Abstract
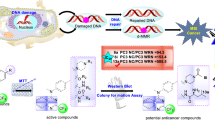
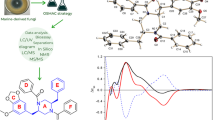
In recent years, derivatives of natural compounds are synthesized to increase the bioavailability, pharmacology, and pharmacokinetics properties. The naphthoquinone, plumbagin (PLU), is well known for its anticancer activity. However, the clinical use of PLU is hindered due to its toxicity. Previous reports have shown that modification of PLU at 5ʹ-hydroxyl group has reduced its toxicity towards normal cell line. In accordance, in the present study, 5ʹ-hydroxyl group of PLU was esterified with S-allyl cysteine (SAC) to obtain PLU-SAC ester. The drug-likeness of PLU-SAC was understood by in silico ADME analysis. PLU-SAC was characterized by UV–visible spectroscopy, mass spectroscopy, and nuclear magnetic resonance (NMR) spectroscopy. Molecular docking and dynamics simulation analysis revealed the interaction of PLU-SAC with proteins of interest in cancer therapy such as human estrogen receptor α, tumor protein p53 negative regulator mouse double minute 2, and cyclin-dependent kinase 2. MMGBSA calculation showed the favorable binding energy which in turn demonstrated the stable binding of PLU-SAC with these proteins. PLU-SAC showed apoptosis in breast cancer cell line (MCF-7) by inducing oxidative stress, disturbing mitochondrial function, arresting cells at G1 phase of cell cycle, and initiating DNA fragmentation. However, PLU-SAC did not show toxicity towards normal Vero cell line. PLU-SAC was synthesized and structurally characterized, and its anticancer activity was determined by in silico and in vitro analysis.







Similar content being viewed by others
Data Availability
Data will be available on request.
References
Wang, T., Wu, F., Jin, Z., Zhai, Z., Wang, Y., Tu, B., Yan, W., & Tang, T. (2014). Plumbagin inhibits LPS-induced inflammation through the inactivation of the nuclear factor-kappa B and mitogen activated protein kinase signaling pathways in RAW 264.7 cells. Food and Chemical Toxicology, 64, 177–183.
Nair, S. V., Baranwal, G., Chatterjee, M., Sachu, A., Vasudevan, A. K., Bose, C., Banerji, A., & Biswas, R. (2016). Antimicrobial activity of plumbagin, a naturally occurring naphthoquinone from Plumbago rosea, against Staphylococcus aureus and Candida albicans. International Journal of Medical Microbiology, 306(4), 237–248.
Chu, H., Yu, H., Ren, D., Zhu, K., & Huang, H. (2016). Plumbagin exerts protective effects in nucleus pulposus cells by attenuating hydrogen peroxide-induced oxidative stress, inflammation and apoptosis through NF-κB and Nrf-2. International Journal of Molecular Medicine, 37(6), 1669–1676.
Pai, S. A., Munshi, R. P., Panchal, F. H., Gaur, I.-S., Mestry, S. N., Gursahani, M. S., & Juvekar, A. R. (2019). Plumbagin reduces obesity and nonalcoholic fatty liver disease induced by fructose in rats through regulation of lipid metabolism, inflammation and oxidative stress. Biomedicine & Pharmacotherapy, 111, 686–694.
Yin, Z., Zhang, J., Chen, L., Guo, Q., Yang, B., Zhang, W., & Kang, W. (2020). Anticancer effects and mechanisms of action of plumbagin: Review of research advances. BioMed Research International, 2020, 1–10.
Jangra, A., Chadha, V., Kumar, D., Kumar, V., & Arora, M. K. (2021). Neuroprotective and acetylcholinesterase inhibitory activity of plumbagin in ICV-LPS induced behavioral deficits in rats. Current Research in Behavioral Sciences, 2, 100060.
