Abstract
Background
Prophylactic antibiotics reduce the risk of deep infection after primary TKA. However, conventional systemic dosing may not provide adequate tissue concentrations against more resistant organisms such as coagulase-negative staphylococci. Regional intravenous administration of antibiotics after tourniquet inflation achieves far higher tissue concentrations but requires foot vein cannulation. The intraosseous route may offer a rapid and reliable method of regional administration.
Questions/Purposes
We compared tissue concentrations of cefazolin achieved with systemic versus regional intraosseous administration.
Methods
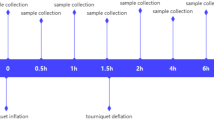
Twenty-two patients undergoing primary TKA were randomized into two groups. Group 1 received 1 g cefazolin systemically 10 minutes before tourniquet inflation. Group 2 received 1 g cefazolin intraosseously in 200 mL of normal saline through a tibial cannula after tourniquet inflation and before skin incision. Subcutaneous fat and femoral bone samples were taken at set intervals during the procedure and antibiotic concentrations measured using a validated technique involving high-performance liquid chromatography.
Results
The overall mean tissue concentration of cefazolin in subcutaneous fat was 186 ug/g in the intraosseous group and 11 ug/g in the systemic group. The mean tissue concentration in bone was 130 ug/g in the intraosseous group and 11 ug/g in the systemic group. These differences were consistent across all sample time points throughout the procedure.
Conclusions
Intraosseous regional administration can achieve concentrations of antibiotic in tissue an order of magnitude higher than systemic administration. Further work is required to determine if this translates into increased efficacy in preventing infection, particularly against coagulase-negative staphylococci.


Similar content being viewed by others
References
Bengtson S, Knutson K. The infected knee arthroplasty. A 6-year follow-up of 357 cases. Acta Orthop Scand. 1991;62:301–311.
Blom AW, Brown J, Taylor AH, Pattison G, Whitehouse S, Bannister GC. Infection after total knee arthroplasty. J Bone Joint Surg Br. 2004;86:688–691.
Burke JF. The effective period of preventive antibiotic action in experimental incisions and dermal lesions. Surgery. 1961;50:161–168.
Carlsson AK, Lidgren L, Lindberg L. Prophylactic antibiotics against early and late deep infections after total hip replacements. Acta Orthop Scand. 1977;48:405–410.
Craig WA. Pharmacokinetic/pharmacodynamic parameters: rationale for antibacterial dosing of mice and men. Clin Infect Dis. 1998;26:1–10.
Cunha BA, Gossling HR, Pasternak HS, Nightingale CH, Quintiliani R. The penetration characteristics of cefazolin, cephalothin, and cephradine into bone in patients undergoing total hip replacement. J Bone Joint Surg Am. 1977;59:856–859.
Davis N, Curry A, Gambhir AK, Panigrahi H, Walker CR, Wilkins EG, Worsley MA, Kay PR. Intraoperative bacterial contamination in operations for joint replacement. J Bone Joint Surg Br. 1999;81:886–889.
de Lalla F, Novelli A, Pellizzer G, Milocchi F, Viola R, Rigon A, Stecca C, Dal Pizzol V, Fallani S, Periti P. Regional and systemic prophylaxis with teicoplanin in monolateral and bilateral total knee replacement procedures: study of pharmacokinetics and tissue penetration. Antimicrob Agents Chemother. 1993;37:2693–2698.
de Lalla F, Viola R, Pellizzer G, Lazzarini L, Tramarin A, Fabris P. Regional prophylaxis with teicoplanin in monolateral or bilateral total knee replacement: an open study. Antimicrob Agents Chemother. 2000;44:316–319.
Fletcher N, Sofianos D, Berkes MB, Obremskey WT. Prevention of perioperative infection. J Bone Joint Surg Am. 2007;89:1605–1618.
Friedman RJ, Friedrich LV, White RL, Kays MB, Brundage DM, Graham J. Antibiotic prophylaxis and tourniquet inflation in total knee arthroplasty. Clin Orthop Relat Res. 1990;260:17–23.
Gillespie WJ, Walenkamp G. Antibiotic prophylaxis for surgery for proximal femoral and other closed long bone fractures. Cochrane Database Syst Rev. 2001;1:CD000244.
Hasan M, Kissoon N, Khan T, Saldajeno V, Goldstein J, Murphy S. Intraosseous infusion and pulmonary fat embolism. Pediatr Crit Care Med. 2001;2:133–138.
