 (MAP2)-immunoreactive neurons in the retina of Bufo marinus: colocalisation with tyrosine hydroxylase and serotonin in amacrine cells. Cell and Tissue Research, 269(1), 175–82. https://doi.org/10.1007/BF00384738
Hung, T. W., Wu, K. J., Wang, Y. S., Bae, E. K., Song, Y., Yoon, J., & Yu, S. J. (2021). Human milk oligosaccharide 2’-fucosyllactose induces neuroprotection from intracerebral hemorrhage stroke. International Journal of Molecular Sciences, 22(18), 9881. https://doi.org/10.3390/ijms22189881
Zhao, J., Bi, W., Xiao, S., Lan, X., Cheng, X., Zhang, J., & Lu, D. (2019). Neuroinflammation induced by lipopolysaccharide causes cognitive impairment in mice. Scientific Reports, 1–12. https://doi.org/10.1038/s41598-019-42286-8
Li, B., Lu, Y., Wang, R., Xu, T., Lei, X., Jin, H., … Liu, X. (2023). MiR ‑ 29c ınhibits TNF ‑ α ‑ ınduced ROS production and apoptosis in mouse hippocampal HT22 cell line, 519–536. https://doi.org/10.1007/s11064-022-03776-w
Ding, L., Xu, X., Li, C., Wang, Y., Xia, X., & Zheng, J. C. (2021). Brain behavior and ımmunity glutaminase in microglia : a novel regulator of neuroinflammation. Brain Behavior and Immunity, 92(November 2020), 139–156. https://doi.org/10.1016/j.bbi.2020.11.038
Thomas, A. G., O’Driscoll, M., C., Bressler, J., Kaufmann, W. E, Rojas, C. J., & Slusher B. S. (2015). Small molecule glutaminase ınhibitors block glutamate release from stimulated microglia ajit, 443(1), 32–36. https://doi.org/10.1016/j.bbrc.2013.11.043.Small
Milewski, K., Hilgier, W., Albrecht, J., & Zieli, M. (2019). Cytokine TNF α increases STAT3-mediated expression of glutaminase isoform KGA in cultured rat astrocytes, 123(September 2018). https://doi.org/10.1016/j.cyto.2019.154774
Krishnasamy, S., Weng, Y., Thammisetty, S. S., Phaneuf, D., Lalancette-hebert, M., & Kriz, J. (2017). Molecular imaging of nestin in neuroinflammatory conditions reveals marked signal induction in activated microglia, 1–14. https://doi.org/10.1186/s12974-017-0816-7
Liu, H., Zhang, J., Xu, X., Lu, S., Yang, D., Xie, C., & Jia, M. (2021). SARM1 promotes neuroinflammation and inhibits neural regeneration after spinal cord injury through NF- κ B signaling. Theranostics, 11(9). https://doi.org/10.7150/thno.49054
Li, S., Wang, N., Zhang, T., Feng, Y., Wang, L., & Sun, J. (2020). Characterization of three connexin32 genes and their role in inflammation-induced ATP release in the Japanese flounder Paralichthys olivaceus. Fish and Shellfish Immunology, 106(August), 181–189. https://doi.org/10.1016/j.fsi.2020.07.066
Lai, Y., Tao, L., Zhao, Y., & Zhang, X. (2017). Cx32 inhibits TNF α -induced extrinsic apoptosis with and without EGFR suppression, 2885–2892. https://doi.org/10.3892/or.2017.5950
Rochfort, K. D., & Cummins, P. M. (2015). Cytokine-mediated dysregulation of zonula occludens-1 properties in human brain microvascular endothelium. Microvascular Research, 100, 48–53. https://doi.org/10.1016/j.mvr.2015.04.010
Wang, L., Zhang, R., Chen, J., Wu, Q., & Kuang, Z. (2017). Baicalin protects against TNF-α-induced Injury by down-regulating miR-191a that targets the tight junction protein ZO-1 in IEC-6 cells. Biological and Pharmaceutical Bulletin, 40(4), 435–443. https://doi.org/10.1248/bpb.b16-00789
Jovinge, S., & Hultgårdh-Nilsson, A., Regnström, J., & Nilsson, J. (1997). Tumor necrosis factor-α activates smooth muscle cell migration in culture and is expressed in the balloon-injured rat aorta. Arteriosclerosis, Thrombosis, and Vascular Biology, 17(3), 490–497. https://doi.org/10.1161/01.ATV.17.3.490
Strien, M. E. van, John J. P. Breve´ 1, S., Fratantoni, S., Schreurs, M. W. J., Bol, J. G. J. M., Strien, M. E. Van, … Dam, A. Van. (2011). Astrocyte-derived tissue transglutaminase ınteracts with fibronectin : A role in astrocyte adhesion and migration ?, 6(9). https://doi.org/10.1371/journal.pone.0025037
Likhitpanichkul, M., Torre, O. M., Gruen, J., Walter, B. A., Hecht, A. C., & Iatridis, J. C. (2017). Do mechanical strain and TNF-α ınteract to amplify pro- ınflammatory cytokine production in human annulus fibrosus Cells?, 49(7), 1214–1220. https://doi.org/10.1016/j.jbiomech.2016.02.029.Do
Pai, S. G., Carneiro, B. A., Mota, J. M., Costa, R., Leite, C. A., Barroso-sousa, R., … Giles, F. J. (2017). Wnt / beta-catenin pathway : modulating anticancer immune response, 1, 1–12. https://doi.org/10.1186/s13045-017-0471-6
