Abstract
Objective
Amyotrophic lateral sclerosis (ALS) is still incurable. Although different therapies can affect the health and survival of patients. Our aim is to evaluate the effect of umbilical mesenchymal stem cells administrated intrathecally to patients with amyotrophic lateral sclerosis on disability development and survival.
Methods
This case-control study involved 67 patients treated with Wharton’s jelly mesenchymal stem cells (WJ-MSC). The treated patients were paired with 67 reference patients from the PRO-ACT database which contains patient records from 23 ALS clinical studies (phase 2/3). Patients in the treatment and reference groups were fully matched in terms of race, sex, onset of symptoms (bulbar/spinal), FT9 disease stage at the beginning of therapy and concomitant amyotrophic lateral sclerosis medications. Progression rates prior to treatment varied within a range of ± 0.5 points. All patients received three intrathecal injections of Wharton’s jelly-derived mesenchymal stem cells every two months at a dose of 30 × 106 cells. Patients were assessed using the ALSFRS-R scale. Survival times were followed-up until March 2020.
Results
Median survival time increased two-fold in all groups. In terms of progression, three response types measured in ALSFRS-R were observed: decreased progression rate (n = 21, 31.3%), no change in progression rate (n = 33, 49.3%) and increased progression rate (n = 13, 19.4%). Risk-benefit ratios were favorable in all groups. No serious adverse drug reactions were observed.
Interpretation
Wharton’s jelly-derived mesenchymal stem cells therapy is safe and effective in some ALS patients, regardless of the clinical features and demographic factors excluding sex. The female sex and a good therapeutic response to the first administration are significant predictors of efficacy following further administrations.

Medical therapeutic experiment with retrospective case-control analyses
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is no causal therapy for amyotrophic lateral sclerosis (ALS) – a rare, fatal, progressive disease that has been rapidly increasing [1] and occurs de novo in 90% [2]. The studies using iPSC-derived motor neurons revealed the complicated molecular nature of this disease related to mitochondrial dysfunction and ER stress, NF aggregate formation, hyperexcitability, and channel deficits [3]. There is still only one approved drug in Europe – riluzole, which extends survival by 3 months on average. No new drugs have been registered for this indication since 1994 [4], partly due to our incomplete understanding of the complex pathogenesis of motor neuron degeneration [5]. Recently, another drug, edaravone, has been registered in Japan and the USA. There is therefore still a huge unmet need for a treatment that could effectively alter the progression rate of this debilitating disease.
Although it is well known that MSC differentiate into neural cells and neuroglia [6], over the course of the last several years stem/stromal cell therapy was proposed for treating ALS based on small observational studies. Evidence from preclinical studies conducted with the animal ALS (SOD1) model provided promising results and led to the initiation of some clinical studies- [7,8,9], Previously, the safety and efficacy of mesenchymal stem cells (MSC) administration was described in small studies which did not evaluate overall survival. The aim of our study was to evaluate the effect of compassionate use of Wharton’s jelly-derived mesenchymal stem cells (WJ-MSC) in terms of progression and survival in ALS patients. This was done in the form of a medical therapeutic experiment (described elsewhere [10]) with retrospective case-control analyses.
Materials and Methods
Patients
The study was conducted at Instytut Terapii Komórkowych S.A. in Olsztyn, Poland (Cell Therapies Institute, FamiCord Group) in cooperation with the Departments of Neurology and Neurosurgery, School of Medicine, Collegium Medicum of the University of Warmia and Mazury in Olsztyn, Poland. The treatment was reviewed by the Ethics Committee of the School of Medicine, University of Warmia and Mazury in Olsztyn, Poland and performed in accordance with the Declaration of Helsinki. Prior to starting the experiment, all patients signed an informed consent form. Patients enrolled into the study were recruited between 2015 and 2018. Enrolled patients met the following profile: clinical diagnosis of definite ALS based on the El Escorial World Federation of Neurology criteria [11], ventilatory independence, age 20–78 years and the ability to attend clinic visits alone or with support. The following laboratory tests were mandatory: C-reactive protein (CRP), sodium, potassium, glucose, blood cell count, coagulation, urea and creatinine.
MSCs Harvesting and Processing
WJ-MSCs were donated from healthy newborns following maternal qualification based on a medical questionnaire conducted after the parents signed an informed consent form. The harvested umbilical cords were transported to the laboratory under monitored conditions and processed within 48 h of delivery. Once disinfected, they were dissected, stripped of any blood vessels and minced into 2 cm3 pieces, which were placed into 6-well plates. The whole procedure was conducted without the use of enzymes. Tissue explants were cultured and incubated at 37 °C in 5% CO2 in air. After 1–2 h, nonadherent cells were washed off and any adherent cells were further expanded. The tissue explants were removed after 2–3 weeks of culture. When the adherent cells reached 90% confluence, they were passaged and reseeded for further expansion at 1.2 × 104 cells/cm2 a 75 cm2 tissue culture flask (BD). To evaluate their numbers, cells were detached and counted in a hemocytometer. After reaching a sufficient number of cells, they were immunophenotyped, cryopreserved and stored in liquid nitrogen vapor.
