Abstract
The aim of the present study was to evaluate the clinical usefulness of applying RT-nested PCR along with RFLP as a method for diagnosis and genotypic differentiation of Hantavirus in the acute-stage sera of HFRS patients as compared to the ELISA technique. A prospective study of patients with suspected HFRS patients was carried out. Sera were collected for serological evaluation by ELISA and RT-nested PCR testing. Primers were selected from the published sequence of the S segment of HTNV strain 76-118 and SEOV strain SR-11, which made it possible to obtain an amplicon of 403 bp by RT-nested PCR. The genotypic differentiations of the RT-nested PCR amplicons were carried out by RFLP. Sequence analyses of the amplicons were used to confirm the accuracy of the results obtained by RFLP. Of the 48 acute-stage sera from suspected HFRS patients, 35 were ELISA-positive while 41 were positive by RT-nested PCR. With Hind III and Hinf I, RFLP profiles of the RT-nested PCR amplicons of the 41 positive sera exhibited two patterns. 33 had RFLP profiles similar to the reference strain R22, and thus belonged to the SEOV type. The other 8 samples which were collected during October–December had RFLP profiles similar to the reference strain 76-118, and thus belonged to the HTNV type. Sequence phylogenetic analysis of RT-nested PCR amplicons revealed sdp1, sdp2 YXL-2008, and sdp3 as close relatives of HTNV strain 76-118, while sdp22 and sdp37 as close relatives of SEOV strain Z37 and strain R22 located in two separate clusters in the phylogenetic tree. These results were identical to those acquired by RFLP. RT-nested PCR integrated with RFLP was a rapid, simple, accurate method for detecting and differentiating the genotypes of Hantavirus in the acute-stage sera of suspected HFRS patients. In Shandong province, the main genotypes of Hantavirus belonged to the SEOV types, while the HTNV types were observed during the autumn–winter season.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
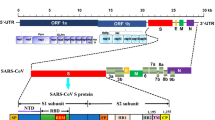
Hemorrhagic fever with renal syndrome (HFRS) is a rodent-borne viral zoonosis caused by viruses of the genus Hantavirus, Bunyaviridae family [1, 2]. Hantaviruses are enveloped, single-stranded, and negative-sense RNA viruses. The genome of Hantavirus consists of three segments, designated as large (L), medium (M), and small (S), respectively, encoding the RNA-dependent RNA polymerase, the glycoprotein precursor (GPC) protein that is processed into two separate envelope glycoproteins (G1, G2), and the nucleocapsid (N) protein [3–5]. Up till now, 21 different Hantavirus species have been reported, among which more than 30 genotypes have been characterized [6]. Each Hantavirus appears to be associated in nature with specific rodent species and it is thought to co-evolve with its rodent hosts. Consequently, Hantaviruses form three large groups according to their rodent hosts: Murinae-, Arvicolinae-, and Sigmodontinae-associated Hantaviruses [3, 7, 8]. Of these, the Murinae-associated Hantaan virus (HTNV), Seoul virus (SEOV), Dobrava virus (DOBV), and the Arvicolinae-associated Puumala virus (PUUV) are causative agents of HFRS. Sin Nombre virus (SNV), Andes virus (ANDV), Black Creek Canal virus (BCCV), Lagna Negra virus (LANV), and other related viruses cause Hantavirus pulmonary syndrome (HPS) [9].
