Abstract
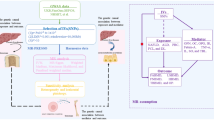
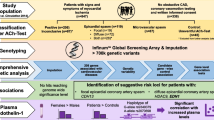
The serum levels and activity of matrix metalloproteinases (MMPs) are associated with the risk of coronary artery calcification (CAC). We sought to investigate the association between MMP-2 -1575G>A (rs243866) and MMP-9 -1562 C>T (rs3918242) SNPs with MMP-2 and MMP-9 serum levels and activity in individuals with CAC. One hundred and fifty-five cases with CAC and 155 healthy individuals as control group from West of Iran were included and frequency of genotypes and alleles of rs243866 and rs3918242 in MMP-2 and MMP-9 genes were determined using PCR–RFLP. We also investigated the serum levels of MMP-2 and MMP-9 and their activity using ELISA and gelatin zymography, respectively. Additionally, serum biochemical parameters including FBS (fasting blood sugar), urea, creatinine, cholesterol, triglyceride, HDL (high-density lipoprotein), LDL (low-density lipoprotein), calcium, and phosphorus as well as blood pressure (systolic blood pressure (SBP) and diastolic blood pressure (DBP)) were measured. Our results showed that both serum levels of MMP-2 and MMP-9 (P < 0.001) and their activity (P < 0.001) were higher in individuals with CAC when compared to the control group. Carrying A and T alleles in MMP-2 -1575G>A (rs243866) and MMP-9 -1562 C>T (rs3918242) SNPs, respectively, may predispose the individuals to CAC by acting as the risk factors. Serum levels and activity of MMP-2 and MMP-9 were found to be higher in CAC cases when compared to the healthy controls. Carriers of A allele in rs243866 SNP and T allele in rs3918242 SNP were shown to have higher MMP-2 and MMP-9 serum levels and activity that may result in increased ECM degradation and support the initiation and development of calcification.


Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code Availability
N/A.
Abbreviations
- BMI:
-
Body mass index
- CAC:
-
Coronary artery calcification
- DBP:
-
Diastolic blood pressure
- SBP:
-
Systolic blood pressure
- SNP:
-
Single-nucleotide polymorphism
- HDL:
-
High-density lipoprotein
- LDL:
-
Low-density lipoprotein
- DFU:
-
Diabetic foot ulcers
- ECM:
-
Extracellular matrix
- FBS:
-
Fasting blood sugar
- HWE:
-
Hardy–Weinberg equilibrium
- T2DM:
-
Type 2 diabetes mellitus
- Tg:
-
Triglyceride
- WT:
-
Wild type
References
Liu, W., Zhang, Y., Yu, C. M., Ji, Q. W., Cai, M., Zhao, Y. X., & Zhou, Y. J. (2015). Current understanding of coronary artery calcification. Journal of Geriatric Cardiology: JGC, 12, 668–675.
Mohammadi-Noori, E., Salehi, N., Mozafari, H., EliehAliKomi, D., Saidi, M., Bahrehmand, F., Vaisi-Raygani, A., Elahirad, S., Moini, A., & Kiani, A. (2020). Association of AHSG gene polymorphisms with serum Fetuin-A levels in individuals with cardiovascular calcification in west of Iran. Molecular Biology Reports, 47, 1809–1820.
Hillerson, D., Wool, T., Ogunbayo, G. O., Sorrell, V. L., & Leung, S. W. (2020). Incidental coronary artery calcification and stroke risk in patients with atrial fibrillation. AJR: American Journal of Roentgenology, 215, 1–7.
Wang, L., Jerosch-Herold, M., Jacobs, D. R., Jr., Shahar, E., Detrano, R., & Folsom, A. R. (2006). Coronary artery calcification and myocardial perfusion in asymptomatic adults: The MESA (Multi-Ethnic Study of Atherosclerosis). Journal of the American College of Cardiology, 48, 1018–1026.