The cells fulfilled the criteria described by Dominici et al. [12] Briefly, the cells were detached from the plate using a trypsin solution upon reaching 60–80% confluence. In preparation for flow cytometry, they were incubated (30 min in the dark) with fluorochrome-conjugated antibodies against MSC-negative surface markers (CD34 FITC, CD14 FITC, CD19 FITC, CD45 FITC and HLA-DR FITC) and MSC-positive surface markers (CD73 PE, CD90 PE, CD105 PE and HLA ABC FITC). Next, the cells were washed, resuspended in Cell Fix solution, and analyzed in a BD FACSCalibur cytometer. Murine anti-IgG1 FITC and anti-IgG1 PE were used as controls. Before administration to the patients, the cells were thawed in a 37 °C water bath. Cell viability was determined with the trypan blue dye exclusion test, based on a thawed reference sample. We did not monitor the proliferation rate or any other indicator of cellular senescence. Patients received only early-passage cells (at the fifth passage or less). The unit volume, number, vitality and morphology of the cells, microbiological purity, results of the serological tests, absence of endotoxins, and immunophenotype of the cells in the finished product adhered to the specifications of the Chief Pharmaceutical Inspectorate.
Reference Group
Reference subjects were obtained from the PRO-ACT database (www.nctu.partners.org/proact). This database contains more than 10,000 patient records from 23 different clinical studies (phase 2/3) and it has been used earlier also by another authors as a reference data set [13, 14]. Each patient was paired with a reference subject, fully matched in terms of race, sex, disease stage (assessed with the FT9 scale), treatment, onset symptoms (bulbar/spinal). Patients with fast progression were identified based on an ALSFRS-R score Loss of >1 point per month and slow progression was defined as <1 point/month [15]. Age differences in 52 of 67 patients (77.6%) were within ± 5 years and in 63 of 67 (94.0%) were within ± 10 years (Supplementary Fig. 1). In terms of progression rates 65 of 67 Pairs (97.0%) were matched within the range ± 0.3 point/month and no patient exceeded 0.5 point/month (Table 1). In 45 patients (67.2%) the difference equaled zero (Supplementary Fig. 2)
ALSFRS-R and Fine’til 9 Scales
ALSFRS-R is the revised (R) functional rating scale for patients with ALS. The basic version assesses the functions of speech, swallowing, self-care and patient mobility [16, 17]. There are 12 questions in the scale, with separate additional items concerning cutting food (for patients with or without gastrostomy). Answers correspond to scores from 0 to 4, where 0 is the largest possible deficit in a given area (e.g. loss of useful speech) and 4 corresponds to lack of any deficit (e.g. normal speech processes). The total score ranges from 0 to 48 points.
FT9 is based on the ALSFRS-R and was described as a tool enabling stratification of patients at various ALS stages [18]. This approach defines 5 disease stages - from 1 to 5 (FT9–1 to FT9–5). Stage 1 means the initial stage (minimally involved) and 5 denotes the most advanced stage of the disease. There are 4 main domains in the ALSFRS-R score (bulbar, upper limb, lower limb, breathing). All 4 domains include 3 separate questions, with a maximum of 4 points to be assigned for each and a maximum total of 12 points for each domain. If a patient receives less than 9 points in one of the 4 main domains, they are staged as FT9–2, and if 2 domains receive less than 9 points – as FT9–3 etc. Patients staged as FT9–1 have not received less than 9 points total in any of the ALSFRS-R domains.
Administration Procedure
MSCs were administered intrathecally. Following a typical lumbar puncture, 2 mL of CSF was collected and the same volume of WJ-MSC suspension in 1 mL 5% human albumin was administered via a needle inserted at the L3/L4 level with the patient in the supine or sitting position. Patients received three MSCs administrations at 2-month intervals, following the same procedure each time. All patients received a WJ-MSC dose of 30 × 106 cells at each injection.
Clinical Evaluation
Clinical evaluation during the study involved physical and neurological examination at each MSCs administration visit. ASLFRS-R assessments were also performed at each administration visit. Additionally, to assess the rate of disability progression, a retrospective ALSFRS-R clinical assessment was performed, covering the six months prior to study entry. The average monthly ASLFRS score was calculated for each patient separately for the pre-treatment and treatment periods. Upon enrollment all patients were stratified according to FT9 level.
Decreased progression rate was defined as a difference of >3 points in the ALSFRS-R between treated vs. reference patients. No change in progression rate (lack of response) was defined as a difference within <3 points and > −3 in the ALSFRS-R. Increased progression rate was defined as a difference of <−3 points in the ALSFRS-R.
Survival Time Analysis
Survival was assessed since the enrollment. Data were obtained by the investigator via telephone and e-mail. At times the patient’s families informed the investigators themselves about the patient’s death. The last survival data update is from March 2020. Statistical methods used for survival analysis are described in the next paragraph.
