Abstract
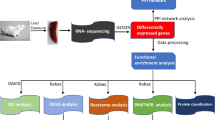
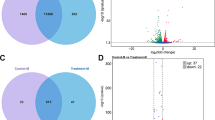
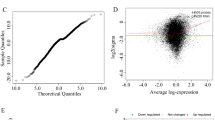
Lead (Pb), a widespread heavy metal, causes severe toxicity in human and animal organs (e.g., bone marrow), whereas the mechanisms of the bone marrow toxicity induced by Pb exposure are unclear. Hence, this study was designed to reveal the hub genes involved in Pb-induced bone marrow toxicity. GSE59894 dataset obtained from Gene Expression Omnibus (GEO) was composed of lead acetate (PbAc2)-treated and control bone marrow samples. Totally 120 and 85 differentially expressed genes (DEGs) were identified on the 1st day, while 153 and 157 DEGs on the 3rd day in the bone marrow treated with 200 and 600 mg/kg of PbAc2, respectively. Notably, a total of 28 and 32 overlapping DEGs were identified in the bone marrow on the 1st and 3rd day treated with PbAc2, respectively. Biological process analysis suggested that the common DEGs were primarily participated in cell differentiation, the response to drug, xenobiotic stimulus, and organic cyclic compound. Pathway analysis demonstrated that the overlapping DEGs were primarily linked to PI3K-Akt, TGF-β, MAPK, and osteoclast differentiation signaling pathways. Moreover, the hub genes, including PLD2, DAPK1, ALB, TNF, FOS, CDKN1A, and TGFB3, might contribute to PbAc2-induced bone marrow toxicity. Overall, our study offers an important insight into the molecular mechanisms of Pb-induced bone marrow toxicity.













Similar content being viewed by others
Data Availability
All data of the present article are included in Supplementary Information files or in the main text.
References
Jafarzadeh E, Soodi M, Tiraihi T, Zarei M, Qasemian-Lemraski M (2022) Study of lead-induced neurotoxicity in cholinergic cells differentiated from bone marrow-derived mesenchymal stem cells. Toxicol Ind Health 38:655–664
Okesola MA, Ajiboye BO, Oyinloye BE, Ojo OA (2019) Effect of Zingiber officinale on some biochemical parameters and cytogenic analysis in lead-induced toxicity in experimental rats. Toxicol Mech Method 29:255–262
Sheng ZJ, Wang S, Zhang X, Li XY, Li BY, Zhang ZL (2020) Long-term exposure to low-dose lead induced deterioration in bone microstructure of male mice. Biol Trace Elem Res 195:491–498
Rafiei H, Shariati M, Khayatzadeh J, Afsharnezhad S, Farhoodi M (2018) Effects of oral dosage of lead acetate II on osteocalcin gene expression in rat mesenchymal stem cells. Rep Biochem Mol Biol 6:131–136
Suljevic D, Handzic N, Focak M, Lasic I, Sipovic F, Sulejmanovic J, Begic S, Alijagic A (2020) Lead exposure influences serum biomarkers, hepatocyte survival, bone marrow hematopoiesis, and the reproductive cycle in Japanese quails. Biol Trace Elem Res 199:1574–1583
Lu HK, Yuan GP, Yin ZQ, Dai SJ, Jia RY, Xu J, Song X, Li L, Lv C (2014) Effects of subchronic exposure to lead acetate and cadmium chloride on rat’s bone: Ca and Pi contents, bone density, and histopathological evaluation. Int J Clin Exp Patho 7:640–647
Beier EE, Holz JD, Sheu TJ, Puzas JE (2016) Elevated lifetime lead exposure impedes osteoclast activity and produces an increase in bone mass in adolescent mice. Toxicol Sci 149:277–288
Qi SS, Zheng HX, Chen C, Jiang H (2019) Du-Zhong (Eucommia ulmoides oliv.) cortex extract alleviates lead acetate-induced bone loss in rats. Biol. Trace Elem. Res. 187:172–180