China is the most severe endemic country with 90 % of the total HFRS cases reported in the world [10]. Although integrated intervention measures involving rodent control, environment management, and vaccination have been implemented, HFRS still remains an important public health problem with 20,000–50,000 human cases diagnosed annually [11]. Recently, many Hantaviruses have been isolated from various rodent species and patients throughout China. Serologic and antigenic studies showed that these isolates were related to either HTNV or SEOV type, which are associated with the rodent subfamily Murinae [12, 13]. Shi et al. [14] compared the nucleotide sequence of the M genome segment of Chinese HTNV and SEOV to those of Korean and Japanese isolates and showed that Chinese Hantaviruses form lineages distinct from other Asian isolates. Liang et al. [13] also showed that at least three subtypes of Hantaviruses are present in China. It has been reported that HTNV and SEOV viruses, which showed different fatality rates (HTNV for 5 ± 10 %, SEOV 1 ± 2 %) and unapparent infection rates (HTNV for 1 ± 4 %, SEOV 8 ± 20 %), coexist in China [10]. This suggests that Hantaviruses with different degrees of virulence coexist in China. The clinical manifestations on admission may be indistinguishable between both the viruses, although the clinical course of HTNV infection is more severe than that of SEOV. Thus it is of significance for diagnosis and prevention to elucidate the differentiation of the viruses. Reverse transcription-polymerase chain reaction (RT-PCR)/restriction fragment length polymorphism (RFLP) has been used to analyze the G2 region, S segment, and spacer region between G1 and G2 of the M segment [15, 16].
The diagnosis of HFRS is made either by isolation of Hantaviruses from the blood of a patient during the febrile period or by showing an increased level of serum antibodies against Hantaviruses during convalescence [10, 11]. However, identification of Hantaviruses in cultured cells or in infected mice requires at least several weeks and it must be done in a biosafety level-2 laboratory.
The indirect immunofluorescent antibody assay (IFA) and enzyme-linked immunosorbent assay (ELISA) are generally accepted as gold standard serological assays [10–12]. However, IFA and ELISA are time consuming and they require specialized equipment and trained personnel. There is also a delay of several days between the onset of the illness and the increased antibody titer, and a positive reaction is often detected only after the acute illness has resolved. Diagnosis can be difficult in the early stage of illness when the antibody titers are not yet high enough to be detected. Therefore, a simple and more rapid laboratory diagnostic method for HFRS is needed. RT-nested PCR assay on the blood sample has proven useful for early diagnosis of HFRS. RT-nested PCR connected with other molecular methods for detecting and genotyping RNA from Hantaviruses is both sensitive and specific in the laboratory [13–19]. However, there are fewer data to evaluate this assay in prospective studies.
In this study, we conducted a prospective study of patients with suspected HFRS who were admitted to three hospitals in Feixian County, Shandong province to evaluate the usefulness of performing RT-nested PCR integrated with RFLP as a method for diagnosing and differentiating the genotypes of Hantavirus in the acute-stage sera of HFRS patients. We also compared the RT-nested PCR results with ELISA results.
Materials and Methods
Samples
From October 2002 to April 2004, patients with acute undifferentiated fever who presented to Fangcheng, Wanggou, and Shangyi town hospitals of Feixian County, Shandong province were considered. After informed consent was obtained, 5 ml acute-stage blood and urine were collected from each patient at the time of admission to hospitals for routine laboratory examination. Patients who had clinical manifestations, routine laboratory tests, and epidemiological histories indicative of HFRS were enrolled in the study. Briefly, the clinical manifestations included acute fever; headache; retro-orbital pain; lumbar back pain and flank tenderness; erythematous flushes on the face, neck, and upper bosom; hemorrhage on skin and mucosa. The routine laboratory results suggestive of HFRS included thrombocytopenia, proteinuria, occult blood in urine, etc. Epidemiological exposure histories indicating that patients had worked in crop fields, been in contact with rodents, and eaten food or drink water contaminated by rodents were also part of the enrollment criteria. The clinically provisional diagnosis of HFRS patients were primarily confirmed by the presence of IgM antibody to Hantavirus by ELISA (Zibo Xinke Science Service Company, China), according to the manufacturer’s recommendations.
Design and Synthesis of Oligonucleotide Primers
According to the published sequences of the S segments of Hantavirus strain 76-118 and strain R22 [15, 17, 18], five primers were synthesized by Shanghai Sangon Biotechnology Corporation.
-
SK1: 5′-ATT GAT GAA CCT ACA GGA C-3′ (HTNV 361-379, SEOV 367-385);
-
SK2: 5′-AGC ATG AAG GCA GAA GAG-3′ (HTNV 595-612, SEOV 601-618);
-
SK3: 5′-ACA AGC ATG TTG GTG GAC-3′ (HTNV 980-997, SEOV 986-1003);
-
SK4: 5′-TGT ATC CCC ATT GAT TGT G-3′ (HTNV 1142-1160, SEOV 1148-1166);
-
SKR: 5′-TAG TAG TAG AC-3′ (1–11 bp).