Statistical Analysis
Patients who received at least three MSCs injections and were assessed at each administration visit were included into this analysis. In addition, the average monthly score decrease rate for the period before and during treatment was calculated. Microsoft Excel and Statistica 13 (TIBCO Software Inc.) were used to perform the analysis. To assess the significance of the difference between the predicted and observed values, the Wilcoxon signed-rank test was used. The association between categorized progression rates (fast/slow) and sex or ALS type was assed using the chi-square test. Survival analysis was performed using a Cox proportional hazard ratio and Kaplan-Meyer curves compared in log-rank and Cox-Mantel tests. In addition, linear and logistic regression, as well as discriminant analysis were performed to identify clinical response type predictive factors. In all cases, 0.05 was defined as the significance level. Statistical analysis was performed in the whole study population as well as in subgroups categorized on the basis of the clinical response and initial clinical and demographic characteristics. The power of the survival analysis indicated that difference in survival rate that we observed at the end of the observation (approx. 40% vs 0%) allows to achieve 90% statistical power in the sample size 11 person per one group (22 persons in the whole study population). In case of 67 patients per group, the statistical power for such proportions equals 100% (Supplementary Fig. 3).
Results
MSCs Treatment Extends Survival in ALS Patients
In the entire study population, the risk of death was decreased in patients treated with MSCs versus the paired control group by 70% (HR 0.30 [95% CI 0.16 to 0.59], p = 0.0004). Median overall survival was almost twice longer in MSC patients than in the reference group (1183 days vs. 640 days, p = 0.002). A similar effect on survival was observed in patients with lower disability at study entry (FT9, 1–2 stage) (p = 0.03), as well as for patients with higher disability at study entry (FT9, 3–5; p = 0.03) (Fig. 1). In the subgroup with decreased progression rate the difference was 1193 days vs. 568 days (p < 0.05 in all five tests) and in the subgroup with no change in progression rate it was 994 days vs. 580 days (p < 0.05 in the Cox-Mantel test). Kaplan-Meier curves for overall survival are presented in Fig. 1.
MSCs Reduce ALS Progression Rates
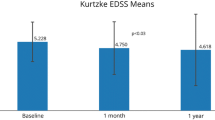
In the whole study population, monthly score reduction (Fig. 2) during therapy was lower than prior to therapy (p = 0.008). From the total of 67 treated patients, 21 presented decrease in progression rate from the ALSFS-R evaluation vs. reference patients who progressed faster, 33 presented no difference in progression rate vs. reference patients, and 13 presented increase in progression rate when compared to the reference patients who progressed slower. These results were consistent with the linear regression analysis that revealed a significant (p = 0.0003) and strong (beta = −0.54, SE 0.15) effect of the MSC treatment. A subgroup analysis indicated that the risk-benefit ratio was favorable for patients who experienced decreased progression rate in all subgroups based on the initial patient characteristics (Table 2).
Early Response Predicts the Final Outcome of MSC Treatment
Discriminant analysis nor logistic regression allowed to identify no single demographic or clinical factor that would be a significant predictor for the type of response; the whole model consisting of these factors was also not significant. We found that following the first MSCs administration ALS patients with a better response in the ALSFRS-R versus reference patients also achieved a better final outcome, defined as a higher probability of having a better ALSFRS-R score after 6 months of MSC treatment. The estimate for effect exerted by the first dose response on the final outcome was at −0.33 (95% CI −0.58 to −0.1, p = 0.0059) in the logistic regression. The values for each ALSFRS-R score difference are presented in Table 3.
Safety
None of the patients from the analyzed group treated with MSCs experienced any serious adverse events related to the cell administration. One patient presented signs of post lumbar puncture syndrome, such as nausea and headache within 1 day following the injection. Four patients suffered from the same syndrome one week following the injection. Two cases of a temperature above 37 degrees Celsius were also reported. Signs of the PLP syndrome were however short-lived and resolved without any complications. No new or unexpected reactions following the lumber puncture and MSCs administration were observed. During the two months following MSCs administration none of the patients reported any unexpected symptoms apart from their ALS. No meningeal signs were detected. No malignancies were reported in the follow-up period.
Discussion
In her March 2020 JAMA Neurology publication, Vijayaraghavan highlighted the problem of limited access to clinical studies for patients with ALS. She described the case of her husband, a 38-years-old neuroscientist suffering from rapidly progressing ALS who – after being excluded from a clinical study – received stem cell therapy when it was already too late (due to the lengthy process of application for extended access) and died [19]. Without calling into the obvious objections related to unproven therapies based on stromal vascular fraction (SVF) [20, 21] or ill-defined “stem cells” [22] (http://ema.europa.eu/en/human-regulatory/overview/advanced-therapy-medicinal-products-overview, https://www.fda.gov/consumers/consumer-updates/fda-warns-about-stem-cell-therapies) administered by clinicians without the proper background or even by persons without a medical license [23], this case clearly shows that there are risks attached not only to action, but also to omission. Not every unregistered therapy should be considered unproven [24]. In the European Union, the Regulation 1394/2007 and national regulations passed under the 2001/83/EC Directive approve compassionate use of unregistered advanced therapy medicinal products manufactured under Good Manufacturing Practice. This is done as part of a Hospital Exemption subject to the approval of an ethics committee. Our results were obtained within this legal framework.