Jiang, Z.-B., Xu, C., Wang, W., Zhang, Y.-Z., Huang, J.-M., Xie, Y.-J., Wang, Q.-Q., Fan, X.-X., Yao, X.-J., & Xie, C. (2021). Plumbagin suppresses non-small cell lung cancer progression through downregulating ARF1 and by elevating CD8+ T cells. Pharmacological Research, 169, 105656.
Cao, Y.-Y., Yu, J., Liu, T.-T., Yang, K.-X., Yang, L.-Y., Chen, Q., Shi, F., Hao, J.-J., Cai, Y., & Wang, M.-R. (2018). Plumbagin inhibits the proliferation and survival of esophageal cancer cells by blocking STAT3-PLK1-AKT signaling. Cell Death & Disease, 9(2), 1–13.
Pan, Q., Zhou, R., Su, M., & Li, R. (2019). The effects of plumbagin on pancreatic cancer: A mechanistic network pharmacology approach. Medical Science Monitor: International Medical Journal of Experimental and Clinical Research, 25, 4648.
Sinha, S., Pal, K., Elkhanany, A., Dutta, S., Cao, Y., Mondal, G., Iyer, S., Somasundaram, V., Couch, F. J., & Shridhar, V. (2013). Plumbagin inhibits tumorigenesis and angiogenesis of ovarian cancer cells in vivo. International Journal of Cancer, 132(5), 1201–1212.
Zhang, R., Wang, Z., You, W., Zhou, F., Guo, Z., Qian, K., Xiao, Y., & Wang, X. (2020). Suppressive effects of plumbagin on the growth of human bladder cancer cells via PI3K/AKT/mTOR signaling pathways and EMT. Cancer Cell International, 20(1), 1–17.
Giacomini, I., Cocetta, V., Carrara, M., Ragazzi, E., & Montopoli, M. (2020). Plumbagin induces cell cycle arrest and apoptosis in A431 cisplatin-resistant cancer cells. Natural Product Communications, 15(4), 1934578X20921627.
Zhong, J., Li, J., Wei, J., Huang, D., Huo, L., Zhao, C., Lin, Y., Chen, W., & Wei, Y. (2019). Plumbagin restrains hepatocellular carcinoma angiogenesis by stromal cell-derived factor (SDF-1)/CXCR4-CXCR7 axis. Medical Science Monitor: International Medical Journal of Experimental and Clinical Research, 25, 6110.
De, U., Son, J. Y., Jeon, Y., Ha, S.-Y., Park, Y. J., Yoon, S., Ha, K.-T., Choi, W. S., Lee, B. M., & Kim, I. S. (2019). Plumbagin from a tropical pitcher plant (Nepenthes alata Blanco) induces apoptotic cell death via a p53-dependent pathway in MCF-7 human breast cancer cells. Food and Chemical Toxicology, 123, 492–500.
Srinivas, P., Gopinath, G., Banerji, A., Dinakar, A., & Srinivas, G. (2004). Plumbagin induces reactive oxygen species, which mediate apoptosis in human cervical cancer cells. Molecular Carcinogenesis: Published in Cooperation with the University of Texas MD Anderson Cancer Center, 40(4), 201–211.
Lee, J.-H., Yeon, J.-H., Kim, H., Roh, W., Chae, J., Park, H.-O., & Kim, D.-M. (2012). The natural anticancer agent plumbagin induces potent cytotoxicity in MCF-7 human breast cancer cells by inhibiting a PI-5 kinase for ROS generation. PLoS ONE, 7(9), e45023.
Jackson, H. L., Cardounel, A. J., Zweier, J. L., & Lockwood, S. F. (2004). Synthesis, characterization, and direct aqueous superoxide anion scavenging of a highly water-dispersible astaxanthin-amino acid conjugate. Bioorganic & Medicinal Chemistry Letters, 14(15), 3985–3991.
Mukherjee, A., Mishra, S., Kotla, N. K., Manna, K., Roy, S., Kundu, B., Bhattacharya, D., Das Saha, K., & Talukdar, A. (2019). Semisynthetic quercetin derivatives with potent antitumor activity in colon carcinom. Acs Omega, 4(4), 7285–7298.