Mori, H., Torii, S., Kutyna, M., Sakamoto, A., Finn, A. V., & Virmani, R. (2018). Coronary artery calcification and its progression: what does it really mean? CJACC Cardiovascular Imaging, 11, 127–142.
Joseph, T. P., Kotecha, N. S., Kumar, H. B. C., Jain, N., Kapoor, A., Kumar, S., Bhatia, E., Mishra, P., & Sahoo, S. K. (2020). Coronary artery calcification, carotid intima-media thickness and cardiac dysfunction in young adults with type 2 diabetes mellitus. Journal of Diabetes and Its Complications, 34, 107609.
Motro, M., & Shemesh, J. (2001). Calcium channel blocker nifedipine slows down progression of coronary calcification in hypertensive patients compared with diuretics. Hypertension (Dallas, Tex.: 1979), 37, 1410–1413.
Manson, J. E., Allison, M. A., Rossouw, J. E., Carr, J. J., Langer, R. D., Hsia, J., Kuller, L. H., Cochrane, B. B., Hunt, J. R., Ludlam, S. E., Pettinger, M. B., Gass, M., Margolis, K. L., Nathan, L., Ockene, J. K., Prentice, R. L., Robbins, J., & Stefanick, M. L. (2007). Estrogen therapy and coronary-artery calcification. The New England Journal of Medicine, 356, 2591–2602.
Kalil, R. S., Flanigan, M., Stanford, W., & Haynes, W. G. (2012). Dissociation between progression of coronary artery calcification and endothelial function in hemodialysis patients: A prospective pilot study. Clinical Nephrology, 78, 1–9.
Chertow, G. M., Burke, S. K., & Raggi, P. (2002). Sevelamer attenuates the progression of coronary and aortic calcification in hemodialysis patients. Kidney international, 62, 245–252.
Chen, C. L., Chen, N. C., Wu, F. Z., & Wu, M. T. (2020). Impact of denosumab on cardiovascular calcification in patients with secondary hyperparathyroidism undergoing dialysis: A pilot study. Osteoporosis International, 31, 1507–1516.
Elieh Ali Komi, D., & Grauwet, K. (2018). Role of mast cells in regulation of T cell responses in experimental and clinical settings. Clinical Reviews in Allergy & Immunology, 54, 432–445.
EliehAliKomi, D., Shafaghat, F., & Haidl, G. (2020). Significance of mast cells in spermatogenesis, implantation, pregnancy, and abortion: Cross talk and molecular mechanisms. American Journal of Reproductive Immunology (New York, N.Y.: 1989), 83, e13228.
Komi, D. E. A., & Redegeld, F. A. (2020). Role of mast cells in shaping the tumor microenvironment. Clinical Reviews in Allergy & Immunology, 58, 313–325.
Komi, D. E. A., Khomtchouk, K., & Santa Maria, P. L. (2020). A review of the contribution of mast cells in wound healing: Involved molecular and cellular mechanisms. Clinical Reviews in Allergy & Immunology, 58, 298–312.
Rao, V. H., Lees, G. E., Kashtan, C. E., Nemori, R., Singh, R. K., Meehan, D. T., Rodgers, K., Berridge, B. R., Bhattacharya, G., & Cosgrove, D. (2003). Increased expression of MMP-2, MMP-9 (type IV collagenases/gelatinases), and MT1-MMP in canine X-linked Alport syndrome (XLAS). Kidney International, 63, 1736–1748.
Najafi, K., Komi, D. E. A., Khazaie, H., Moini, A., Vaisi, A., Raygani, Ahmadi, H. R., Ghadami, M. R., & Kiani, A. (2019). Investigation of serum levels and activity of matrix metalloproteinases 2 and 9 (MMP2, 9) in opioid and methamphetamine-dependent patients. Acta Medica Iranica, 56, 559–562.
Mirabdaly, S., Elieh Ali Komi, D., Shakiba, Y., Moini, A., & Kiani, A. (2020). Effects of temozolomide on U87MG glioblastoma cell expression of CXCR4, MMP2, MMP9, VEGF, anti-proliferatory cytotoxic and apoptotic properties. Molecular Biology Reports, 47, 1187–1197.
