Abstract
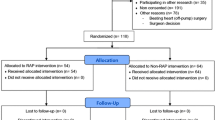
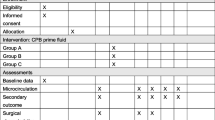
This randomized, double-blind study evaluated the short-term effects and safety of perioperative retrograde autologous priming (RAP) for cardiopulmonary bypass (CPB) in patients with cardiac replacement surgery to determine if this approach is a better substitute for crystal liquids priming in patients with valvular heart disease. We observed that RAP significantly decreased the actual priming volume, preserved the hematocrit and hemoglobin level during CPB to a certain degree, and decreased lactate accumulation in CPB period. Moreover, RAP lowered the volume of transfusion and dosage blood products. Thus, our results showed that RAP approach effectively improved tissue perfusion and lowered intraoperative Lac levels, by reducing the hemodilution, which safely and reliably improve the microcirculation perfusion.

Similar content being viewed by others
References
Zaid, R. R., et al. (2013). Pre- and post-operative diastolic dysfunction in patients with valvular heart disease: Diagnosis and therapeutic implications. Journal of the American College of Cardiology, 62(21), 1922–1930.
Khilji, S. A., & Khan, A. H. (2004). Acute renal failure after cardiopulmonary bypass surgery. Journal of Ayub Medical College, Abbottabad, 16(3), 25–28.
Ekert, H., et al. (2006). Elective administration in infants of low-dose recombinant activated factor VII (rFVIIa) in cardiopulmonary bypass surgery for congenital heart disease does not shorten time to chest closure or reduce blood loss and need for transfusions: A randomized, double-blind, parallel group, placebo-controlled study of rFVIIa and standard haemostatic replacement therapy versus standard haemostatic replacement therapy. Blood Coagulation and Fibrinolysis, 17(5), 389–395.
Song, L., et al. (2011). Effects of peri-operative glucose levels on adverse outcomes in infants receiving open-heart surgery for congenital heart disease with cardiopulmonary bypass. Perfusion, 26(2), 133–139.
Ranieri, V. M., et al. (1999). Time-course of impairment of respiratory mechanics after cardiac surgery and cardiopulmonary bypass. Critical Care Medicine, 27(8), 1454–1460.
Kapoor, P., et al. (2011). Changes in myocardial lactate, pyruvate and lactate–pyruvate ratio during cardiopulmonary bypass for elective adult cardiac surgery: Early indicator of morbidity. Journal of Anaesthesiology Clinical Pharmacology, 27(2), 225–232.
Murai, N., et al. (2005). Venous drainage method for cardiopulmonary bypass in single-access minimally invasive cardiac surgery: Siphon and vacuum-assisted drainage. Journal of Artificial Organs, 8(2), 91–94.
Dogan, R., et al. (2003). Three unusual cases where cardiopulmonary bypass was used in thoracic surgery. Respiration, 70(5), 537–540.
Gruenwald, C. E., et al. (2010). Management and monitoring of anticoagulation for children undergoing cardiopulmonary bypass in cardiac surgery. The Journal of Extra-Corporeal Technology, 42(1), 9–19.
Salis, S., et al. (2008). Cardiopulmonary bypass duration is an independent predictor of morbidity and mortality after cardiac surgery. Journal of Cardiothoracic and Vascular Anesthesia, 22(6), 814–822.
Kearsey, C., et al. (2013). Assessing the effectiveness of retrograde autologous priming of the cardiopulmonary bypass machine in isolated coronary artery bypass grafts. Annals of The Royal College of Surgeons of England, 95(3), 207–210.
Rosengart, T. K., et al. (1998). Retrograde autologous priming for cardiopulmonary bypass: A safe and effective means of decreasing hemodilution and transfusion requirements. Journal of Thoracic and Cardiovascular Surgery, 115(2), 426–438. (discussion pp. 438–439).
Murphy, G. S., et al. (2004). The failure of retrograde autologous priming of the cardiopulmonary bypass circuit to reduce blood use after cardiac surgical procedures. Anesthesia & Analgesia, 98(5), 1201–1207.
Bliacheriene, F., et al. (2012). Anesthesia for cardiac surgery under cardiopulmonary bypass in pregnant patients: Experience with nine cases. International Journal of Obstetric Anesthesia, 21(4), 388–389.
