Abstract
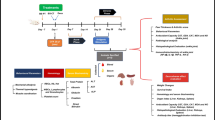
The study aimed to evaluate the therapeutic effect of boric acid (BA) in experimentally induced septic arthritis. A total of 30 rats, 6 rats in each group (5 groups), were used in the study. No treatment was applied to the rats in the control group. Only BA was administered intraperitoneally (IP) to the rats in the bor group. Escherichia coli was administered at a single dose of 25 μL, 1 × 1010 cfu/rat from the right foot pad of the rats, via intra-articular route, to the mice in the arthritis, arthritis-bor, and arthritis-antb groups. Then, BA at a dose of 50 mg/kg and cefazolin at a dose of 25 mg/kg were administered to the rats in the arthritis-bor and arthritis-antb groups, respectively, for 7 days via the IP route. At the end of the study, all animals were euthanized following the ethical rules. Blood and tissue samples were taken from the rats for biochemical and histopathological analyses. The levels of GSH, MDA, Endoglin, Endocan, and TNF-β markers were measured in the blood samples taken. A significant decrease was observed in MDA and Endoglin levels in the boric acid–administered group compared with the arthritis group, while a significant increase was observed at the GSH level. Histopathologically, it was determined that the reactive surrounding tissue response in the bor group was significantly reduced. As a result, a significant decrease in inflammation was found biochemically and histopathologically in the groups treated with BA.


Similar content being viewed by others
Change history
07 February 2022
A Correction to this paper has been published: https://doi.org/10.1007/s12011-022-03130-9
References
Gottlieb M, Holladay D, Rice M (2019) Current approach to the evaluation and management of septic arthritis. Pediatr Emerg Care 35:509–513
Hassan AS, Rao A, Manadan AM, Block JA (2017) Peripheral bacterial septic arthritis: review of diagnosis and management. JCR J Clin Rheumatol 23:435–442
Kromann NC, Johansen ME, Hvolris J (2017) Septic arthritis. Ugeskr Laeger 179(3):2–6
Agarwal A, Aggarwal AN (2016) Bone and joint infections in children: septic arthritis. Indian J Pediatr 83:825–833
Brown DW, Sheffer BW (2019) Pediatric septic arthritis: an update. Orthop Clin 50:461–470
Wall C, Donnan L (2015) Septic arthritis in children. Aust Fam Physician 44:213–215
Cohen E, Katz T, Rahamim E et al (2020) Septic arthritis in children: Updated epidemiologic, microbiologic, clinical and therapeutic correlations. Pediatr Neonatol 61:325–330
NI Montgomery HR Epps 2017 Pediatric septic arthritis OrthopClin 48 209 216
Carpenter CR, Schuur JD, Everett WW, Pines JM (2011) Evidence-based diagnostics: adult septic arthritis. Acad Emerg Med 18:781–796
García-Arias M, Balsa A, Mola EM (2011) Septic arthritis. Best Pract Res Clin Rheumatol 25:407–421. https://doi.org/10.1016/j.berh.2011.02.001
Mathew AJ, Ravindran V (2014) Infections and arthritis. Best Pract Res Clin Rheumatol 28:935–959
Johnson JR, Gajewski A, Lesse AJ, Russo TA (2003) Extraintestinal pathogenic Escherichia coli as a cause of invasive nonurinary infections. J Clin Microbiol 41:5798
Wasiński B (2019) Extra-intestinal pathogenic Escherichia coli–threat connected with food-borne infections. Ann Agric Environ Med 26:532–537
Gaußmann B, Hess C, Grafl B et al (2018) Escherichia coli isolates from femoral bone marrow of broilers exhibit diverse pheno-and genotypic characteristics that do not correlate with macroscopic lesions of bacterial chondronecrosis with osteomyelitis. Avian Pathol 47:271–280
Hamzaoui A, Salem R, Koubaa M et al (2009) Escherichia coli osteomyelitis of the ischium in an adult. Orthop Traumatol Surg Res 95:636–638
Marcos Sánchez F, Aragón Díez A, Arbol Linde F, et al (2004) [Vertebral osteomyelitis caused by E. coli]. An Med Interna Madr Spain 1984 21 43 44.