Chen, N. X., O’Neill, K. D., Chen, X., Kiattisunthorn, K., Gattone, V. H., & Moe, S. M. (2011). Activation of arterial matrix metalloproteinases leads to vascular calcification in chronic kidney disease. American Journal of Nephrology, 34, 211–219.
Radunovic, M., Nikolic, N., Milenkovic, S., Tomanovic, N., Boricic, I., Dimitrijevic, M., Novakovic, I., & Basta-Jovanovic, G. (2016). The MMP-2 and MMP-9 promoter polymorphisms and susceptibility to salivary gland cancer. Journal of BUON, 21, 597–602.
Singh, K., Agrawal, N. K., Gupta, S. K., & Singh, K. (2013). A functional single nucleotide polymorphism -1562C>T in the matrix metalloproteinase-9 promoter is associated with type 2 diabetes and diabetic foot ulcers. The International Journal of Lower Extremity Wounds, 12, 199–204.
Habel, A. F., Ghali, R. M., Bouaziz, H., Daldoul, A., Hadj-Ahmed, M., Mokrani, A., Zaied, S., Hechiche, M., Rahal, K., Yacoubi-Loueslati, B., & Almawi, W. Y. (2019). Common matrix metalloproteinase-2 gene variants and altered susceptibility to breast cancer and associated features in Tunisian women. Tumour Biology, 41, 1010428319845749.
Ting, W. C., Chen, L. M., Pao, J. B., Yang, Y. P., You, B. J., Chang, T. Y., Lan, Y. H., Lee, H. Z., & Bao, B. Y. (2013). Genetic polymorphisms of matrix metalloproteinases and clinical outcomes in colorectal cancer patients. International Journal of Medical Sciences, 10, 1022–1027.
Tian, Y., An, F., Wang, J., Liu, C., Wu, H., Cao, Y., Wang, J., & Wang, G. (2019). MMP2 and MMP10 polymorphisms are related to steroid-induced osteonecrosis of the femoral head among Chinese Han population. BioMed Research International, 2019, 8298193.
Chacon-Cortes, D., & Griffiths, L. (2014). Methods for extracting genomic DNA from whole blood samples: Current perspectives. Journal of Biorepository Science for Applied Medicine, 2, 1–9.
EliehAliKomi, D., Sadeghi-Shabestari, M., Shanebandi, D., Babaloo, Z., Razavi, A., Sadigh-Eteghad, S., & Kazemi, T. (2019). Investigation of chitinase3like-1 (Chiti3L1) gene polymorphism (rs4950928) with susceptibility to allergic asthma in Iranian Northwestern Azeri population. Research in Molecular Medicine, 7, 17–24.
Aslanian-Kalkhoran, L., Elieh-Ali-Komi, D., Sadeghi-Shabestari, M., Shanebandi, D., Babaloo, Z., Razavi, A., Sadigh-Eteghad, S., & Kazemi, T. (2017). Investigation of Fc receptor-like 3 (FCRL-3) gene polymorphism (rs7528684) with susceptibility to allergic asthma in Iranian North-Western Azeri population. Clinical Laboratory, 63, 1301–1305.
Rybakowski, J. K. (2009). Matrix metalloproteinase-9 (MMP9)—A mediating enzyme in cardiovascular disease, cancer, and neuropsychiatric disorders. Cardiovascular Psychiatry and Neurology, 2009, 904836.
Fanjul-Fernández, M., Folgueras, A. R., Cabrera, S., & López-Otín, C. (2010). Matrix metalloproteinases: Evolution, gene regulation and functional analysis in mouse models. Biochimica et Biophysica Acta, 1803, 3–19.