Our study yielded highly encouraging results when it comes to WJ-MSC administration in all subgroups distinguished based on demographical and clinical factors. For comparison, riluzole studies showed a survival slope change only in patients with the bulbar disease. This drug has been approved for ALS in 1994 [4], although it extends the life expectancy only by approximately 3 months. In 2017, a new medication, edaravone, was registered in the USA. We showed that WJ-MSC therapy extends survival to a comparable extent (HR 0.30 in our study vs. 0.33 for edaravone [25]). Our results confirm the previously published studies that reported on the safety and/or efficacy of MSC administration in patients with ALS in smaller groups [26,27,28,29,30,31,32,33,34,35,36], but we are the first to present a survival analysis in such a large patient population.
In 2019, the FDA [37] and a group of experts [38] published guidelines on the conduct of ALS clinical studies, with a goal of exploring its clinical and genetic biomarkers. Therefore, apart from reporting general efficacy, an important question, especially when considered that therapy was financed by the patients themselves or charities, regarded the prediction of response to MSC treatment. Our research indicated that the female sex and a positive clinical response (decreased progression rate) to the first MSC administration when compared to the strictly matched reference patient is a significant predictor for overall efficacy of the treatment. We would like to propose this tool for clinicians to allow them to obtain more informed consent, accordingly to the recent suggestions [39,40,41].
The results of this study are encouraging, however several limitations must be stressed. The case-control study is well established in the evidence-based hierarchy as better than case series, but weaker than randomized, double-blind, controlled studies. The case-control design assumes equality of the groups and the selection of a single control for each patient. Such selection may be fraught with a selection bias. In a group with 67 pairs we may expect this bias to affect all subgroups, but the reader must bear in mind that coincidence cannot be excluded; this refers to both patients who progressed slower and faster after administration. For this reason, a more beneficial avenue to be pursued for clinical use may be comparing the treated patient with the group of all reference subjects matching the criteria, which was not possible in this analysis due to the case-control design, which requires an equal number of patients. Secondly, the cut-off for the ALSFRS-R functional assessment follow-up period was 6 months following last administration. This was due to the fact that in the reference group the observation period rarely exceeded 12 months, out of which 6 months were used in this analysis as the comparison to the pre-treatment period. Assessment of the clinical response persistence in patients who experienced decreased progression rate was therefore based on linear regression modelling. Thirdly, we did not control genetic factors which may influence survival even in patients with sporadic ALS [42], thus we cannot exclude that the reason for the observed improvement is genetic mismatch, especially since as much as 50% of the variance in ALS has a genetic background [43].
Our study did not investigate the mechanisms involved in clinical improvement. The suggested role of natural killer cells [44] and regulatory T cells [45, 46] is in line with the mechanism of action of MSC described by other authors [47,48,49,50]. Some studies indicated that human neural stem cells transplanted into a spinal cord in patients with ALS differentiated into neurons which were still detected 2.5 years after administration; however, it is not known whether the same happens after administration of MSC [51]. Future studies should combine survival and molecular analyses. Suggested predictors include neutrophils and CD4 T cells [52], Serum Retinol-Binding Protein 4 [53], C-reactive protein [54] and 233 differential expressed genes in ALS monocytes, especially those related to inflammation (IL1B, IL8, FOSB, CXCL1, CXCL2) [55]. Nevertheless genetic testing is unfortunately still limited, even in clinical studies. Moreover, further studies into the factors related to donor selection, dosage and dosing schemes may be opportunities to achieve even better results.
Keeping in mind the study limitation, our results suggest that treatment with MSC substantially reduces the rate of progression and yields a twofold extension of survival in those who achieved a positive response to the first administration in comparison to the reference subject. These HR values were even better than those achieved with the registered drug, edaravone. Demographic factors have a certain impact on the risk-benefit ratio, so they should be discussed with the patient before the start of therapy. MSC administration was absolutely safe. Eligibility for the treatment should be confirmed following first administration based on the progression rate in comparison with at least one reference subject (more would be beneficial). Future studies should focus on confirming these observations in double-blind, controlled studies, optimally with a three-arm design to investigate additive or synergic effects with edaravone.
References
Chiò, A., Mora, G., Moglia, C., Manera, U., Canosa, A., Cammarosano, S., Ilardi, A., Bertuzzo, D., Bersano, E., Cugnasco, P., Grassano, M., Pisano, F., Mazzini, L., Calvo, A., & for the Piemonte and Valle d’Aosta Register for ALS (PARALS). (2017). Secular trends of amyotrophic lateral sclerosis: The Piemonte and Valle d’Aosta register. JAMA Neurology, 74(9), 1097–1104.