Bich VNT, Hongu T, Miura Y, Katagiri N, Ohbayashi N, Yamashita-Kanemaru Y, Shibuya A, Funakoshi Y, Kanaho Y (2018) Physiological function of phospholipase D2 in anti-tumor immunity: regulation of CD8(+) T lymphocyte proliferation. Sci Rep 8:6283
Zhou GX, Yu L, Yang WJ, Wu W, Fang LL, Liu ZJ (2016) Blockade of PLD2 ameliorates intestinal mucosal inflammation of inflammatory bowel disease. Mediat Inflamm 2016:2543070
Ganesan R, Henkels KM, Wrenshall LE, Kanaho Y, Paolo G, Frohman MA, Gomez-Cambronero J (2018) Oxidized LDL phagocytosis during foam cell formation in atherosclerotic plaques relies on a PLD2-CD36 functional interdependence. J Leukocyte Biol 103:867–883
Wang S, Mi RJ, Cai ZP, Wang ZM, Zeng CY, Xie ZY, Li JT, Ma MJ, Liu WJ, Su HJ et al (2022) DAPK1 interacts with the p38 isoform MAPK14, preventing its nuclear translocation and stimulation of bone marrow adipogenesis. Stem Cells 40:508–522
Wang S, Su HJ, Feng P, Deng W, Su CY, Wu YF, Shen HY (2020) Loss of death-associated protein kinase 1 in human bone marrow mesenchymal stem cells decreases immunosuppression of CD4+T cells. J Int Med Res 48:0300060520933453
Chen KM, Jiang T, Zeng QS, Wang SF, Li L (2022) Bone marrow mesenchymal stem co-culture inhibited the proliferation of endometrial cancer cells by upregulating miR-141-3p/death associated protein kinase 1 (DAPK1) axis. J Biomater Tiss Eng 12:1314–1319
Wang N, Desai A, Ge B, Li WY, Jin XH, Bai HZ, Yu K, Ye HG (2020) Prognostic value of hypoalbuminemia at diagnosis in de novo non-M3 acute myeloid leukemia. Leukemia Lymphoma 61:641–649
Shabestari M, Shabestari YR, Landin MA, Pepaj M, Cleland TP, Reseland JE, Eriksen EF (2020) Altered protein levels in bone marrow lesions of hip osteoarthritis: Analysis by proteomics and multiplex immunoassays. Int J Rheum Dis 23:788–799
Wu XL, Hou QH, Zhao ZY, Wang J, Guo YZ, Lu LG, Han J (2022) Effects of soy-whey protein nutritional supplementation on hematopoiesis and immune reconstitution in an allogeneic transplanted mice. Nutrients 14:3014
Wu LZ, Zhang GR, Guo CB, Zhao XY, Shen DY, Yang N (2020) MiR-128-3p mediates TNF-alpha-induced inflammatory responses by regulating Sirt1 expression in bone marrow mesenchymal stem cells. Biochem Biophys Res Commun 521:98–105
Manso BA, Krull JE, Gwin KA, Lothert PK, Welch BM, Novak AJ, Parikh SA, Kay NE, Medina KL (2021) Chronic lymphocytic leukemia B-cell-derived TNF alpha impairs bone marrow myelopoiesis. Iscience 24:101994
Aguilar G, Cordova F, Koning T, Sarmiento J, Boric MP, Birukov K, Cancino J, Varas-Godoy M, Soza A, Alves NG et al (2021) TNF-alpha-activated eNOS signaling increases leukocyte adhesion through the S- nitrosylation. Am J Physiol Heart Circ Physiol 321:H1083–H1095
Morris EV, Suchacki KJ, Hocking J, Cartwright R, Sowman A, Gamez B, Lea R, Drake MT, Cawthorn WP, Edwards CM (2020) Myeloma cells down-regulate adiponectin in bone marrow adipocytes via TNF-alpha. J Bone Miner Res 35:942–955
Yang FH, Jia YS, Sun Q, Zheng CY, Liu CY, Wang W, Du L, Kang SQ, Niu XF, Li JY (2020) Raloxifene improves TNF-alpha-induced osteogenic differentiation inhibition of bone marrow mesenchymal stem cells and alleviates osteoporosis. Exp Ther Med 20:309–314
Song YM, Hu SL, Zhang JL, Zhu L, Zhao XR, Chen QP, Zhang JH, Bai Y, Pan Y, Shao CL (2021) Fractionated irradiation of right thorax induces abscopal damage on bone marrow cells via TNF-alpha and SAA. Int J Mol Sci 22:9964