For RT-nested PCR, SK1 and SK4 served as outer primers, while SK2 and SK4 served as inner primers. SKR was synthesized as reverse transfer primer.
Reagents
Avian myeloblastosis virus reverse transcriptase (AMV RTase), dNTPs were purchased from promega. Hinf I and Hind III were products of Huamei Biotechnology Company. Taq DNA polymerase was obtained from Shanghai Sangon Biotechnology Corporation. PCR thermal cycler was purchased from PE Corporation. Hantavirus strain 76-118 and strain R22 were purchased as positive controls from Institute of Virology, Wuhan University.
RNA Extraction
Total RNA was isolated from the acute-stage sera of suspected HFRS patients using the guanidine isothiocyanate-phenol-chloroform procedure as described by Chomczynski and Nicoletla [19]. 400 μl denaturing buffer (4 M guanidine isothiocyanate, 25 mM sodium citrate, pH 7.0, 0.5 % sarcosyl, and 0.1 % β-mercaptoethanol) was added to 100 μl sera and mixed thoroughly. To this mixture, 50 μl sodium acetate (2 M, pH 4.0) and 100 μl chloroform were sequentially added and vigorously vortexed. The suspension was then placed on ice for 15 min and centrifuged at 10,000×g for 10 min at 4 °C. The RNA was precipitated with an equal volume of isopropanol and re-suspended in denaturing buffer. The RNA was precipitated again with isopropanol, washed with anhydrous ethanol, and dissolved in DEPC-treated water.
RT-Nested PCR
cDNA Synthesis
All the extracted virus RNA was used to transcribe in a reaction mixture which contained 4 μl 5× RT Buffer, 0.1 M RNasin 2 μl, 4× dNTP 1 μl, AMV RTase 1 μl, SKR 1 μl, and at last DEPC-treated water was added up to 20 μl. Transcription was done at 37 °C for 60 min, and then AMV RTase was inactivated at 95 °C for 10 min.
Initial PCR
Reverse-transcribed RNA was amplified in a volume of 100 μl which contained 20 μl cDNA, 2 μl (1 U/μl) Taq DNA polymerase, 8 μl MgCl2 (25 mM), 1 μl 4× dNTP, 10 μl 10× PCR buffer, and 2 μl outer primer pairs (SK1 and SK4). 60 μl liquid olefin was added, 35 cycles at 94 °C for 1 min, 58 °C for 1 min, and 72 °C for 1 min were performed, followed by a final extension at 72 °C for 7 min.
Nested PCR
Nested PCR was performed using the same conditions as the initial PCR, substituting inner primer SK2 and SK3 for outer primers and the amplicons from the initial PCR reaction as templates. The nested PCR amplicons were detected by electrophoresis in 2 % agarose containing ethidium bromide and visualized under ultraviolet light.
In parallel with each of initial and nested PCR amplification of the isolates, cDNAs or amplicons from the international reference strains (strain 76-118 and strain R22) were used as positive controls, respectively, and distilled water was used as a negative control. To avoid contamination, RNA extraction, the reagent setup, initial and nested PCR, and electrophoresis were all performed in separate rooms.
RFLP
Nested PCR amplicon was mixed with 5 U Hind III, or Hinf I in a volume of 20 μl reaction system and incubated at 37 °C for 3 h. Electrophoresis of DNA fragments was carried out in 2 % agarose containing ethidium bromide and visualized under ultraviolet light. The genotypes of Hantavirus in the sera of patients were determined by comparing their digestion profiles with those of the two prototype virus strains (Table 1).