Liu, G., David, B. T., Trawczynski, M., & Fessler, R. G. (2020). Advances in pluripotent stem cells: History, mechanisms, technologies, and applications. Stem Cell Reviews and Reports, 16, 3–32.
Zhao, A., Pan, Y., & Cai, S. (2020). Patient-specific cells for modeling and decoding amyotrophic lateral sclerosis: Advances and challenges. Stem Cell Reviews and Reports, 16, 482–502.
Bensimon, G., Lacomblez, L., & Meininger, V. (1994). A controlled trial of riluzole in amyotrophic lateral sclerosis. ALS/Riluzole study group. The New England Journal of Medicine, 330(9), 585–591.
Chen, H. K. S., Sakowski, S. A., & Feldman, E. L. (2016). Intraspinal stem cell transplantation for amyotrophic lateral sclerosis. Annals of Neurology, 3, 342–353.
George, S., Hamblin, M. R., & Abrahamse, H. (2019). Differentiation of Mesenchymal stem cells to neuroglia: In the context of cell Signalling. Stem Cell Reviews and Reports, 15, 814–826.
Zhao, C. P., Zhang, C., Zhouet, S.-N., et al. (2007). Human mesenchymal stromal cells ameliorate the phenotype of SOD1-G93A ALS mice. Cytotherapy, 9(5), 414–426.
Zhang, C., Zhou, C., Teng, J.-J., Zhao, R. L., Song, Y. Q., & Zhang, C. (2009). Multiple administrations of human marrow stromal cells through cerebrospinal fluid prolong survival in a transgenic mouse model of amyotrophic lateral sclerosis. Cytotherapy, 11(3), 299–306.
Marconi, S., Bonaconsa, M., Scambi, I., Squintani, G. M., Rui, W., Turano, E., Ungaro, D., D’Agostino, S., Barbieri, F., Angiari, S., Farinazzo, A., Constantin, G., del Carro, U., Bonetti, B., & Mariotti, R. (2013). Systemic treatment with adipose-derived mesenchymal stem cells ameliorates clinical and pathological features in the amyotrophic lateral sclerosis murine model. Neuroscience, 248, 333–343.
Boruczkowski, D., & Zdolińska-Malinowska, I. (2019). A retrospective analysis of safety and efficacy of Wharton’s jelly stem cell Administration in Children with Spina bifida. Stem Cell Reviews and Reports, 15, 717–729.
El Brooks, B. R. (1994). Escorial world federation of neurology criteria for the diagnosis of amyotrophic lateral sclerosis. Subcommittee on motor neuron diseases/amyotrophic lateral sclerosis of the world federation of neurology research group on neuromuscular diseases and the El Escorial "Clinical limits of amyotrophic lateral sclerosis" workshop contributors. Journal of the Neurological Sciences, 124, 96–107.
Dominici, M., le Blanc, K., Mueller, I., et al. (2006). Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy, 8(4), 315–317.
Goutman, S. A., Brown, M. B., Glass, J. D., Boulis, N. M., Johe, K., Hazel, T., Cudkowicz, M., Atassi, N., Borges, L., Patil, P. G., Sakowski, S. A., & Feldman, E. L. (2018). Long-term phase 1/2 intraspinal stem cell transplantation outcomes in ALS. Annals of Clinical Translational Neurology, 5(6), 730–740.
Taylor, A. A., Fournier, C., Polak, M., Wang, L., Zach, N., Keymer, M., Glass, J. D., Ennist, D. L., & The Pooled Resource Open-Access ALS Clinical Trials Consortium. (2016). Predicting disease progression in amyotrophic lateral sclerosis. Annals of Clinical Translational Neurology, 3(11), 866–875.
Siwek, T., Barczewska, M., Grabarczyk, L., et al. (2018). Mesenchymal stem cell (MSC) transplantation in patients with amyotrophic lateral sclerosis (ALS): Is there a “responder population”? Journal of Neurology and Neuroscience, 9(3), 260.
Miano, B., Stoddard, G. J., Davis, S., et al. (2004). Inter-evaluator reliability of the ALS functional rating scale. Amyotrophic Lateral Sclerosis and Other Motor Neuron Disorders, 5(4), 235–239.
Gordon, P.H., Miller, R.G., Moore. D.H. ALSFRS-R. Amyotroph Lateral Scler Other Motor Neuron Disord 5(Suppl 1), 90–3 (2004).
Thakore, N. J., Lapin, B. R., Kinzy, T. G., & Pioro, E. P. (2018). Deconstructing progression of amyotrophic lateral sclerosis in stages: A Markov modeling approach. Amyotroph Lateral Scler Frontotemporal Degener, 19(7–8), 483–494.
Vijayaraghavan, M. (2020). Improving access to clinical trials for amyotrophic lateral sclerosis treatment. JAMA Neurology, 77, 671. https://doi.org/10.1001/jamaneurol.2020.0421.