Fan P, Yu XY, Chen CH, Gao JW, Xu YZ, Xie XH, Wang YT (2022) Parkin-mediated mitophagy protects against TNF-?-induced stress in bone marrow mesenchymal stem cells. Exp Gerontol 164:111829
Bao WR, Zhang QW, Zheng HM, Li LF, Liu M, Cheng HY, Wong TL, Zhang G, Lu AP, Bian ZX et al (2021) Radix Astragali polysaccharide RAP directly protects hematopoietic stem cells from chemotherapy-induced myelosuppression by increasing FOS expression. Int J Biol Macromol 183:1715–1722
Zhang YF, Yang M, Zhang S, Yang ZQ, Zhu YF, Wang Y, Chen Z, Lv X, Huang Z, Xie YL et al (2022) BHLHE40 promotes osteoclastogenesis and abnormal bone resorption via c-Fos/NFATc1. Cell Biosci 12:20
Jeong S, Seong JH, Kang JH, Lee DS, Yim M (2021) Dynamin-related protein 1 positively regulates osteoclast differentiation and bone loss. FEBS Lett 595:58–67
Juran CM, Zvirblyte J, Cheng-Campbell M, Blaber EA, Almeida EAC (2021) CDKN1A deletion or suppression by cyclic stretch enhance the osteogenic potential of bone marrow mesenchymal stem cell-derived cultures. Stem Cell Res 56:102513
Yang ZY, Liu X, Wang LG, Wang T, Chen YQ, Teng XM, Li JJ, Shao LB, Hui J, Ye WX et al (2020) The protective effects of HMGA2 in the senescence process of bone marrow-derived mesenchymal stromal cells. J Tissue Eng Regen Med 14:588–599
Luo Y, Liang C, Liu Y, Liu XP, Xu Y (2020) RXR alpha and MRTF-A have a synergistic effect in the retinoic acid-induced neural-like differentiation of adult bone marrow-derived mesenchymal stem cells. Cell Biol Int 44:1373–1381
Hiew VV, Teoh PL (2022) Collagen modulates the biological characteristics of WJ-MSCs in basal and osteoinduced conditions. Stem Cells Int 2022:2116367
Samsonraj RM, Dudakovic A, Manzar B, Sen B, Dietz AB, Cool SM, Rubin J, van Wijnen AJ (2018) Osteogenic stimulation of human adipose-derived mesenchymal stem cells using a fungal metabolite that suppresses the polycomb group protein EZH2. Stem Cell Transl Med 7:197–209
Du GF, Cheng XY, Zhang Z, Han LJ, Wu KL, Li YJ, Lin XS (2021) TGF-beta induced key genes of osteogenic and adipogenic differentiation in human mesenchymal stem cells and miRNA-mRNA regulatory networks. Front Genet 12:759596
Liang XY, Hou YF, Han LJ, Yu SX, Zhang YY, Cao XM, Yan JS (2021) ELMO1 regulates RANKL-stimulated differentiation and bone resorption of osteoclasts. Front Cell Dev Biol 9:702916
Zhang YL, Liu L, Su YW, Xian CRYJ (2022) miR-6315 attenuates methotrexate treatment-induced decreased osteogenesis and increased adipogenesis potentially through modulating TGF-beta/Smad2 signalling. Biomedicines 9:926
Ma YG, Ran D, Cao Y, Zhao HY, Song RL, Zou H, Gu JH, Yuan Y, Bian JC, Zhu JQ et al (2021) The effect of P2X7 on cadmium-induced osteoporosis in mice. J Hazard Mater 405:124251
Zhu XJ, He Y, Zhang QY, Ma DR, Zhao HF (2023) Lead induced disorders of lipid metabolism and glycometabolism in the liver of developmental Japanese quails (Coturnix japonica) via inhibiting PI3K/Akt signaling pathway. Comp Biochem Physiol C Toxicol Pharmacol 263:109489
Zhao ZH, Du KJ, Wang T, Wang JY, Cao ZP, Chen XM, Song H, Zheng G, Shen XF (2021) Maternal lead exposure impairs offspring learning and memory via decreased GLUT4 membrane translocation. Front Cell Dev Biol 9:648261
Fiorim J, Simoes MR, de Azevedo BF, Ribeiro RF, dos Santos L, Padilha AS, Vassallo DV (2020) Increased endothelial nitric oxide production after low level lead exposure in rats involves activation of angiotensin II receptors and PI3K/Akt pathway. Toxicology 443:152557