Sequence Alignments and Phylogenetic Analysis
According to the RFLP results, RT-nested PCR amplicons of five representative patients’ sera were sequenced. The GenBank accession numbers of the five PCR amplicons were sdp1, EU370775; sdp2, YXL-2008 EU370776; sdp3, EU370777; sdp22, EU370778; and sdp37, EU370779. The sequences were aligned together with the nucleotide sequences deposited in GenBank by Clustal X (version 1.8) program. Phylogenetic analysis was performed with the distance-based neighbor-joining (NJ) method (PHYLIP 3.63). The Jukes–Cantor distances were used for phylogenetic inference. It was done in the following way: (1) 1,000 bootstrap replicates were performed on the sequencing data using SEQBOOT program; (2) the distance matrix was calculated with DNADIST program; (3) a set of 1,000 phylogenetic trees based on the matrix was calculated using NEIGHBOUR program; and (4) CONSENCE program was used to create the consensus tree. The tree was imported into the TreeView program for text editing and printing. VarPlot for Windows software was used to calculate ratios of non-synonymous to synonymous substitutions of nucleotide sequence.
Nucleotide Sequence Accession Number
The GenBank accession numbers for the S genes used for comparison in this study were PUU, AF442613; Tula, NC005227; Z37, AF187082; 80-39, AY273791; R22, AF488707; K24-e7, AF288653; Gou3, AF184988; Z10, AF184987; S85-46, AF288659; AH09, AF285264; BjHD01, AY627049; SNV, NC005216; L99, AF288299; 76-118, M14626; and LR1, AF288294.
Results
RT-Nested PCR
Totally 48 acute-stage sera of suspected HFRS patients were collected during the study period. 35 of them were ELISA-positive. The 403 bp bands could be amplified in 43 out of the 48 samples (Table 1).
RFLP
Comparing with the RFLP profiles of the prototype Hantavirus (Table 2; Fig. 1), 33 of the 41 samples had the same RFLP profiles, their RFLP profiles were close to those of strain R22, their DNA amplicons were digested into 155, 115, 60, 32/39 bp by Hinf I, and had no restriction site of Hind III (Fig. 2). The RFLP profiles of the other 8 samples had the RFLP profiles similar to that of 76-118 strain, their DNA amplicons were digested into 280, 60, 60 bp by Hinf I and digested into 175, 228 bp by Hind III (Fig. 3). All of the 8 sera were collected between October and December.
RFLP analysis in the S gene amplicons of prototype virus strain 76-118 and strain R22 with Hind III, Hinf I. Lanes 1, 5, 9: Marker pUC19DNA/Msp I (Hpa II). Lanes 2–4: Amplicons of strain R22 digested by Hinf I, Hind III, and uncut. Lanes 6–8: Amplicons of strain 76-118 digested by Hinf I, Hind III, and uncut
Phylogenetic Analysis of Hantavirus S Gene
In the phylogenetic analysis, sdp1, sdp2 YXL-2008, and sdp3 were closely related to strain 76-118; sdp22 and sdp37 were clustered with Z37 and R22 strains (Fig. 4).
Phylogenetic tree for Hantavirus in the sera of patients based on the partial sequence of S gene segments, excluding the primer sequences. Bootstrap values are expressed in percentages after sampling 1,000 times. Accession numbers of published sequences: PUU, AF442613; Tula, NC005227; Z37, AF187082; 80-39, AY273791; R22, AF488707; K24-e7, AF288653; Gou3, AF184988; Z10, AF184987; S85-46, AF288659; AH09, AF285264; BjHD01, AY627049; SNV, NC005216; L99, AF288299; 76-118, M14626; and LR1, AF288294
Discussion
The diagnosis of HFRS has traditionally been based on the assessment of the antibody titer in the serum samples obtained during the acute and convalescent stage of illness by serological methods, such as ELISA, IFA, etc. Although the specificity and sensitivity of serological methods were much higher, they did not provide a direct evidence of virus infection. In addition, it takes several weeks to confirm the diagnosis through serological testing for establishing a fourfold or greater titer increase. The delay in administering effective antibiotic treatment of some patients can lead to severe complications or mortality [10, 11]. Thus, achieving a rapid and precise diagnosis is necessary for proper medical management of HFRS. The PCR assay is a useful tool for facilitating the diagnosis of infectious diseases that are caused by fastidious or slow-growing microorganisms. The PCR results can be made available within 24 h, and this can greatly help in proper patient management. In the present study, the antibodies positive rates detected by serological methods were much lower, especially for patients whose courses of disease ≤7 days (Table 1). This could be most possibly because of the latent period for antibody production after the Hantavirus invades the human body. Compared with serological methods, RT-nested PCR was more sensitive and specific and provided a direct evidence of viral infection. In our study, Hantavirus was detected in all patients whose course of disease ≤7 days, indicating that RT-nested PCR was suitable for early diagnosis of Hantavirus infection.