Voelker, R. (2018). Crackdown on stem cell product. JAMA, 319(7), 649.
Voelker, R. (2019). Another stem cell company is put on notice. JAMA., 322(1), 19.
The Australian Stem Cell Handbook (2015) http://www.stemcellsaustralia.edu.au/AboutUs/Document-Library.aspx
Fu, W., Smith, C., Turner, L., Fojtik, J., et al. (2019). Characteristics and Scope of Training of Clinicians Participating in the US Direct-to-Consumer Marketplace for Unproven Stem Cell Interventions. JAMA., 321(24), 2463–2464.
Cossu, G., Birchall, M., Brown, T., de Coppi, P., Culme-Seymour, E., Gibbon, S., Hitchcock, J., Mason, C., Montgomery, J., Morris, S., Muntoni, F., Napier, D., Owji, N., Prasad, A., Round, J., Saprai, P., Stilgoe, J., Thrasher, A., & Wilson, J. (2018). Lancet commission: Stem cells and regenerative medicine. The Lancet Commissions, 391(10123), 883–910.
Okada, M., Yamashita, S., Ueyama, H., Ishizaki, M., Maeda, Y., & Ando, Y. (2018). Long-term effects of edaravone on survival of patients with amyotrophic lateral sclerosis. eNeurologicalSci, 11, 11–14.
Karussis, D., Karageorgiou, C., Vaknin-Dembinsky, A., Gowda-Kurkalli, B., Gomori, J. M., Kassis, I., Bulte, J. W., Petrou, P., Ben-Hur, T., Abramsky, O., & Slavin, S. (2010). Safety and immunological effects of Mesenchymal stem cell transplantation in patients with multiple sclerosis and amyotrophic lateral sclerosis. Archives of Neurology, 67(10), 1187–1194.
Mazzini, L., Ferrero, I., Luparello, V., Rustichelli, D., Gunetti, M., Mareschi, K., Testa, L., Stecco, A., Tarletti, R., Miglioretti, M., Fava, E., Nasuelli, N., Cisari, C., Massara, M., Vercelli, R., Oggioni, G. D., Carriero, A., Cantello, R., Monaco, F., & Fagioli, F. (2010). Mesenchymal stem cell transplantation in amyotrophic lateral sclerosis: A phase I clinical trial. Experimental Neurology, 223(1), 229–237.
Mazzini, L., Mareschi, K., Ferrero, I., Miglioretti, M., Stecco, A., Servo, S., Carriero, A., Monaco, F., & Fagioli, F. (2012). Mesenchymal stromal cell transplantation in amyotrophic lateral sclerosis: A long-term safety study. Cytotherapy, 14(1), 56–60.
Prabhakar, S., Marwaha, N., Lal, V., et al. (2012). Autologous bone marrow-derived stem cells in amyotrophic lateral sclerosis: A pilot study. Neurology India, 60(5), 465–469.
Oh, K. W., Moon, C., Kim, H. Y., Oh, S. I., Park, J., Lee, J. H., Chang, I. Y., Kim, K. S., & Kim, S. H. (2015). Phase I trial of repeated intrathecal autologous bone marrow-derived mesenchymal stromal cells in amyotrophic lateral sclerosis. Stem Cells Translational Medicine, 4(6), 590–597.
Zhang, R., Chen, H., Zheng, Z., et al. (2015). Umbilical cord-derived mesenchymal stem cell therapy for neurological disorders via inhibition of mitogen-activated protein kinase pathway-mediated apoptosis. Molecular Medicine Reports, 11(3), 1807–1812.
Petrou, P., Gothelf, Y., Argov, Z., Gotkine, M., Levy, Y. S., Kassis, I., Vaknin-Dembinsky, A., Ben-Hur, T., Offen, D., Abramsky, O., Melamed, E., & Karussis, D. (2016). Safety and clinical effects of Mesenchymal stem cells secreting Neurotrophic factor transplantation in patients with amyotrophic lateral sclerosis: Results of phase 1/2 and 2a clinical trials. JAMA Neurology, 73(3), 337–344.
Staff, N.P, Madigan, N. N., Morris, J., et al. (2016). Safety of intrathecal autologous adipose-derived mesenchymal stromal cells in patients with ALS. Neurology., 87(21), 2230–2234.
Sykova, E., Rychmach, P., Drahorádová, I., et al. (2017). Transplantation of Mesenchymal stromal cells in patients with amyotrophic lateral sclerosis: Results of phase I/IIa clinical trial. Cell Transplantation, 26(4), 647–658.
Barczewska, M., Grudniak, M., Maksymowicz, S., Siwek, T., Ołdak, T., Jezierska-Woźniak, K., Gładysz, D., & Maksymowicz, W. (2019). Safety of intrathecal injection of Wharton's jelly-derived mesenchymal stem cells in amyotrophic lateral sclerosis therapy. Neural Regeneration Research, 14(2), 313–318.