Newman, D. J., & Cragg, G. M. (2020). Natural products as sources of new drugs over the nearly four decades from 01/1981 to 09/2019. Journal of Natural Products, 83(3), 770–803.
Xu, G., Shi, H., Ren, L., Gou, H., Gong, D., Gao, X., & Huang, N. (2015). Enhancing the anti-colon cancer activity of quercetin by self-assembled micelles. International Journal of Nanomedicine, 10, 2051.
Ma, Y.-T., Yang, Y., Cai, P., Sun, D.-Y., Sánchez-Murcia, P. A., Zhang, X.-Y., Jia, W.-Q., Lei, L., Guo, M., & Gago, F. (2018). A series of enthalpically optimized docetaxel analogues exhibiting enhanced antitumor activity and water solubility. Journal of Natural Products, 81(3), 524–533.
Cui, Q., Lu, S., Ni, B., Zeng, X., Tan, Y., Chen, Y. D., & Zhao, H. (2020). Improved prediction of aqueous solubility of novel compounds by going deeper with deep learning. Frontiers in Oncology, 10, 121.
Shimada, H., Yamaoka, Y., Morita, R., Mizuno, T., Gotoh, K., Higuchi, T., Shiraishi, T., & Imamura, Y. (2012). Possible mechanism of superoxide formation through redox cycling of plumbagin in pig heart. Toxicology in Vitro, 26, 252–257.
Sagar, S., Esau, L., Moosa, B., Khashab, N. M., Bajic, V. B., & Kaur, M. (2014). Cytotoxicity and apoptosis induced by a plumbagin derivative in estrogen positive MCF-7 breast cancer cells. Anti-Cancer Agents in Medicinal Chemistry (Formerly Current Medicinal Chemistry-Anti-Cancer Agents), 14(1), 170–180.
Sakao, K., Fujii, M., & Hou, D. X. (2009). Acetyl derivate of quercetin increases the sensitivity of human leukemia cells toward apoptosis. BioFactors, 35(4), 399–405.
Sreelatha, T., Hymavathi, A., Babu, K. S., Murthy, J. M., Pathipati, U. R., & Rao, J. M. (2009). Synthesis and insect antifeedant activity of plumbagin derivatives with the amino acid moiety. Journal of Agricultural and Food Chemistry, 57(14), 6090–6094.
Hazra, B., Sarkar, R., Bhattacharyya, S., Ghosh, P. K., Chel, G., & Dinda, B. (2002). Synthesis of plumbagin derivatives and their inhibitory activities against Ehrlich ascites carcinoma in vivo and Leishmania donovani promastigotes in vitro. Phytotherapy Research: An International Journal Devoted to Pharmacological and Toxicological Evaluation of Natural Product Derivatives, 16(2), 133–137.
Gammon, D. W., Steenkamp, D. J., Mavumengwana, V., Marakalala, M. J., Mudzunga, T. T., Hunter, R., & Munyololo, M. (2010). Conjugates of plumbagin and phenyl-2-amino-1-thioglucoside inhibit MshB, a deacetylase involved in the biosynthesis of mycothiol. Bioorganic & Medicinal Chemistry, 18(7), 2501–2514.
Dandawate, P., Khan, E., Padhye, S., Gaba, H., Sinha, S., Deshpande, J., Swamy, K. V., Khetmalas, M., Ahmad, A., & Sarkar, F. H. (2012). Synthesis, characterization, molecular docking and cytotoxic activity of novel plumbagin hydrazones against breast cancer cells. Bioorganic & Medicinal Chemistry Letters, 22(9), 3104–3108.
Dandawate, P., Vemuri, K., Swamy, K. V., Khan, E. M., Sritharan, M., & Padhye, S. (2014). Synthesis, characterization, molecular docking and anti-tubercular activity of Plumbagin-Isoniazid Analog and its β-cyclodextrin conjugate. Bioorganic & Medicinal Chemistry Letters, 24(21), 5070–5075.
