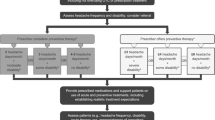
Opinion statement
-
Stratify care by choosing the optimal medication for a migraine. Severe pain, significant disability, and associated features such as nausea or vomiting necessitate early treatment with specific, high efficacy therapy.
-
Migraine patients may have a spectrum of headache presentations ranging from tension-type headaches to migraine headaches with or without aura. Mild headache types may respond to simple analgesics, though there is evidence that migraineurs will respond to migraine-specific medications such as the triptans for a range of headache phenotypes.
-
Physicians should provide patients with medication to treat nausea and vomiting. They may be infrequent accompaniments, but medication such as a neuroleptic may avoid a trip to the emergency room.
-
Provide rescue medication for an occasional failure of usual treatment to avoid further disability or emergency room visits.
-
Avoid medication overuse by matching treatment to patient needs. A cycle of repetitive and escalating medication use can lead to transformation of migraine into chronic daily headache with analgesic-dependent rebound.
Similar content being viewed by others
References and Recommended Reading
Lipton RB, Stewart WF, Diamond S, et al.: Prevalence and burden of migraine in the United States: results from American Migraine II. Headache 2001, 41:646–657. This paper describes the epidemiology of migraine in the population, and its socioeconomic impact. It is an important extension and addition to the American Migraine I study, which was completed 10 years prior to this paper.
Rasmussen BK, Jensen R, Schroll M, Olesen J: Epidemiology of headache in a general population: a prevalence study. J Clin Epidemiol 1991, 44:1147–1157.
Stewart WF, Lipton RB, Celentano DD, Reed ML: Prevalence of migraine headache in the United States: relation to age, income, race, and other socioeconomic factors. JAMA 1991, 267:64–69.
Headache Classification Committee of the International Headache Society: Classification and diagnostic criteria for headache disorder, cranial neuralgias, and facial pain. Cephalalgia 1988, 8(suppl):1–96.
Featherstone HJ: Migraine and muscle contraction headache: a continuum. Headache 1985, 25:194–198.
Cady R, Schreiber C, Faarmer K, Sheftell F: Primary headaches: a convergence hypothesis. Headache 2002, 42:204–216.
Cady RK, Lipton RB, Tall C, et al.: Treatment of mild headache in disabled migraine sufferers: results of the Spectrum study. Headache 2000, 40:792–797.
Mathew NT, Reuveni U, Penez F: Transformed or evolutive migraine. Headache 1987, 27:102–106. Although from 1987, this paper discusses and supports the concept of early treatment of migraine, and demonstrated higher efficacy of medication when used early in the migraine attack.
Mathew NT, Kurman R, Penez F: Drug induced refractory headache: clinical features and management. Headache 1990, 30:634–638.
Raskin NH: Headache edn 2. New York: Churchill Livingstone, Inc; 1988.
Loder E, Tietjen GE, Marcus DA: Evaluation and management issues in migraine. J Clin Outcomes Manage 1999, 6:58–74.
Lipton RB, Stewart WF, Stone AM, et al.: Stratified care vs step care strategies for migraine: the Disability in Strategies of Care (DISC) Study. JAMA 2000, 284:2640–2641.
Ottervanger JP, Wilson JHP, Stricker BHC: Drug-induced chest pain and myocardial infarction. Reports to a national centre and review of the literature. Eur Clin Pharmacol 1997, 53:105–110. Finally, migraineurs can get therapy for their headache matched to their treatment needs.
Maassen VanDenBrink A, Reekers M, Bax WA, et al.: Coronary side effect potential of current and prospective antimigraine drugs. Circulation 1998, 98:25–30.
Lipton RB, Stewart WF: Acute migraine therapy: do doctors understand what patients with migraine want from therapy? Headache 1999, 3(suppl):S20-S26.
Silberstein SD: Evaluation and emergency treatment of headache. Headache 1992, 32:396–407.
Tepper SJ, Rapoport AM: The triptans: a summary. CNS Drugs 1999, 12:403–417.
Moskowitz MA, Cutrer FM: Sumatriptan: a receptor targeted treatment for migraine. Ann Rev Med 1993, 44:145–154.
Humphrey PPA, Feniuk W, Perren MJ, et al.: Serotonin and migraine. Ann N Y Acad Sci 1990, 600:587–588.
Goadsby PG: The pharmacology of headache. Prog Neurobiol 2000, 62:509–525.
Ferrari MD, Roon KI, Lipton RB, Goadsby PJ: Oral triptans (5-HT 1B/1D agonists) in acute migraine treatment: a meta-analysis of 53 trials. Lancet 2001, 358:1668–1675.
Perrin VL: Clinical pharmacokinetics of ergotamine in migraine and cluster headache. Clin Pharmacokinet 1985, 10:334–352.
Clinical update on dihydroergotamine. Satellite Symposium at the 8th Congress of the International Headache Society; Amsterdam, The Netherlands. June 11 to 14, 1997;
Lipton RB, Baggish JE, Stewart WF, et al.: Efficacy and safety of acetaminophen in the non-prescription treatment of migraine: results of a randomized, double blind, placebo-controlled, population-based study. Arch Intern Med 2000, 160:3486–3492.
Welch KMA: Naproxen sodium in the treatment of migraine. Cephalalgia 1986, 6(suppl):85–92.
Kellstein DE, Lipton RB, Geetha R, et al.: Evaluation of a novel, solubilized formulation of ibuprofen in the treatment of migraine headache: a randomized, double blind, placebo-controlled, dose-ranging study. Cephalalgia 2000, 20:233–243.
Lipton RB, Stewart WF, Ryan RE, et al.: Efficacy and safety of acetaminophen, aspirin, and caffeine in alleviating migraine headache pain: three double blind, randomized, placebo-controlled trials. Arch Neurol 1998, 55:210–217.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Lucas, S. Initial abortive treatments for migraine headache. Curr Treat Options Neurol 4, 343–350 (2002). https://doi.org/10.1007/s11940-002-0044-y
Issue Date:
DOI: https://doi.org/10.1007/s11940-002-0044-y