US Department of Health and Human Services Food and Drug Administration. Amyotrophic lateral sclerosis: developing drugs for treatment guidance for industry. Published September 2019. Accessed May 8, 2020. https://www.fda.gov/media/130964/download
Oh, K.-W., Noh, M.-Y., Kwon, M.-S., Kim, H. Y., Oh, S. I., Park, J., Kim, H. J., Ki, C. S., & Kim, S. H. (2018). Repeated Intrathecal Mesenchymal stem cells for amyotrophic lateral sclerosis. Annals of Neurology, 84(3), 361–373.
van den Berg, L. H., Sorenson, E., Gronseth, G., et al. (2019). Airlie house ALS clinical trials guidelines group. Revised Airlie House consensus guidelines for design and implementation of ALS clinical trials. Neurology., 92(14), e1610–e1623.
Bowman, M., Racke, M., Kissel, J., & Imitola, J. (2015). Responsibilities of health care professionals in counseling and educating patients with incurable neurological diseases regarding “stem cell tourism”: Caveat emptor. JAMA Neurology, 72(11), 1342–1345.
Bowman, M., Racke, M., Kissel, J., & Imitola, J. (2015). Responsibilities of health care professionals in counseling and educating patients with incurable neurological diseases regarding “stem cell tourism.”. JAMA Neurology, 72(11), 1342–1345.
Sugarman, J., Barker, R. A., & Charo, R. A. (2019). A professional standard for informed consent for stem cell therapies. JAMA., 322(17), 1651–1652.
Fogh, I., Lin, K., Tiloca, C., Rooney, J., Gellera, C., Diekstra, F. P., Ratti, A., Shatunov, A., van Es, M. A., Proitsi, P., Jones, A., Sproviero, W., Chiò, A., McLaughlin, R. L., Sorarù, G., Corrado, L., Stahl, D., del Bo, R., Cereda, C., Castellotti, B., Glass, J. D., Newhouse, S., Dobson, R., Smith, B. N., Topp, S., van Rheenen, W., Meininger, V., Melki, J., Morrison, K. E., Shaw, P. J., Leigh, P. N., Andersen, P. M., Comi, G. P., Ticozzi, N., Mazzini, L., D’Alfonso, S., Traynor, B. J., van Damme, P., Robberecht, W., Brown, R. H., Landers, J. E., Hardiman, O., Lewis, C. M., van den Berg, L. H., Shaw, C. E., Veldink, J. H., Silani, V., al-Chalabi, A., & Powell, J. (2016). Association of a Locus in the CAMTA1 gene with survival in patients with sporadic amyotrophic lateral sclerosis. JAMA Neurology, 73(7), 812–820.
Ryan, M., Heverin, M., McLaughlin, R. L., & Hardiman, O. (2019). Lifetime risk and heritability of amyotrophic lateral sclerosis. JAMA Neurology, 76(11), 1367–1374.
Garofalo, S., Cocozza, G., Porzia, A., Inghilleri, M., Raspa, M., Scavizzi, F., Aronica, E., Bernardini, G., Peng, L., Ransohoff, R. M., Santoni, A., & Limatola, C. (2020). Natural killer cells modulate motor neuron-immune cell cross talk in models of amyotrophic lateral sclerosis. Nature Communications, 11, 1773.
Beers, D. R., Zhao, W., & Appel, S. H. (2018). The role of regulatory T lymphocytes in amyotrophic lateral sclerosis. JAMA Neurology, 75(6), 656–658.
Sheean, R. K., McKay, F. C., Cretney, E., Bye, C. R., Perera, N. D., Tomas, D., Weston, R. A., Scheller, K. J., Djouma, E., Menon, P., Schibeci, S. D., Marmash, N., Yerbury, J. J., Nutt, S. L., Booth, D. R., Stewart, G. J., Kiernan, M. C., Vucic, S., & Turner, B. J. (2018). Association of Regulatory T-cell expansion with progression of amyotrophic lateral sclerosis: A study of humans and a transgenic mouse model. JAMA Neurology, 75(6), 681–689.
Corsello, T., Amico, G., Corrao, S., Anzalone, R., Timoneri, F., Lo Iacono, M., Russo, E., Spatola, G. F., Uzzo, M. L., Giuffrè, M., Caprnda, M., Kubatka, P., Kruzliak, P., Conaldi, P. G., & la Rocca, G. (2019). Wharton’s jelly Mesenchymal stromal cells from human umbilical cord: A close-up on Immunomodulatory molecules featured in situ and in vitro. Stem Cell Reviews and Reports, 15, 900–918.
Zou, X., Gu, D., Zhang, G., Zhong, L., Cheng, Z., Liu, G., & Zhu, Y. (2016). NK cell regulatory property is involved in the protective role of MSC-derived extracellular vesicles in renal ischemic reperfusion injury. Human Gene Therapy, 27, 926–935.