Bahrehmand, F., Vaisi-Raygani, A., Kiani, A., Rahimi, Z., Tavilani, H., Ardalan, M., Vaisi-Raygani, H., Shakiba, E., & Pourmotabbed, T. (2015). Matrix metalloproteinase 9 polymorphisms and systemic lupus erythematosus: Correlation with systemic inflammatory markers and oxidative stress. Lupus, 24, 597–605.
Lehmann, D. J., Williams, J., McBroom, J., & Smith, A. D. (2001). Using meta-analysis to explain the diversity of results in genetic studies of late-onset Alzheimer’s disease and to identify high-risk subgroups. Neuroscience, 108, 541–554.
Raygani, A. V., Zahrai, M., Soltanzadeh, A., Doosti, M., Javadi, E., & Pourmotabbed, T. (2004). Analysis of association between butyrylcholinesterase K variant and apolipoprotein E genotypes in Alzheimer’s disease. Neuroscience Letters, 371, 142–146.
Shahmohamadnejad, S., Vaisi-Raygani, A., Shakiba, Y., Kiani, A., Rahimi, Z., Bahrehmand, F., Shakiba, E., & Pourmotabbed, T. (2015). Association between butyrylcholinesterase activity and phenotypes, paraoxonase192 rs662 gene polymorphism and their enzymatic activity with severity of rheumatoid arthritis: Correlation with systemic inflammatory markers and oxidative stress, preliminary report. Clinical Biochemistry, 48, 63–69.
Wågsäter, D., Zhu, C., Björkegren, J., Skogsberg, J., & Eriksson, P. (2011). MMP-2 and MMP-9 are prominent matrix metalloproteinases during atherosclerosis development in the Ldlr(−/−)Apob(100/100) mouse. International Journal of Molecular Medicine, 28, 247–253.
Soliman, A. R., Sadek, K. M., Thabet, K. K., Ahmed, D. H., & Mohamed, O. M. (2019). The role of matrix metalloproteinases 2 in atherosclerosis of patients with chronic kidney disease in type 2 diabetes. Saudi Journal of Kidney Diseases and Transplantation, 30, 387–393.
Qin, X., Corriere, M. A., Matrisian, L. M., & Guzman, R. J. (2006). Matrix metalloproteinase inhibition attenuates aortic calcification. Arteriosclerosis, Thrombosis, and Vascular Biology, 26, 1510–1516.
Liu, R., Chen, B., Chen, J., & Lan, J. (2018). Leptin upregulates smooth muscle cell expression of MMP-9 to promote plaque destabilization by activating AP-1 via the leptin receptor/MAPK/ERK signaling pathways. Experimental and Therapeutic Medicine, 16, 5327–5333.
Kieffer, P., Giummelly, P., Schjoth, B., Carteaux, J. P., Villemot, J. P., Hornebeck, W., & Atkinson, J. (2001). Activation of metalloproteinase-2, loss of matrix scleroprotein content and coronary artery calcification. Atherosclerosis, 157, 251–254.
Harendza, S., Lovett, D. H., Panzer, U., Lukacs, Z., Kuhnl, P., & Stahl, R. A. (2003). Linked common polymorphisms in the gelatinase a promoter are associated with diminished transcriptional response to estrogen and genetic fitness. The Journal of Biological Chemistry, 278, 20490–20499.
Dofara, S. G., Chang, S. L., & Diorio, C. (2020). Gene polymorphisms and circulating levels of MMP-2 and MMP-9: A review of their role in breast cancer risk. Anticancer Research, 40, 3619–3631.
Zhen, G. D., Zhao, L. B., Wu, S. S., Chen, M. Y., Li, Z. H., Zhou, S. Z., & Li, Z. F. (2017). Associations of MMP-2 and MMP-9 gene polymorphism with ulinastatin efficacy in patients with severe acute pancreatitis. Bioscience Reports, 37, 4.
Rollin, J., Régina, S., Vourc’h, P., Iochmann, S., Bléchet, C., Reverdiau, P., & Gruel, Y. (2007). Influence of MMP-2 and MMP-9 promoter polymorphisms on gene expression and clinical outcome of non-small cell lung cancer. Lung Cancer (Amsterdam, Netherlands), 56, 273–280.