Kodera, Y., Suzuki, A., Imada, O., Kasuga, S., Sumioka, I., Kanezawa, A., Taru, N., Fujikawa, M., Nagae, S., & Masamoto, K. (2002). Physical, chemical, and biological properties of S-allylcysteine, an amino acid derived from garlic. Journal of Agricultural and Food Chemistry, 50(3), 622–632.
Chuah, S. C., Moore, P. K., & Zhu, Y. Z. (2007). S-allylcysteine mediates cardioprotection in an acute myocardial infarction rat model via a hydrogen sulfide-mediated pathway. American Journal of Physiology-Heart and Circulatory Physiology, 293(5), H2693–H2701.
Johnson, P., Loganathan, C., Iruthayaraj, A., Poomani, K., & Thayumanavan, P. (2018). S-allyl cysteine as potent anti-gout drug: Insight into the xanthine oxidase inhibition and anti-inflammatory activity. Biochimie, 154, 1–9.
Chen, P., Hu, M., Liu, F., Yu, H., & Chen, C. (2019). S-allyl-l-cysteine (SAC) protects hepatocytes from alcohol-induced apoptosis. FEBS Open Bio, 9(7), 1327–1336.
Ruiz-Sánchez, E., Pedraza-Chaverri, J., Medina-Campos, O. N., Maldonado, P. D., & Rojas, P. (2020). S-allyl cysteine, a garlic compound, produces an antidepressant-like effect and exhibits antioxidant properties in mice. Brain Sciences, 10(9), 592.
Agbana, Y. L., Ni, Y., Zhou, M., Zhang, Q., Kassegne, K., Karou, S. D., Kuang, Y., & Zhu, Y. (2020). Garlic-derived bioactive compound S-allylcysteine inhibits cancer progression through diverse molecular mechanisms. Nutrition Research, 73, 1–14.
Meunier, B. (2008). Hybrid molecules with a dual mode of action: Dream or reality? Accounts of Chemical Research, 41(1), 69–77.
Gupta, A., Saha, P., Descôteaux, C., Leblanc, V., Asselin, É., & Bérubé, G. (2010). Design, synthesis and biological evaluation of estradiol–chlorambucil hybrids as anticancer agents. Bioorganic & Medicinal Chemistry Letters, 20(5), 1614–1618.
Wilson Castrillón, A.H.-R., Prieto, L. J., Conesa-Milián, L., Carda, M., Naranjo, T., Maldonado, M. E., & Cardona-G, W. (2019). Synthesis and in-vitro evaluation of s-allyl cysteine ester-caffeic acid amide hybrids as potential anticancer agents. Iranian Journal of Pharmaceutical Research: IJPR, 18(4), 1770.
Morris, G. M., Huey, R., Lindstrom, W., Sanner, M. F., Belew, R. K., Goodsell, D. S., & Olson, A. J. (2009). AutoDock4 and AutoDockTools4: Automated docking with selective receptor flexibility. Journal of Computational Chemistry, 30(16), 2785–2791.
Shiau, A. K., Barstad, D., Loria, P. M., Cheng, L., Kushner, P. J., Agard, D. A., & Greene, G. L. (1998). The structural basis of estrogen receptor/coactivator recognition and the antagonism of this interaction by tamoxifen. Cell, 95(7), 927–937.
Byth, K. F., Cooper, N., Culshaw, J. D., Heaton, D. W., Oakes, S. E., Minshull, C. A., Norman, R. A., Pauptit, R. A., Tucker, J. A., & Breed, J. (2004). Imidazo [1, 2-b] pyridazines: A potent and selective class of cyclin-dependent kinase inhibitors. Bioorganic & Medicinal Chemistry Letters, 14(9), 2249–2252.