Kordelas, L., Rebmann, V., Ludwig, A.-K., Radtke, S., Ruesing, J., Doeppner, T. R., Epple, M., Horn, P. A., Beelen, D. W., & Giebel, B. (2014). MSC-derived exosomes: A novel tool to treat therapy-refractory graft-versus-host disease. Leukemia., 28, 970–973.
Rostami, Z., Khorashadizadeh, M., & Naseri, M. (2020). Immunoregulatory properties of mesenchymal stem cells: Micro-RNAs. Immunology Letters, 219, 34–45.
Tadesse, T., Gearing, M., Senitzer, D., Saxe, D., Brat, D. J., Bray, R., Gebel, H., Hill, C., Boulis, N., Riley, J., Feldman, E., Johe, K., Hazel, T., Polak, M., Bordeau, J., Federici, T., & Glass, J. D. (2014). Analysis of graft survival in a trial of stem cell transplant in ALS. Annals of Clinical Translational Neurology, 1(11), 900–908.
Murdock, B. J., Zhou, T., Kashlan, S. R., Little, R. J., Goutman, S. A., & Feldman, E. L. (2017). Correlation of peripheral immunity with rapid amyotrophic lateral sclerosis progression. JAMA Neurology, 74(12), 1446–1454.
Rosenbohm, A., Nagel, G., Peter, R. S., Brehme, T., Koenig, W., Dupuis, L., Rothenbacher, D., Ludolph, A. C., & for the ALS Registry Study Group. (2018). Association of Serum Retinol-Binding Protein 4 concentration with risk for and prognosis of amyotrophic lateral sclerosis. JAMA Neurology, 75(5), 600–607.
Lunetta, C., Lizio, A., Maestri, E., Sansone, V. A., Mora, G., Miller, R. G., Appel, S. H., & Chiò, A. (2017). Serum C-reactive protein as a prognostic biomarker in amyotrophic lateral sclerosis. JAMA Neurology, 74(6), 660–667.
Zhao, W., Beers, D. R., Hooten, K. G., Sieglaff, D. H., Zhang, A., Kalyana-Sundaram, S., Traini, C. M., Halsey, W. S., Hughes, A. M., Sathe, G. M., Livi, G. P., Fan, G. H., & Appel, S. H. (2017). Characterization of gene expression phenotype in amyotrophic lateral sclerosis monocytes. JAMA Neurology, 74(6), 677–685.
Acknowledgements
This study was possible thanks to the invaluable cooperation of the patients and their families. We also want to thank the nurses, laboratory assistants, speech therapists and physiotherapists for their work and care provided to the patients. Special thanks should be extended to the people who supported the public fund-rising initiatives that allowed the patients to participate in this experiment regardless of their financial status. We would also like to thank prof. Krzysztof Selmaj and prof. Marcin Mycko for invaluable help in the process of analyzing research data.
Funding
The study was conducted in the pay-to-participate formula, with the costs covered either by the patients or from a public fund-raising campaign conducted by charities.
Author information
Authors and Affiliations
Contributions
M.B., S.M. I.Z.-M., T.S. and M.G. participated in the study concept, design and drafting of the manuscript and critical revision of the manuscript. M.B. and S.M. participated in data acquisition.
I.Z.-M. conducted the statistical analysis. S.M., I.Z.-M. and M.G. interpreted the data.
Corresponding author
Ethics declarations
Potential Conflict of Interest
Instytut Terapii Komórkowych S.A. (ITK) in Olsztyn is a private medical institution specialized in innovative commercial therapy which uses MSC. The Institute is partially owned by the University of Warmia and Mazury and controlled by Polski Bank Komórek Macierzystych S.A. (PBKM). M.B., S.M. and T.S. are employees of the Instytut Terapii Komórkowych S.A. I.Z.-M. and M.G. are employees of the Polski Bank Komórek Macierzystych S.A. The management of the ITK and PBKM had no influence on the collection, analysis and interpretation of data.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Ethics Approval
The experimental treatment was reviewed by the Bioethics Committee of the School of Medicine, University of Warmia and Mazury in Olsztyn, Poland (resolution no. 36/2014 of June 2014 and no. 8/2016 of February 2016) and performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplementary Fig. 1
Histogram of differences in age between patients treated with mesenchymal stem cells and the paired reference persons (PNG 75 kb)
Supplementary Fig. 2
Histogram of differences in the rate of progression between the patients treated with mesenchymal stem cells and the paired reference persons (PNG 205 kb)
Supplementary Fig. 3
Histogram of differences in the rate of progression between the patients being treated and the paired reference person. The power of survival analysis depending on the size of the treated group (PNG 297 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Barczewska, M., Maksymowicz, S., Zdolińska-Malinowska, I. et al. Umbilical Cord Mesenchymal Stem Cells in Amyotrophic Lateral Sclerosis: an Original Study. Stem Cell Rev and Rep 16, 922–932 (2020). https://doi.org/10.1007/s12015-020-10016-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-020-10016-7