Habib, M. Z., Ebeid, M. A., Faramawy, Y., Saad, S. T., Magdoub, H. M. El, Attia, A. A., … Abdel-tawab, A. M. (2020). Effects of lithium on cytokine neuro-inflammatory mediators, Wnt/β-catenin signaling and microglial activation in the hippocampus. Toxicology and Applied Pharmacology. Elsevier Inc. https://doi.org/10.1016/j.taap.2020.115073
Jang, J., Jung, Y., Chae, S., Chung, S., Kim, S., & Yoon, Y. (2017). Biochemical and biophysical research communications WNT / b -catenin pathway modulates the TNF- a -induced in fl ammatory response in bronchial epithelial cells. Biochemical and Biophysical Research Communications, 484(2), 442–449. https://doi.org/10.1016/j.bbrc.2017.01.156
Inyoo, S., Suttitheptumrong, A., & Pattanakitsakul, S. (2017). Synergistic effect of TNF- a and dengue virus ınfection on adhesion molecule reorganization in human endothelial cells, 186–191. https://doi.org/10.7883/yoken.JJID.2016.123
Kamianowska, M., & Szczepa, M. (2011). Effects of erythropoietin on ICAM ‐ 1 and PECAM ‐ 1 expressions on human umbilical vein endothelial cells subjected to oxidative stress, (April). https://doi.org/10.1002/cbf.1768
Li, J., Tan, M., Xiang, Q., Zhou, Z., & Yan, H. (2017). Thrombin-activated platelet-derived exosomes regulate endothelial cell expression of ICAM-1 via microRNA-223 during the thrombosis-in fl ammation response. Thrombosis Research, 154, 96–105. https://doi.org/10.1016/j.thromres.2017.04.016
Hade, M. D., Suire, C. N., & Suo, Z. (2021). Mesenchymal stem cell-derived exosomes: Applications in regenerative medicine. Cells, 10(8), 1–48. https://doi.org/10.3390/cells10081959
Chaput, N., Schartz, N. E. C., André, F., Taïeb, J., Novault, S., Bonnaventure, P., … Zitvogel, L. (2004). Exosomes as potent cell-free peptide-based vaccine. II. Exosomes in CpG adjuvants efficiently prime naive Tc1 lymphocytes leading to tumor rejection. The Journal of Immunology, 172(4), 2137–2146. https://doi.org/10.4049/jimmunol.172.4.2137
Lai, R. C., Yeo, R. W. Y., Tan, K. H., & Lim, S. K. (2013). Exosomes for drug delivery - A novel application for the mesenchymal stem cell. Biotechnology Advances, 31(5), 543–551. https://doi.org/10.1016/j.biotechadv.2012.08.008
Spitz, S., Bolognin, S., Brandauer, K., Füßl, J., Schuller, P., & Schobesberger, S. (2022). Development of a multi-sensor integrated midbrain organoid-on- a-chip platform for studying Parkinson’s disease, (August). https://doi.org/10.1101/2022.08.19.504522
Huang, Q., Tang, B., Romero, J. C., Yang, Y., Elsayed, S. K., Pahapale, G., … Gracias, D. H. (2022). Shell microelectrode arrays (MEAs) for brain organoids. Science Advances, 8(33). https://doi.org/10.1126/sciadv.abq5031
Kabay, G., Manz, A., & Dincer, C. (2022). Microfluidic roadmap for translational nanotheranostics. Small Methods, 6(2). https://doi.org/10.1002/smtd.202101217
Acknowledgements
Financial support provided by The Scientific and Technological Research Council of Turkey (TUBITAK) under grant number 119M578 is highly appreciated. P.S-M. gratefully acknowledges the TUBITAK 2211-A National Graduate Scholarship Program and 2214-A International Doctoral Research Fellowship Program. E.D. acknowledges 2210-C National Graduate Scholarship Program. We also acknowledge Finnadvance Company for providing microfluidic chip platforms.
Author information
Authors and Affiliations
Contributions
Conceptualization: P.S-M., E.D. and O.Y-C.; Writing – Original Draft Preparation: P.S-M., E.D. and L.S.; Writing – Review & Editing: C.B-A., O.Y.C. and also P.S-M.; Supervision and Funding Acquisition: O.Y-C. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing Interest
The authors declare no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Saglam-Metiner, P., Duran, E., Sabour-Takanlou, L. et al. Differentiation of Neurons, Astrocytes, Oligodendrocytes and Microglia From Human Induced Pluripotent Stem Cells to Form Neural Tissue-On-Chip: A Neuroinflammation Model to Evaluate the Therapeutic Potential of Extracellular Vesicles Derived from Mesenchymal Stem Cells. Stem Cell Rev and Rep 20, 413–436 (2024). https://doi.org/10.1007/s12015-023-10645-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-023-10645-8