Allen, J. G., Bourbeau, M. P., Wohlhieter, G. E., Bartberger, M. D., Michelsen, K., Hungate, R., Gadwood, R. C., Gaston, R. D., Evans, B., & Mann, L. W. (2009). Discovery and optimization of chromenotriazolopyrimidines as potent inhibitors of the mouse double minute 2− tumor protein 53 protein− protein interaction. Journal of Medicinal Chemistry, 52(22), 7044–7053.
Bowers, K.J., Chow, D.E., Xu, H., Dror, R.O., Eastwood, M.P., Gregersen, B.A., Klepeis, J.L., Kolossvary, I., Moraes, M.A., Sacerdoti, F.D. (2006). Scalable algorithms for molecular dynamics simulations on commodity clusters, SC'06: Proceedings of the 2006 ACM/IEEE Conference on Supercomputing, IEEE, pp. 43–43.
Ellman, G. L. (1959). Tissue sulfhydryl groups. Archives of Biochemistry and Biophysics, 82(1), 70–77.
Rotruck, J. T., Pope, A. L., Ganther, H. E., Swanson, A. B., Hafeman, D. G., & Hoekstra, W. G. (1973). Selenium: Biochemical role as a component of glutathione peroxidase. Science, 179(4073), 588–590.
Kakkar, P., Das, B., Viswanathan, P. (1984). A modified spectrophotometric assay of superoxide dismutase. Indian Journal of Biochemistry and Biophysics, 21(2), 130–132.
Hadwan, M. H. (2016). New method for assessment of serum catalase activity. Indian Journal of Science and Technology, 9(4), 1–5.
Onitilo, A. A., Engel, J. M., Greenlee, R. T., & Mukesh, B. N. (2009). Breast cancer subtypes based on ER/PR and Her2 expression: Comparison of clinicopathologic features and survival. Clinical Medicine & Research, 7(1–2), 4–13.
Ali, S., & Coombes, R. C. (2000). Estrogen receptor alpha in human breast cancer: Occurrence and significance. Journal of Mammary Gland Biology and Neoplasia, 5(3), 271–281.
Agrawal, A., Yang, J., Murphy, R. F., & Agrawal, D. K. (2006). Regulation of the p14ARF-Mdm2-p53 pathway: An overview in breast cancer. Experimental and Molecular Pathology, 81(2), 115–122.
Carr, M. I., & Jones, S. N. (2016). Regulation of the Mdm2-p53 signaling axis in the DNA damage response and tumorigenesis. Translational Cancer Research, 5(6), 707.
Brekman, A., Singh, K. E., Polotskaia, A., Kundu, N., & Bargonetti, J. (2011). A p53-independent role of Mdm2 in estrogen-mediated activation of breast cancer cell proliferation. Breast Cancer Research, 13(1), 1–14.
Burgess, A., Chia, K. M., Haupt, S., Thomas, D., Haupt, Y., & Lim, E. (2016). Clinical overview of MDM2/X-targeted therapies. Frontiers in Oncology, 6, 7.
Harbour, J. W., Luo, R. X., Dei Santi, A., Postigo, A. A., & Dean, D. C. (1999). Cdk phosphorylation triggers sequential intramolecular interactions that progressively block Rb functions as cells move through G1. Cell, 98(6), 859–869.
Whittaker, S. R., Mallinger, A., Workman, P., & Clarke, P. A. (2017). Inhibitors of cyclin-dependent kinases as cancer therapeutics. Pharmacology & Therapeutics, 173, 83–105.
Vijayan, S., Loganathan, C., Sakayanathan, P., Thayumanavan, P. (2021). In silico and in vitro investigation of anticancer effect of newly synthesized nonivamide-s-allyl cysteine ester. Journal of Biomolecular Structure and Dynamics, 1–15.
Bothiraja, C., Joshi, P. P., Dama, G. Y., & Pawar, A. P. (2011). Rapid method for isolation of plumbagin, an alternative medicine from roots of Plumbago zeylanica. European Journal of Integrative Medicine, 3, 39–42.