Hua, Y., Song, L., Wu, N., Lu, X., Meng, X., Gu, D., & Yang, Y. (2009). Polymorphisms of MMP-2 gene are associated with systolic heart failure risk in Han Chinese. The American Journal of the Medical Sciences, 337, 344–348.
Beber, A. R., Polina, E. R., Biolo, A., Santos, B. L., Gomes, D. C., La Porta, V. L., Olsen, V., Clausell, N., Rohde, L. E., & Santos, K. G. (2016). Matrix metalloproteinase-2 polymorphisms in chronic heart failure: Relationship with susceptibility and long-term survival. PLoS ONE, 11, e0161666.
Pérez-Hernández, N., Vargas-Alarcón, G., Martínez-Rodríguez, N., Martínez-Ríos, M. A., Peña-Duque, M. A., Peña-Díaz Ade, L., Valente-Acosta, B., Posadas-Romero, C., Medina, A., & Rodríguez-Pérez, J. M. (2012). The matrix metalloproteinase 2–1575 gene polymorphism is associated with the risk of developing myocardial infarction in Mexican patients. Journal of Atherosclerosis and Thrombosis, 19, 718–727.
Wu, H. D., Bai, X., Chen, D. M., Cao, H. Y., & Qin, L. (2013). Association of genetic polymorphisms in matrix metalloproteinase-9 and coronary artery disease in the Chinese Han population: A case–control study. Genetic Testing and Molecular Biomarkers, 17, 707–712.
Saedi, M., Vaisi-Raygani, A., Khaghani, S., Shariftabrizi, A., Rezaie, M., Pasalar, P., Rahimi, Z., & Pourmotabbed, T. (2012). Matrix metalloproteinase-9 functional promoter polymorphism 1562C>T increased risk of early-onset coronary artery disease. Molecular Biology Reports, 39, 555–562.
Bahrehmand, F., Vaisi-Raygani, A., Kiani, A., Rahimi, Z., Tavilani, H., Navabi, S. J., Shakiba, E., Hassanzadeh, N., & Pourmotabbed, T. (2012). Matrix metalloproteinase-2 functional promoter polymorphism G1575A is associated with elevated circulatory MMP-2 levels and increased risk of cardiovascular disease in systemic lupus erythematosus patients. Lupus, 21, 616–624.
Reynolds, J. J. (1996). Collagenases and tissue inhibitors of metalloproteinases: A functional balance in tissue degradation. Oral Diseases, 2, 70–76.
Elieh Ali Komi, D., & Bjermer, L. (2019). Mast cell-mediated orchestration of the immune responses in human allergic asthma: Current insights. Clinical Reviews in Allergy & Immunology, 56, 234–247.
Acknowledgements
This work was performed in partial fulfillment of the requirements for the biochemistry MSc thesis of Saeed Elahirad, in the School of Medicine, Kermanshah University of Medical Sciences Kermanshah, Iran. The authors gratefully acknowledge the Research Council of Kermanshah University of Medical Sciences (Grant Number 95294) for financial support.
Funding
This work was supported by the Research Council of Kermanshah University of Medical Sciences (Grant No.: 95294).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by SE, DEAK, and AK. The first draft of the manuscript was written by AK and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical Approval
This study was approved by the ethics committee of Kermanshah Medical University (EC. 95294). All patients signed a consent form.
Consent for Publication
Patients signed informed consent regarding publishing their data and photographs.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Handling Editor: Y. Robert Li.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Elahirad, S., Elieh Ali Komi, D., Kiani, A. et al. Association of Matrix Metalloproteinase-2 (MMP-2) and MMP-9 Promoter Polymorphisms, Their Serum Levels, and Activities with Coronary Artery Calcification (CAC) in an Iranian Population. Cardiovasc Toxicol 22, 118–129 (2022). https://doi.org/10.1007/s12012-021-09707-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-021-09707-5