Matsuura H, Sue M, Takahara M, Kuninaga N (2019) Escherichia coli rib osteomyelitis. QJM 112:35–36
Moustafa A, Kheireldine R, Khan Z, et al (2019) Cervical spinal osteomyelitis with epidural abscess following an Escherichia coli urinary tract infection in an immunocompetent host. Case Rep Infect Dis 2019:
Xie Z, Cui X, Zhao C et al (2013) Gentamicin-loaded borate bioactive glass eradicates osteomyelitis due to Escherichia coli in a rabbit model. Antimicrob Agents Chemother 57:3293
Braga JFV, Chanteloup NK, Trotereau A et al (2016) Diversity of Escherichia coli strains involved in vertebral osteomyelitis and arthritis in broilers in Brazil. BMC Vet Res 12:1–12
Mathews CJ, Weston VC, Jones A et al (2010) Bacterial septic arthritis in adults. The Lancet 375:846–855
Acaroz U, Ince S, Arslan-Acaroz D et al (2018) The ameliorative effects of boron against acrylamide-induced oxidative stress, inflammatory response, and metabolic changes in rats. Food Chem Toxicol 118:745–752
Arslan-Acaroz D, Bayşu-Sozbilir N (2020) Ameliorative effect of boric acid against formaldehyde-induced oxidative stress in A549 cell lines. Environ Sci Pollut Res 27:4067–4074
Ince S, Kucukkurt I, Acaroz U, et al (2019) Boron ameliorates arsenic-induced DNA damage, proinflammatory cytokine gene expressions, oxidant/antioxidant status, and biochemical parameters in rats. J Biochem Mol Toxicol 33:e22252
Nielsen FH (2014) Update on human health effects of boron. J Trace Elem Med Biol 28:383–387
Brittingham A, Wilson WA (2014) The antimicrobial effect of boric acid on Trichomonas vaginalis. Sex Transm Dis 41:718–722
Haesebrouck F, Baele M, De Keyser H et al (2009) Antimicrobial activity of an acetic and boric acid solution against Staphylococcus pseudintermedius. Vlaams Diergeneeskd Tijdschr 78:89–90
Beutler E, Duron O, Kelly B (1963) Improved method for the determination of blood glutathione. J Lab Clin Med 61:882–888
Yoshioka T, Kawada K, Shimada T, Mori M (1979) Lipid peroxidation in maternal and cord blood and protective mechanisms. Am J Obstet Gynecol 135:972–976
Castellazzi L, Mantero M, Esposito S (2016) Update on the management of pediatric acute osteomyelitis and septic arthritis. Int J Mol Sci 17:855
Arnold JC, Bradley JS (2015) Osteoarticular infections in children. Infect Dis Clin 29:557–574
Mellata M (2013) Human and avian extraintestinal pathogenic Escherichia coli: infections, zoonotic risks, and antibiotic resistance trends. Foodborne Pathog Dis 10:916–932
Ergönül Ö, Aydin M, Azap A et al (2016) Healthcare-associated Gram-negative bloodstream infections: antibiotic resistance and predictors of mortality. J Hosp Infect 94:381–385
Lefebvre M-A, Quach C, Daniel SJ (2015) Chronic suppurative otitis media due to nontuberculous mycobacteria: a case of successful treatment with topical boric acid. Int J Pediatr Otorhinolaryngol 79:1158–1160
Schmidt M, Schaumberg JZ, Steen CM, Boyer MP (2010) Boric acid disturbs cell wall synthesis in Saccharomyces cerevisiae. Int J Microbiol 2010:930465
Güzel Y, Golge UH, Goksel F et al (2016) The efficacy of boric acid used to treat experimental osteomyelitis caused by methicillin-resistant Staphylococcus aureus: an in vivo study. Biol Trace Elem Res 173:384–389
