Abstract
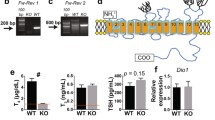
It is well known that excess iodide can lead to thyroid colloid retention, a classic characteristic of iodide-induced goiter. However, the mechanism has not been fully unrevealed. Iodide plays an important role in thyroid function at multiple steps of thyroid colloid synthesis and transport among which sodium/iodide symporter (NIS) and pendrin are essential. In our study, we fed female BALB/c mice with different concentrations of high-iodine water including group A (control group, 0 μg/L), group B (1500 μg/L), group C (3000 μg/L), group D (6000 μg/L), and group E (12,000 μg/L). After 7 months of feeding, we found that excess iodide could lead to different degrees of thyroid colloid retention. Besides, NIS and pendrin expression were downregulated in the highest dose group. The thyroid iodide intake function detected by urine iodine assay and thyroidal 125I experiments showed that the urine level of iodine increased, while the iodine intake rate decreased when the concentration of iodide used in feeding water increased (all p < 0.05 vs. control group). In addition, transmission electron microscopy (TEM) indicated a reduction in the number of intracellular mitochondria of thyroid cells. Based on these findings, we concluded that the occurrence of thyroid colloid retention exacerbated by excess iodide was associated with the suppression of NIS and pendrin expression, providing an additional insight of the potential mechanism of action of excess iodide on thyroid gland.




Similar content being viewed by others
References
Braverman LE (1994) Iodine and the thyroid: 33 years of study. Thyroid 4:351–356
Kahaly GJ, Dienes HP, Beyer J, Hommel G (1998) Iodide induces thyroid autoimmunity in patients with endemic goitre: a randomised, double-blind, placebo-controlled trial. Eur J Endocrinol 139:290–297
Laurberg P, Pedersen KM, Hreidarsson A, Sigfusson N, Iversen E, Knudsen PR (1998) Iodine intake and the pattern of thyroid disorders: a comparative epidemiological study of thyroid abnormalities in the elderly in Iceland and in Jutland, Denmark. J Clin Endocrinol Metab 83:765–769
Laurberg P, Bulow Pedersen I, Knudsen N, Ovesen L, Andersen S (2001) Environmental iodine intake affects the type of nonmalignant thyroid disease. Thyroid 11:457–469
Roti E, Uberti ED (2001) Iodine excess and hyperthyroidism. Thyroid 11:493–500
Li Y, Teng D, Shan Z, Teng X, Guan H, Yu X, Fan C, Chong W, Yang F, Dai H, Gu X, Yu Y, Mao J, Zhao D, Li J, Chen Y, Yang R, Li C, Teng W (2008) Antithyroperoxidase and antithyroglobulin antibodies in a five-year follow-up survey of populations with different iodine intakes. J Clin Endocrinol Metab 93:1751–1757
Laurberg P, Cerqueira C, Ovesen L, Rasmussen LB, Perrild H, Andersen S, Pedersen IB, Carle A (2010) Iodine intake as a determinant of thyroid disorders in populations. Best Pract Res Clin Endocrinol Metab 24:13–27
Kohn LD, Saji M, Kosugi M, Ban T, Giuliani C, Hidaka A, Shimura H, Shimura Y, Okajima F (1993) The synthesis and secretion of thyroid hormones: regulation by multiple hormones and signals which can be subverted by autoantibodies to the thyrotropin receptor, thyroid diseases: basic science, pathology. Clin and Lab Diagn 1993:59–118
Carrasco N (1993) Iodide transport in the thyroid. Biochim Biophys Acta 1154:65–82
Everett LA, Glaser B, Beck JC, Idol JR, Buchs A, Heyman M, Adawi F, Hazani E, Nassir E, Baxevanis AD, Sheffield VC, Green ED (1997) Pendred syndrome is caused by mutations in a putative sulphate transport gene (PDS). Nat Genet 17:411–422
Scott DA, Wang R, Kreman TM, Sheffield VC, Karniski LP (1999) The Pendred syndrome gene encodes a chloride-iodide transport protein. Nat Genet 21:440–443
Dohan O, De la Vieja A, Paroder V, Riedel C, Artani M, Reed M, Ginter CS, Carrasco N (2003) The sodium/iodide symporter (NIS): characterization, regulation, and medical significance. Endocr Rev 24:48–77
Royaux IE, Suzuki K, Mori A, Katoh R, Everett LA, Kohn LD, Green ED (2000) Pendrin, the protein encoded by the Pendred syndrome gene (PDS), is an apical porter of iodide in the thyroid and is regulated by thyroglobulin in FRTL-5 cells. Endocrinology 141:839–845
Bizhanova A, Kopp P (2009) The sodium-iodide symporter NIS and pendrin in iodide homeostasis of the thyroid. Endocrinology 150:1084–1090
Gillam MP, Sidhaye AR, Lee EJ, Rutishauser J, Stephan CW, Kopp P (2004) Functional characterization of pendrin in apolarized cell system. Evidence for pendrin-mediated apical iodide efflux. J Biol Chem 279:13004–13010