Colangelo, N., et al. (2006). Vacuum-assisted venous drainage in extrathoracic cardiopulmonary bypass management during minimally invasive cardiac surgery. Perfusion, 21(6), 361–365.
Hou, X., et al. (2009). Retrograde autologous priming of the cardiopulmonary bypass circuit reduces blood transfusion in small adults: A prospective, randomized trial. European Journal of Anaesthesiology, 26(12), 1061–1066.
Saxena, P., et al. (2003). Intraoperative autologous blood donation and retrograde autologous priming for cardiopulmonary bypass: A safe and effective technique for blood conservation. Annals of Cardiac Anaesthesia, 6(1), 47–51.
Silver, H. (1975). Banked and fresh autologous blood in cardiopulmonary bypass surgery. Transfusion, 15(6), 600–603.
Balachandran, S., et al. (2002). Retrograde autologous priming of the cardiopulmonary bypass circuit reduces blood transfusion after coronary artery surgery. The Annals of Thoracic Surgery, 73(6), 1912–1918.
Welsby, I. J., et al. (2002). The association of complication type with mortality and prolonged stay after cardiac surgery with cardiopulmonary bypass. Anesthesia & Analgesia, 94(5), 1072–1078.
Manrique, A., et al. (2009). The association of renal dysfunction and the use of aprotinin in patients undergoing congenital cardiac surgery requiring cardiopulmonary bypass. Anesthesia & Analgesia, 109(1), 45–52.
Hwang, J., et al. (2011). The effect of retrograde autologous priming of the cardiopulmonary bypass circuit on cerebral oxygenation. Journal of Cardiothoracic and Vascular Anesthesia, 25(6), 995–999.
Huebler, M., et al. (2006). Cardiopulmonary bypass for complex cardiac surgery using bivalirudin anticoagulation in a patient with heparin antibodies. Journal of Cardiac Surgery, 21(3), 286–288.
Murphy, G. S., et al. (2006). Retrograde autologous priming of the cardiopulmonary bypass circuit: Safety and impact on postoperative outcomes. Journal of Cardiothoracic and Vascular Anesthesia, 20(2), 156–161.
Ortega, G. M., et al. (2003). Alteration of vancomycin pharmacokinetics during cardiopulmonary bypass in patients undergoing cardiac surgery. American Journal of Health-System Pharmacy, 60(3), 260–265.
Ling, I. S., et al. (1992). Changes of blood viscosity in patients undergoing cardiac surgery during cardiopulmonary bypass. Ma Zui Xue Za Zhi = Anaesthesiologica Sinica, 30(3), 153–157.
Ranucci, M., et al. (2006). Lowest hematocrit on cardiopulmonary bypass impairs the outcome in coronary surgery: An Italian multicenter study from the National Cardioanesthesia Database. Texas Heart Institute Journal, 33(3), 300–305.
Sanchez, A. S. Salinas, et al. (2000). Adrenal cortex carcinoma with right atrium involvement. Surgery with cardiopulmonary bypass. Actas Urologicas Espanolas, 24(7), 590–593.
Grieco, G., et al. (1996). Evaluating neuroprotective agents for clinical anti-ischemic benefit using neurological and neuropsychological changes after cardiac surgery under cardiopulmonary bypass. Methodological strategies and results of a double-blind, placebo-controlled trial of GM1 ganglioside. Stroke, 27(5), 858–874.
Kato, Y., et al. (1996). Deep hypothermia cardiopulmonary bypass and direct surgery of two large aneurysms at the vertebro-basilar junction. Acta Neurochirurgica (Wien), 138(9), 1057–1066.
Gruenwald, C. E., et al. (2010). Randomized, controlled trial of individualized heparin and protamine management in infants undergoing cardiac surgery with cardiopulmonary bypass. Journal of the American College of Cardiology, 56(22), 1794–1802.
Acknowledgments
This study was supported by the Technological Innovation Talent Special Foundation of Harbin, China (2009RFXXS018) and the Youth Science Foundation of Heilongjiang Province (QC2013C116).
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Cheng, M., Li, JQ., Wu, TC. et al. Short-Term Effects and Safety Analysis of Retrograde Autologous Blood Priming for Cardiopulmonary Bypass in Patients with Cardiac Valve Replacement Surgery. Cell Biochem Biophys 73, 441–446 (2015). https://doi.org/10.1007/s12013-015-0661-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-015-0661-1