Abou-Ezzi G, Supakorndej T, Zhang JZ, Anthony B, Krambs J, Celik H, Karpova D, Craft CS, Link DC (2019) TGF-beta signaling plays an essential role in the lineage specification of mesenchymal stem/progenitor cells in fetal bone marrow. Stem Cell Rep 13:48–60
Zhang J, Qin XL, Deng YF, Lu J, Li ZD, Feng Y, Yan X, Chen MJ, Gao L, Xu Y et al (2021) Transforming growth factor-beta 1 enhances mesenchymal characteristics of Buffalo (Bubalus bubalis) bone marrow-derived mesenchymal stem cells. Cell Reprogram 23:127–138
Bataller A, Montalban-Bravo G, Soltysiak KA, Garcia-Manero G (2019) The role of TGF beta in hematopoiesis and myeloid disorders. Leukemia 33:1076–1089
Zhang JH, Mo L, Huang HR, Xu JK, Fan YN, Li WF, Wang HB, Zhou C, Fang HJ, He W et al (2022) Loureirin B downregulates osteoclast differentiation of bone marrow macrophages by targeting the MAPK signaling pathway. Sci Rep 12:14382
Li L, Feng J, Sun L, Xuan YW, Wen L, Li YX, Yang S, Zhu BA, Tian XY, Li S et al (2022) Cannabidiol promotes osteogenic differentiation of bone marrow mesenchymal stem cells in the inflammatory microenvironment via the CB2-dependent p38 MAPK signaling pathway. Int J Stem Cells 15:405–414
Jiang YX, Xin N, Xiong Y, Guo YJ, Yuan Y, Zhang Q, Gong P (2022) Alpha CGRP regulates osteogenic differentiation of bone marrow mesenchymal stem cells through ERK1/2 and p38 MAPK signaling pathways. Cell Transplant 31:09636897221107636
Wang B, Gong S, Han LZ, Shao WK, Li ZL, Xu JW, Lv X, Xiao BJ, Feng Y (2022) Knockdown of HDAC9 inhibits osteogenic differentiation of human bone marrow mesenchymal stem cells partially by suppressing the MAPK signaling pathway. Clin Interv Aging 17:777–787
Ganter B, Tugendreich S, Pearson CI, Ayanoglu E, Baumhueter S, Bostian KA, Brady L, Browne LJ, Calvin JT, Day GJ et al (2005) Development of a large-scale chemogenomics database to improve drug candidate selection and to understand mechanisms of chemical toxicity and action. J Biotechnol 119:219–244
Funding
This study was supported by The Open Project of Anhui Province Key Laboratory of Embryo Development and Reproductive Regulation (No. FSKFKT011), Talent Introduction Program of Anhui Science and Technology University (No. DKYJ202003), The Open Project of Anhui Province Key Laboratory of Wetland Ecosystem Protection and Restoration (No. AHZDSYS2019-01), Natural Science Foundation of Anhui Provincial Education Department (No. KJ2020A0083) and The Open Project of Longyan University & Fujian Provincial Key Laboratory for Prevention and Control of Animal Infectious Diseases and Biotechnology (No. ZDSYS2020004).
Author information
Authors and Affiliations
Contributions
XF Li designed the study, prepared the figures and analyzed the results. B Yang prepared the tables and wrote the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
12011_2023_3733_MOESM10_ESM.xlsx
Supplementary file10 The overlapping DEGs identified in the bone marrow on the 1st and 3rd day treated with PbAc600 (XLSX 10 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, B., Li, X. Unveiling the Mechanisms of Bone Marrow Toxicity Induced by Lead Acetate Exposure. Biol Trace Elem Res 202, 1041–1066 (2024). https://doi.org/10.1007/s12011-023-03733-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-023-03733-w