Bidart JM, Mian C, Lazar V, Russo D, Filetti S, Caillou B, Schlumberger M (2000) Expression of pendrin and the Pendred syndrome (PDS) gene in human thyroid tissues. J Clin Endocrinol Metab 85:2028–2033
Fraser GR, Morgans ME, Trotter WR (1960) The syndrome of sporadic goitre and congenital deafness. Q J Med 29:279–295
Kopp P (1999) Pendred’s syndrome: clinical characteristics and molecular basis. Current Opin Endocrinol Diabetes 6:261–269
Calil-Silveira J, Serrano-Nascimento C, Nunes MT (2012) Iodide treatment acutely increases pendrin (SLC26A4) mRNA expression in the rat thyroid and the PCCl3 thyroid cell line by transcriptional mechanisms. Mol Cell Endocrinol 350:118–124
Kogai T, Endo T, Saito T, Miyazaki A, Kawaguchi A, Onaya T (1997) Regulation by thyroid-stimulating hormone of sodium/iodide symporter gene expression and protein levels in FRTL-5 cells. Endocrinology 138:2227–2232
Suzuki K, Mori A, Saito J, Moriyama E, Ullianich L, Kohn LD (1999) Follicular thyroglobulin suppresses iodide uptake by suppressing expression of the sodium/iodide symporter gene. Endocrinology 140:5422–5430
Wolff J, Chaikoff IL (1948) Plasma inorganic iodide as a homeostatic regulator of thyroid function. J Biol Chem 174:555–564
Wolff J, Chaikoff IL, Goldberg RC, Meier JR (1949) The temporary nature of the inhibitory action of excess iodine on organic iodine synthesis in the normal thyroid. Endocrinology 45:504–513
Braverman LE, Ingbar SH (1963) Changes in thyroidal function during adaptation to large doses of iodide. J Clin Invest 42:1216–1231
Chang DC, Wheeler MH, Woodcock JP, Curley I, Lazarus JR, Fung H, John R, Hall R, McGregor AM (1987) The effect of preoperative Lugol’s iodine on thyroid blood flow in patients with Graves’ hyperthyroidism. Surgery 102:1055–1061
Arntzenius AB, Smit LJ, Schipper J, van der Heide D, Meinders AE (1991) Inverse relation between iodine intake and thyroid blood flow: color Doppler flow imaging in euthyroid humans. J. Clin. Endocrinol Metab 73:1051–1055
Grollman EF, Smolar A, Ommaya A, Tombaccini D, Santisteban P (1986) Iodine suppression of iodide uptake in FRTL-5 thyroid cells. Endocrinology 118:2477–2482
Suzuki K, Kimura H, Wu H, Kudo N, Kim WB, Suzuki S, Yoshida A, Caturegli P, Kohn LD (2010) Excess iodide decreases transcription of NIS and VEGF genes inrat FRTL-5 thyroid cells. BBRC 393:286–290
Riedel C, Levy O, Carrasco N (2001) Post-transcriptional regulation of the sodium/iodide symporter by thyrotropin. J Biol Chem 276:21458–21463
Taylor JP, Metcalfe RA, Watson PF, Weetman AP, Trembath RC (2002) Mutations of the PDS gene, encoding pendrin, are associated with protein mislocalization and loss of iodide efflux: implications for thyroid dysfunction in Pendred syndrome. J Clin Endocrinol Metab 87:1778–1784
Yoshida A, Taniguchi S, Hisatome I, Royaux IE, Green ED, Kohn LD, Suzuki K (2002) Pendrin is an iodide-specific apical porter responsible for iodide efflux from thyroid cells. J Clin Endocrinol Metab 87:3356–3361
Yoshida A, Hisatome I, Taniguchi S, Sasaki N, Yamamoto Y, Miake J, Fukui H, Shimizu H, Okamura T, Okura T, Igawa O, Shigemasa C, Green ED, Kohn LD, Suzuki K (2004) Mechanism of iodide/chloride exchange by pendrin. Endocrinology 145:4301–4308
Joanta AE, Filip A, Clichici S, Andrei S, Daicoviciu D (2006) Iodide excess exerts oxidative stress in some target tissues of the thyroid hormones. Acta Physiol Hung Dec 93(4):347–359
Zhang N, Wang L, Duan Q, Lin L, Ahmed M, Wang T, Yao X (2015) Metallothionein-I/II knockout mice aggravate mitochondrial superoxide production and peroxiredoxin 3 expression in thyroid after excessive iodide exposure. Oxidative Med Cell Longev 2015:267027. doi:10.1155/2015/267027 Epub 2015 May 25
Zimmermann MB, Boelaert K (2015) Iodine deficiency and thyroid disorders. Lancet Diabetes Endocrinol. Apr 3(4):286–295
Acknowledgments
This work was supported by the National Natural Science Foundation of China (grant number 81373038) and the Doctor Starting Foundation of Guangzhou Medical University (grant number 2006GD059). The authors wish to acknowledge Mr. Hui-qiu Zhang and Yong-Jian Zhang for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Chen, Xy., Lin, Ch., Yang, Lh. et al. The Effect on Sodium/Iodide Symporter and Pendrin in Thyroid Colloid Retention Developed by Excess Iodide Intake. Biol Trace Elem Res 172, 193–200 (2016). https://doi.org/10.1007/s12011-015-0580-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-015-0580-4