Bronowicka-Adamska, P., Bentke, A., Lasota, M., & Wróbel, M. (2020). Effect of S-Allyl–L-cysteine on MCF-7 cell line 3-mercaptopyruvate sulfurtransferase/sulfane sulfur system, viability and apoptosis. International Journal of Molecular Sciences, 21(3), 1090.
Sumiyoshi, H., & Wargovich, M. J. (1990). Chemoprevention of 1, 2-dimethylhydrazine-induced colon cancer in mice by naturally occurring organosulfur compounds. Cancer Research, 50(16), 5084–5087.
Sigounas, G., Hooker, J., Anagnostou, A., & Steiner, M. (1997). S-allylmercaptocysteine inhibits cell proliferation and reduces the viability of erythroleukemia, breast, and prostate cancer cell lines. Nutrition and Cancer, 27(2), 186–191.
Cave, D., Ilisso, C. P., Mosca, L., Pagano, M., Martino, E., Porcelli, M., & Cacciapuoti, G. (2017). The anticancer effects of S-adenosylmethionine on breast cancer cells. JSM Chem, 5, 1049.
Othman, S., & Kozurkova, M. (2018). Sulfur containing acridine derivatives in preclinical studies with cancer cell lines. Current Medicinal Chemistry, 25(17), 1968–1975.
De Greef, D., Barton, E.M., Sandberg, E.N., Croley, C.R., Pumarol, J., Wong, T.L., Das, N., Bishayee, A. (2020). Anticancer potential of garlic and its bioactive constituents: A systematic and comprehensive review. Seminars in Cancer Biology, Elsevier.
Galadari, S., Rahman, A., Pallichankandy, S., & Thayyullathil, F. (2017). Reactive oxygen species and cancer paradox: To promote or to suppress? Free Radical Biology and Medicine, 104, 144–164.
Powolny, A. A., & Singh, S. V. (2008). Plumbagin-induced apoptosis in human prostate cancer cells is associated with modulation of cellular redox status and generation of reactive oxygen species. Pharmaceutical Research, 25(9), 2171–2180.
Yang, L., Zheng, X. L., Sun, H., Zhong, Y. J., Wang, Q., He, H. N., Shi, X. W., Zhou, B., Li, J. K., & Lin, Y. (2011). Catalase suppression-mediated H2O2 accumulation in cancer cells by wogonin effectively blocks tumor necrosis factor-induced NF-κB activation and sensitizes apoptosis. Cancer Science, 102(4), 870–876.
Harris, I. S., Treloar, A. E., Inoue, S., Sasaki, M., Gorrini, C., Lee, K. C., Yung, K. Y., Brenner, D., Knobbe-Thomsen, C. B., & Cox, M. A. (2015). Glutathione and thioredoxin antioxidant pathways synergize to drive cancer initiation and progression. Cancer Cell, 27(2), 211–222.
Kim, J.-Y., Choi, J.-Y., Lee, H.-J., Byun, C. J., Park, J.-H., Park, J. H., Cho, H.-S., Cho, S.-J., Jo, S. A., & Jo, I. (2015). The green tea component (-)-epigallocatechin-3-gallate sensitizes primary endothelial cells to arsenite-induced apoptosis by decreasing c-jun n-terminal kinase-mediated catalase activity. PLoS ONE, 10(9), e0138590.
Carlisi, D., Buttitta, G., Di Fiore, R., Scerri, C., Drago-Ferrante, R., Vento, R., & Tesoriere, G. (2016). Parthenolide and DMAPT exert cytotoxic effects on breast cancer stem-like cells by inducing oxidative stress, mitochondrial dysfunction and necrosis. Cell Death & Disease, 7(4), e2194–e2194.
Sznarkowska, A., Kostecka, A., Meller, K., & Bielawski, K. P. (2017). Inhibition of cancer antioxidant defense by natural compounds. Oncotarget, 8(9), 15996.
Clarke, R., Leonessa, F., Welch, J. N., & Skaar, T. C. (2001). Cellular and molecular pharmacology of antiestrogen action and resistance. Pharmacological Reviews, 53(1), 25–72.