With the development of the molecular biology, RFLP and gene sequencing are routinely applied in genotyping [20]. RFLP is a technique in which organisms may be differentiated by analysis of patterns derived from cleavage of their DNA. If two organisms differ in the distance between sites of cleavage of a particular restriction endonuclease, the length of the fragments produced will differ when the DNA is digested with a restriction enzyme. The similarity of the patterns generated can be used to differentiate species (and even strains) from one another [15, 20]. In Fei county, Shandong province, RT-nested PCR/RFLP analysis showed that HFRS is caused mainly by two serotypes of Hantavirus, HTNV and SEOV. The results in our study are consistent with those obtained from serological data [10].
Nucleotide sequence analysis is the most accurate, reliable genotyping method, which can detect single-nucleotide differences [14]. However, it could not be widely developed in China due to cost limitations. To overcome this, RT-nested PCR/RFLP genotyping method, combined with sequence analysis of specific virus strains, can be used as an alternate technique for epidemiology and vaccine strain screening.
At present, the prevalent genotypes of Hantavirus were mainly HTNV and SEOV type in China and each type was also classified into different subtypes [21, 22]. The areas prone to epidemics were in a state of continual evolution. In recent years, in the studied areas the dominant genotypes varied from HTNV type into SEOV type. This resulted in gene drift and transition of the Hantavirus associated with long-term and persistent infection in the host [23, 24]. In addition, the virus gene may vary to some extent in the presence of herd immunity. The study proved that two different Hantavirus types co-existed in the Shandong province, the former type was SEOV and the latter, HTNV type which was also found in autumn and winter. No significant difference was found between S fragment of the two Hantavirus types and the standard strain by analyzing the RFLP profiles. The two different Hantavirus types coexisted in HFRS severe epidemic areas, providing more opportunities for different types to recombine with each other. So we need to strengthen the epidemiological surveillance in future and pay more attention to the variation of the Hantavirus genotype in order to prevent the explosion of severe epidemic situations.
References
Schmaljohn, C. S., & Dalrymple, J. M. (1983). Analysis of Hantaan virus RNA: Evidence for a new genus of Bunyaviridae. Virology, 131, 482–491.
Nichol, S. T., Spiropoulou, C. F., Morzunov, S., et al. (1993). Genetic identification of a Hantavirus associated with an outbreak of acute respiratory illness. Science, 262, 914–917.
Plyusnin, A., Vapalahti, O., & Vaheri, A. (1996). Hantavirus: Genome structure, expression and evolution. Journal of General Virology, 77, 2677–2687.
Clement, J. P. (2003). Hantavirus. Antiviral Research, 57, 121–127.
Vapalahti, O., Mustonen, J., Lundkvist, A., et al. (2003). Hantavirus infections in Europe. Lancet Infect Disease, 3, 653–661.
Muranyi, W., Bahr, U., Zeier, M., et al. (2005). Hantavirus Infection. Journal of the American Society of Nephrology, 16, 3669–3679.
Hughes, A. L., & Friedman, R. (2000). Evolutionary diversification of protein-coding genes of Hantaviruses. Molecular Biology and Evolution, 17, 1558–1568.
Zeier, M., Handermann, M., Bahr, U., et al. (2005). New ecological aspects of Hantavirus infection: A Change of a paradigm and a challenge of prevention–a review. Virus Genes, 30, 157–180.
Hart, C. A., & Bennettb, M. (1999). Hantavirus infections: Epidemiology and pathogenesis. Microbes and Infection, 1, 1229–1237.
Song, G. (1999). Epidemiological progresses of hemorrhagic fever with renal syndrome in China. Chinese Medical Journal, 112, 472–477.