Saito T, Bokhove M, Croci R et al (2017) Structural basis of the human endoglin-BMP9 interaction: insights into BMP signaling and HHT1. Cell Rep 19:1917–1928
Altomonte M, Montagner R, Fonsatti E et al (1996) Expression and structural features of endoglin (CD105), a transforming growth factor β 1 and β 3 binding protein, in human melanoma. Br J Cancer 74:1586–1591
Barbara NP, Wrana JL, Letarte M (1999) Endoglin is an accessory protein that interacts with the signaling receptor complex of multiple members of the transforming growth factor-β superfamily. J Biol Chem 274:584–594
Lassalle P, Molet S, Janin A et al (1996) ESM-1 is a novel human endothelial cell-specific molecule expressed in lung and regulated by cytokines. J Biol Chem 271:20458–20464
Scherpereel A, Depontieu F, Grigoriu B et al (2006) Endocan, a new endothelial marker in human sepsis. Crit Care Med 34:532–537
Kali A, Shetty KR (2014) Endocan: a novel circulating proteoglycan. Indian J Pharmacol 46:579
Takaoka Y, Abe Y, Haraguchi R, Kito K (2010) Lymphotoxin (TNF-beta). Nihon Rinsho Jpn J Clin Med 68:93–95
Calmon-Hamaty F, Combe B, Hahne M, Morel J (2011) Lymphotoxin α revisited: general features and implications in rheumatoid arthritis. Arthritis Res Ther 13:1–5
Ruddle NH (2014) Lymphotoxin and TNF: how it all began—a tribute to the travelers. Cytokine Growth Factor Rev 25:83–89
Aggarwal BB, Gupta SC, Kim JH (2012) Historical perspectives on tumor necrosis factor and its superfamily: 25 years later, a golden journey. Blood J Am Soc Hematol 119:651–665
Buch MH, Conaghan PG, Quinn MA et al (2004) True infliximab resistance in rheumatoid arthritis: a role for lymphotoxin α? Ann Rheum Dis 63:1344–1346
O’Rourke KP, O’Donoghue G, Adams C et al (2008) High levels of Lymphotoxin-Beta (LT-Beta) gene expression in rheumatoid arthritis synovium: clinical and cytokine correlations. Rheumatol Int 28:979–986
Chiang EY, Kolumam GA, Yu X et al (2009) Targeted depletion of lymphotoxin-α–expressing TH 1 and TH 17 cells inhibits autoimmune disease. Nat Med 15:766–773
Guis S, Balandraud N, Bouvenot J et al (2007) Influence of- 308 A/G polymorphism in the tumor necrosis factor α gene on etanercept treatment in rheumatoid arthritis. Arthritis Care Res 57:1426–1430
Mugnier B, Balandraud N, Darque A et al (2003) Polymorphism at position- 308 of the tumor necrosis factor α gene influences outcome of infliximab therapy in rheumatoid arthritis. Arthritis Rheum Off J Am Coll Rheumatol 48:1849–1852
Seitz M, Wirthmüller U, Möller B, Villiger P (2007) The- 308 tumour necrosis factor-α gene polymorphism predicts therapeutic response to TNFα-blockers in rheumatoid arthritis and spondyloarthritis patients. Rheumatology 46:93–96
Eroğlu HA, Makav M, Adali Y, Citil M (2020) Effects of ozone and L-carnitine on kidney MDA, GSH, and GSHPx levels in acetaminophen toxicity. Kafkas Üniversitesi Vet Fakültesi Derg 26(1):127–134
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yıldız, K., Makav, M., Adalı, Y. et al. Therapeutic Effects of Boric Acid in a Septic Arthritis Model Induced by Escherichia coli in Rats. Biol Trace Elem Res 200, 4762–4770 (2022). https://doi.org/10.1007/s12011-021-03065-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-021-03065-7