Hill C, Flamant R, Mazas F, Evrard J. Prophylactic cefazolin versus placebo in total hip replacement. Report of a multicentre double-blind randomised trial. Lancet. 1981;1:795–796.
Hoddinott C, Lovering AM, Fernando HC, Dixon JH, Reeves DS. Determination of bone and fat concentrations following systemic cefamandole and regional cefuroxime administration in patients undergoing knee arthroplasty. J Antimicrob Chemother. 1990;26:823–829.
Josefson A. A new method of treatment—intraosseous injection. Acta Med Scand. 1934;81:550–554.
Lazzarini L. Regional and systemic prophylaxis with teicoplanin in total knee arthroplasty. J Arthroplasty. 2003;18:342–346.
Mattson S, Bourve L, Pearce S, Hurtig M, Burger J, Black W. Intraosseous gentamicin perfusion of the distal metacarpus in standing horses. Vet Surg. 2004;33:180–186.
Miller BS, Harper WP, Hughes JS, Sonnabend DH, Walsh WR. Regional antibiotic prophylaxis in elbow surgery. J Shoulder Elbow Surg. 2004;13:57–59.
Nickinson R, Board T, Gambhir A, Porter M, Kay P. The microbiology of the infected knee arthroplasty. Int Orthop. 2010;34:505–510.
Phillips JE, Crane TP, Noy M, Elliott TSJ, Grimer RJ. The incidence of deep prosthetic infections in a specialist orthopaedic hospital: a 15-year prospective survey. J Bone Joint Surg Br. 2006;88:943–948.
Rubio-Martínez L, López-Sanromán J, Cruz AM, Santos M, San Román F. Medullary plasma pharmacokinetics of vancomycin after intravenous and intraosseous perfusion of the proximal phalanx in horses. Vet Surg. 2005;34:618–624.
Scheuch BC, Van Hoogmoed LM, Wilson WD, Snyder JR, MacDonald MH, Watson ZE, Steffey EP. Comparison of intraosseous or intravenous infusion for delivery of amikacin sulfate to the tibiotarsal joint of horses. Am J Vet Res. 2002;63:374–380.
Schurman DJ, Hirshman HP, Kajiyama G, Moser K, Burton DS. Cefazolin concentrations in bone and synovial fluid. J Bone Joint Surg Am. 1978;60:359–362.
Shavit I, Hoffmann Y, Galbraith R, Waisman Y. Comparison of two mechanical intraosseous infusion devices: a pilot, randomized crossover trial. Resuscitation. 2009;80:1029–1033.
Tobias JD, Ross AK. Intraosseous infusions: a review for the anesthesiologist with a focus on pediatric use. Anesth Analg. 2010;110:391–401.
Waisman M, Roffman M, Bursztein S, Heifetz M. Intraosseous regional anesthesia as an alternative to intravenous regional anesthesia. J Trauma. 1995;39:1153–1156.
Yamada K, Matsumoto K, Tokimura F, Okazaki H, Tanaka S. Are bone and serum cefazolin concentrations adequate for antimicrobial prophylaxis? Clin Orthop Relat Res. 2011;469:3486–3494.
Acknowledgments
We thank Irene Zeng, MSc (Hons), for her assistance with statistical analysis, Grant Moore, BSc (Hons), for his assistance with laboratory analysis, and the charitable trust Clinical Research and effective practice (CCRep) for their funding support. We also thank Vidicare (San Antonio, TX, USA) for supplying the intraosseous needles without charge.
Author information
Authors and Affiliations
Corresponding author
Additional information
The institution of one of the authors (MZ) received funding from the Centre for Clinical Research and effective practice (CCRep), a charitable trust with no relationship to the subject of this article.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
Clinical Orthopaedics and Related Research neither advocates nor endorses the use of any treatment, drug, or device. Readers are encouraged to always seek additional information, including FDA-approval status, of any drug or device prior to clinical use.
Procedures and sample collection were performed at Middlemore Hospital, Auckland, New Zealand. Sample analysis was performed at Canterbury Health Laboratories, Christchurch, New Zealand.
About this article
Cite this article
Young, S.W., Zhang, M., Freeman, J.T. et al. Higher Cefazolin Concentrations with Intraosseous Regional Prophylaxis in TKA. Clin Orthop Relat Res 471, 244–249 (2013). https://doi.org/10.1007/s11999-012-2469-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-012-2469-2