Bai, X., & Huang, C. (2002). Strengthen further the study on hemorrhagic fever with renal syndrome. Chinese Journal of Infectious Diseases, 20, 197–198.
Tang, Y. W., Li, Y. L., Ye, K. L., et al. (1991). Distribution of Hantavirus serotypes Hantaan and Seoul causing hemorrhagic fever with renal syndrome and identification by hemagglutination inhibition assay. Journal of Clinical Microbiology, 29, 1924–1927.
Liang, M., Li, D., Xiao, S. Y., et al. (1994). Antigenic and molecular characterization of Hantavirus isolates from China. Virus Research, 31, 219–233.
Shi, X. H., Liang, M. F., Hang, C. S., et al. (1998). Nucleotide sequence and phylogenetic analysis of the medium (M) genomic RNA segments of three Hantaviruses isolated in China. Virus Research, 56, 69–76.
Kim, E. C., Kim, I. S., Choi, Y., et al. (1994). Rapid differentiation between Hantaan and Seoul viruses by PCR and restriction enzyme analysis. Journal of Medical Virology, 43, 245–248.
Xiao, S. Y., Liang, M., & Schmaljohn, C. S. (1993). Molecular and antigenic characterization of HV114, a Hantavirus isolated from a patient with haemorrhagic fever with renal syndrome in China. Journal of General Virology, 74, 1657–1659.
Schmaljohn, C. S., Jennings, G. B., Hay, J., et al. (1986). Coding strategy of the S genome segment of Hantavirus. Virology, 155, 633–643.
Arikawa, J., Lapenotiere, H. F., Iacono-Connors, L., et al. (1990). Coding properties of the S and the M genome segments of Sapporo rat virus: Comparison to other causative agents of hemorrhagic fever with renal syndrome. Virology, 176, 114–125.
Chomczynski, P., & Sacchi, N. (1987). Single-step method of RNA isolation by acid guanidinium thiocyanate—phenol-chloroform extraction. Analytical Biochemistry, 162, 156–159.
Ahn, C., Cho, J. T., Lee, J. G., et al. (2000). Detection of Hantaan and Seoul viruses by reverse transcriptase-polymerase chain reaction (RT-PCR) and restriction fragment length polymorphism (RFLP) in renal syndrome patients with hemorrhagic fever. Clinical Nephrology, 53, 79–89.
Wang, H., Yoshimatsu, K., Ebihara, H., et al. (2000). Genetic diversity of Hantaviruses isolated in China and characterization of novel Hantaviruses isolated from Niviventer confucianus and Rattus rattus. Virology, 278, 332–345.
Wang, S. W., Hang, C. S., Wang, H., et al. (2002). Genotype and clade distribution of Hantavirus in China. China Journal of Virology, 18, 211–216.
Kang, D., Ruan, Y., Fu, J., et al. (2001). Epidemiological changes of hemorrhage fever with renal syndrome in Shandong Province, 1990–1998. Chinese Journal of Epidemiology, 17, 341–342.
Li, D., Schmaljohn, A. L., Anderson, K., et al. (1995). Complete nucleotides sequences of the M and S segment of two Hantavirus isolates from California;evidence for reassortment in nature among virus related to Hantavirus pulmonary syndrome. Virology, 206, 973–983.
Acknowledgments
This study was supported by National Natural Science Foundation of China (No. 30872155 and No. 30972523); China Special Grant for the Prevention and Control of Infectious Diseases (2013ZX10004 805 – 003, 2013ZX10004 217-002); The twelfth five year research foundation of Military Medical Sciences and Technology [the key program (AWS11L009) and the Special Grant for health protection (11BJZ01)]; and Developing Plans for Science and Technology of Shandong Province (No. 022130111).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, YX., Zhao, ZT., Cao, WC. et al. Clinical Application of RT-Nested PCR Integrated with RFLP in Hantavirus Detection and Genotyping: A Prospective Study in Shandong Province, PR China. Cell Biochem Biophys 67, 1521–1527 (2013). https://doi.org/10.1007/s12013-013-9655-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-013-9655-z