Abstract
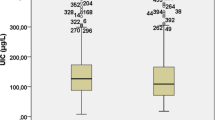
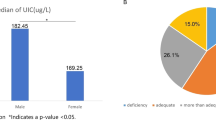
The objective was to determine the prevalence of iodine deficiency among hypothyroid patients and the effect of dietary goitrogens on indices of iodine and thyroid status. This is a case-control study of 106 subjects who were recruited from King Abdulaziz University Hospital, Jeddah. Blood and urine were collected for serum thyroid hormones, thyroid autoantibodies, thyroglobulin (Tg) and urinary iodine concentration (UIC). Dietary iodine and goitrogenic food intake were assessed by questionnaire. Using World Health Organization (WHO) cutoff values for UIC, both controls and cases were iodine deficient (85% and 83%, respectively). Furthermore, dietary iodine was deficient in 23% of controls and 36% of cases. In cases, there was a positive association between UIC levels and serum thyroid stimulating hormone (r = 0.405, p < 0.01) and a negative association with serum fT4 (r = −0.358, p < 0.01). Serum Tg antibody titers were also positively associated with dietary iodine (r = 0.328, p < 0.05). Patients with elevated serum autoantibodies had lower UIC and dietary iodine than those with normal serum autoantibodies. UIC was associated with dietary goitrogens including turnip (r = 0.280, p < 0.05) and pine (r = 0.289, p < 0.05) among cases. Iodine deficiency is common and the consumption of dietary goitrogens is high among euthyroid and hypothyroid subjects living in Jeddah.


Similar content being viewed by others
References
Clugston G, Benoist B. Eliminating iodine deficiency disorders. Bull World Health Organ 2002;80:341.
Li M, Ma G, Boyages S, et al. Re-emergence of iodine deficiency in Australia. Asia Pac J Clin Nutr 2001;10:200–3.
Dunn J, Van deer Haar F. Detection of ID. A practical guide to the correction of ID. Technical manual no. 3. The Netherlands: ICCIDD/UNICEF/WHO, 1990:13–20
Brauer V, Brauer W, Führer D, et al. Iodine Nutrition, Nodular Thyroid Disease, and Urinary Iodine Excretion in a German University Study Population. Thyroid 2005;15(4):364–70
Gons M, Kok J, Tegelaers W, et al. Concentration of plasma thyroglobulin and urinary excretion of iodinated material in the diagnosis of thyroid disorders in congenital hypothyroidism. Acta Endocrinol 1983;104(1):27–34
Aminorroaya A, Amini M, Rezvanian H, et al. Effects of iodized salt consumption on goiter prevalence in Isfahan: the possible role of goitrogens. Endocr Pract 2001;7:95–8
Fitzpatrick M. Soy formulas and the effects of isoflavones on the thyroid. N Z Med J 2000;113:24–26.
Laurberg P, Pedersen K, Hreidarsson A, et al. Iodine intake and the pattern of thyroid disorders: a comparative epidemiological study of thyroid abnormalities in the elderly in Iceland and in Jutland, Denmark. J Clin Endocrinol Metab 1998;83:765–769
World Health Organization (WHO)/ United Nations Children’s Fund (UNICEF)/International Council for Control of Iodine Deficiency Disorders (ICCIDD). Assessment of the iodine deficiency disorders and monitoring their elimination. A guide for program managers, 2nd ed. Geneva: WHO, 2001, Report of Consultation, 4–6 May 1999, WHO/NHI/01.1
Andersen S, Pedersen K, Pedrsen I, et al. Variations in urinary iodine excretion and thyroid function. A 1-year study in healthy men. Eur J Endocrinol 2001;144:461–5
Rasmussen L, Ovesen L, BuÈlow I, et al. Evaluation of a semi-quantitative food frequency questionnaire to estimate iodine intake. Eur J Clin Nutr 2001;55:287–292
Alissa EM, Bahjri SM, Ferns GAA. Dietary macronutrient intake of Saudi males and its relationship to classical coronary risk factors. Saudi Med J 2005;26:447–53
Abalkhail B. Hypercholesterolemia and susceptibility to CVD among white and blue collars in Jeddah. Saudi Med J 1998;19(2):123–9
Wynn M & Ma A. Human reproduction and iodine deficiency: Is it a problem in UK? J Nutr Environ Med 1998;8:53–64
Al-Nuaim A, Almazrou Y, Kamel M, et al. Iodine deficiency in Saudi Arabia. Ann Saudi Med 1997;17(3):293–7
Moosa K, Abdulwahab A, Alsayyad J. National study on the prevalence of IDD among schoolchildren 8–12 years of age in Bahrain. East Mediterr Health J 2001;7(4/5):609–16
Alhosani H, Osman H, Abdelwareth L, et al. Prevalence of IDD in the UAE measured by raised TSH levels. East Mediterr Health 2003;9(1/2):123–30
Ericsson U & Lindgarde F. Effects of cigarette smoking on thyroid function and the prevalence of goiter, thyrotoxicosis and autoimmune thyroiditis. J Intern Med 1991;229:67–71
Hak A, Pols H, Visser T, et al. Subclinical hypothyroidism is an independent risk factor for atherosclerosis and myocardial infarction in elderly women: the Rotterdam Study. Ann Intern Med 2000;132:270–278
Delange F. The disorders induced by iodine deficiency. Thyroid. 1994;4(1):107–28
Mariotti S, Barbesino G, Caturegli P, et al. Assay of thyroglobulin in serum with thyroglobulin autoantibodies: an unobtainable goal? J Clin Endocrinol Metab 1995;80:468–472
Massoudi M, Meilahn E, Orchard T, et al. Prevalence of thyroid antibodies among healthy middle-aged women. Findings from the thyroid study in healthy women. Ann Epidemiol 1995;5:229–233
Carle´ A, Laurberg P, Knudsen N, et al. Thyroid peroxidase and thyroglobulin auto-antibodies in patients with newly diagnosed overt hypothyroidism. Autoimmunity 2006;39(6):497–503
Weetman A. Autoimmune thyroid disease: propagation and progression. Eur J Endocrinol 2003;148:1–9
Lee S, Lewis J, Buss D. Iodine in British foods and diets. Br J Nutr 1994;72:435–46
Acknowledgment
This study was supported by a grant number (427/ 004/ح) from King Abdulaziz University, Jeddah, Saudi Arabia.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alissa, E.M., AlShali, K. & Ferns, G.A. Iodine Deficiency Among Hypothyroid Patients Living in Jeddah. Biol Trace Elem Res 130, 193–203 (2009). https://doi.org/10.1007/s12011-009-8329-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-009-8329-6