Prall, O. W., Rogan, E. M., & Sutherland, R. L. (1998). Estrogen regulation of cell cycle progression in breast cancer cells. The Journal of Steroid Biochemistry and Molecular Biology, 65(1–6), 169–174.
Makowska, K., Estañ, M., Ganan-Gomez, I., Boyano-Adánez, M., García-Pérez, A., & Sancho, P. (2014). Changes in mitochondrial function induced by dequalinium precede oxidative stress and apoptosis in the human prostate-cancer cell line PC-3. Molecular Biology, 48(3), 359–370.
Zaidieh, T., Smith, J. R., Ball, K. E., & An, Q. (2019). ROS as a novel indicator to predict anticancer drug efficacy. BMC Cancer, 19(1), 1–14.
Cheng, M.-H., Pan, C.-Y., Chen, N.-F., Yang, S.-N., Hsieh, S., Wen, Z.-H., Chen, W.-F., Wang, J.-W., Lu, W.-H., & Kuo, H.-M. (2020). Piscidin-1 induces apoptosis via mitochondrial reactive oxygen species-regulated mitochondrial dysfunction in human osteosarcoma cells. Scientific Reports, 10(1), 1–15.
Perillo, B., Di Donato, M., Pezone, A., Di Zazzo, E., Giovannelli, P., Galasso, G., Castoria, G., & Migliaccio, A. (2020). ROS in cancer therapy: The bright side of the moon. Experimental & Molecular Medicine, 52(2), 192–203.
Cao, J., Zhang, M., Wang, B., Zhang, L., Fang, M., & Zhou, F. (2021). Chemoresistance and metastasis in breast cancer molecular mechanisms and novel clinical strategies. Frontiers in Oncology, 11, 1701.
DeSantis, C. E., Ma, J., Gaudet, M. M., Newman, L. A., Miller, K. D., Goding Sauer, A., Jemal, A., & Siegel, R. L. (2019). Breast cancer statistics, 2019. CA: a Cancer Journal for Clinicians, 69(6), 438–451.
Ma, C. X., Gao, F., Luo, J., Northfelt, D. W., Goetz, M., Forero, A., Hoog, J., Naughton, M., Ademuyiwa, F., & Suresh, R. (2017). NeoPalAna: Neoadjuvant palbociclib, a cyclin-dependent kinase 4/6 inhibitor, and anastrozole for clinical stage 2 or 3 estrogen receptor–positive breast cancer. Clinical Cancer Research, 23(15), 4055–4065.
Teo, Z. L., Versaci, S., Dushyanthen, S., Caramia, F., Savas, P., Mintoff, C. P., Zethoven, M., Virassamy, B., Luen, S. J., & McArthur, G. A. (2017). Combined CDK4/6 and PI3Kα inhibition is synergistic and immunogenic in triple-negative breast cancer. Cancer Research, 77(22), 6340–6352.
Acknowledgements
Mrs. V. Sudha acknowledges Periyar University for the award of University Research Fellowship. Dr. S. Penislusshiyan acknowledges Human Resource Development, Department of Health Research, Ministry of Health and Family Welfare, India, for the award of young scientist fellowship (Ref. No. R.12014/51/2020-HR). The authors thank the Department of Computer Science, Periyar University, for providing the high-performance computer facility.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by SV. Analysis, supervision of the work, and manuscript preparation were done by CL. In silico analysis was carried out by PS. Supervision of the work, correction, review and editing of the manuscript was done by PT. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Approval
Not applicable.
Consent to Participate
Not applicable.
Consent to Publish
Not applicable.
Conflict of Interest
The authors declare no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Vijayan, S., Loganathan, C., Sakayanathan, P. et al. Synthesis and Characterization of Plumbagin S-Allyl Cysteine Ester: Determination of Anticancer Activity In Silico and In Vitro. Appl Biochem Biotechnol 194, 5827–5847 (2022). https://doi.org/10.1007/s12010-022-04079-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12010-022-04079-0