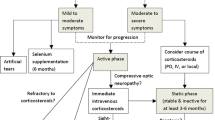
Opinion statement
The treatment of thyroid eye disease is very complex, owing to the varied nature of the symptoms and the variable course of the disease. The first step in treatment should be achieving an euthyroid state or monitoring for the development of hyperthyroidism if the patient is euthyroid at presentation. The second step is local measures (artificial tears and ointment, cessation of smoking) along with careful visual follow-up (acuity, color vision, automated visual fields, fundus examination, ocular motility, and external examination) to assess for the development of optic neuropathy, proptosis, diplopia, and lid abnormalities. If external irritation or orbital discomfort cannot be managed with conservative local measures, then a trial of oral corticosteroids or orbital radiation can be considered. If optic neuropathy develops without proptosis, corticosteroids—starting with an intravenous course, then oral medication —should be used. If there is either an initial improvement in optic neuropathy with corticosteroids, but worsening with subsequent tapering of corticosteroids or no initial improvement, radiation treatment or orbital decompression can be done. If optic neuropathy develops with proptosis, corticosteroids—starting with an intravenous course, then oral medication—should be used for rapid visual improvement. Orbital decompression should then be done to resolve both the optic neuropathy and the proptosis. If for medical reasons the patient with optic neuropathy and proptosis is not a surgical candidate, then radiation treatment can be done, but there will be little change in the proptosis. Proptosis without optic neuropathy can be treated with orbital decompression both for cosmetic reasons and for comfort. Occasionally, this will also resolve lid retraction, and return the lids to an acceptable position in terms of cosmesis and corneal exposure. Diplopia is best treated initially with press-on prisms or patching. Once the disease is stable (ie, no variation in proptosis or change in ocular motility measurements for at least 6 months), eye muscle surgery can be planned. Eye muscle surgery should follow orbital decompression because there is a reasonable possibility that decompression will change ocular motility. If there is corneal exposure or unacceptable lid position and proptosis is not an issue, eyelid surgery, at times on both upper and lower lids, can be done. Eyelid surgery should follow eye muscle surgery because a change in eye position, particularly with vertical muscle surgery, can change eyelid position. Finally, the patient should be made aware at the time of diagnosis that there is unlikely to be a return to normal appearance (ie, appearance before the development of thyroid eye disease).
Similar content being viewed by others
References and Recommended Reading
Bartley GB, Fatourechi V, Kadrmas EF, et al.: The incidence of Graves’ ophthalmopathy in Olmstead County, Minnesota. Am J Ophthalmol 1995, 120:511–517. One of a series of articles from the Mayo Clinic experience with Graves’ ophthalmopathy.
Burch HB, Wartofsky L: Graves’ ophthalmopathy: current concepts regarding pathogenesis and management. Endocr Rev 1993, 14:747–793. Comprehensive, well-referenced review of the topic.
Wiernsinga WM, Smit T, van der Gaarg R, Koomneef L: Temporal relationship between onset of Graves’ ophthalmopathy and onset of thyroidal Graves’ disease. J Endocrinol Invest 1988, 11:615–619.
Bartley G, Gorman CA: Perspective: diagnostic criteria for Graves’ ophthalmopathy. Am J Ophthalmol 1995, 119:792–795.
Perros P, Crombie AL, Kendall-Taylor P: Natural history of thyroid associated ophthalmopathy. Clin Endocrinol 1995, 42:45–50.
Bartalena L, Marcocci C, Tanda ML, et al.: Cigarette smoking and treatment outcomes in Graves’ ophthalmopathy. Ann Intern Med 1998, 129:632–635.
Tagami T, Tanaka K, Sugawa H, et al.: High-dose intravenous steroid pulse therapy in thyroid-associated ophthalmopathy. Endocr J 1996, 43:689–699.
Claridge KG, Ghabrial R, Davis G, et al.: Combined radiotherapy and medical immunosupression in the management of thyroid eye disease. Eye 1997, 11:717–722.
Prummel MF, Mourits MP, Blank L, et al.: Randomized double-blind trial of prednisone versus radiotherapy in Graves’ ophthalmopathy. Lancet 1993, 342:949–954.
Lund VJ, Larkin G, Fells P, Adams G: Orbital decompression for thyroid eye disease: a comparison of external and endoscopic techniques. J Laryngol Otol 1997, 111:1051–1055.
Pitz GKS, Muller-Forell W, Hommel G: Randomized trial of intravenous immunoglobulins versus prednisolone in Graves’ ophthalmopathy. Clin Exp Immunol 1996, 106:197–202.
Leovey A, Bako G, Szabo J, et al.: Combined cyclosporin-A and methylprednisolone treatment of Graves’ ophthalmopathy. Acta Med Hung 1992, 49:179–185.
Krassas GE, Kaltsas T, Dumas A, et al.: Lanreotide in the treatment of patients with thyroid eye disease. Eur J Endocrinol 1997, 136:416–422.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Cornblath, W.T. Thyroid eye disease. Curr Treat Options Neurol 2, 401–405 (2000). https://doi.org/10.1007/s11940-000-0038-6
Issue Date:
DOI: https://doi.org/10.1007/s11940-000-0038-6